Abstract
Purpose
Proliferating cell nuclear antigen-associated factor (PAF) is involved in cancer cell growth and associated with cell death induced by ultraviolet (UV) radiation. However, the contribution of PAF to radiotherapy sensitivity in non-small cell lung cancer (NSCLC) is unknown. The aim of this study was to investigate the relationship between PAF expression and radiotherapy response in NSCLC.
Methods
Associations between PAF expression and patient survival outcomes were evaluated using publicly available online gene expression datasets. RNA interference was performed to knockdown PAF expression in the NSCLC cells. The effects of PAF knockdown on cell proliferation, migration, apoptosis, DNA damage, and activation of MEK/ERK and Wnt/β-catenin signaling pathways following X‑ray irradiation were evaluated in vitro.
Results
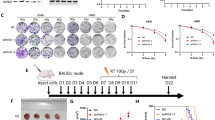
PAF was found to be overexpressed in lung cancer tissues compared with normal samples, and elevated PAF expression was significantly correlated with inferior patient survival. In vitro, knockdown of PAF inhibited cell proliferation, cell apoptosis, and migration induced by X‑ray irradiation. Moreover, X‑ray-induced intracellular DNA strand damage was more obvious following PAF knockdown. Additionally, PAF knockdown inhibited activation of the MEK/ERK and Wnt/β-catenin signaling pathways in X‑ray-irradiated A549 cells.
Conclusion
These data demonstrate that reduced expression of PAF enhances radiosensitivity in NSCLC cells. Mechanistically, inhibition of the MEK/ERK and Wnt/β-catenin signaling pathways caused by PAF interference may lead to impaired cell function and enhance sensitivity to X‑rays. Targeting PAF may therefore serve as a potential therapeutic strategy to increase the efficiency of radiotherapy in NSCLC patients, ultimately improving patient survival.





Similar content being viewed by others
Change history
29 January 2021
In the PDF the order of the email addresses of the corresponding authors was changed.
References
Chen W, Zheng R, Baade PD et al (2016) Cancer statistics in China, 2015. CA Cancer J Clin 66(2):115–132
Siegel RL, Miller KD, Jemal A (2020) Cancer statistics, 2020. CA Cancer J Clin 70(1):7–30
Miller KD, Nogueira L, Mariotto AB et al (2019) Cancer treatment and survivorship statistics, 2019. CA Cancer J Clin 69(5):363–385
Triggiani L, Colosini A, Buglione M et al (2018) Exploring the role of enzalutamide in combination with radiation therapy: an in vitro study. Anticancer Res 38(6):3487–3492
Changizi V, Bahrami M, Esfahani M et al (2017) Prevention of γ‑radiation-induced DNA damage in human lymphocytes using a serine-magnesium sulfate mixture. Sultan Qaboos Univ Med J 17(2):e162–e167
Murad H, Alghamian Y, Aljapawe A et al (2018) Effects of ionizing radiation on the viability and proliferative behavior of the human glioblastoma T98G cell line. BMC Res Notes 11(1):330
Skrzypski M, Jassem J (2018) Consolidation systemic treatment after radiochemotherapy for unresectable stage III non-small cell lung cancer. Cancer Treat Rev 66:114–121
Nagata Y, Kimura T (2018) Stereotactic body radiotherapy (SBRT) for stage I lung cancer. Jpn J Clin Oncol 48(5):405–409
Ricardi U, Badellino S, Filippi AR (2015) Stereotactic body radiotherapy for early stage lung cancer: history and updated role. Lung Cancer 90(3):388–396
Maier P, Hartmann L, Wenz F et al (2016) Cellular pathways in response to ionizing radiation and their targetability for tumor radiosensitization. Int J Mol Sci 17(1):102
Yu P, Huang B, Shen M et al (2001) p15PAF, a novel PCNA associated factor with increased expression in tumor tissues. Oncogene 20(4):484–489
Zhang T, Guo J, Gu J et al (2019) KIAA0101 is a novel transcriptional target of FoxM1 and is involved in the regulation of hepatocellular carcinoma microvascular invasion by regulating epithelial-mesenchymal transition. J Cancer 10(15):3501–3516
Kato T, Daigo Y, Aragaki M et al (2012) Overexpression of KIAA0101 predicts poor prognosis in primary lung cancer patients. Lung Cancer 75(1):110–118
Wang X, Jung Y, Jun S et al (2016) PAF-Wnt signaling-induced cell plasticity is required for maintenance of breast cancer cell stemness. Nat Commun 7(1):10633
Jin C, Liu Z, Li Y et al (2018) PCNA-associated factor P15PAF, targeted by FOXM1, predicts poor prognosis in high-grade serous ovarian cancer patients. Int J Cancer 143(11):2973–2984
Turchi L, Fareh M, Aberdam E et al (2009) ATF3 and p15PAF are novel gatekeepers of genomic integrity upon UV stress. Cell Death Differ 16(5):728–737
