Abstract
Summary
In this systematic review, the effects of osteoporosis patient education were examined. All studies found an effect on physical function, but for the other themes, the results were inconclusive. The findings indicate a need for further research in this topic.
Introduction
Osteoporosis is a chronic disease with serious consequences for the individual and major societal costs. With the aim of fracture prevention, many countries offer osteoporosis patient education. The objectives were to examine the effects and mediators of osteoporosis patient education and describe the characteristics of studies with and without an effect. Though, none of the included studies reported mediators, and therefore, we could not examine that.
Methods
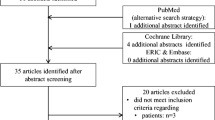
Six databases were searched in October 2020. Two researchers independently conducted title and abstract screening as well as full-text review. Records were included if participants had osteoporosis, and the patient education was group-based, face-to-face, and addressed two or more aspects, e.g., diet, medication, and exercise. The Cochrane Collaboration tools were used for risk of bias assessment. Finally, data were extracted into a standardized form and presented narratively.
Results
In total, 2934 records were identified, and 13 studies met the inclusion criteria. All six studies examining the effects of patient education on physical function demonstrated improvements. In addition, one out of two RCT studies and one non-randomized study reported improved psychological wellbeing. Just one out of five RCT studies showed improvements regarding physical discomfort and disability. Effects on health-related quality of life, adherence and persistence, and knowledge of osteoporosis were inconclusive.
Conclusion
There is limited evidence for the effectiveness of osteoporosis patient education. There is a need for high-quality randomized controlled trials, which should describe the characteristics of the interventions and examine the mechanisms of osteoporosis patient education.
PROSPERO registration number
CRD42020211930


Similar content being viewed by others
Code availability
Not applicable.
References
Hernlund E, Svedbom A, Ivergård M, Compston J, Cooper C, Stenmark J, McCloskey EV, Jönsson B, Kanis JA (2013) Osteoporosis in the European Union: medical management, epidemiology and economic burden. A report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 8(1–2):136. https://doi.org/10.1007/s11657-013-0136-1
Lips P, van Schoor NM (2005) Quality of life in patients with osteoporosis. Osteoporos Int 16(5):447–455. https://doi.org/10.1007/s00198-004-1762-7
Rothmann MJ, Jakobsen PR, Jensen CM, Hermann AP, Smith AC, Clemensen J (2018) Experiences of being diagnosed with osteoporosis: a meta-synthesis. Arch Osteoporos 13(1):21. https://doi.org/10.1007/s11657-018-0436-6
World Health Organization (2003) Prevention and management of osteoporosis: report of a WHO scientific group, vol 921. WHO technical report series, Geneva
Kanis JA, Delmas P, Burckhardt P, Cooper C, Torgerson D (1997) Guidelines for diagnosis and management of osteoporosis. The European Foundation for Osteoporosis and Bone Disease. Osteoporos Int 7(4):390–406. https://doi.org/10.1007/bf01623782
Gold DT, McClung B (2006) Approaches to patient education: emphasizing the long-term value of compliance and persistence. Am J Med 119(4):32S-37S. https://doi.org/10.1016/j.amjmed.2005.12.021
Wilton-Clark MS, Feasel AL, Kline GA, Billington EO (2020) Autonomy begets adherence: decisions to start and persist with osteoporosis treatment after group medical consultation. Arch Osteoporos 15 (1). https://doi.org/10.1007/s11657-020-00809-1
