Abstract
Objectives
To analyse the age, period and cohort effects on the mean body mass index (BMI) and obesity over the past two decades in Estonia.
Methods
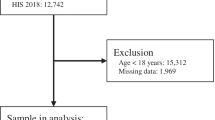
Study used data from nationally representative repeated cross-sectional surveys on 11,547 men and 16,298 women from 1996 to 2018. The independent effects of age, period and cohort on predicted mean BMI and probability of obesity (BMI ≥ 30 kg/m2) were modelled using hierarchical age–period–cohort analysis.
Results
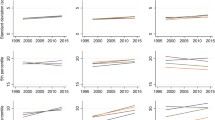
Curvilinear association between age and mean BMI was found for men, whereas the increase in mean BMI was almost linear for women. The predicted mean BMI for 40-year-old men had increased by 6% and probability of obesity by 1.8 times over 1996–2018; the period effects were slightly smaller for women. Men from the 1970s birth cohort had higher mean BMI compared to the average, whereas no significant cohort effects were found for obesity outcome.
Conclusions
Population-level BMI changes in Estonia during 1996–2018 were mostly driven by period rather than cohort-specific changes.


Similar content being viewed by others
References
Aasvee K, Rasmussen M, Kelly C, Kurvinen E, Giacchi MV, Ahluwalia N (2015) Validity of self-reported height and weight for estimating prevalence of overweight among Estonian adolescents: the Health Behaviour in School-aged Children study. BMC Res Notes 8(606):6. https://doi.org/10.1186/s13104-015-1587-9
Allman-Farinelli MA, Chey T, Bauman AE, Gill T, James WP (2008) Age, period and birth cohort effects on prevalence of overweight and obesity in Australian adults from 1990 to 2000. Eur J Clin Nutr 62:898–907. https://doi.org/10.1038/sj.ejcn.1602769
An R, Xiang X (2016) Age–period–cohort analyses of obesity prevalence in US adults. Public Health 141:163–169. https://doi.org/10.1016/j.puhe.2016.09.021
Bell A, Jones K (2014) Don’t birth cohorts matter? A commentary and simulation exercise on Reither, Hauser, and Yang’s (2009) age–period–cohort study of obesity. Soc Sci Med 101:176–180. https://doi.org/10.1016/j.socscimed.2013.09.004
Bell A, Jones K (2018) The hierarchical age–period–cohort model: Why does it find the results that it finds? Qual Quant 52:783–799. https://doi.org/10.1007/s11135-017-0488-5
Benziger CP, Roth GA, Moran AE (2016) The Global Burden of Disease Study and the preventable burden of NCD. Glob Heart 11:393–397. https://doi.org/10.1016/j.gheart.2016.10.024
Bowling A (2005) Mode of questionnaire administration can have serious effects on data quality. J Public Health-UK 27:281–291. https://doi.org/10.1093/pubmed/fdi031
Brixiova Z, Vartia L, Wörgötter A (2010) Capital flows and the boom-bust cycle: the case of Estonia. Econ Syst 34:55–72. https://doi.org/10.1016/j.ecosys.2009.11.002
Centers for Disease Control and Prevention (2018) Adult obesity causes & consequences. https://www.cdc.gov/obesity/adult/causes.html. Accessed 7 Feb 2020
Clarke P, O’Malley PM, Johnston LD, Schulenberg JE (2009) Social disparities in BMI trajectories across adulthood by gender, race/ethnicity and lifetime socio-economic position: 1986–2004. Int J Epidemiol 38:499–509. https://doi.org/10.1093/ije/dyn214
Courtemanche CJ, Pinkston JC, Ruhm CJ, Wehby GL (2016) Can Changing economic factors explain the rise in obesity? South Econ J 82:1266–1310. https://doi.org/10.1002/soej.12130
Diouf I, Charles MA, Ducimetiere P, Basdevant A, Eschwege E, Heude B (2010) Evolution of obesity prevalence in France: an age–period–cohort analysis. Epidemiology 21:360–365. https://doi.org/10.1097/ede.0b013e3181d5bff5
