Abstract
Introduction and hypothesis
Studies have suggested that a posterior vaginal wall prolapse might compress the urethra and mask stress urinary incontinence (SUI), much like an anterior vaginal wall prolapse. A recent study with urethral pressure reflectometry (UPR) has shown that the urethral closure mechanism deteriorates after anterior colporrhaphy; this could explain the occurrence of postoperative de novo SUI. We hypothesized that urethral pressure would also decrease after posterior colporrhaphy.
Methods
This was a prospective, observational study where women with posterior vaginal wall prolapse ≥stage II were examined before and after posterior colporrhaphy. We performed prolapse staging according to the Pelvic Organ Prolapse Quantification system, UPR measurements at rest, during squeezing and straining, and standardized stress tests with 300 ml saline. The women filled out International Consultation on Incontinence-Urinary incontinence (ICIQ-UI) short forms. The sample size was 18, with a power of 99.9% and a level of significance of 5%. Parameters were compared using paired t tests or Fisher’s exact test, where appropriate; p values <0.05 were considered statistically significant.
Results
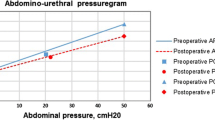
Eighteen women with posterior vaginal wall prolapse ≥stage II were recruited. One woman did not undergo surgery. There were no changes in urethral pressure at rest (p = 0.4), during squeezing (p = 0.2) or straining (p = 0.2), before and after surgery. The results of the stress tests and ICIQ-UI short forms were the same after surgery.
Conclusions
The urethral closure mechanism is not affected by posterior colporrhaphy. Our study does not support the theory that the posterior vaginal wall prolapse compresses the urethra and masks SUI.

Similar content being viewed by others
References
Marinkovic SP, Stanton SL. Incontinence and voiding difficulties associated with prolapse. J Urol. 2004;171:1021–8. doi:10.1097/01.ju.0000111782.37383.e2.
Nguyen JN, Yazdany T, Burchette RJ. Urodynamic evaluation of urethral competency in women with posterior vaginal support defects. Urology. 2007;69:87–90. doi:10.1016/j.urology.2006.09.068.
Smith TM, DeLancey JOL, Fenner DE. Post-reduction stress urinary incontinence rates in posterior versus anterior pelvic organ prolapse: a secondary analysis. Int Urogynecol J. 2013;24:1355–60. doi:10.1007/s00192-012-2019-1.
Ellström Engh AM, Ekeryd A, Magnusson Å, et al. Can de novo stress incontinence after anterior wall repair be predicted? Acta Obstet Gynecol Scand. 2011;90:488–93. doi:10.1111/j.1600-0412.2011.01087.x.
Svenningsen R, Borstad E, Spydslaug AE, et al. Occult incontinence as predictor for postoperative stress urinary incontinence following pelvic organ prolapse surgery. Int Urogynecol J. 2012;23:843–9. doi:10.1007/s00192-012-1764-5.
Visco AG, Brubaker L, Nygaard I, et al. The role of preoperative urodynamic testing in stress-continent women undergoing sacrocolpopexy: the Colpopexy and Urinary Reduction Efforts (CARE) randomized surgical trial. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19:607–14. doi:10.1007/s00192-007-0498-2.
Khayyami Y, Klarskov N, Lose G. The promise of urethral pressure reflectometry: an update. Int Urogynecol J. 2016;27:1449–58 doi:10.1007/s00192-016-2964-1.
Klarskov N, Lose G. Urethral pressure reflectometry vs urethral pressure profilometry in women: a comparative study of reproducibility and accuracy. BJU Int. 2007;100:351–6. doi:10.1111/j.1464-410X.2007.06922.x.
Saaby M-L, Klarskov N, Lose G. Urethral pressure reflectometry during intra-abdominal pressure increase—an improved technique to characterize the urethral closure function in continent and stress urinary incontinent women. Neurourol Urodyn. 2013;32:1103–8. doi:10.1002/nau.22368.
Saaby M-L, Klarskov N, Lose G. The impact of tension-free vaginal tape on the urethral closure function: mechanism of action. Neurourol Urodyn. 2015;34:50–4. doi:10.1002/nau.22513.
Khayyami Y, Klarskov N, Lose G. Abstract: urethral pressure reflectometry predicts stress urinary incontinence after anterior colporrhaphy. Neurourol Urodyn. 2016;35:S1–S471. doi:10.1002/nau.23074.
Myers DL, Lasala CA, Hogan JW, Rosenblatt PL. The effect of posterior wall support defects on urodynamic indices in stress urinary incontinence. Obstet Gynecol. 1998;91:710–4.
Khayyami Y, Lose G, Klarskov N. Urethral pressure reflectometry in women with pelvic organ prolapse: a study of reproducibility. Int Urogynecol J. 2016;28:705–10. doi:10.1007/s00192-016-3187-1.
Klarskov N. Urethral pressure reflectometry. A method for simultaneous measurements of pressure and cross-sectional area in the female urethra. Dan Med J. 2012;59:B4412.
Haylen BT, Maher CF, Barber MD, et al. An International Urogynecological association (IUGA)/International continence society (ICS) joint report on the terminology for female pelvic organ prolapse (POP). Int Urogynecol J. 2016;27:165–94. doi:10.1007/s00192-015-2932-1.
Zivkovic F, Tamussino K, Haas J. Contribution of the posterior compartment to the urinary continence mechanism. Obstet Gynecol. 1998;91:229–33.
Schäfer W. Some biomechanical aspects of continence function. Scand J Urol Nephrol Suppl. 2001;207:44–60. discussion 106–25.
Mouritsen L, Larsen JP. Symptoms, bother and POPQ in women referred with pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2003;14:122–7. doi:10.1007/s00192-002-1024-1.
Weber AM. Is urethral pressure profilometry a useful diagnostic test for stress urinary incontinence? Obstet Gynecol Surv. 2001;56:720–35.
Ellerkmann RM, Cundiff GW, Melick CF, et al. Correlation of symptoms with location and severity of pelvic organ prolapse. Am J Obstet Gynecol. 2001;185:1332–7; discussion 1337–8. doi:10.1067/mob.2001.119078.
Acknowledgements
We thank Nurse Berit Sejersen Larsen for her assistance with all examinations in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The study was conducted at the Department of Gynecology and Obstetrics, Herlev Gentofte hospital and funded by the University of Copenhagen as a PhD scholarship. The University of Copenhagen was not involved in the study.
Conflicts of interest
Yasmine Khayyami, Gunnar Lose, and Niels Klarskov have received honoraria as investigators from Astellas. Gunnar Lose has also been a consultant for Contura.
Rights and permissions
About this article
Cite this article
Khayyami, Y., Lose, G. & Klarskov, N. Posterior colporrhaphy does not affect the urethral closure mechanism. Int Urogynecol J 29, 125–130 (2018). https://doi.org/10.1007/s00192-017-3401-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-017-3401-9