Abstract
Purpose
To systematically analyse post-operative outcomes following enhanced microfracture procedures in focal cartilage injuries of the knee.
Methods
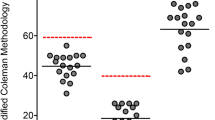
Database searches were conducted in PubMed, EMBASE and Cochrane Library databases up to 30 November 2018, for clinical studies in humans that assessed surgical outcomes of enhanced microfracture procedures in focal cartilage injuries of the knee. The clinical, functional and imaging outcomes were assessed and summarized. The MINORS scale was used to assess the methodological quality of the studies included.
Results
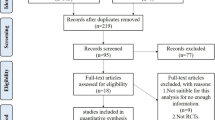
Ten studies were included comprising a total of 331 patients (mean age of 37.0 ± 5.5 years, body mass 25.2 ± 1.7 kg m2, 56% male and 42% left knee), 278 femoral condyle chondral defects (147 medial, 35 lateral and 78 undefined) and 43 chondral defects distributed by the tibial plateau, patella and femoral trochlea. The chondral defects were mostly Outerbridge grade III or IV and the mean defect size was 3.2 ± 0.6 cm2. Studies consistently demonstrated significant improvement in the patient-reported outcome measures from baseline to final follow-up. Overall, imaging outcomes showed inconsistent results. Treatment-related adverse events were poorly reported.
Conclusion
Enhanced microfracture techniques significantly result in improved patient-reported outcome measures over the MCID, but provide inconsistent imaging results. Current clinical evidence does not allow for unequivocal recommendation of enhanced microfracture to treat symptomatic focal grade III/IV knee cartilage lesions.
Level of evidence
IV.

Similar content being viewed by others
Abbreviations
- MFX:
-
Microfracture
- MCID:
-
Minimal clinically important difference
- AMIC:
-
The autologous matrix-induced chondrogenesis
- CS:
-
Chondroitin sulphate
- MRI:
-
Magnetic resonance imaging
- MOCART:
-
Magnetic Resonance Observation of Cartilage Repair Tissue
- IKDC:
-
International Knee Documentation Committee Subjective Knee Form
- WOMAC:
-
Western Ontario and McMaster Universities Arthritis Index
- KOOS:
-
Knee Injury and Osteoarthritis Outcome Score
- VAS:
-
Visual Analogue Scale
References
Anders S (2013) A randomized, controlled trial comparing autologous matrix-induced chondrogenesis (AMIC®) to microfracture: analysis of 1- and 2-year follow-up data of 2 centers. Open Orthop J 3:133–143
Arshi A, Fabricant PD, Go DE, Williams RJ, McAllister DR, Jones KJ (2018) Can biologic augmentation improve clinical outcomes following microfracture for symptomatic cartilage defects of the knee? A systematic review. Cartilage 9:146–155
Benthien JP, Behrens P (2010) Autologous matrix-induced chondrogenesis (AMIC): combining microfracturing and a collagen I/III Matrix for articular cartilage resurfacing. Cartilage 1:65–68
Bertho P, Pauvert A, Pouderoux T, Robert H (2018) Treatment of large deep osteochondritis lesions of the knee by autologous matrix-induced chondrogenesis (AMIC): preliminary results in 13 patients. Orthop Traumatol Surg Res 104:695–700
Brown WE, Potter HG, Marx RG, Wickiewicz TL, Warren RF (2004) Magnetic resonance imaging appearance of cartilage repair in the knee. Clin Orthop Relat Res 422:214–223
Chevrier A, Hoemann CD, Sun J, Buschmann MD (2007) Chitosan-glycerol phosphate/blood implants increase cell recruitment, transient vascularization and subchondral bone remodeling in drilled cartilage defects. Osteoarthr Cartil 15:316–327
Chuah YJ, Peck Y, Lau JEJ, Hee HT, Wang D-A (2017) Hydrogel based cartilaginous tissue regeneration: recent insights and technologies. Biomater Sci 5:613–631
Chung JY, Lee DH, Kim TH, Kwack KS, Yoon KH, Min BH (2014) Cartilage extra-cellular matrix biomembrane for the enhancement of microfractured defects. Knee Surg Sport Traumatol Arthrosc 22:1249–1259
