Abstract
Introduction and hypothesis
To evaluate the efficacy of vaginal CO2 laser in women with stress predominant urinary incontinence (SUI) compared with the sham treatment.
Methods
A randomized controlled trial with sham treatment was conducted between January 2019 and April 2021. Women with predominant SUI were recruited and randomized into two groups: the CO2 laser group (n = 29) and the sham group (n = 30). The International Consultation on Continence Questionnaire—Urinary Incontinence Short Form (ICIQ-UI SF) was used to evaluate the efficacy at 3 months postoperatively. All participants in both groups were advised to perform pelvic floor muscle training (PFMT) after the intervention.
Results
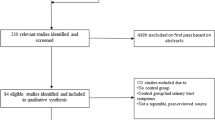
A total of 59 women were studied. A total of 29 women were included in the CO2 laser group and 30 women were included in the sham group. The baseline scores of the ICIQ-UI SF were similar in both groups. A significant improvement in urinary incontinence scores was found in both groups 3 months after treatment (p < 0.001). However, there were no statistically significant differences between the two groups at 3 months (p = 0.8281). There were no changes in bladder neck descent or levator hiatal area immediately after intervention or 3 months after completion of treatment in either group. Most participants who received the active intervention reported mild vaginal pain during the procedure that resolved spontaneously at the end of treatment.
Conclusions
Fractional CO2 laser treatment does not provide any benefit over the sham technique in alleviating SUI symptoms. The improvement in SUI symptoms in both groups might be related to PFMT.
This study was registered with the Thai Clinical Trial Register (TCTR20190131004).

Similar content being viewed by others
Data Availability
The data will be available on request.
References
Bhide AA, Khullar V, Swift S, Digesu GA. The use of laser in urogynaecology. Int Urogynecology J. 2019;30(5):683–92. https://doi.org/10.1007/s00192-018-3844-7.
Digesu GA, Tailor V, Preti M, Vieira-Baptista P, Tarcan T, Stockdale C, et al. The energy based devices for vaginal “rejuvenation”, urinary incontinence, vaginal cosmetic procedures, and other vulvo-vaginal disorders: an international multidisciplinary expert panel opinion. Neurourol Urodyn. 2019;38(3):1005–8. https://doi.org/10.1002/nau.23927.
Preti M, Vieira-Baptista P, Digesu GA, Bretschneider CE, Damaser M, Demirkesen O, et al. The clinical role of LASER for vulvar and vaginal treatments in gynecology and female urology: an ICS/ISSVD best practice consensus document. J Low Genit Tract Dis. 2019;23(2):151–60. https://doi.org/10.1097/LGT.0000000000000462.
Gambacciani M, Palacios S. Laser therapy for the restoration of vaginal function. Maturitas. 2017;99:10–5. https://doi.org/10.1016/j.maturitas.2017.01.012.
Kunzi-Rapp K, Dierickx CC, Cambier B, Drosner M. Minimally invasive skin rejuvenation with Erbium: YAG laser used in thermal mode. Lasers Surg Med. 2006;38(10):899–907. https://doi.org/10.1002/lsm.20380.
El-Domyati M, Abd-El-Raheem T, Medhat W, Abdel-Wahab H, Al AM. Multiple fractional erbium: yttrium-aluminum-garnet laser sessions for upper facial rejuvenation: clinical and histological implications and expectations. J Cosmet Dermatol. 2014;13(1):30–7. https://doi.org/10.1111/jocd.12079.
Tadir Y, Gaspar A, Lev-Sagie A, Alexiades M, Alinsod R, Bader A, et al. Light and energy based therapeutics for genitourinary syndrome of menopause: consensus and controversies. Lasers Surg Med. 2017;49(2):137–59. https://doi.org/10.1002/lsm.22637.
Lapii GA, Yakovleva AY, Neimark AI. Structural reorganization of the vaginal mucosa in stress urinary incontinence under conditions of Er:YAG laser treatment. Bull Exp Biol Med. 2017;162(4):510–4. https://doi.org/10.1007/s10517-017-3650-0.
Franić D, Fistonić I. Laser therapy in the treatment of female urinary incontinence and genitourinary syndrome of menopause: an update. BioMed Res Int. 2019;2019:1576359. https://doi.org/10.1155/2019/1576359.
Buckley BS, Lapitan MCM, Epidemiology Committee of the Fourth International Consultation on Incontinence, Paris, 2008. Prevalence of urinary incontinence in men, women, and children--current evidence: findings of the Fourth International Consultation on Incontinence. Urology. 2010;76(2):265–70. https://doi.org/10.1016/j.urology.2009.11.078.
Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Int Urogynecol J. 2010;21(1):5–26. https://doi.org/10.1007/s00192-009-0976-9.
Carr LK, Robert M, Kultgen PL, Herschorn S, Birch C, Murphy M, et al. Autologous muscle derived cell therapy for stress urinary incontinence: a prospective, dose ranging study. J Urol. 2013;189(2):595–601. https://doi.org/10.1016/j.juro.2012.09.028.
