Abstract
Purpose
Morphometric studies on idiopathic Chiari malformation type 1 (CM1) pathogenesis have been mainly based on post-natal neuroimaging. Prenatal clues related to CM1 development are lacking. We present pre- and post-natal imaging time course in idiopathic CM1 and assess fetal skull and brain biometry to establish if clues about CM1 development are present at fetal age.
Methods
Multicenter databases were screened to retrieve intrauterine magnetic resonance (iuMR) of children presenting CM1 features at post-natal scan. Syndromes interfering with skull-brain growth were excluded. Twenty-two morphometric parameters were measured at fetal (average 24.4 weeks; range 21 to 32) and post-natal (average 15.4 months; range 1 to 45) age; matched controls were included.
Results
Among 7000 iuMR cases, post-natal scans were available for 925, with postnatal CM1 features reported in seven. None of the fetuses presented CM1 features. Tonsillar descent was clear at a later post-natal scan in all seven cases. Six fetal parameters resulted to be statistically different between CM1 and controls: basal angle (p = 0.006), clivo-supraoccipital angle (p = 0.044), clivus’ length (p = 0.043), posterior cranial fossa (PCF) width (p = 0.009), PCF height (p = 0.045), and PCFw/BPDb (p = 0.013). Postnatally, only the clivus’ length was significant between CM1 cases and controls.
Conclusion
Pre- and post-natal CM1 cases did not share striking common features, making qualitative prenatal assessment not predictive; however, our preliminary results support the view that some of the pathogenetic basis of CM1 may be embedded to some extent already in intrauterine life.

