Abstract
Aims/hypothesis
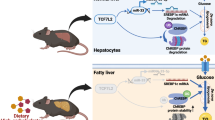
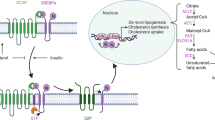
Hyperglucagonaemia-stimulated hepatic glucose production (HGP) contributes to hyperglycaemia during type 2 diabetes. A better understanding of glucagon action is important to enable efficient therapies to be developed for the treatment of diabetes. Here, we aimed to investigate the role of p38 MAPK family members in glucagon-induced HGP and determine the underlying mechanisms by which p38 MAPK regulates glucagon action.
Methods
p38α, β, γ and δ MAPK siRNAs were transfected into primary hepatocytes, followed by measurement of glucagon-induced HGP. Adeno-associated virus serotype 8 carrying p38α MAPK short hairpin RNA (shRNA) was injected into liver-specific Foxo1 knockout, liver-specific Irs1/Irs2 double knockout and Foxo1S273D knockin mice. Foxo1S273A knockin mice were fed a high-fat diet for 10 weeks. Pyruvate tolerance tests, glucose tolerance tests, glucagon tolerance tests and insulin tolerance tests were carried out in mice, liver gene expression profiles were analysed and serum triglyceride, insulin and cholesterol levels were measured. Phosphorylation of forkhead box protein O1 (FOXO1) by p38α MAPK in vitro was analysed by LC–MS.
Results
We found that p38α MAPK, but not the other p38 isoforms, stimulates FOXO1-S273 phosphorylation and increases FOXO1 protein stability, promoting HGP in response to glucagon stimulation. In hepatocytes and mouse models, inhibition of p38α MAPK blocked FOXO1-S273 phosphorylation, decreased FOXO1 levels and significantly impaired glucagon- and fasting-induced HGP. However, the effect of p38α MAPK inhibition on HGP was abolished by FOXO1 deficiency or a Foxo1 point mutation at position 273 from serine to aspartic acid (Foxo1S273D) in both hepatocytes and mice. Moreover, an alanine mutation at position 273 (Foxo1S273A) decreased glucose production, improved glucose tolerance and increased insulin sensitivity in diet-induced obese mice. Finally, we found that glucagon activates p38α through exchange protein activated by cAMP 2 (EPAC2) signalling in hepatocytes.
Conclusions/interpretation
This study found that p38α MAPK stimulates FOXO1-S273 phosphorylation to mediate the action of glucagon on glucose homeostasis in both health and disease. The glucagon-induced EPAC2–p38α MAPK–pFOXO1-S273 signalling pathway is a potential therapeutic target for the treatment of type 2 diabetes.
Graphical abstract








Similar content being viewed by others
Abbreviations
- AAV8:
-
Adeno-associated virus serotype 8
- AMPK:
-
AMP-activated protein kinase
- ATGL:
-
Adipose triglyceride lipase
- CaMKII:
-
Calcium calmodulin-dependent kinase II
- CREB:
-
cAMP-responsive element-binding protein
- DIO:
-
Diet-induced obese
- DKO:
-
Liver-specific Irs1 and Irs2 double knockout
- EPAC2:
-
Exchange protein activated by cAMP 2
- FAO:
-
Fatty acid oxidation
- FOXO1:
-
Forkhead box protein O1
- G6PC:
-
Glucose-6-phosphatase
- HFD:
-
High-fat diet
- HGP:
-
Hepatic glucose production
- HMOX1:
-
Heme oxygenase 1
- INSP3R1:
-
Inositol triphosphate receptor 1
- PCK:
-
Phosphoenolpyruvate carboxykinase
- PKA:
-
Protein kinase A
- pp38:
-
p38 phosphorylated at T180/Y182
- shRNA:
-
Short hairpin RNA
- t-FOXO1:
-
Total FOXO1
- TKO:
-
Liver-specific Irs1, Irs2 and Foxo1 triple knockout
- WT:
-
Wild-type
References
D’alessio D (2011) The role of dysregulated glucagon secretion in type 2 diabetes. Diabetes Obes Metab 13:126–132. https://doi.org/10.1111/j.1463-1326.2011.01449.x
