Abstract
Purpose
Post-traumatic stress disorder (PTSD) can affect family members of patients admitted to the intensive care unit (ICU). Easily accessible patient’s and relative’s information may help develop accurate risk stratification tools to direct relatives at higher risk of PTSD toward appropriate management.
Methods
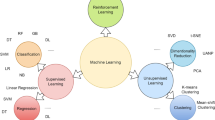
PTSD was measured 90 days after ICU discharge using validated instruments (Impact of Event Scale and Impact of Event Scale-Revised) in 2374 family members. Various supervised machine learning approaches were used to predict PTSD in family members and evaluated on an independent held-out test dataset. To better understand variables’ contributions to PTSD predicted probability, we used machine learning interpretability methods on the best predictive algorithm.
Results
Non-linear ensemble learning tree-based methods showed better predictive performances (Random Forest—area under curve, AUC = 0.73 [0.68–0.77] and XGBoost—AUC = 0.73 [0.69–0.78]) than regularized linear models, kernel-based models, or deep learning models. In the best performing algorithm, most important features that positively contributed to PTSD’s predicted probability were all non-modifiable factors, namely, lower patient’s age, longer duration of ICU stay, relative’s female sex, lower relative’s age, relative being a spouse/child, and patient’s death in ICU. A sensitivity analysis in bereaved relatives did not alter the algorithm’s predictive performance.
Conclusion
We propose a machine learning-based approach to predict PTSD in relatives of ICU patients at an individual level. In this model, PTSD is mostly influenced by non-modifiable factors.



Similar content being viewed by others
Data availability
Data are available on request to the corresponding author. Authorization from the steering committee will be required. The data collected for the study, including individual participant data (deidentified participant data) and a data dictionary defining each field in the set, will be made available in a web repository with publication, with investigator support. The proposal will be submitted to the steering committee and a data agreement will be signed.
References
Yehuda R (2002) Post-traumatic stress disorder. N Engl J Med 346:108–114. https://doi.org/10.1056/NEJMra012941
Azoulay E, Pochard F, Kentish-Barnes N et al (2005) Risk of post-traumatic stress symptoms in family members of intensive care unit patients. Am J Respir Crit Care Med 171:987–994. https://doi.org/10.1164/rccm.200409-1295OC
Jones C, Skirrow P, Griffiths RD et al (2004) Post-traumatic stress disorder-related symptoms in relatives of patients following intensive care. Intensive Care Med 30:456–460. https://doi.org/10.1007/s00134-003-2149-5
Wendlandt B, Ceppe A, Choudhury S et al (2018) Risk factors for post-traumatic stress disorder symptoms in surrogate decision-makers of patients with chronic critical illness. Ann Am Thorac Soc 15:1451–1458. https://doi.org/10.1513/AnnalsATS.201806-420OC
Herridge MS, Azoulay É (2023) Outcomes after critical illness. N Engl J Med 388:913–924. https://doi.org/10.1056/NEJMra2104669
Kentish-Barnes N, Chaize M, Seegers V et al (2015) Complicated grief after death of a relative in the intensive care unit. Eur Respir J 45:1341–1352. https://doi.org/10.1183/09031936.00160014
Siegel MD, Hayes E, Vanderwerker LC et al (2008) Psychiatric illness in the next of kin of patients who die in the intensive care unit. Crit Care Med 36:1722–1728. https://doi.org/10.1097/CCM.0b013e318174da72
Lautrette A, Darmon M, Megarbane B et al (2007) A communication strategy and brochure for relatives of patients dying in the ICU. N Engl J Med 356:469–478. https://doi.org/10.1056/NEJMoa063446
Jabre P, Belpomme V, Azoulay E et al (2013) Family presence during cardiopulmonary resuscitation. N Engl J Med 368:1008–1018. https://doi.org/10.1056/NEJMoa1203366
Kentish-Barnes N, Chevret S, Valade S et al (2022) A three-step support strategy for relatives of patients dying in the intensive care unit: a cluster randomised trial. Lancet 399:656–664. https://doi.org/10.1016/S0140-6736(21)02176-0