Laslett LL, Lynch J, Sullivan TR, McNeil JD (2011) Osteoporosis education improves osteoporosis knowledge and dietary calcium: comparison of a 4 week and a one-session education course. Int J Rheum Dis 14(3):239–247. https://doi.org/10.1111/j.1756-185X.2011.01628.x
Francis KL, Matthews BL, Van Mechelen W, Bennell KL, Osborne RH (2009) Effectiveness of a community-based osteoporosis education and self-management course: a wait list controlled trial. Osteoporos Int 20(9):1563–1570. https://doi.org/10.1007/s00198-009-0834-0
Davis GC, White TL, Yang A (2006) A bone health intervention for older adults living in residential settings. Res Nurs Health 29(6):566–575. https://doi.org/10.1002/nur.20162
Gaines JM, Narrett M, Parrish JM (2010) The effect of the addition of osteoporosis education to a bone health screening program for older adults. Geriatr Nurs 31(5):348–360. https://doi.org/10.1016/j.gerinurse.2010.04.011
Jensen A, Lomborg K, Langdahl B, Wind G, Jensen AL, Langdahl BL (2016) Managing a bone healthy lifestyle after attending multifaceted group education. Calcif Tissue Int 99(3):272–281. https://doi.org/10.1007/s00223-016-0147-1
Jensen A, Lomborg K, Wind G, Langdahl B (2014) Effectiveness and characteristics of multifaceted osteoporosis group education -a systematic review. Osteoporos Int 25(4):1209–1224. https://doi.org/10.1007/s00198-013-2573-5
Morfeld J-C, Vennedey V, Müller D, Pieper D, Stock S (2017) Patient education in osteoporosis prevention: a systematic review focusing on methodological quality of randomised controlled trials. Osteoporos Int 28(6):1779–1803. https://doi.org/10.1007/s00198-017-3946-y
Giangregorio LM, Macintyre NJ, Thabane L, Skidmore CJ, Papaioannou A (2013) Exercise for improving outcomes after osteoporotic vertebral fracture. Cochrane Database Syst Rev (1):Cd008618. https://doi.org/10.1002/14651858.CD008618.pub2
Hiligsmann M, Salas M, Hughes DA, Manias E, Gwadry-Sridhar FH, Linck P, Cowell W (2013) Interventions to improve osteoporosis medication adherence and persistence: a systematic review and literature appraisal by the ISPOR Medication Adherence & Persistence Special Interest Group. Osteoporos Int 24(12):2907–2918. https://doi.org/10.1007/s00198-013-2364-z
Gleeson T, Iversen MD, Avorn J, Brookhart AM, Katz JN, Losina E, May F, Patrick AR, Shrank WH, Solomon DH (2009) Interventions to improve adherence and persistence with osteoporosis medications: a systematic literature review. Osteoporos Int 20(12):2127–2134. https://doi.org/10.1007/s00198-009-0976-0
Gai QY, Lv H, Li YP, Fu QM, Li P (2020) Education intervention for older adults with osteoporosis: a systematic review. Osteoporos Int 31(4):625–635. https://doi.org/10.1007/s00198-019-05166-5
Lai P, Chua SS, Chan SP (2010) A systematic review of interventions by healthcare professionals on community-dwelling postmenopausal women with osteoporosis. Osteoporos Int 21(10):1637–1656. https://doi.org/10.1007/s00198-010-1199-0
Cooper H, Booth K, Fear S, Gill G (2001) Chronic disease patient education: lessons from meta-analyses. Patient Educ Couns 44(2):107–117. https://doi.org/10.1016/s0738-3991(00)00182-8
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. PLoS Med 6(7):e1000100. https://doi.org/10.1371/journal.pmed.1000100
Higgins JPT, Thomas J, Chandler J, Cumpson M, Li T, Page MJ, Welch VA (2019) Cochrane handbook for systematic reviews of interventions vol 6.0. Cochrane. www.training.cochrane.org/handbook
Abrahamson SJ, Khan F (2006) Brief osteoporosis education in an inpatient rehabilitation setting improves knowledge of osteoporosis in elderly patients with low-trauma fractures. Int J Rehabil Res 29(1):61–64. https://doi.org/10.1097/01.mrr.0000191847.10940.0b
Devereux K, Robertson D, Briffa NK (2005) Effects of a water-based program on women 65 years and over: a randomised controlled trial. Aust J Physiother 51(2):102–108. https://doi.org/10.1016/s0004-9514(05)70038-6