Magnusson I, Rothman D, Katz L, Shulman R, Shulman G (1992) Increased rate of gluconeogenesis in type II diabetes mellitus. A 13C nuclear magnetic resonance study. J Clin Investig 90(4):1323–1327. https://doi.org/10.1172/JCI115997
Unger RH, Cherrington AD (2012) Glucagonocentric restructuring of diabetes: a pathophysiologic and therapeutic makeover. J Clin Investig 122(1):4–12. https://doi.org/10.1172/JCI60016
Haeusler RA, Kaestner KH, Accili DJJoBC (2010) FoxOs function synergistically to promote glucose production. J Biol Chem 285(46):35245–35248. https://doi.org/10.1074/jbc.C110.175851
Zhang K, Li L, Qi Y et al (2012) Hepatic suppression of Foxo1 and Foxo3 causes hypoglycemia and hyperlipidemia in mice. Endocrinology 153(2):631–646. https://doi.org/10.1210/en.2011-1527
Matsumoto M, Pocai A, Rossetti L, DePinho RA, Accili D (2007) Impaired regulation of hepatic glucose production in mice lacking the forkhead transcription factor Foxo1 in liver. Cell Metab 6(3):208–216. https://doi.org/10.1016/j.cmet.2007.08.006
Koo S-H, Flechner L, Qi L et al (2005) The CREB coactivator TORC2 is a key regulator of fasting glucose metabolism. Nature 437(7062):1109–1114. https://doi.org/10.1038/nature03967
Xu W, Kasper LH, Lerach S, Jeevan T, Brindle PK (2007) Individual CREB-target genes dictate usage of distinct cAMP-responsive coactivation mechanisms. EMBO J 26(12):2890–2903. https://doi.org/10.1038/sj.emboj.7601734
Wu Y, Pan Q, Yan H et al (2018) Novel mechanism of Foxo1 phosphorylation in glucagon signaling in control of glucose homeostasis. Diabetes 67(11):2167–2182. https://doi.org/10.2337/db18-0674
Johnson GL, Lapadat R (2002) Mitogen-activated protein kinase pathways mediated by ERK, JNK, and p38 protein kinases. Science 298(5600):1911–1912. https://doi.org/10.1126/science.1072682
Ono K, Han J (2000) The p38 signal transduction pathway activation and function. Cell Signal 12(1):1–13. https://doi.org/10.1016/S0898-6568(99)00071-6
Cuenda A, Sanz-Ezquerro JJ (2017) P38γ and p38δ: from spectators to key physiological players. Trends Biochem Sci 42(6):431–442. https://doi.org/10.1016/j.tibs.2017.02.008
Raingeaud J, Whitmarsh AJ, Barrett T, Derijard B, Davis RJ (1996) MKK3-and MKK6-regulated gene expression is mediated by the p38 mitogen-activated protein kinase signal transduction pathway. Mol Cell Biol 16(3):1247–1255. https://doi.org/10.1128/MCB.16.3.1247
Cao W, Collins QF, Becker TC et al (2005) p38 mitogen-activated protein kinase plays a stimulatory role in hepatic gluconeogenesis. J Biol Chem 280(52):42731–42737. https://doi.org/10.1074/jbc.M506223200
Ozcan L, Wong CC, Li G et al (2012) Calcium signaling through CaMKII regulates hepatic glucose production in fasting and obesity. Cell Metab 15(5):739–751. https://doi.org/10.1016/j.cmet.2012.03.002
Asada S, Daitoku H, Matsuzaki H et al (2007) Mitogen-activated protein kinases, Erk and p38, phosphorylate and regulate Foxo1. Cell Signal 19(3):519–527. https://doi.org/10.1016/j.cellsig.2006.08.015
Dong XC, Copps KD, Guo S et al (2008) Inactivation of hepatic Foxo1 by insulin signaling is required for adaptive nutrient homeostasis and endocrine growth regulation. Cell Metab 8(1):65–76. https://doi.org/10.1016/j.cmet.2008.06.006
Yan H, Yang W, Zhou F et al (2019) Estrogen improves insulin sensitivity and suppresses gluconeogenesis via the transcription factor Foxo1. Diabetes 68(2):291–304. https://doi.org/10.2337/db18-0638
Guo X, Li X, Yang W et al (2021) Metformin targets Foxo1 to control glucose homeostasis. Biomolecules 11(6):873. https://doi.org/10.3390/biom11060873