Azoulay E, Forel J, Vinatier I et al (2018) Questions to improve family-staff communication in the ICU: a randomized controlled trial. Intensive Care Med 44:1879–1887. https://doi.org/10.1007/s00134-018-5423-2
White DB, Angus DC, Shields A-M et al (2018) A randomized trial of a family-support intervention in intensive care units. N Engl J Med 378:2365–2375. https://doi.org/10.1056/NEJMoa1802637
Curtis JR, Treece PD, Nielsen EL et al (2016) Randomized trial of communication facilitators to reduce family distress and intensity of end-of-life care. Am J Respir Crit Care Med 193:154–162. https://doi.org/10.1164/rccm.201505-0900OC
Curtis JR, Back AL, Ford DW et al (2013) Effect of communication skills training for residents and nurse practitioners on quality of communication with patients with serious illness: a randomized trial. JAMA 310:2271–2281. https://doi.org/10.1001/jama.2013.282081
Kentish-Barnes N, Chevret S, Champigneulle B et al (2017) Effect of a condolence letter on grief symptoms among relatives of patients who died in the ICU: a randomized clinical trial. Intensive Care Med 43:473–484. https://doi.org/10.1007/s00134-016-4669-9
Carson SS, Cox CE, Wallenstein S et al (2016) Effect of palliative care-led meetings for families of patients with chronic critical illness: a randomized clinical trial. JAMA 316:51–62. https://doi.org/10.1001/jama.2016.8474
de Miranda S, Pochard F, Chaize M et al (2011) Postintensive care unit psychological burden in patients with chronic obstructive pulmonary disease and informal caregivers: A multicenter study. Crit Care Med 39(1):112–118. https://doi.org/10.1097/CCM.0b013e3181feb824
Ehooman F, Biard L, Lemiale V et al (2019) Long-term health-related quality of life of critically ill patients with haematological malignancies: a prospective observational multicenter study. Ann Intensive Care 9(1):2. https://doi.org/10.1186/s13613-018-0478-3
Azoulay E, Kouatchet A, Jaber S et al (2013) Noninvasive mechanical ventilation in patients having declined tracheal intubation. Intensive Care Med 39(2):292–301. https://doi.org/10.1007/s00134-012-2746-2
Azoulay E, Resche-Rigon M, Megarbane B et al (2022) Association of COVID-19 acute respiratory distress syndrome with symptoms of posttraumatic stress disorder in family members after ICU discharge. JAMA 327(11):1042–1050. https://doi.org/10.1001/jama.2022.2017
Kentish-Barnes N, Seegers V, Legriel S et al (2016) CAESAR: a new tool to assess relatives' experience of dying and death in the ICU. Intensive Care Med 42(6):995–1002. https://doi.org/10.1007/s00134-016-4260-4
Marx BP, Lee DJ, Norman SB et al (2022) Reliable and clinically significant change in the clinician-administered PTSD Scale for DSM-5 and PTSD Checklist for DSM-5 among male veterans. Psychol Assess 34:197–203. https://doi.org/10.1037/pas0001098
Creamer M, Bell R, Failla S (2003) Psychometric properties of the Impact of Event Scale—revised. Behav Res Ther 41:1489–1496. https://doi.org/10.1016/j.brat.2003.07.010
Hoge CW, Riviere LA, Wilk JE et al (2014) The prevalence of post-traumatic stress disorder (PTSD) in US combat soldiers: a head-to-head comparison of DSM-5 versus DSM-IV-TR symptom criteria with the PTSD checklist. Lancet Psychiatry 1:269–277. https://doi.org/10.1016/S2215-0366(14)70235-4
Witteveen AB, Bramsen I, Hovens JE, van der Ploeg HM (2005) Utility of the impact of event scale in screening for posttraumatic stress disorder. Psychol Rep 97:297–308. https://doi.org/10.2466/pr0.97.1.297-308
Collins GS, Reitsma JB, Altman DG, Moons KGM (2015) Transparent reporting of a multivariable prediction model for individual prognosis or diagnosis (TRIPOD): the TRIPOD statement. Ann Intern Med 162(1):55–63. https://doi.org/10.7326/M14-0697
Chen T, Guestrin C (2016) XGBoost: a scalable tree boosting system. In: Proceedings of the 22nd ACM SIGKDD International Conference on Knowledge Discovery and Data Mining. ACM, New York, NY, USA, pp 785–794
Breiman L (2001) Random forests. Mach Learn 45:5–32. https://doi.org/10.1023/A:1010933404324
Pedregosa F, Varoquaux G, Gramfort A et al (2011) Scikit-learn: machine learning in Python. J Mach Learn Res 12:2825–2830