D’Antimo C, Biggi F, Borean A, Di Fabio S, Pirola I (2017) Combining a novel leucocyte-platelet-concentrated membrane and an injectable collagen scaffold in a single-step AMIC procedure to treat chondral lesions of the knee: a preliminary retrospective study. Eur J Orthop Surg Traumatol 27:673–681
Devitt BM, Bell SW, Webster KE, Feller JA, Whitehead TS (2017) Surgical treatments of cartilage defects of the knee: systematic review of randomised controlled trials. Knee 24:508–517
Gao L, Orth P, Cucchiarini M, Madry H (2019) Autologous matrix-induced chondrogenesis: a systematic review of the clinical evidence. Am J Sports Med 47:222–231
Gille J, Behrens P, Volpi P, de Girolamo L, Reiss E, Zoch W, Anders S (2013) Outcome of Autologous Matrix Induced Chondrogenesis (AMIC) in cartilage knee surgery: data of the AMIC Registry. Arch Orthop Trauma Surg 133:87–93
Goyal D, Keyhani S, Lee EH, Hui JHP (2013) Evidence-based status of microfracture technique: a systematic review of level I and II studies. Arthroscopy 29:1579–1588
Hancock KJ, Westermann RR, Shamrock AG, Duchman KR, Wolf BR, Amendola A (2019) Trends in knee articular cartilage treatments: an american board of orthopaedic surgery database study. J Knee Surg 32:85–90
Heijink A, Gomoll AH, Madry H, Drobnic M, Filardo G, Espregueira-Mendes J, Van Dijk CN (2012) Biomechanical considerations in the pathogenesis of osteoarthritis of the knee. Knee Surg Sports Traumatol Arthrosc 20:423–435
Hoemann CD, Hurtig M, Rossomacha E, Sun J, Chevrier A, Shive MS, Buschmann MD (2005) Chitosan-glycerol phosphate/blood implants improve hyaline cartilage repair in ovine microfracture defects. J Bone Joint Surg Am 87:2671–2686
Hoemann CD, Sun J, McKee MD, Chevrier A, Rossomacha E, Rivard G-E, Hurtig M, Buschmann MD (2007) Chitosan-glycerol phosphate/blood implants elicit hyaline cartilage repair integrated with porous subchondral bone in microdrilled rabbit defects. Osteoarthritis Cartilage 15:78–89
Hoemann CD, Tran-Khanh N, Chevrier A, Chen G, Lascau-Coman V, Mathieu C, Changoor A, Yaroshinsky A, McCormack RG, Stanish WD, Buschmann MD (2015) Chondroinduction Is the Main Cartilage Repair Response to Microfracture and Microfracture With BST-CarGel: results as Shown by ICRS-II Histological Scoring and a Novel Zonal Collagen Type Scoring Method of Human Clinical Biopsy Specimens. Am J Sports Med 43:2469–2480
Ioannidis JPA (2005) Why most published research findings are false. PLoS Med 2:e124
Irrgang J (2012) Summary of clinical outcome measures for sports-related knee injuries. AOSSM Outcomes Task Force. http://www.privatehomepage.com. Accessed 03 Oct 2019
Jones KJ, Kelley BV, Arshi A, McAllister DR, Fabricant PD (2019) Comparative effectiveness of cartilage repair with respect to the minimal clinically important difference. Am J Sports Med. https://doi.org/10.1177/0363546518824552
Knutsen G, Drogset JO, Engebretsen L, Grontvedt T, Isaksen V, Ludvigsen TC, Roberts S, Solheim E, Strand T, Johansen O (2007) A randomized trial comparing autologous chondrocyte implantation with microfracture. Findings at five years. J Bone Joint Surg Am 89:2105–2112
Knutsen G, Engebretsen L, Ludvigsen TC, Drogset JO, Grontvedt T, Solheim E, Strand T, Roberts S, Isaksen V, Johansen O (2004) Autologous chondrocyte implantation compared with microfracture in the knee. A randomized trial. J Bone Joint Surg Am 86:455–464
Kusano T, Jakob RP, Gautier E, Magnussen RA, Hoogewoud H, Jacobi M (2012) Treatment of isolated chondral and osteochondral defects in the knee by autologous matrix-induced chondrogenesis (AMIC). Knee Surg Sport Traumatol Arthrosc 20:2109–2115
Lee YHD, Suzer F, Thermann H (2014) Autologous matrix-induced chondrogenesis in the knee: a review. Cartilage 5:145–153
Makris EA, Gomoll AH, Malizos KN, Hu JC, Athanasiou KA (2014) Repair and tissue engineering techniques for articular cartilage. Nat Rev Rheumatol 11:21–34