Sterne J, Savović J, Page M, Elbers R, Blencowe N, Boutron I, Cates C, Cheng H-Y, Corbett M, Eldridge S, Hernán M, Hopewell S, Hróbjartsson A, Junqueira D, Jüni P, Kirkham J, Lasserson T, Li T, McAleenan A, Reeves B, Shepperd S, Shrier I, Stewart L, Tilling K, White I, Whiting P, Higgins J (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366 (l4898). https://doi.org/10.1136/bmj.l4898
Sterne J, Hernán M, Reeves B, Savović J, Berkman N, Viswanathan M, Henry D, Altman D, Ansari M, Boutron I, Carpenter J, Chan A, Churchill R, Deeks J, Hróbjartsson A, Kirkham J, Jüni P, Loke Y, Pigott T, Ramsay C, Regidor D, Rothstein H, Sandhu L, Santaguida P, Schünemann H, Shea B, Shrier I, Tugwell P, Turner L, Valentine J, Waddington H, Waters E, Wells G, Whiting P, Higgins J (2016) ROBINS-I: a tool for assessing risk of bias in non-randomized studies of interventions. BMJ 355 (i4919). https://doi.org/10.1136/bmj.i4919
Harrison JE, Chow R, Dornan J, Goodwin S, Strauss A (1993) Evaluation of a program for rehabilitation of osteoporotic patients (PRO): 4-year follow-up. Osteoporos Int 3(1):13–17. https://doi.org/10.1007/BF01623171
Peel C, Lein D, Kitchin B, Morgan S (2001) ‘Tone your bones’: a model for health education for older adults. J Phys Ther Educ 15(2):23–28
Billington EO, Feasel AL, Kline GA (2020) At odds about the odds: women’s choices to accept osteoporosis medications do not closely agree with physician-set treatment thresholds. J Gen Intern Med 35(1):276–282. https://doi.org/10.1007/s11606-019-05384-x
Grahn Kronhed A-C, Enthoven P, Spångeus A, Willerton C (2020) Mindfulness and modified medical yoga as intervention in older women with osteoporotic vertebral fracture. J Altern Complement Med 36(7):610–619. https://doi.org/10.1089/acm.2019.0450
Alp A, Kanat E, Yurtkuran M (2007) Efficacy of a self-management program for osteoporotic subjects. Am J Phys Med Rehabil 86(8):633–640. https://doi.org/10.1097/PHM.0b013e31806dd428
Bergland A, Thorsen H, Kåresen R (2011) Effect of exercise on mobility, balance, and health-related quality of life in osteoporotic women with a history of vertebral fracture: a randomized, controlled trial. Osteoporos Int 22(6):1863–1871. https://doi.org/10.1007/s00198-010-1435-7
Olsen C, Bergland A (2014) The effect of exercise and education on fear of falling in elderly women with osteoporosis and a history of vertebral fracture: results of a randomized controlled trial. Osteoporos Int 25(8):2017–2025. https://doi.org/10.1007/s00198-014-2724-3
Bianchi ML, Duca P, Vai S, Guglielmi G, Viti R, Battista C, Scillitani A, Muscarella S, Luisetto G, Camozzi V et al (2015) Improving adherence to and persistence with oral therapy of osteoporosis. Osteoporos Int 26(5):1629–1638. https://doi.org/10.1007/s00198-015-3038-9
Gold DT, Stegmaier K, Bales CW, Lyles KW, Westlund RE, Drezner MK (1993) Psychosocial functioning and osteoporosis in late life: results of a multidisciplinary intervention. J Womens Health 2(2):149–155. https://doi.org/10.1089/jwh.1993.2.149
Gold DT, Lyles KW, Bales CW, Drezner MK (1989) Editorial: teaching patients coping behaviors: an essential part of successful management of osteoporosis. J Bone Miner Res 4(6):799–801
Gold DT, Shipp KM, Pieper CF, Duncan PW, Martinez S, Lyles KW (2004) Group treatment improves trunk strength and psychological status in older women with vertebral fractures: results of a randomized, clinical trial. J Am Geriatr Soc 52(9):1471–1478. https://doi.org/10.1111/j.1532-5415.2004.52409.x
Chow R, Harrison J, Dornan J (1989) Prevention and rehabilitation of osteoporosis program: exercise and osteoporosis. Int J Rehabil Res 12(1):49–56. https://doi.org/10.1097/00004356-198903000-00005
Kessenich CR, Guyatt GH, Patton CL, Griffith LE, Hamlin A, Rosen CJ (2000) Support group intervention for women with osteoporosis. Rehabil Nurs 25(3):88–92
