Abstract
Summary
Individuals with low socio-economic status (SES) have a more than 25% higher risk of fragility fractures than individuals with high SES. Body mass index and lifestyle appear to mediate the effect of SES on fracture risk. Strategies to prevent fractures should aim to reduce unhealthy behaviours through tackling structural inequalities.
Introduction
This systematic review and meta-analysis aimed to evaluate the impact of socio-economic status (SES) on fragility fracture risk.
Methods
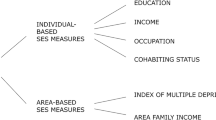
Medline, Embase, and CINAHL databases were searched from inception to 28 April 2021 for studies reporting an association between SES and fragility fracture risk among individuals aged ≥50 years. Risk ratios (RR) were combined in meta-analyses using random restricted maximum likelihood models, for individual-based (education, income, occupation, cohabitation) and area-based (Index of Multiple Deprivation, area income) SES measures.
Results
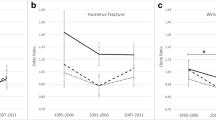
A total of 61 studies from 26 different countries including more than 19 million individuals were included. Individual-based low SES was associated with an increased risk of fragility fracture (RR 1.27 [95% CI 1.12, 1.44]), whilst no clear association was seen when area-based measures were used (RR 1.08 [0.91, 1.30]). The strength of associations was influenced by the type and number of covariates included in statistical models: RR 2.69 [1.60, 4.53] for individual-based studies adjusting for age, sex and BMI, compared with RR 1.06 [0.92, 1.22] when also adjusted for health behaviours (smoking, alcohol, and physical activity). Overall, the quality of the evidence was moderate.
Conclusion
Our results show that low SES, measured at the individual level, is a risk factor for fragility fracture. Low BMI and unhealthy behaviours are important mediators of the effect of SES on fracture risk. Strategies to prevent fractures and reduce unhealthy behaviours should aim to tackle structural inequalities in society thereby reducing health inequalities in fragility fracture incidence.



Similar content being viewed by others
References
Woolf SH, Schoomaker H (2019) Life expectancy and mortality rates in the United States, 1959-2017. Jama 322(20):1996–2016
Morrison MMJATBPGJ (2020) Health equity in England: the Marmot review 10 years on. Institute of Health Equity, London
Nations U (2015) 17 UN Sustainable Development Goals
Pickett KE, Wilkinson RG (2015) Income inequality and health: a causal review. Soc Sci Med 128:316–326
Marmot MG (2003) Understanding social inequalities in health. Perspect Biol Med 46(3 Suppl):S9–S23
Valentin G, Pedersen SE, Christensen R, Friis K, Nielsen CP, Bhimjiyani A, Gregson CL, Langdahl BL (2020) Socio-economic inequalities in fragility fracture outcomes: a systematic review and meta-analysis of prognostic observational studies. Osteoporos Int 31(1):31–42. https://doi.org/10.1007/s00198-019-05143-y
Petit M, Bryere J, Maravic M, Pallaro F, Marcelli C (2017) Hip fracture incidence and social deprivation: results from a French ecological study. Osteoporos Int 28(7):2045–2051. https://doi.org/10.1007/s00198-017-3998-z
Vestergaard P, Rejnmark L, Mosekilde L (2006) Socioeconomic aspects of fractures within universal public healthcare: a nationwide case-control study from Denmark. Scand J Public Health 34(4):371–377. https://doi.org/10.1080/14034940500441223
Brennan SL, Yan L, Lix LM, Morin SN, Majumdar SR, Leslie WD (2015) Sex- and age-specific associations between income and incident major osteoporotic fractures in Canadian men and women: a population-based analysis. Osteoporos Int 26(1):59–65. https://doi.org/10.1007/s00198-014-2914-z