Methot S, Changoor A, Tran-Khanh N, Hoemann CD, Stanish WD, Restrepo A, Shive MS, Buschmann MD (2016) Osteochondral biopsy analysis demonstrates that BST-CarGel treatment improves structural and cellular characteristics of cartilage repair tissue compared with microfracture. Cartilage 7:16–28
Mithoefer K, McAdams T, Williams RJ, Kreuz PC, Mandelbaum BR (2009) Clinical efficacy of the microfracture technique for articular cartilage repair in the knee: an evidence-based systematic analysis. Am J Sports Med 37:2053–2063
Mithoefer K, Venugopal V, Manaqibwala M (2016) Incidence, degree, and clinical effect of subchondral bone overgrowth after microfracture in the knee. Am J Sports Med 44:2057–2063
Moher D, Liberati A, Tetzlaff J, Altman DG (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med 151(264–9):W64
Montgomery SR, Foster BD, Ngo SS, Terrell RD, Wang JC, Petrigliano FA, McAllister DR (2014) Trends in the surgical treatment of articular cartilage defects of the knee in the United States. Knee Surg Sports Traumatol Arthrosc 22:2070–2075
Moyad TF (2011) Cartilage injuries in the adult knee: evaluation and management. Cartilage 2:226–236
Orth P, Gao L, Madry H (2019) Microfracture for cartilage repair in the knee: a systematic review of the contemporary literature. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-019-05359-9
Pascarella A, Ciatti R, Pascarella F, Latte C, Di Salvatore MG, Liguori L, Iannella G (2010) Treatment of articular cartilage lesions of the knee joint using a modified AMIC technique. Knee Surg Sport Traumatol Arthrosc 18:509–513
Patrascu JM, Freymann U, Kaps C, Poenaru DV (2010) Repair of a post-traumatic cartilage defect with a cell-free polymer-based cartilage implant: a follow-up at two years by MRI and histological review. J Bone Joint Surg Br 92:1160–1163
Pipino G, Risitano S, Alviano F, Wu EJ, Bonsi L, Vaccarisi DC, Indelli PF (2019) Microfractures and hydrogel scaffolds in the treatment of osteochondral knee defects: a clinical and histological evaluation. J Clin Orthop Trauma 10:67–75
Roos EMLL (2003) The Knee injury and Osteoarthritis Outcome Score (KOOS): from joint injury to osteoarthritis. Heal Qual Life Outcomes 1:64
Saltzman BM, Redondo ML, Beer A, Cotter EJ, Frank RM, Yanke AB, Cole BJ (2018) Wide variation in methodology in Level I and II studies on cartilage repair: a systematic review of available clinical trials comparing patient demographics, treatment means, and outcomes reporting. Cartilage. https://doi.org/10.1177/1947603518809398
Schiavone A, Chiara P, Regno D, Mazzitelli G, Apolito RD, Corona K, Vasso M (2017) Good clinical results with autologous matrix-induced chondrogenesis (Amic) technique in large knee chondral defects. Knee Surg Sport Traumatol Arthrosc 26:1130–1136
Schneider U (2016) Controlled, randomized multicenter study to compare compatibility and safety of ChondroFiller liquid (cell free 2-component collagen gel) with microfracturing of patients with focal cartilage defects of the knee joint. Video J Orthop Surg 1:1–8
Shaikh N, Seah MKT, Khan WS (2017) Systematic review on the use of autologous matrix-induced chondrogenesis for the repair of articular cartilage defects in patients. World J Orthop 8:588–601
Sharma B, Fermanian S, Gibson M, Unterman S, Herzka DA, Cascio B, Coburn J, Hui AY, Marcus N, Gold GE, Elisseeff JH (2013) Human cartilage repair with a photoreactive adhesive-hydrogel composite. Sci Transl Med 5:1676
Shimozono Y, Yasui Y, Ross AW, Miyamoto W, Kennedy JG (2017) Scaffolds based therapy for osteochondral lesions of the talus: a systematic review. World J Orthop 8:798–808
Shive MS, Stanish WD, McCormack R, Forriol F, Mohtadi N, Pelet S, Desnoyers J, Méthot S, Vehik K, Restrepo A (2015) BST-CarGel® treatment maintains cartilage repair superiority over microfracture at 5 years in a multicenter randomized controlled trial. Cartilage 6:62–72