Haregu TN, Mohamed SF, Muthuri S, Khayeka-Wandabwa C, Kyobutungi C (2018) Body mass index and wealth index: positively correlated indicators of health and wealth inequalities in Nairobi slums. Glob Health Epidemiol Genom 3:e11–e11. https://doi.org/10.1017/gheg.2018.10
Helasoja V, Prattala R, Dregval L, Pudule I, Kasmel A (2002) Late response and item nonresponse in the Finbalt Health Monitor survey. Eur J Public Health 12:117–123
Henderson DR, McNab RM, Rozsas T (2008) Did inequality increase in transition? An analysis of the transition countries of Eastern Europe and Central Asia. Eastern Eur Econ 46:28–49
Hoare E, Skouteris H, Fuller-Tyszkiewicz M, Millar L, Allender S (2014) Associations between obesogenic risk factors and depression among adolescents: a systematic review. Obes Rev 15:40–51. https://doi.org/10.1111/obr.12069
Ikeda N (2016) Validity of self-reports of height and weight among the general adult population in Japan: findings from National Household Surveys. PLoS ONE 11:e0148297. https://doi.org/10.1371/journal.pone.0148297
Jaacks LM, Gordon-Larsen P, Mayer-Davis EJ, Adair LS, Popkin B (2013) Age, period and cohort effects on adult body mass index and overweight from 1991 to 2009 in China: the China Health and Nutrition Survey. Int J Epidemiol 42:828–837. https://doi.org/10.1093/ije/dyt052
Jiang T, Gilthorpe MS, Shiely F, Harrington JM, Perry IJ, Kelleher CC, Tu YK (2013) Age–period–cohort analysis for trends in body mass index in Ireland. BMC Public Health 13:889. https://doi.org/10.1186/1471-2458-13-889
Jofre-Bonet M, Serra-Sastre V, Vandoros S (2018) The impact of the Great Recession on health-related risk factors, behaviour and outcomes in England. Soc Sci Med 197:213–225. https://doi.org/10.1016/j.socscimed.2017.12.010
Johnson W, Li L, Kuh D, Hardy R (2015) How has the age-related process of overweight or obesity development changed over time? co-ordinated analyses of individual participant data from five United Kingdom birth cohorts. PLOS Med 12:e1001828. https://doi.org/10.1371/journal.pmed.1001828
Keyes KM, Utz RL, Robinson W, Li G (2010) What is a cohort effect? Comparison of three statistical methods for modeling cohort effects in obesity prevalence in the United States, 1971–2006. Soc Sci Med 70:1100–1108. https://doi.org/10.1016/j.socscimed.2009.12.018
Klumbiene J, Petkeviciene J, Helasoja V, Prattala R, Kasmel A (2004) Sociodemographic and health behaviour factors associated with obesity in adult populations in Estonia, Finland and Lithuania. Eur J Public Health 14:390–394. https://doi.org/10.1093/eurpub/14.4.390
Lange S, Vollmer S (2017) The effect of economic development on population health: a review of the empirical evidence. Br Med Bull 121:47–60. https://doi.org/10.1093/bmb/ldw052
Leinsalu M, Vågerö D, Kunst AE (2004) Increasing ethnic differences in mortality in Estonia after the collapse of the Soviet Union. J Epidemiol Commun Health 58:583–589. https://doi.org/10.1136/jech.2003.013755
Liu H, Umberson D (2015) Gender, stress in childhood and adulthood, and trajectories of change in body mass. Soc Sci Med 139:61–69. https://doi.org/10.1016/j.socscimed.2015.06.026
Murayama H, Shaw BA (2017) Heterogeneity in Trajectories of body mass index and their associations with mortality in old age: a literature review. J Obes Metab Syndr 26:181–187. https://doi.org/10.7570/jomes.2017.26.3.181
OECD (2019) The heavy burden of obesity: the economics of prevention, OECD Health Policy Studies, OECD Publishing, Paris. https://doi.org/10.1787/67450d67-en. Accessed 7 Feb 2020
Pomerleau J et al (2000) Patterns of body weight in the Baltic Republics. Public Health Nutr 3:3–10
