Abstract
Purpose
To investigate which factors influence time to death in hospital in critically ill patients worldwide, including the possible impact of gross national income (GNI).
Methods
This was a pre-defined post hoc analysis of the Intensive Care Over Nations (ICON) database, which included 10,069 patients. For this sub-analysis, we included only the 2062 60-day in-hospital non-survivors (22.3 %) among the 9258 patients with available hospital mortality and length-of-stay data. We categorized these non-survivors into three groups according to the time of death after ICU admission: early (<5 days), intermediate (6–28 days) or late (>28 days).
Results
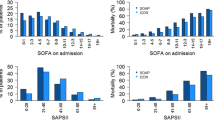
Time to death in hospital was early in 1068 of the 2062 non-survivors (52 %), intermediate in 808 (39 %), and late in 186 (9 %). Patients who died early had higher severity scores and were more likely to require mechanical ventilation on ICU admission, whereas those who died late were more likely to be older and to have had infection on ICU admission or during the ICU stay. Multilevel analysis indicated a stepwise increase in the risk of late or intermediate deaths according to increasing GNI. Patients admitted to ICUs in countries with high or upper-middle GNI were more likely to die late than those admitted to countries with low/lower-middle GNI [odds ratio (95 % confidence interval) 4.78 (1.94–11.76), p < 0.001, and 1.64 (1.10–2.45), p = 0.02, respectively].
Conclusions
Duration of hospital stay prior to death in critically ill patients is longer in older patients, surgical patients, and patients with infection. GNI is a major determinant of time to death in hospital in these patients. These observations may have important organizational and ethical implications.

Similar content being viewed by others
References
Brinkman S, Bakhshi-Raiez F, Abu-Hanna A, de Jonge E, de Keizer NF (2013) Determinants of mortality after hospital discharge in ICU patients: literature review and Dutch cohort study. Crit Care Med 41:1237–1251
Sakr Y, Lobo SM, Moreno RP, Gerlach H, Ranieri VM, Michalopoulos A, Vincent JL (2012) Patterns and early evolution of organ failure in the intensive care unit and their relation to outcome. Crit Care 16:R222
Daviaud F, Grimaldi D, Dechartres A, Charpentier J, Geri G, Marin N, Chiche JD, Cariou A, Mira JP, Pène F (2015) Timing and causes of death in septic shock. Ann Intensive Care 5:16
Mayr VD, Dunser MW, Greil V, Jochberger S, Luckner G, Ulmer H, Friesenecker BE, Takala J, Hasibeder WR (2006) Causes of death and determinants of outcome in critically ill patients. Crit Care 10:R154
Tsai TC, Jha AK (2014) Hospital consolidation, competition, and quality: is bigger necessarily better? JAMA 312:29–30
Shortell SM, Zimmerman JE, Gillies RR, Duffy J, Devers KJ, Rousseau DM, Knaus WA (1992) Continuously improving patient care: practical lessons and an assessment tool from the National ICU Study. QRB Qual Rev Bull 18:150–155
Sakr Y, Moreira CL, Rhodes A, Ferguson ND, Kleinpell R, Pickkers P, Kuiper MA, Lipman J, Vincent JL (2015) The impact of hospital and ICU organizational factors on outcome in critically ill patients: Results from the extended prevalence of infection in intensive care study. Crit Care Med 43:519–526
Vincent JL, Marshall JC, Namendys-Silva SA, Francois B, Martin-Loeches I, Lipman J, Reinhart K, Antonelli M, Pickkers P et al (2014) Assessment of the worldwide burden of critical illness: the intensive care over nations (ICON) audit. Lancet Respir Med 2:380–386
Le Gall JR, Lemeshow S, Saulnier F (1993) A new Simplified Acute Physiology Score (SAPS II) based on a European/North American multicenter study. JAMA 270:2957–2963
Knaus WA, Draper EA, Wagner DP, Zimmerman JE (1985) APACHE II: a severity of disease classification system. Crit Care Med 13:818–829
Vincent JL, Moreno R, Takala J, Willatts S, De Mendonca A, Bruining H, Reinhart CK, Suter PM, Thijs LG (1996) The SOFA (Sepsis-related Organ Failure Assessment) score to describe organ dysfunction/failure. On behalf of the Working Group on Sepsis-Related Problems of the European Society of Intensive Care Medicine. Intensive Care Med 22:707–710
Calandra T, Cohen J (2005) The international sepsis forum consensus conference on definitions of infection in the intensive care unit. Crit Care Med 33:1538–1548
The World Bank. GNI per capita, Atlas method (current US$). Available at: http://data.worldbank.org/indicator/NY.GNP.PCAP.CD. Accessed Jan 2012
Iwashyna TJ, Hodgson CL, Pilcher D, Bailey M, van Lint A, Chavan S, Bellomo R (2016) Timing of onset and burden of persistent critical illness in Australia and New Zealand: a retrospective, population-based, observational study. Lancet Respir Med 4:566–573
Gomersall CD (2010) Critical care in the developing world—a challenge for us all. Crit Care 14:131
Bagshaw SM, Stelfox HT, McDermid RC, Rolfson DB, Tsuyuki RT, Baig N, Artiuch B, Ibrahim Q, Stollery DE et al (2014) Association between frailty and short- and long-term outcomes among critically ill patients: a multicentre prospective cohort study. CMAJ 186:E95–102
Santamaria JD, Duke GJ, Pilcher DV, Cooper DJ, Moran J, Bellomo R (2015) The timing of discharge from the intensive care unit and subsequent mortality. A prospective, multicenter study. Am J Respir Crit Care Med 191:1033–1039
Watters DA, Hollands MJ, Gruen RL, Maoate K, Perndt H, McDougall RJ, Morriss WW, Tangi V, Casey KM, McQueen KA (2015) Perioperative mortality rate (POMR): a global indicator of access to safe surgery and anaesthesia. World J Surg 39:856–864
Curtis JR, Vincent JL (2010) Ethics and end-of-life care for adults in the intensive care unit. Lancet 376:1347–1353
Acknowledgments
The authors would like to thank Hassane Njimi for his help with the statistical analyses.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest to declare.
Additional information
Take-home message: Duration of hospital stay prior to death in critically ill patients is longer in older patients, surgical patients, and patients with infection. Gross national income is a major determinant of time to death in these patients.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Martin-Loeches, I., Wunderink, R.G., Nanchal, R. et al. Determinants of time to death in hospital in critically ill patients around the world. Intensive Care Med 42, 1454–1460 (2016). https://doi.org/10.1007/s00134-016-4479-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-016-4479-0