Abstract
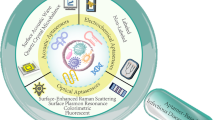
Nowadays, infectious diseases have been considered as life-threatening concerns worldwide. Traditional methods based on clinical features and epidemiological information have been successfully applied in infection diagnosis. However, these methods are either relatively complicated or time-consuming. Aptamer, a specific DNA/RNA binder, can serve as field-deployable sensors (termed aptasensors), and is thus highly promising to construct point-of-use tools for infection diagnosis. In this chapter, we will present the basic features of most prevalent infectious diseases and the efforts to obtain aptamers against their pathogen counterparts. Then, we will discuss the design strategies and working principles of typical aptasensors, nanomaterial-involved aptasensors, and microfluidics-integrated aptasensors for typical infectious diseases such as cholera, tuberculosis, anthrax, malaria, viral hepatitis, AIDS and COVID-19, as well as their application for infectious diseases profiling and cellular monitoring. It can be anticipated that aptamers will play a pivotal role in the future development of advanced diagnostic techniques of intricate infectious diseases.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Jones KE, Patel NG, Levy MA, Storeygard A, Balk D, Gittleman JL, Daszak P (2008) Global trends in emerging infectious diseases. Nature 451(7181):990–993
Park KS (2018) Nucleic acid aptamer-based methods for diagnosis of infections. Biosens Bioelectron 102:179–188
Morens DM, Fauci AS (2013) Emerging infectious diseases: threats to human health and global stability. PLoS Pathog 9(7):e1003467
Molefe P, Masamba P, Oyinloye B, Mbatha L, Meyer M, Kappo A (2018) Molecular application of aptamers in the diagnosis and treatment of cancer and communicable diseases. Pharmaceuticals 11 (4)
Mossong J, Hens N, Jit M, Beutels P, Auranen K, Mikolajczyk R, Massari M, Salmaso S, Tomba GS, Wallinga JJP (2008) Social contacts and mixing patterns relevant to the spread of infectious diseases. PLoS Med 5(3):e74
Mazar J, Li Y, Rosado A, Phelan P, Kedarinath K, Parks GD, Alexander KA, Westmoreland TJ (2018) Zika virus as an oncolytic treatment of human neuroblastoma cells requires CD24. PLoS ONE 13(7):e0200358
Yang S, Wu J, Ding C, Cui Y, Zhou Y, Li Y, Deng M, Wang C, Xu K, Ren J, Ruan B, Li L (2017) Epidemiological features of and changes in incidence of infectious diseases in China in the first decade after the SARS outbreak: an observational trend study. Lancet Infect Dis 17(7):716–725
Cyranoski DJN (2017) SARS outbreak linked to Chinese bat cave. Nature 552:15–16
Nkengasong J (2020) China’s response to a novel coronavirus stands in stark contrast to the 2002 SARS outbreak response. Nat Med 26(3):310–311
Du Toit A (2018) Continued risk of Ebola virus outbreak. Nat Rev Microbiol 16(9):521
Bornholdt ZA, Turner HL, Murin CD, Li W, Sok D, Souders CA, Piper AE, Goff A, Shamblin JD, Wollen SEJS (2016) Isolation of potent neutralizing antibodies from a survivor of the 2014 Ebola virus outbreak. Science 351(6277):1078–1083
Li G, De Clercq E (2020) Therapeutic options for the 2019 novel coronavirus (2019-nCoV). Nat Rev Drug Discov 19(3):149–150
McGuinness WA, Malachowa N, DeLeo F (2017) Focus: infectious diseases: vancomycin resistance in Staphylococcus aureus. N Engl J Med 90(2):269
Gagneux S (2018) Ecology and evolution of Mycobacterium tuberculosis. Nat Rev Microbiol 16(4):202