Bhimjiyani A, Neuburger J, Jones T, Ben-Shlomo Y, Gregson CL (2018) The effect of social deprivation on hip fracture incidence in England has not changed over 14 years: an analysis of the English Hospital Episodes Statistics (2001-2015). Osteoporos Int 29(1):115–124. https://doi.org/10.1007/s00198-017-4238-2
Kanis J, Oden A, Johnell O, Jonsson B, De Laet C, Dawson A (2001) The burden of osteoporotic fractures: a method for setting intervention thresholds. Osteoporos Int 12(5):417–427
Kanis J, McCloskey E, Johansson H, Oden A, Ström O, Borgström F (2010) Development and use of FRAX® in osteoporosis. Osteoporos Int 21(2):407–413
Droomers M, Schrijvers CT, Mackenbach JP (2001) Educational level and decreases in leisure time physical activity: predictors from the longitudinal GLOBE study. J Epidemiol Community Health 55(8):562–568. https://doi.org/10.1136/jech.55.8.562
Droomers M, Schrijvers CT, Mackenbach JP (2004) Educational differences in starting excessive alcohol consumption: explanations from the longitudinal GLOBE study. Soc Sci Med 58(10):2023–2033. https://doi.org/10.1016/S0277-9536(03)00411-8
Stronks K, van de Mheen HD, Looman CW, Mackenbach JP (1997) Cultural, material, and psychosocial correlates of the socioeconomic gradient in smoking behavior among adults. Prev Med 26(5 Pt 1):754–766. https://doi.org/10.1006/pmed.1997.0174
De Laet C, Kanis J, Odén A, Johanson H, Johnell O, Delmas P, Eisman J, Kroger H, Fujiwara S, Garnero P (2005) Body mass index as a predictor of fracture risk: a meta-analysis. Osteoporos Int 16(11):1330–1338
Xiang B-Y, Huang W, Zhou G-Q, Hu N, Chen H, Chen C (2017) Body mass index and the risk of low bone mass–related fractures in women compared with men: a PRISMA-compliant meta-analysis of prospective cohort studies. Medicine 96(12):e5290
Gonnelli S, Caffarelli C, Nuti R (2014) Obesity and fracture risk. Clinical Cases in Mineral and Bone Metabolism 11(1):9–14
Cohen AK, Rai M, Rehkopf DH, Abrams B (2013) Educational attainment and obesity: a systematic review. Obes Rev 14(12):989–1005. https://doi.org/10.1111/obr.12062
Brennan SL, Pasco JA, Urquhart DM, Oldenburg B, Hanna F, Wluka AE (2009) The association between socioeconomic status and osteoporotic fracture in population-based adults: a systematic review. Osteoporos Int 20(9):1487–1497
Kristensen P, Thillemann T, Pedersen A, Søballe K, Johnsen S (2017) Socioeconomic inequality in clinical outcome among hip fracture patients: a nationwide cohort study. Osteoporos Int 28(4):1233–1243
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JP, Clarke M, Devereaux PJ, Kleijnen J, Moher D (2009) The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. J Clin Epidemiol 62(10):e1–e34
Lundqvist A, Andersson E, Ahlberg I, Nilbert M, Gerdtham U (2016) Socioeconomic inequalities in breast cancer incidence and mortality in Europe—a systematic review and meta-analysis. The European Journal of Public Health 26(5):804–813
Huguet A, Hayden JA, Stinson J, McGrath PJ, Chambers CT, Tougas ME, Wozney L (2013) Judging the quality of evidence in reviews of prognostic factor research: adapting the GRADE framework. Syst Rev 2:71. https://doi.org/10.1186/2046-4053-2-71
Hayden JA, Cote P, Steenstra IA, Bombardier C, Group Q-LW (2008) Identifying phases of investigation helps planning, appraising, and applying the results of explanatory prognosis studies. J Clin Epidemiol 61(6):552–560. https://doi.org/10.1016/j.jclinepi.2007.08.005
Hayden JA, van der Windt DA, Cartwright JL, Cote P, Bombardier C (2013) Assessing bias in studies of prognostic factors. Ann Intern Med 158(4):280–286. https://doi.org/10.7326/0003-4819-158-4-201302190-00009
Higgins JP, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (2019) Cochrane handbook for systematic reviews of interventions. In. John Wiley & Sons,