Similar content being viewed by others
References
Chiari H (1891) Ueber Veränderungen des Kleinhirns infolge von Hydrocephalie des Grosshirns 1). DMW - Dtsch Medizinische Wochenschrift 17:1172–1175. https://doi.org/10.1055/s-0029-1206803
Barkovich AJ, Wippold FJ, Sherman JL, Citrin CM (1986) Significance of cerebellar tonsillar position on MR. Am J Neuroradiol 7:795–800
Poretti A, Ashmawy R, Garzon-Muvdi T et al (2016) Chiari type 1 deformity in children: pathogenetic, clinical, neuroimaging, and management aspects. Neuropediatrics 47:293–307. https://doi.org/10.1055/s-0036-1584563
Urbizu A, Martin BA, Moncho D et al (2018) Machine learning applied to neuroimaging for diagnosis of adult classic Chiari malformation: role of the basion as a key morphometric indicator. J Neurosurg 129:779–791. https://doi.org/10.3171/2017.3.JNS162479
Raybaud C, Jallo GI (2018) Chiari 1 deformity in children: etiopathogenesis and radiologic diagnosis. Handb Clin Neurol 155:25–48. https://doi.org/10.1016/B978-0-444-64189-2.00002-0
Chatrath A, Marino A, Taylor D et al (2019) Chiari I malformation in children—the natural history. Child’s Nerv Syst 35:1793–1799. https://doi.org/10.1007/s00381-019-04310-0
Piper RJ, Afshari FT, Soon WC et al (2021) UK Chiari 1 study: protocol for a prospective, observational, multicentre study. BMJ Open 11:1–6. https://doi.org/10.1136/bmjopen-2020-043712
Hiremath SB, Fitsiori A, Boto J et al (2020) The perplexity surrounding chiari malformations - are we any wiser now? Am J Neuroradiol 41:1975–1981. https://doi.org/10.3174/ajnr.A6743
Aintzane Urbizu, Tahir N. Khan, Ashley-Koch A (2017) Genetic dissection of Chiari malformation type 1 using endophenotypes and stratification. J Rare Dis Res Treat 2:35–42. https://doi.org/10.29245/2572-9411/2017/2.1082
Marin-Padilla M, Marin-Padilla TM (1981) Morphogenesis of experimentally induced Arnold-Chiari malformation. J Neurol Sci 50:29–55. https://doi.org/10.1016/0022-510X(81)90040-X
Schady W, Metcalfe RA, Butler P (1987) The incidence of craniocervical bony anomalies in the adult Chiari malformation. J Neurol Sci 82:193–203. https://doi.org/10.1016/0022-510X(87)90018-9
Nishikawa M, Sakamoto H, Hakuba A et al (1997) Pathogenesis of Chiari malformation: a morphometric study of the posterior cranial fossa. J Neurosurg 86:40–47. https://doi.org/10.3171/jns.1997.86.1.0040
Gholampour S, Gholampour H (2020) Correlation of a new hydrodynamic index with other effective indexes in Chiari I malformation patients with different associations. Sci Rep 10:1–13. https://doi.org/10.1038/s41598-020-72961-0
Nwotchouang BST, Ibrahimy A, Loth DM et al (2021) Imaging and health metrics in incidental cerebellar tonsillar ectopia: findings from the Adolescent Brain Cognitive Development Study (ABCD). Neuroradiology 63:1913–1924. https://doi.org/10.1007/s00234-021-02759-y
Milhorat TH, Chou MW, Trinidad EM et al (1999) Chiari I malformation redefined: clinical and radiographic findings for 364 symptomatic patients. Neurosurgery 44:1005–1017. https://doi.org/10.1097/00006123-199905000-00042
Sgouros S, Kountouri M, Natarajan K (2006) Posterior fossa volume in children with Chiari malformation type I. J Neurosurg 105 PEDIAT:101–106. https://doi.org/10.3171/ped.2006.105.2.101
Trigylidas T, Baronia B, Vassilyadi M, Ventureyra ECG (2008) Posterior fossa dimension and volume estimates in pediatric patients with Chiari I malformations. Child’s Nerv Syst 24:329–336. https://doi.org/10.1007/s00381-007-0432-4
Furtado SV, Reddy K, Hegde AS (2009) Posterior fossa morphometry in symptomatic pediatric and adult Chiari I malformation. J Clin Neurosci 16:1449–1454. https://doi.org/10.1016/j.jocn.2009.04.005
Urbizu A, Poca MA, Vidal X et al (2014) MRI-based morphometric analysis of posterior cranial fossa in the diagnosis of Chiari malformation type I. J Neuroimaging 24:250–256. https://doi.org/10.1111/jon.12007
Alperin N, Loftus JR, Oliu CJ et al (2014) Magnetic resonance imaging measures of posterior cranial fossa morphology and cerebrospinal fluid physiology in Chiari malformation type i. Neurosurgery 75:515–522. https://doi.org/10.1227/NEU.0000000000000507
Alkoç OA, Songur A, Eser O et al (2015) Stereological and morphometric analysis of MRI Chiari malformation type-1. J Korean Neurosurg Soc 58:454–461. https://doi.org/10.3340/jkns.2015.58.5.454
Yan H, Han X, Jin M et al (2016) Morphometric features of posterior cranial fossa are different between Chiari I malformation with and without syringomyelia. Eur Spine J 25:2202–2209. https://doi.org/10.1007/s00586-016-4410-y
Righini A, Parazzini C, Doneda C, et al (2011) Fetal MRI features related to the Chiari malformations. Neurol Sci 32 Suppl 3:279–281. https://doi.org/10.1007/s10072-011-0694-1
Christophe C, Bernard D (1999) Magnetic resonance imaging cranial and cerebral dimensions: is there a relationship with Chiari I malformation? A preliminary report in children. Eur J Paediatr Neurol 3:15–24. https://doi.org/10.1053/ejpn.1999.0174
Eppelheimer MS, Houston JR, Bapuraj JR et al (2018) A retrospective 2D morphometric analysis of adult female Chiari type I patients with commonly reported and related conditions. Front Neuroanat 12:2. https://doi.org/10.3389/fnana.2018.00002
Freedman DA (2009) Statistical models: theory and practice. Cambridge University Press
Stoica P, Selén Y (2004) Model-order selection: a review of information criterion rules. IEEE Signal Process Mag 21:36–47
Roller LA, Bruce BB, Saindane AM (2015) Demographic confounders in volumetric MRI analysis: is the posterior fossa really small in the adult Chiari 1 malformation? Am J Roentgenol 204:835–841. https://doi.org/10.2214/AJR.14.13384
Parazzini C, Righini A, Rustico M et al (2008) Prenatal magnetic resonance imaging: brain normal linear biometric values below 24 gestational weeks. Neuroradiology 50:877–883. https://doi.org/10.1007/s00234-008-0421-7
Tilea B, Alberti C, Adamsbaum C et al (2009) Cerebral biometry in fetal magnetic resonance imaging: new reference data. Ultrasound Obstet Gynecol 33:173–181. https://doi.org/10.1002/uog.6276
Conte G, Milani S, Palumbo G et al (2018) Prenatal brain MR imaging: reference linear biometric centiles between 20 and 24 gestational weeks. Am J Neuroradiol 39:963–967. https://doi.org/10.3174/ajnr.A5574
Cogan DG, Barrows LJ (1954) Platybasia and the Arnold-Chiari malformation. AMA Arch Ophthalmol 52:13–29. https://doi.org/10.1001/archopht.1954.00920050015002
Diniz JM, Botelho RV (2020) The role of clivus length and cranial base flexion angle in basilar invagination and Chiari malformation pathophysiology. Neurol Sci 41:1751–1757. https://doi.org/10.1007/s10072-020-04248-1
Triulzi F, Parazzini C, Righini A (2005) MRI of fetal and neonatal cerebellar development. Semin Fetal Neonatal Med 10:411–420. https://doi.org/10.1016/j.siny.2005.05.004
Tuna IS, Kelly TG, Kelly MS et al (2014) The pediatric cerebellum: a pictorial review of normal anatomy using MRI and diffusion tensor imaging. Neurographics 4:158–167. https://doi.org/10.3174/ng.4140096
Khalsa SSS, Siu A, DeFreitas TA et al (2017) Comparison of posterior fossa volumes and clinical outcomes after decompression of Chiari malformation type I. J Neurosurg Pediatr 19:511–517. https://doi.org/10.3171/2016.11.PEDS16263
Rousseau F, Glenn OA, Iordanova B et al (2006) Registration-based approach for reconstruction of high-resolution in utero fetal MR brain images. Acad Radiol 13:1072–1081
Khawam M, de Dumast P, Deman P et al (2021) Fetal brain biometric measurements on 3D super-resolution reconstructed T2-weighted MRI: an intra- and inter-observer agreement study. Front Pediatr 10:639746
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This work was partially supported by grants from the Italian Ministry of Health (“Ricerca corrente” funds to Denis Peruzzo).
Conflict of interest
The Authors have no conflicts of interest.
Ethics approval
Research procedures were performed under the IRB approvals 2015/482 and 2021/ST/232 for retrospective clinical notes review.
Informed consent
Informed consent for acquisition and storage into anonymized databases of the images and the clinical data was obtained from each patient.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.