Siclari A, Mascaro G, Gentili C, Cancedda R, Boux E (2012) A cell-free scaffold-based cartilage repair provides improved function hyaline-like repair at one year. Clin Orthop Relat Res 470:910–919
Siclari A, Mascaro G, Gentili C, Kaps C, Cancedda R, Boux E (2014) Cartilage repair in the knee with subchondral drilling augmented with a platelet-rich plasma-immersed polymer-based implant. Knee Surg Sports Traumatol Arthrosc 22:1225–1234
Siclari A, Mascaro G, Kaps C, Boux E (2014) A 5-year follow-up after cartilage repair in the knee using a platelet-rich plasma-immersed polymer-based implant. Open Orthop J 8:346–354
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (minors): development and validation of a new instrument. ANZ J Surg 73:712–716
Sofu H, Camurcu Y, Ucpunar H, Ozcan S, Yurten H, Sahin V (2019) Clinical and radiographic outcomes of chitosan-glycerol phosphate/blood implant are similar with hyaluronic acid-based cell-free scaffold in the treatment of focal osteochondral lesions of the knee joint. Knee Surg Sports Traumatol Arthrosc 27:773–781
Solheim E, Hegna J, Inderhaug E (2017) Long-term clinical follow-up of microfracture versus mosaicplasty in articular cartilage defects of medial femoral condyle. Knee 24:1402–1407
Solheim E, Hegna J, Inderhaug E (2018) Long-term survival after microfracture and mosaicplasty for knee articular cartilage repair: a comparative study between two treatments cohorts. Cartilage. https://doi.org/10.1177/1947603518783482
Stanish WD, McCormack R, Forriol F, Mohtadi N, Pelet S, Desnoyers J, Restrepo A, Shive MS (2013) Novel scaffold-based BST-CarGel treatment results in superior cartilage repair compared with microfracture in a randomized controlled trial. J Bone Joint Surg Am 95:1640–1650
Steadman JR, Briggs KK, Rodrigo JJ, Kocher MS, Gill TJ, Rodkey WG (2003) Outcomes of microfracture for traumatic chondral defects of the knee: average 11-year follow-up. Arthroscopy 19:477–484
Steinwachs M, Cavalcanti N, Mauuva Venkatesh Reddy S, Werner C, Tschopp D, Choudur HN (2019) Arthroscopic and open treatment of cartilage lesions with BST-CARGEL scaffold and microfracture: a cohort study of consecutive patients. Knee 26:174–184
Wolf MT, Zhang H, Sharma B, Marcus NA, Pietzner U, Fickert S, Lueth A, Albers GHR, Elisseeff JH (2018) Two-year follow-Up and remodeling kinetics of ChonDux hydrogel for full-thickness cartilage defect repair in the knee. Cartilage. https://doi.org/10.1177/1947603518800547
Funding
The authors declare that there was no funding for this study.
Author information
Authors and Affiliations
Contributions
CBC, TRV and RA designed and implemented the systematic review protocol, CBC, TRV and RA collected, analyzed and interpreted the data collected, CBC, TRV and RA critically reviewed the scientific content of the manuscript, CBC, RA, JEM and RAS drafted the manuscript, and all authors (CBC, RA, TRV, DAL, JEM and RAS) have read, reviewed and given final approval for the version to be published.
Corresponding author
Ethics declarations
Conflict of interest
JEM and RAS are shareholders, and CBC, TRV, DAL and RAS are current employees of Stemmatters, Biotecnologia e Medicina Regenerativa SA. Stemmatters is currently developing a proprietary medical device to be used in the context of enhanced microfracture surgical treatment. Stemmatters is actively pursuing patents related to the content of the manuscript. This manuscript was not influenced by personal or financial relationship with Stemmatters or any other third party.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
da Cunha, C.B., Andrade, R., Veloso, T.R. et al. Enhanced microfracture using acellular scaffolds improves results after treatment of symptomatic focal grade III/IV knee cartilage lesions but current clinical evidence does not allow unequivocal recommendation. Knee Surg Sports Traumatol Arthrosc 28, 3245–3257 (2020). https://doi.org/10.1007/s00167-019-05832-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-019-05832-5