Wolinsky FD, Bentler SE, Liu L, Obrizan M, Cook EA, Wright KB, Geweke JF, Chrischilles EA, Pavlik CE, Ohsfeldt RL, Jones MP, Richardson KK, Rosenthal GE, Wallace RB (2009) Recent hospitalization and the risk of hip fracture among older Americans. J Gerontol A Biol Sci Med Sci 64(2):249–255. https://doi.org/10.1093/gerona/gln027
Goldman S, Radomislensky I, Ziv A, Israel Trauma G, Peleg K (2018) The impact of neighborhood socioeconomic disparities on injury. Int J Public Health 63(7):855–863. https://doi.org/10.1007/s00038-018-1119-1
Langeard A, Pothier K, Chastan N, Marcelli C, Chavoix C, Bessot N (2019) Reduced gait and postural stability under challenging conditions in fallers with upper limb fracture. Aging Clin Exp Res 31(4):483–489. https://doi.org/10.1007/s40520-018-0992-z
Cano RP, Galan FG, Dilsen G (1993) Risk factors for hip fracture in Spanish and Turkish women. Bone 14:69–72
Allali F, Rostom S, Bennani L, Abouqal R, Hajjaj-Hassouni N (2010) Educational level and osteoporosis risk in postmenopausal Moroccan women: a classification tree analysis. Clin Rheumatol 29(11):1269–1275. https://doi.org/10.1007/s10067-010-1535-y
Al-Algawy AAH, Baiee HA, Hasan S, Jassim I, Razaq M, Kamel F, Ali A, Khudhair E (2019) Risk factors associated with hip fractures among adult people in Babylon City, Iraq. Open Access Maced J Med Sci 7(21):3608–3614. https://doi.org/10.3889/oamjms.2019.734
Benetou V, Orfanos P, Feskanich D, Michaelsson K, Pettersson-Kymmer U, Ahmed LA, Peasey A, Wolk A, Brenner H, Bobak M, Wilsgaard T, Schottker B, Saum KU, Bellavia A, Grodstein F, Klinaki E, Valanou E, Papatesta EM, Boffetta P, Trichopoulou A (2015) Education, marital status, and risk of hip fractures in older men and women: the CHANCES project. Osteoporos Int 26(6):1733–1746. https://doi.org/10.1007/s00198-015-3054-9
Cauley JA, Wu L, Wampler NS, Barnhart JM, Allison M, Chen Z, Jackson R, Robbins J (2007) Clinical risk factors for fractures in multi-ethnic women: the Women's Health Initiative. J Bone Miner Res 22(11):1816–1826. https://doi.org/10.1359/jbmr.070713
Chen FP, Fu TS, Lin YC, Fan CM (2018) Risk factors and quality of life for the occurrence of hip fracture in postmenopausal women. Biom J 41(3):202–208. https://doi.org/10.1016/j.bj.2018.04.001
Colon-Emeric CS, Biggs DP, Schenck AP, Lyles KW (2003) Risk factors for hip fracture in skilled nursing facilities: who should be evaluated? Osteoporos Int 14(6):484–489. https://doi.org/10.1007/s00198-003-1384-5
Crandall CJ, Han W, Greendale GA, Seeman T, Tepper P, Thurston R, Karvonen-Gutierrez C, Karlamangla AS (2014) Socioeconomic status in relation to incident fracture risk in the Study of Women's Health Across the Nation. Osteoporos Int 25(4):1379–1388. https://doi.org/10.1007/s00198-013-2616-y
Espino DV, Palmer RF, Miles TP, Mouton CP, Wood RC, Bayne NS, Markides KP (2000) Prevalence, incidence, and risk factors associated with hip fractures in community-dwelling older Mexican Americans: results of the Hispanic EPESE study. Establish Population for the Epidemiologic Study for the Elderly. J Am Geriatr Soc 48(10):1252–1260. https://doi.org/10.1111/j.1532-5415.2000.tb02598.x
Farahmand BY, Persson PG, Michaelsson K, Baron JA, Parker MG, Ljunghall S, Swedish Hip Fracture G (2000) Socioeconomic status, marital status and hip fracture risk: a population-based case-control study. Osteoporos Int 11(9):803–808. https://doi.org/10.1007/s001980070060
Fernandez-Ruiz M, Guerra-Vales JM, Trincado R, Medrano MJ, Benito-Leon J, Bermejo-Pareja F (2014) Hip fracture in three elderly populations of central Spain: data from the NEDICES study. Intern Emerg Med 9(1):33–41. https://doi.org/10.1007/s11739-011-0728-y