Longuet C, Sinclair EM, Maida A et al (2008) The glucagon receptor is required for the adaptive metabolic response to fasting. Cell Metab 8(5):359–371. https://doi.org/10.1016/j.cmet.2008.09.008
Cheng X, Ji Z, Tsalkova T, Mei F (2008) Epac and PKA: a tale of two intracellular cAMP receptors. Acta Biochim Biophys Sin 40(7):651–662. https://doi.org/10.1111/j.1745-7270.2008.00438.x
Jiang G, Zhang BB (2003) Glucagon and regulation of glucose metabolism. Am J Physiol Endocrinol Metab 284(4):E671–E678. https://doi.org/10.1152/ajpendo.00492.2002
Jing Y, Liu W, Cao H et al (2015) Hepatic p38α regulates gluconeogenesis by suppressing AMPK. J Hepatol 62(6):1319–1327. https://doi.org/10.1016/j.jhep.2014.12.032
Wang Y, Li G, Goode J et al (2012) Inositol-1, 4, 5-trisphosphate receptor regulates hepatic gluconeogenesis in fasting and diabetes. Nature 485(7396):128–132. https://doi.org/10.1038/nature10988
Marik PE, Bellomo R (2013) Stress hyperglycemia: an essential survival response! Crit Care 17(2):1–7. https://doi.org/10.1186/cc12514
Qing H, Desrouleaux R, Israni-Winger K et al (2020) Origin and function of stress-induced IL-6 in murine models. Cell 182(2):372–387. https://doi.org/10.1016/j.cell.2020.05.054. (e314)
Canovas B, Nebreda AR (2021) Diversity and versatility of p38 kinase signalling in health and disease. Nat Rev Mol Cell Biol 22(5):346–366. https://doi.org/10.1038/s41580-020-00322-w
Huang C-C, You J-L, Wu M-Y, Hsu K-S (2004) Rap1-induced p38 mitogen-activated protein kinase activation facilitates AMPA receptor trafficking via the GDI· Rab5 complex: potential role in (S)-3, 5-dihydroxyphenylglycine-induced long term depression. J Biol Chem 279(13):12286–12292. https://doi.org/10.1074/jbc.M312868200
Zhang W-S, Pan A, Zhang X et al (2019) Inactivation of NF-κB2 (p52) restrains hepatic glucagon response via preserving PDE4B induction. Nat Commun 10(1):1–10. https://doi.org/10.1038/s41467-019-12351-x
Ke B, Zhao Z, Ye X et al (2015) Inactivation of NF-κB p65 (RelA) in liver improves insulin sensitivity and inhibits cAMP/PKA pathway. Diabetes 64(10):3355–3362. https://doi.org/10.2337/db15-0242
Yan J, Mei FC, Cheng H et al (2013) Enhanced leptin sensitivity, reduced adiposity, and improved glucose homeostasis in mice lacking exchange protein directly activated by cyclic AMP isoform 1. Mol Cell Biol 33(5):918–926. https://doi.org/10.1128/MCB.01227-12
Rena G, Guo S, Cichy SC, Unterman TG, Cohen P (1999) Phosphorylation of the transcription factor forkhead family member FKHR by protein kinase B. J Biol Chem 274(24):17179–17183. https://doi.org/10.1074/jbc.274.24.17179
Matsuzaki H, Daitoku H, Hatta M, Tanaka K, Fukamizu A (2003) Insulin-induced phosphorylation of FKHR (Foxo1) targets to proteasomal degradation. Proc Natl Acad Sci 100(20):11285–11290. https://doi.org/10.1073/pnas.1934283100
Biggs WH III, Meisenhelder J, Hunter T, Cavenee WK, Arden KC (1999) Protein kinase B/Akt-mediated phosphorylation promotes nuclear exclusion of the winged helix transcription factor FKHR1. Proc Natl Acad Sci 96(13):7421–7426. https://doi.org/10.1073/pnas.96.13.7421
Saline M, Badertscher L, Wolter M et al (2019) AMPK and AKT protein kinases hierarchically phosphorylate the N-terminus of the FOXO1 transcription factor, modulating interactions with 14-3-3 proteins. J Biol Chem 294(35):13106–13116. https://doi.org/10.1074/jbc.RA119.008649
Yun H, Park S, Kim MJ et al (2014) AMP-activated protein kinase mediates the antioxidant effects of resveratrol through regulation of the transcription factor FoxO1. FEBS J 281(19):4421–4438. https://doi.org/10.1111/febs.12949
