Abstract
Introduction and hypothesis
Understanding patient preferences regarding provider characteristics is an under-explored area in urogynecology. This study aims to describe patient preferences for urogynecologic care, including provider gender, age, experience, and presence of medical trainees.
Methods
This was a multicenter, cross-sectional, survey-based study assessing patient preferences with a voluntary, self-administered, anonymous questionnaire prior to their first urogynecology consult. A 5-point Likert scale addressing provider gender, age, experience, and presence of trainees was used. Descriptive statistics summarized patient characteristics and provider preferences. Chi-squared (or Fisher’s exact) test was used to test for associations.
Results
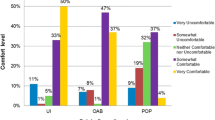
Six hundred fifteen women participated from eight sites including all geographic regions across the US; 70.8% identified as white with mean age of 58.5 ± 14.2 years. Urinary incontinence was the most commonly reported symptom (45.9%); 51.4% saw a female provider. The majority of patients saw a provider 45–60 years old (42.8%) with > 15 years’ experience (60.9%). Sixty-five percent of patients preferred a female provider; 10% preferred a male provider. Sixteen percent preferred a provider < 45 years old, 36% preferred 45–60 years old, and 11% of patients preferred a provider > 60 years old. Most patients preferred a provider with 5–15 or > 15 years’ experience (49% and 46%, respectively). Eleven percent preferred the presence of trainees while 24% preferred trainee absence.
Conclusion
Patient preferences regarding urogynecologic providers included female gender and provider age 45–60 years old with > 5 years’ experience. Further study is needed to identify qualitative components associated with these preferences.


Similar content being viewed by others
References
Rayburn WF, Liu CQ, Elwell EC, Rogers RG. Diversity of physician faculty in obstetrics and gynecology. J Reprod Med. 2016;61(1–2):22–6.
Neubardt SB, moderator. Women’s liberation and the male gynecologist [roundtable]. Med Aspect Hum Sex 1974;8:158–199.
Jolliff L, Leadley J, Coakley E, Sloane RA. Women in US academic medicine and science: statistics and benchmarking report 2011–2012. Washington, DC: Association of American Medical Colleges; 2012.
Haar E, Halitsky V, Stricker G. Factors related to the preference for a female gynecologist. Med Care. 1975;13:782–90.
Johnson AM, Schnatz PF, Kelsey AM, Ohannessian CM. Do women prefer care from female or male obstetrician–gynecologists? A study of patient gender preference. J Am Osteopath Assoc. 2005;105:369–79.
Plunkett BA, Kohli P, Milad MP. The importance of physician gender in the selection of an obstetrician or a gynecologist. Am J Obstet Gynecol. 2002;186(5):926–8.
Janssen SM, Lagro-Janssen AL. Physician’s gender, communication style, patient preferences and patient satisfaction in gynecology and obstetrics: a systematic review. Patient Educ Couns. 2012;89(2):221–6. https://doi.org/10.1016/j.pec.2012.06.034.
Huis Int’Veld EA, Canales FL, Furnas HJ. The impact of a plastic surgeon’s gender on patient choice. Aesthet Surg J. 2017 Apr 1;37(4):466–71.
Dusch MN, O’Sullivan PS, Ascher NL. Patient perceptions of female surgeons: how surgeon demeanor and type of surgery affect patient preference. J Surg Res. 2014 Mar;187(1):59–64.
Abghari MS, Takemoto R, Sadiq A, Karia R, Phillips D, Egol KA. Patient perceptions and preferences when choosing an orthopaedic surgeon. Iowa Orthop J. 2014;34:204–8.
Brueseke T, Muffly T, Rayburn W, Connolly A, Nieto M, De La Cruz J, et al. Workforce analysis of female pelvic medicine and reconstructive surgery, 2015 to 2045. Female Pelvic Med Reconst Surg. 2016;22:385–9.
York NL, DaRosa DA, Markwell SJ, Niehaus AH, Folse R. Patients’ attitudes toward the involvement of medical students in their care. Am J Surg. 1995;169(4):421–3.
O’Malley PG, Omori DM, Laudry FJ, Jackson J, Kroenke K. A prospective study to assess the effect of ambulatory teaching on patient satisfaction. Acad Med. 1997;72(11):1015–7.
Malcolm CE, Wong KK, Elwood-Martin R. Patients’ perceptions and experiences of family medicine residents in the office. Can Fam Physician. 2008;54(4):570–1.
Jiang X, Altomare C, Egan JF, Tocco DB, Schnatz PF. The ObGyn clerkship: are students denied the opportunity to provide patient care and what is the role of gender? Conn Med. 2012;76(4):231–6.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG. Research electronic data capture (REDCap)--a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform. 2009;42(2):377–81. https://doi.org/10.1016/j.jbi.2008.08.010.
(2011) TF–IDF. In: Sammut C., Webb G.I. (eds) Encyclopedia of Machine Learning. Springer, Boston, MA.
Joachims T. A probabilistic analysis of the Rocchio algorithm with TFIDF for text categorization: DTIC document, 1996.
Fellows I. wordcloud: Word Clouds, 2018. R package version 2.6. https://CRAN.R-project.org/package=wordcloud.
Funding
This study was supported by a grant from the AUGS/SGS Group of the Fellows’ Pelvic Research Network. The funding source had no role in the conduct of the research, data collection, analysis, interpretation of data, writing of the manuscript, or decision to submit the manuscript for publication. Statistical analysis of research reported in this publication was partially supported by National Center for Advancing Translational Sciences of the National Institutes of Health under award number UL1TR003096.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
This study was supported by a grant from the AUGS/SGS Group of the Fellows’ Pelvic Research Network.
The authors report no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 86 kb)
Rights and permissions
About this article
Cite this article
Hoke, T.P., Berger, A.A., Pan, C.C. et al. Assessing patients’ preferences for gender, age, and experience of their urogynecologic provider. Int Urogynecol J 31, 1203–1208 (2020). https://doi.org/10.1007/s00192-019-04189-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-019-04189-0