Holmberg T, Moller S, Rothmann MJ, Gram J, Herman AP, Brixen K, Tolstrup JS, Hoiberg M, Bech M, Rubin KH (2019) Socioeconomic status and risk of osteoporotic fractures and the use of DXA scans: data from the Danish population-based ROSE study. Osteoporos Int 30(2):343–353. https://doi.org/10.1007/s00198-018-4768-2
Johansson H, Hongslo Vala C, Oden A, Lorentzon M, McCloskey E, Kanis JA, Harvey NC, Ohlsson C, Stefan Lohmander L, Karrholm J, Mellstrom D (2018) Low risk for hip fracture and high risk for hip arthroplasty due to osteoarthritis among Swedish farmers. Osteoporos Int 29(3):741–749. https://doi.org/10.1007/s00198-017-4355-y
Kauppi M, Heliovaara M, Impivaara O, Knekt P, Jula A (2011) Parity and risk of hip fracture in postmenopausal women. Osteoporos Int 22(6):1765–1771. https://doi.org/10.1007/s00198-010-1392-1
Ma CC, Burchfiel CM, Grove J, Fekedulegn D, Lu Y, Andrew ME, Willcox B, Masaki KH, Curb JD, Rodriguez BL (2011) Risk factors for fractures among Japanese-American men: the Honolulu Heart Program and Honolulu–Asia Aging Study. Arch Osteoporos 6(1-2):197–207
Meyer HE, Henriksen C, Falch JA, Pedersen JI, Tverdal A (1995) Risk factors for hip fracture in a high incidence area: a case-control study from Oslo, Norway. Osteoporos Int 5(4):239–246. https://doi.org/10.1007/BF01774013
Pluskiewicz W, Adamczyk P, Czekajlo A, Grzeszczak W, Drozdzowska B (2014) Influence of education, marital status, occupation, and the place of living on skeletal status, fracture prevalence, and the course and effectiveness of osteoporotic therapy in women in the RAC-OST-POL Study. J Bone Miner Metab 32(1):89–95. https://doi.org/10.1007/s00774-013-0471-8
Ren Y, Hu J, Lu B, Zhou W, Tan B (2019) Prevalence and risk factors of hip fracture in a middle-aged and older Chinese population. Bone 122:143–149. https://doi.org/10.1016/j.bone.2019.02.020
Rodrigues AM, Eusebio M, Santos MJ, Gouveia N, Tavares V, Coelho PS, Mendes JM, Branco JC, Canhao H (2018) The burden and undertreatment of fragility fractures among senior women. Arch Osteoporos 13(1):22. https://doi.org/10.1007/s11657-018-0430-z
Sanfelix-Gimeno G, Sanfelix-Genoves J, Hurtado I, Reig-Molla B, Peiro S (2013) Vertebral fracture risk factors in postmenopausal women over 50 in Valencia, Spain. A population-based cross-sectional study. Bone 52(1):393–399. https://doi.org/10.1016/j.bone.2012.10.022
Shin CS, Kim MJ, Shim SM, Kim JT, Yu SH, Koo BK, Cho HY, Choi HJ, Cho SW, Kim SW, Kim SY, Yang SO, Cho NH (2012) The prevalence and risk factors of vertebral fractures in Korea. J Bone Miner Metab 30(2):183–192. https://doi.org/10.1007/s00774-011-0300-x
Syddall HE, Evandrou M, Dennison EM, Cooper C, Sayer AA (2012) Social inequalities in osteoporosis and fracture among community-dwelling older men and women: findings from the Hertfordshire Cohort Study. Arch Osteoporos 7:37–48. https://doi.org/10.1007/s11657-012-0069-0
Tsutsumimoto K, Doi T, Makizako H, Hotta R, Nakakubo S, Makino K, Suzuki T, Shimada H (2018) Cognitive frailty is associated with fall-related fracture among older people. J Nutr Health Aging 22(10):1216–1220
van Lenthe FJ, Avendano M, van Beeck EF, Mackenbach JP (2011) Childhood and adulthood socioeconomic position and the hospital-based incidence of hip fractures after 13 years of follow-up: the role of health behaviours. J Epidemiol Community Health 65(11):980–985. https://doi.org/10.1136/jech.2010.115782
Wang Y, Ding H, Wang X, Wei Z, Feng S (2019) Associated factors for osteoporosis and fracture in Chinese elderly. Med Sci Monit 25:5580–5588. https://doi.org/10.12659/MSM.914182
Wändell P, Li X, Carlsson A, Sundquist J, Sundquist K (2021) Osteoporotic fractures among foreign-born individuals: a national Swedish study. Osteoporos Int 32(2):343–352