Lundberg SM, Lee S-I (2017) A unified approach to interpreting model predictions. In: Guyon I, Luxburg UV, Bengio S et al (eds) Advances in neural information processing systems 30. Curran Associates Inc, pp 4765–4774
Lundberg SM, Erion G, Chen H et al (2020) From local explanations to global understanding with explainable AI for trees. Nat Mach Intell 2:2522–5839
Anderson WG, Arnold RM, Angus DC, Bryce CL (2008) Posttraumatic stress and complicated grief in family members of patients in the intensive care unit. J Gen Intern Med 23:1871–1876. https://doi.org/10.1007/s11606-008-0770-2
Cameron JI, Chu LM, Matte A et al (2016) One-year outcomes in caregivers of critically ill patients. N Engl J Med 374:1831–1841. https://doi.org/10.1056/NEJMoa1511160
Robert R, Le Gouge A, Kentish-Barnes N et al (2017) Terminal weaning or immediate extubation for withdrawing mechanical ventilation in critically ill patients (the ARREVE observational study). Intensive Care Med. https://doi.org/10.1007/s00134-017-4891-0
Probst DR, Gustin JL, Goodman LF et al (2016) ICU versus non-ICU hospital death: family member complicated grief, posttraumatic stress, and depressive symptoms. J Palliat Med 19:387–393. https://doi.org/10.1089/jpm.2015.0120
Nievergelt CM, Maihofer AX, Klengel T et al (2019) International meta-analysis of PTSD genome-wide association studies identifies sex- and ancestry-specific genetic risk loci. Nat Commun 10:4558. https://doi.org/10.1038/s41467-019-12576-w
The SUPPORT Principal Investigators (1995) A controlled trial to improve care for seriously ill hospitalized patients. The study to understand prognoses and preferences for outcomes and risks of treatments (SUPPORT). The SUPPORT Principal Investigators. JAMA 274:1591–1598
Nelson JE, Azoulay É (2019) Intensive care unit provision at the end of life: miles travelled, miles to go. Lancet Respir Med 7:560–562. https://doi.org/10.1016/S2213-2600(19)30168-7
Gerstel E, Engelberg RA, Koepsell T, Curtis JR (2008) Duration of withdrawal of life support in the intensive care unit and association with family satisfaction. Am J Respir Crit Care Med 178:798–804. https://doi.org/10.1164/rccm.200711-1617OC
Funding
The study sponsor is the French government. It had no role in the study design; the collection, analysis, interpretation of data; writing of the report; and in the decision to submit the paper for publication.
Author information
Authors and Affiliations
Contributions
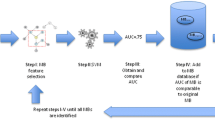
All authors have made significant contribution for this manuscript, to the study design; and interpretation of data for the work; all have also contributed to drafting the work or reviewing it critically for important intellectual content; all approved the final version to be published; all authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. EA, NKB, and FP are the study; PI, TD and ED are the methodologists dedicated to machine learning technologies. All authors have taken part to every single step of the development and validation of the algorithm. EA and ED directly accessed and verified the underlying data reported in the manuscript. All authors have full access to all the data in the study and accept responsibility to submit for publication. This manuscript has not been published elsewhere. However, as mentioned in the Methods and Fig. 1, the database was built using consecutive trials and cohort studies, each having been published.
Corresponding author
Ethics declarations
Conflicts of interest
EA reports support for the current manuscript from Programme Hospitalier de Recherche Clinique of the French Ministry of Health (PHRC) and ANR-RHU-5th Wave (RHU FAME 2021); outside the submitted work, grants from MSD-AVENIR and Alexion, and lecture honoraria from Pfizer, Alexion, and Sanofi. All other authors report no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dupont, T., Kentish-Barnes, N., Pochard, F. et al. Prediction of post-traumatic stress disorder in family members of ICU patients: a machine learning approach. Intensive Care Med 50, 114–124 (2024). https://doi.org/10.1007/s00134-023-07288-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-023-07288-1