Fig. S1
The three cases (C3 in A-C; C6 in D-F; C7 in G-I) with neonatal (within 3 months) and a further later scan are reported: some TH and/or PCF crowding being visible at neonatal age, with worsening at follow-up scan. (PNG 1894 kb)

Fig. S2
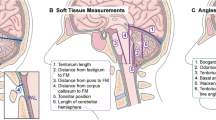
Primary morphometric parameters as were assessed on iuMR scans: posterior fossa angle (α), tentorial angle (β), clivo-supraoccipital angle (γ) and basal angle (δ) on the midsagittal plane in A; FODb (AB), Twining’s line (CD), clivus’ length (CE), foramen magnum AP-b (EF), foramen magnum AP-L (GH), PCFh (IJ) on the midsagittal plane in B; intracranial area (enclosed by the red line) and PCF area (enclosed by the yellow line) on the midsagittal plane in C; FODc (KL) in D; BPDc (MN) and BPDb (OP) on the coronal plane in E; PCFw (QR) and foramen magnum LL (ST) on the coronal plane in F. (PNG 906 kb)

Fig. S3
Primary morphometric parameters as were assessed on post-natal MR imaging: posterior fossa angle (α), tentorial angle (β), clivo-supraoccipital angle (γ) and basal angle (δ) on the midsagittal plane in A; FODb (AB), Twining’s line (CD), clivus’ length (CE), foramen magnum AP-b (EF), foramen magnum AP-L (GH), PCFh (IJ) on the midsagittal plane in B; intracranial area (enclosed by the red line) and PCF area (enclosed by the yellow line) on the midsagittal plane in C; FODc (KL) in D; BPDc (MN) and BPDb (OP) on the coronal plane in E; PCFw (QR) and foramen magnum LL (ST) on the coronal plane in F. (PNG 935 kb)

Fig. S4
Plots of the analyzed parameters of the seven fetal cases (X) are reported with respect to interval variation of normal controls (95 th centile of confidence). GA: gestational age. (PNG 616 kb)
Table S1
(DOCX 31 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Palumbo, G., Arrigoni, F., Peruzzo, D. et al. Onset of Chiari type 1 malformation: insights from a small series of intrauterine MR imaging cases. Neuroradiology 65, 1387–1394 (2023). https://doi.org/10.1007/s00234-023-03183-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-023-03183-0