Abstract
Purpose
Fluoroscopy is widely used to guide diagnostic and therapeutic spine procedures. The purpose of this study was to quantify radiation incident on the operator (operator Air Kerma) during a wide range of fluoroscopy-guided spine procedures and its correlation with the amount of radiation incident on the patient (Kerma Area Product—KAP).
Methods
We retrospectively included 57 consecutive fluoroscopically guided spine procedures. KAP [Gy cm2] and total fluoroscopy time were recorded for each procedure. An electronic dosimeter recorded the operator Air Kerma [μGy] for each procedure. Operator Air Kerma for each procedure, correlation between KAP and operator Air Kerma, and between KAP and fluoroscopy time was obtained.
Results
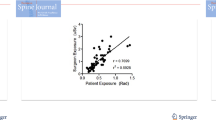
Operator Air Kerma was widely variable across procedures, with median value of 6.4 μGy per procedure. Median fluoroscopy time and median KAP per procedure were 2.6 min and 4.7 Gy cm2, respectively. There was correlation between operator Air Kerma and KAP (r 2 = 0.60), with a slope of 1.6 μGy Air Kerma per unit Gy cm2 KAP incident on the patient and between fluoroscopy time and KAP (r 2 = 0.63).
Conclusion
Operator Air Kerma during individual fluoroscopy-guided spine procedures can be approximated from the commonly and readily available information of the total amount of radiation incident on the patient, measured as KAP.





Similar content being viewed by others
References
Kim TW, Jung JH, Jeon HJ et al (2010) Radiation exposure to physicians during interventional pain procedures. Korean J Pain 23:24–27
el-Khoury GY, Renfrew DL (1991) Percutaneous procedures for the diagnosis and treatment of lower back pain: diskography, facet-joint injection, and epidural injection. AJR Am J Roentgenol 157:685–691
Mroz TE, Yamashita T, Davros WJ et al (2008) Radiation exposure to the surgeon and the patient during kyphoplasty. J Spinal Disord Tech 21:96–100
Tjardes T, Shafizadeh S, Rixen D et al (2010) Image-guided spine surgery: state of the art and future directions. Eur Spine J 19:25–45
Efstathopoulos EP, Pantos I, Andreou M et al (2011) Occupational radiation doses to the extremities and the eyes in interventional radiology and cardiology procedures. Br J Radiol 84:70–77
Botwin KP, Thomas S, Gruber RD et al (2002) Radiation exposure of the spinal interventionalist performing fluoroscopically guided lumbar transforaminal epidural steroid injections. Arch Phys Med Rehabil 83:697–701
Botwin KP, Fuoco GS, Torres FM et al (2003) Radiation exposure to the spinal interventionalist performing lumbar discography. Pain Physician 6:295–300
Botwin KP, Freeman ED, Gruber RD et al (2001) Radiation exposure to the physician performing fluoroscopically guided caudal epidural steroid injections. Pain Physician 4:343–348
Zhou Y, Singh N, Abdi S et al (2005) Fluoroscopy radiation safety for spine interventional pain procedures in university teaching hospitals. Pain Physician 8:49–53
Choi HC (2011) Fluoroscopic radiation exposure during percutaneous kyphoplasty. J Korean Neurosurg Soc 49:37–42
Manchikanti L, Cash KA, Moss TL et al (2003) Risk of whole body radiation exposure and protective measures in fluoroscopically guided interventional techniques: a prospective evaluation. BMC Anesthesiol 3:2
Stecker MS, Balter S, Towbin RB et al (2009) Guidelines for patient radiation dose management. J Vasc Interv Radiol 20:S263–S273
Manchikanti L, Cash KA, Moss TL et al (2002) Radiation exposure to the physician in interventional pain management. Pain Physician 5:385–393
Kallmes DF, O E, Roy SS et al (2003) Radiation dose to the operator during vertebroplasty: prospective comparison of the use of 1-cc syringes versus an injection device. AJNR Am J Neuroradiol 24:1257–1260
Mehdizade A, Lovblad KO, Wilhelm KE et al (2004) Radiation dose in vertebroplasty. Neuroradiology 46:243–245
Ortiz AO, Natarajan V, Gregorius DR et al (2006) Significantly reduced radiation exposure to operators during kyphoplasty and vertebroplasty procedures: methods and techniques. AJNR Am J Neuroradiol 27:989–994
Fish DE, Kim A, Ornelas C et al (2011) The risk of radiation exposure to the eyes of the interventional pain physician. Radiol Res Pract 2011:609537
Lee KP, Lee KM, Park MS et al (2012) Measurements of surgeons’ exposure to ionizing radiation dose during intraoperative use of C-arm fluoroscopy. Spine (Phila Pa 1976) 37:1240–1244
Fishman SM, Smith H, Meleger A et al (2002) Radiation safety in pain medicine. Reg Anesth Pain Med 27:296–305
Mahesh M (2001) Fluoroscopy: patient radiation exposure issues. Radiographics 21:1033–1045
Kruger RP, Faciszewski TMD (2003) Radiation dose reduction to medical staff during vertebroplasty: a review of techniques and methods to mitigate occupational dose. Spine (Phila Pa 1976) 28:1608–1613
Goodman BS, Carnel CT, Mallempati S et al (2011) Reduction in average fluoroscopic exposure times for interventional spinal procedures through the use of pulsed and low-dose image settings. Am J Phys Med Rehabil 90:908–912
Cho JH, Kim JY, Kang JE et al (2011) A study to compare the radiation absorbed dose of the C-arm fluoroscopic modes. Korean J Pain 24:199–204
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
We declare that all procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
For this type of retrospective study formal consent is not required.
Rights and permissions
About this article
Cite this article
Roccatagliata, L., Presilla, S., Pravatà, E. et al. Radiation dose to the operator during fluoroscopically guided spine procedures. Neuroradiology 59, 885–892 (2017). https://doi.org/10.1007/s00234-017-1868-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-017-1868-1