Nielsen D, Ryg J, Nielsen W, Knold B, Nissen N, Brixen K (2010) Patient education in groups increases knowledge of osteoporosis and adherence to treatment: a two-year randomized controlled trial. Patient Educ Couns 81(2):155–160. https://doi.org/10.1016/j.pec.2010.03.010
Nielsen D, Ryg J, Nissen N, Nielsen W, Knold B, Brixen K (2008) Multidisciplinary patient education in groups increases knowledge on osteoporosis: a randomized controlled trial. Scand J Public Health 36(4):346–352. https://doi.org/10.1177/1403494808089558
Smulders E, Weerdesteyn V, Groen BE, Duysens J, Eijsbouts A, Laan R, van Lankveld W (2010) Efficacy of a short multidisciplinary falls prevention program for elderly persons with osteoporosis and a fall history: a randomized controlled trial. Arch Phys Med Rehabil 91(11):1705–1711. https://doi.org/10.1016/j.apmr.2010.08.004
Smulders E, Weerdesteyn V, Groen B, Duysens J, Laan R, van Lankveld W (2008) The development of a multi-modal fall prevention program for persons with osteoporosis. In: Vincent M, Moreau T (eds) Accidental falls: causes, preventions and interventions. Nova Publisher Inc, New York, pp 185–201
Tüzün S, Akyuz G, Eskiyurt N, Memis A, Kuran B, Icagasioglu A, Sarpel T, Ozdemir F, Ozgirgin N, Gunaydin R, Cakci A, Yurtkuran M (2013) Impact of the training on the compliance and persistence of weekly bisphosphonate treatment in postmenopausal osteoporosis: a randomized controlled study. Int J Med Sci 10(13):1880–1887. https://doi.org/10.7150/ijms.5359
McGuinness LA, Higgins JPT (2020) Risk-of-bias VISualization (robvis): an R package and Shiny web app for visualizing risk-of-bias assessments. Research Synthesis Methods. https://doi.org/10.1002/jrsm.1411
Chen CM, Chang WC, Lan TY (2015) Identifying factors associated with changes in physical functioning in an older population. Geriatr Gerontol Int 15(2):156–164. https://doi.org/10.1111/ggi.12243
Stuck AE, Walthert JM, Nikolaus T, Büla CJ, Hohmann C, Beck JC (1999) Risk factors for functional status decline in community-living elderly people: a systematic literature review. Soc Sci Med 48(4):445–469. https://doi.org/10.1016/S0277-9536(98)00370-0
Guillemin F, Martinez L, Calvert M, Cooper C, Ganiats T, Gitlin M, Horne R, Marciniak A, Pfeilschifter J, Shepherd S, Tosteson A, Wade S, Macarios D, Freemantle N (2013) Fear of falling, fracture history, and comorbidities are associated with health-related quality of life among European and US women with osteoporosis in a large international study. Osteoporos Int 24(12):3001–3010. https://doi.org/10.1007/s00198-013-2408-4
Funnell S, Rogers P (2011) Purposeful program theory: effective use of theories of change and logic models. 1 edn. John Wiley And Sons Ltd, United States of America
Acknowledgements
The authors would like to thank Simon Humeniuk Esrup for his assistance with the title and abstract screening and Magnus Grønlund Bendtsen for assisting with the risk of bias assessment.
Funding
The research was supported by National Research Center for Bone Health, Zealand University Hospital and National Institute of Public Health, University of Southern Denmark.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Mette Friberg Hitz has received grants from Orkla Care, Denmark, UCB, Ellab Fond, and Amgen and received personal payment in relation to lectures and advisory board meetings. Mette Rubæk, Teresa Holmberg, Bodil Marie Thuesen Schønwandt, and Susan Andersen declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rubæk, M., Hitz, M.F., Holmberg, T. et al. Effectiveness of patient education for patients with osteoporosis: a systematic review. Osteoporos Int 33, 959–977 (2022). https://doi.org/10.1007/s00198-021-06226-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-021-06226-5