Stöhr O, Tao R, Miao J, Copps KD, White MF (2021) FoxO1 suppresses Fgf21 during hepatic insulin resistance to impair peripheral glucose utilization and acute cold tolerance. Cell Rep 34(12):108893. https://doi.org/10.1016/j.celrep.2021.108893
Nakae J, Cao Y, Oki M et al (2008) Forkhead transcription factor FoxO1 in adipose tissue regulates energy storage and expenditure. Diabetes 57(3):563–576. https://doi.org/10.2337/db07-0698
Johanns M, Lai Y-C, Hsu M-F et al (2016) AMPK antagonizes hepatic glucagon-stimulated cyclic AMP signalling via phosphorylation-induced activation of cyclic nucleotide phosphodiesterase 4B. Nat Commun 7:10856. https://doi.org/10.1038/ncomms10856
Kim J, Okamoto H, Huang Z et al (2017) Amino acid transporter Slc38a5 controls glucagon receptor inhibition-induced pancreatic α cell hyperplasia in mice. Cell Metab 25(6):1348–1361. https://doi.org/10.1016/j.cmet.2017.05.006. (e1348)
Perry RJ, Zhang D, Guerra MT et al (2020) Glucagon stimulates gluconeogenesis by INSP3R1-mediated hepatic lipolysis. Nature 579(7798):279–283. https://doi.org/10.1038/s41586-020-2074-6
Perry RJ, Camporez J-PG, Kursawe R et al (2015) Hepatic acetyl CoA links adipose tissue inflammation to hepatic insulin resistance and type 2 diabetes. Cell 160(4):745–758. https://doi.org/10.1016/j.cell.2015.01.012
Liu W, Sun C, Yan Y et al (2022) Hepatic P38 activation modulates systemic metabolism through fgf21-mediated interorgan communication. Diabetes 71(1):60–72. https://doi.org/10.2337/db21-0240
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Acknowledgements
The authors thank L. Li (Proteomics Service Center, University of Texas Health Science Center, Houston. TX, USA) for help in the analysis of the LC–MS/MS data.
Data availability
All data from this article are available from the corresponding authors on request.
Funding
This work was supported by National Institutes of Health grants (R01 DK095118, R01 DK120968, and R01 DK124588), an ADA Career Development Award (1-15-CD-09), faculty start-up funds from Texas A&M University Health Science Center and AgriLife Research, and an USDA National Institute of Food and Agriculture grant (Hatch 1010958) to SG (PI). SG is the recipient of the 2015 ADA Research Excellence Thomas R. Lee Award and is a 2021 Presidential Impact Fellow at Texas A&M University.
Authors’ relationships and activities
The authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Contribution statement
SG conceived the hypothesis, designed the experiments, performed the data analyses and wrote the manuscript. WY designed and conducted the experiments, performed the data analyses and wrote the manuscript. WL conducted the experiments. QP and ZS helped design the study, performed the animal studies, analysed the data and assisted in the preparation of the manuscript. XL, WA and WJ performed the animal studies and assisted in the preparation of the manuscript.. WL, XL, WA, QP, ZS and WJ critically reviewed the manuscript. All authors approved the final version of the manuscript. SG is the guarantor of this work and, as such, had full access to all the data in the study and takes responsibility for the integrity of the data and accuracy of the data analysis.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yang, W., Liao, W., Li, X. et al. Hepatic p38α MAPK controls gluconeogenesis via FOXO1 phosphorylation at S273 during glucagon signalling in mice. Diabetologia 66, 1322–1339 (2023). https://doi.org/10.1007/s00125-023-05916-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-023-05916-5