Struchkov VA, Demidova NI, Strazhevskaia NB (1997) Primary gamma-induced unrepairable DNA damage in HeLa cells. Biull Eksp Biol Med 124(7):53–56
Yan R, Zhu K, Dang C et al (2016) Paf15 expression correlates with rectal cancer prognosis, cell proliferation and radiation response. Oncotarget 7(25):38750–38761
Chandrashekar DS, Bashel B, Balasubramanya S et al (2017) UALCAN: a portal for facilitating tumor subgroup gene expression and survival analyses. Neoplasia 19(8):649–658
Gyorffy B, Surowiak P, Budczies J et al (2013) Online survival analysis software to assess the prognostic value of biomarkers using transcriptomic data in non-small-cell lung cancer. PLoS One 8(12):e82241
Steel GG, Deacon JM, Duchesne GM et al (1987) The dose-rate effect in human tumour cells. Radiother Oncol 9(4):299–310
Hwang JH, Joo JC, Kim DJ et al (2016) Cordycepin promotes apoptosis by modulating the ERK-JNK signaling pathway via DUSP5 in renal cancer cells. Am J Cancer Res 6(8):1758–1771
Nusse R, Clevers H (2017) Wnt/beta-catenin signaling, disease, and emerging therapeutic modalities. Cell 169(6):985–999
Bradley JD, Paulus R, Komaki R et al (2015) Standard-dose versus high-dose conformal radiotherapy with concurrent and consolidation carboplatin plus paclitaxel with or without cetuximab for patients with stage IIIA or IIIB non-small-cell lung cancer (RTOG 0617): a randomised, two-by-two factorial phase 3 study. Lancet Oncol 16(2):187–199
Emanuele MJ, Ciccia A, Elia AE et al (2011) Proliferating cell nuclear antigen (PCNA)-associated KIAA0101/PAF15 protein is a cell cycle-regulated anaphase-promoting complex/cyclosome substrate. Proc Natl Acad Sci USA 108(24):9845–9850
Povlsen LK, Beli P, Wagner SA et al (2012) Systems-wide analysis of ubiquitylation dynamics reveals a key role for PAF15 ubiquitylation in DNA-damage bypass. Nat Cell Biol 14(10):1089–1098
Li G, Luna C, Gonzalez P (2016) miR-183 inhibits UV-induced DNA damage repair in human trabecular meshwork cells by targeting of KIAA0101. Invest Ophthalmol Vis Sci 57(4):2178–2186
Ong D, Hu B, Ho YW et al (2017) PAF promotes stemness and radioresistance of glioma stem cells. Proc Natl Acad Sci USA 114(43):E9086–E9095
Brunner TB, Hahn SM, McKenna WG et al (2004) Radiation sensitization by inhibition of activated Ras. Strahlenther Onkol 180(11):731–740
Marvaso G, Barone A, Amodio N et al (2014) Sphingosine analog fingolimod (FTY720) increases radiation sensitivity of human breast cancer cells in vitro. Cancer Biol Ther 15(6):797–805
Wang Q, Wang Y, Li Y et al (2013) NS5ATP9 contributes to inhibition of cell proliferation by hepatitis C virus (HCV) nonstructural protein 5A (NS5A) via MEK/extracellular signal regulated kinase (ERK) pathway. Int J Mol Sci 14(5):10539–10551
Chen K, Chen L, Li L et al (2020) A positive feedback loop between Wnt/beta-catenin signaling and hTERT regulates the cancer stem cell-like traits in radioresistant nasopharyngeal carcinoma cells. J Cell Biochem. https://doi.org/10.1002/jcb.29681
Wu D, Li L, Yan W (2016) Knockdown of TC‑1 enhances radiosensitivity of non-small cell lung cancer via the Wnt/beta-catenin pathway. Biol Open 5(4):492–498
Wen J, Xiong K, Aili A et al (2020) PEX5, a novel target of microRNA-31-5p, increases radioresistance in hepatocellular carcinoma by activating Wnt/beta-catenin signaling and homologous recombination. Theranostics 10(12):5322–5340
Funding
This research project was supported by the National Natural Science Foundation of China (Grant No. 81402540; Grant No. 81672972) and the Medical and Health Science Foundation of Zhejiang Province (Grant No. 2018255396).
Author information
Authors and Affiliations
Contributions
Conception and design: M Chen; administrative support: P Zhang; provision of study materials: X Hu; data analysis and interpretation: Y Chen, Y Jin; manuscript writing: all authors; final approval of manuscript: all authors.
Corresponding authors
Ethics declarations
Conflict of interest
Y. Chen, Y. Jin, H. Ying, P. Zhang, M. Chen, and X. Hu declare that they have no competing interests.
Caption Electronic Supplementary Material
66_2020_1708_MOESM1_ESM.pdf
Supplementary Fig.1 Knockdown of PAF in H358 cells inhibits cell proliferation and enhances cell apoptosis in response to radiation.
Rights and permissions
About this article
Cite this article
Chen, Y., Jin, Y., Ying, H. et al. Synergistic effect of PAF inhibition and X-ray irradiation in non-small cell lung cancer cells. Strahlenther Onkol 197, 343–352 (2021). https://doi.org/10.1007/s00066-020-01708-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-020-01708-7