Xavier RM, Giarola IC, Ocampos GP, Plapler PG, de Camargo OP, de Rezende MU (2019) Profile of patients with osteoporotic fractures and factors that decrease prevention. Acta Ortop Bras 27(2):95–99. https://doi.org/10.1590/1413-785220192702214727
Zacharopoulou G, Zacharopoulou V, Voudouri E, Leondiou L, Dermatis Z (2019) Socioeconomic and clinical risk factors of hip fracture among the elderly: a case-control study. Br J Healthc Manag 25(10):1–16
Zhang XJ, Zhu YB, Liu S, Chen W, Liu B, Zhang F, Lv HZ, Ji CN, Zhang XL, Zhang YZ (2019) Incidence of low-energy upper extremity fractures and the risk factors in Chinese people 50 years or older. Orthop Surg 11(2):304–310. https://doi.org/10.1111/os.12448
Hansen L, Mathiesen AS, Vestergaard P, Ehlers LH, Petersen KD (2013) A health economic analysis of osteoporotic fractures: who carries the burden? Arch Osteoporos 8(1-2):126
Kim J, Jang SN, Lim JY (2019) Pre-existing disability and its risk of fragility hip fracture in older adults. Int J Environ Res Public Health 16(7). https://doi.org/10.3390/ijerph16071237
Lin KB, Yang NP, Lee YH, Chan CL, Wu CH, Chen HC, Chang NT (2018) The incidence and factors of hip fractures and subsequent morbidity in Taiwan: an 11-year population-based cohort study. PLoS One 13(2):e0192388. https://doi.org/10.1371/journal.pone.0192388
Navarro M, Sosa M, Saavedra P, Lainez P, Marrero M, Torres M, Medina C (2009) Poverty is a risk factor for osteoporotic fractures. Osteoporos Int 20(3):393–398
Navarro MC, Saavedra P, Jódar E, Gómez de Tejada MJ, Mirallave A, Sosa M (2013) Osteoporosis and metabolic syndrome according to socio-economic status, contribution of PTH, vitamin D and body weight: the Canarian Osteoporosis Poverty Study (COPS). Clin Endocrinol 78(5):681–686
Park SB, Kim J, Jeong JH, Lee JK, Chin DK, Chung CK, Lee SH, Lee JY (2016) Prevalence and incidence of osteoporosis and osteoporotic vertebral fracture in Korea: nationwide epidemiological study focusing on differences in socioeconomic status. Spine (Phila Pa 1976) 41(4):328–336. https://doi.org/10.1097/BRS.0000000000001291
Peel NM, McClure RJ, Hendrikz JK (2007) Psychosocial factors associated with fall-related hip fractures. Age Ageing 36(2):145–151. https://doi.org/10.1093/ageing/afl167
Suen LK (1998) Occupation and risk of hip fracture. J Public Health Med 20(4):428–433. https://doi.org/10.1093/oxfordjournals.pubmed.a024798
Trimpou P, Landin-Wilhelmsen K, Oden A, Rosengren A, Wilhelmsen L (2010) Male risk factors for hip fracture-a 30-year follow-up study in 7,495 men. Osteoporos Int 21(3):409–416. https://doi.org/10.1007/s00198-009-0961-7
Korpelainen R, Korpelainen J, Heikkinen J, Vaananen K, Keinanen-Kiukaanniemi S (2006) Lifelong risk factors for osteoporosis and fractures in elderly women with low body mass index--a population-based study. Bone 39(2):385–391. https://doi.org/10.1016/j.bone.2006.01.143
Lee KH, Kim JY, Yim SJ, Moon DH, Choi GH, Moon KH (2014) Incidence and risk factors of subsequent hip fractures in Korea: multicenter study. J Korean Med Sci 29(7):992–994. https://doi.org/10.3346/jkms.2014.29.7.992
Reimers A, Laflamme L (2007) Hip fractures among the elderly: personal and contextual social factors that matter. J Trauma Acute Care Surg 62(2):365–369
Brennan SL, Winzenberg TM, Pasco JA, Wluka AE, Dobbins AG, Jones G (2013) Social disadvantage, bone mineral density and vertebral wedge deformities in the Tasmanian Older Adult Cohort. Osteoporos Int 24(6):1909–1916. https://doi.org/10.1007/s00198-012-2211-7
Cassell E, Clapperton A (2013) A decreasing trend in fall-related hip fracture incidence in Victoria, Australia. Osteoporos Int 24(1):99–109. https://doi.org/10.1007/s00198-012-1937-6