Wu JM. Stress incontinence in women. N Engl J Med. 2021;384(25):2428–36. https://doi.org/10.1056/NEJMcp1914037.
Han L, Wang L, Wang Q, Li H, Zang H. Association between pelvic organ prolapse and stress urinary incontinence with collagen. Exp Ther Med. 2014;7(5):1337–41. https://doi.org/10.3892/etm.2014.1563.
Apichatwong K, Asdornwised U, Pinyopasakul W, Tantiwong A, Leerasiri P. Factors associated with sexual functions in women with urinary incontinence. Nurs Sci J. 2016;34(4):47–56.
González Isaza P, Jaguszewska K, Cardona JL, Lukaszuk M. Long-term effect of thermoablative fractional CO2 laser treatment as a novel approach to urinary incontinence management in women with genitourinary syndrome of menopause. Int Urogynecol J. 2018;29(2):211–5. https://doi.org/10.1007/s00192-017-3352-1.
Dabaja H, Lauterbach R, Matanes E, Gruenwald I, Lowenstein L. The safety and efficacy of CO2 laser in the treatment of stress urinary incontinence. Int Urogynecol J. 2020;31(8):1691–6. https://doi.org/10.1007/s00192-019-04204-4.
Alcalay M, Ben Ami M, Greenshpun A, Hagay Z, Schiff E. Fractional-pixel CO2 laser treatment in patients with urodynamic stress urinary incontinence: 1-year follow-up. Lasers Surg Med. 2021;53(7):960–7. https://doi.org/10.1002/lsm.23329.
Franić D, Fistonić I, Franić-Ivanišević M, Perdija Ž, Križmarić M. Pixel CO2 laser for the treatment of stress urinary incontinence: a prospective observational multicenter study. Lasers Surg Med. 2021;53(4):514–20. https://doi.org/10.1002/lsm.23319.
Nalewczynska AA, Barwijuk M, Kolczewski P, Dmoch-Gajzlerska E. Pixel-CO2 laser for the treatment of stress urinary incontinence. Lasers Med Sci. 2022;37(2):1061–7. https://doi.org/10.1007/s10103-021-03353-7.
Palacios S, Ramirez M. Efficacy of the use of fractional CO2RE intima laser treatment in stress and mixed urinary incontinence. Eur J Obstet Gynecol Reprod Biol. 2020;244:95–100. https://doi.org/10.1016/j.ejogrb.2019.10.048.
Ranjbar A, Mehrnoush V, Darsareh F, Kotb A, Zakaria A, Shekari M, et al. Vaginal laser therapy for stress urinary incontinence: a systematic review of prospective randomized clinical trials. J Menopausal Med. 2022;28(3):103–11. https://doi.org/10.6118/jmm.22017.
Aguiar LB, Politano CA, Costa-Paiva L, Juliato CRT. Efficacy of fractional CO2 laser, promestriene, and vaginal lubricant in the treatment of urinary symptoms in postmenopausal women: a randomized clinical trial. Lasers Surg Med. 2020;52(8):713–20. https://doi.org/10.1002/lsm.23220.
Seki AS, Bianchi-Ferraro AMHM, Fonseca ESM, Sartori MGF, Girão MJBC, Jarmy-Di Bella ZIK. CO2 Laser and radiofrequency compared to a sham control group in treatment of stress urinary incontinence (LARF study arm 3). A randomized controlled trial. Int Urogynecol J. 2022;33(12):3535–42. https://doi.org/10.1007/s00192-022-05091-y.
Blaganje M, Šćepanović D, Žgur L, Verdenik I, Pajk F, Lukanović A. Non-ablative Er:YAG laser therapy effect on stress urinary incontinence related to quality of life and sexual function: a randomized controlled trial. Eur J Obstet Gynecol Reprod Biol. 2018;224:153–8. https://doi.org/10.1016/j.ejogrb.2018.03.038.
Lauterbach R, Aharoni S, Justman N, Farago N, Gruenwald I, Lowenstein L. The efficacy and safety of a single maintenance laser treatment for stress urinary incontinence: a double-blinded randomized controlled trial. Int Urogynecol J. 2022;33(12):3499–504. https://doi.org/10.1007/s00192-022-05103-x.
Funding
Faculty of Medicine, Khon Kaen university, Khon Kaen, Thailand.
Author information
Authors and Affiliations
Contributions
Teerayut Temtanakitpaisan: Protocol development, Data collection or management, Data analysis and Manuscript writing.
Chompilas Chongsomchai: Protocol development and Manuscript editing.
Pranom Buppasiri: Protocol development and Manuscript editing.
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Temtanakitpaisan, T., Chongsomchai, C. & Buppasiri, P. Fractional CO2 laser treatment for women with stress predominant urinary incontinence: a randomized controlled trial. Int Urogynecol J 34, 2827–2832 (2023). https://doi.org/10.1007/s00192-023-05655-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-023-05655-6