Reile R, Leinsalu M (2019) Factors associated with improving diet and physical activity among persons with excess body weight. Eur J Public Health 29:1166–1171. https://doi.org/10.1093/eurpub/ckz170
Reile R, Tekkel M, Veideman T (2019) Eesti täiskasvanud rahvastiku tervisekäitumise uuring 2018 [Health Behaviour among Estonian Adult Population, 2018], Tervise Arengu Instituut, Tallinn. https://www.tai.ee/et/terviseandmed/uuringud/download/484. Accessed 7 Feb 2020
Reither EN, Hauser RM, Yang Y (2009) Do birth cohorts matter? Age–period–cohort analyses of the obesity epidemic in the United States. Soc Sci Med 69:1439–1448. https://doi.org/10.1016/j.socscimed.2009.08.040
Reither EN, Land KC, Jeon SY, Powers DA, Masters RK, Zheng H et al (2015) Clarifying hierarchical age–period–cohort models: a rejoinder to Bell and Jones. Soc Sci Med 145:125–128. https://doi.org/10.1016/j.socscimed.2015.07.013
Robinson HA, Dam R, Hassan L, Jenkins D, Buchan I, Sperrin M (2019) Post-2000 growth trajectories in children aged 4–11 years: a review and quantitative analysis. Prev Med Rep 14:100834. https://doi.org/10.1016/j.pmedr.2019.100834
Siervo M et al (2015) Age-related changes in resting energy expenditure in normal weight, overweight and obese men and women. Maturitas 80:406–413. https://doi.org/10.1016/j.maturitas.2014.12.023
Titma M, Tuma NB, Silver BD (1998) Winners and losers in the postcommunist transition: new evidence from Estonia. Post-Sov Aff 14:114–136. https://doi.org/10.1080/1060586X.1998.10641449
Townshend T, Lake A (2017) Obesogenic environments: current evidence of the built and food environments. Perspect Public Health 137:38–44. https://doi.org/10.1177/1757913916679860
Tu YK, Chien KL, Burley V, Gilthorpe MS (2011) Unravelling the effects of age, period and cohort on metabolic syndrome components in a Taiwanese population using partial least squares regression. BMC Med Res Methodol 11:82. https://doi.org/10.1186/1471-2288-11-82
Vidra N, Trias-Llimós S, Janssen F (2019) Impact of obesity on life expectancy among different European countries: secondary analysis of population-level data over the 1975–2012 period. BMJ Open 9:e028086. https://doi.org/10.1136/bmjopen-2018-028086
Vieira LS, Bierhals IO, Vaz JDS, Meller FO, Wehrmeister FC, Assuncao MCF (2019) Socioeconomic status throughout life and body mass index: a systematic review and meta-analysis. Cad Saude Publica 35:e00125518. https://doi.org/10.1590/0102-311x00125518
Wilson R, Abbott JH (2018) Age, period and cohort effects on body mass index in New Zealand, 1997–2038. Aust Nz J Publ Heal 42:396–402. https://doi.org/10.1111/1753-6405.12804
Wirth K et al (2017) Biomarkers associated with sedentary behaviour in older adults: a systematic review. Ageing Res Rev 35:87–111. https://doi.org/10.1016/j.arr.2016.12.002
World Health Organisation Obesity: Situation and Trends. http://www.who.int/gho/ncd/risk_factors/obesity_text/en. Accessed 7 Feb 2020
Wullems JA, Verschueren SMP, Degens H, Morse CI, Onambélé GLJB (2016) A review of the assessment and prevalence of sedentarism in older adults, its physiology/health impact and non-exercise mobility counter-measures. Biogerontology 17:547–565. https://doi.org/10.1007/s10522-016-9640-1
Yang Y, Land K (2013) Age–period–cohort analysis: new models, methods, and empirical applications. Chapmann and Hall, New York. https://doi.org/10.1201/b13902
Funding
No specific funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Reile, R., Baburin, A., Veideman, T. et al. Long-term trends in the body mass index and obesity risk in Estonia: an age–period–cohort approach. Int J Public Health 65, 859–869 (2020). https://doi.org/10.1007/s00038-020-01447-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00038-020-01447-7