Curtis EM, van der Velde R, Moon RJ, van den Bergh JP, Geusens P, de Vries F, van Staa TP, Cooper C, Harvey NC (2016) Epidemiology of fractures in the United Kingdom 1988-2012: variation with age, sex, geography, ethnicity and socioeconomic status. Bone 87:19–26. https://doi.org/10.1016/j.bone.2016.03.006
Jones S, Johansen A, Brennan J, Butler J, Lyons RA (2004) The effect of socioeconomic deprivation on fracture incidence in the United Kingdom. Osteoporos Int 15(7):520–524. https://doi.org/10.1007/s00198-003-1564-3
Maharlouei N, Khodayari M, Forouzan F, Rezaianzadeh A, Lankarani KB (2014) The incidence rate of hip fracture in Shiraz, Iran during 2008-2010. Arch Osteoporos 9:165. https://doi.org/10.1007/s11657-013-0165-9
Oliveira CM, Alves SM, Pina MF (2016) Marked socioeconomic inequalities in hip fracture incidence rates during the Bone and Joint Decade (2000-2010) in Portugal: age and sex temporal trends in a population based study. J Epidemiol Community Health 70(8):755–763. https://doi.org/10.1136/jech-2015-206508
Quah C, Boulton C, Moran C (2011) The influence of socioeconomic status on the incidence, outcome and mortality of fractures of the hip. J Bone Joint Surg (Br) 93(6):801–805. https://doi.org/10.1302/0301-620X.93B6.24936
Bacon WE, Hadden WC (2000) Occurrence of hip fractures and socioeconomic position. J Aging Health 12(2):193–203. https://doi.org/10.1177/089826430001200203
Brennan SL, Leslie WD, Lix LM, Johansson H, Oden A, McCloskey E, Kanis JA (2014) FRAX provides robust fracture prediction regardless of socioeconomic status. Osteoporos Int 25(1):61–69. https://doi.org/10.1007/s00198-013-2525-0
Guilley E, Herrmann F, Rapin CH, Hoffmeyer P, Rizzoli R, Chevalley T (2011) Socioeconomic and living conditions are determinants of hip fracture incidence and age occurrence among community-dwelling elderly. Osteoporos Int 22(2):647–653. https://doi.org/10.1007/s00198-010-1287-1
Taylor AJ, Gary LC, Arora T, Becker DJ, Curtis JR, Kilgore ML, Morrisey MA, Saag KG, Matthews R, Yun H, Smith W, Delzell E (2011) Clinical and demographic factors associated with fractures among older Americans. Osteoporos Int 22(4):1263–1274. https://doi.org/10.1007/s00198-010-1300-8
Zingmond DS, Soohoo NF, Silverman SL (2006) The role of socioeconomic status on hip fracture. Osteoporos Int 17(10):1562–1568. https://doi.org/10.1007/s00198-006-0161-7
Conway DI, McMahon AD, Brown D, Leyland AH (2019) Measuring socioeconomic status and inequalities. 150 cours Albert Thomas, 69372 Lyon Cedex 08, France© International Agency for Research on Cancer Distributed by WHO Press, World Health Organization, 20 Avenue Appia, 1211 Geneva 27, Switzerland 71
Osler M, McGue M, Lund R, Christensen K (2008) Marital status and twins’ health and behavior: an analysis of middle-aged Danish twins. Psychosom Med 70(4):482–487
Funding
AB was supported by a Linda Edwards Memorial PhD Studentship funded by the Royal (formerly National) Osteoporosis Society.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
GV, MBR, EKJ, KF, AB, YBS, AH, CPN, and CLG declare that they have no conflicts of interest. BL has received research funding for her institution from Amgen and Novo Nordisk and honoraria for advisory boards and lectures from UCB, Eli Lilly, Amgen, Gedeon Richter, and Gilead.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 832 kb)
Rights and permissions
About this article
Cite this article
Valentin, G., Ravn, M., Jensen, E. et al. Socio-economic inequalities in fragility fracture incidence: a systematic review and meta-analysis of 61 observational studies. Osteoporos Int 32, 2433–2448 (2021). https://doi.org/10.1007/s00198-021-06038-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-021-06038-7