Hethcote HW (2000) The mathematics of infectious diseases. SIAM Rev Soc Ind Appl Math 42(4):599–653
Schnadig VB (2017) Cytopathology of infectious and inflammatory diseases. Elsevier Inc., New York, pp 22–80
Yang S, Rothman RE (2004) PCR-based diagnostics for infectious diseases: uses, limitations, and future applications in acute-care settings. Lancet Infect Dis 4(6):337–348
Mahony JB (2014) Nucleic acid amplification-based diagnosis of respiratory virus infections. Expert Rev Anti Infect Ther 8(11):1273–1292
Mori Y, Notomi T (2009) Loop-mediated isothermal amplification (LAMP): a rapid, accurate, and cost-effective diagnostic method for infectious diseases. J Infect Chemother 15(2):62–69
Dunn MR, Jimenez RM, Chaput JC (2017) Analysis of aptamer discovery and technology. Nat Rev Chem 1(10):0076
McKeague M, DeRosa MC (2012) Challenges and opportunities for small molecule aptamer development. J Nucleic Acids 2012:748913
Kaper JB, Morris JG, Levine MM (1995) Cholera. Clin Microbiol Rev 8(1):48
Davies HG, Bowman C, Luby SP (2017) Cholera—management and prevention. J Infect 74:S66-S73
Ramamurthy TJL (1993) Emergence of novel strain of Vibrio cholerae with epidemic potential in southern and eastern India. Lancet 341:703–704
Mekalanos JJ, Swartz DJ, Pearson GDN, Harford N, Groyne F, Dewilde M (1983) Cholera toxin genes: nucleotide sequence, deletion analysis and vaccine development. Nature 306(5943):551–557
Frohnmeyer E, Tuschel N, Sitz T, Hermann C, Dahl GT, Schulz F, Baeumner AJ, Fischer M (2019) Aptamer lateral flow assays for rapid and sensitive detection of cholera toxin. Analyst 144(5):1840–1849
Bruno JG, Kiel JL (2002) Use of magnetic beads in selection and detection of biotoxin Aptamers by Electrochemiluminescence and enzymatic methods. Biotechniques 32(1):178–183
Frohnmeyer E, Frisch F, Falke S, Betzel C, Fischer M (2018) Highly affine and selective aptamers against cholera toxin as capture elements in magnetic bead-based sandwich ELAA. J Biotechnol 269:35–42
Panic N, Maetzel H, Bulajic M, Radovanovic M, Lohr JM (2020) Pancreatic tuberculosis: a systematic review of symptoms, diagnosis and treatment. United Eur Gastroent 8(4):396–402
Muneer A, Macrae B, Krishnamoorthy S, Zumla A (2019) Urogenital tuberculosis—epidemiology, pathogenesis and clinical features. Nat Rev Urol 16(10):573–598
Li L, Liu Z, Zhang H, Yue W, Li CW, Yi C (2018) A point-of-need enzyme linked aptamer assay for Mycobacterium tuberculosis detection using a smartphone. Sens Actuators B Chem 254:337–346
He F, Xiong Y, Liu J, Tong F, Yan D (2016) Construction of Au-IDE/CFP10-ESAT6 aptamer/DNA-AuNPs MSPQC for rapid detection of Mycobacterium tuberculosis. Biosens Bioelectron 77:799–804
Zhang X, Feng Y, Duan S, Su L, Zhang J, He F (2019) Mycobacterium tuberculosis strain H37Rv Electrochemical Sensor Mediated by Aptamer and AuNPs-DNA. ACS Sens 4(4):849–855
Ansari N, Ghazvini K, Ramezani M, Shahdordizadeh M, Yazdian-Robati R, Abnous K, Taghdisi SM (2017) Selection of DNA aptamers against Mycobacterium tuberculosis Ag85A, and its application in a graphene oxide-based fluorometric assay. Microchim Acta 185(1):21
McNerney R, Daley P (2011) Towards a point-of-care test for active tuberculosis: obstacles and opportunities. Nat Rev Microbiol 9(3):204–213
Thakur H, Kaur N, Sareen D, Prabhakar N (2017) Electrochemical determination of M. tuberculosis antigen based on Poly(3,4-ethylenedioxythiophene) and functionalized carbon nanotubes hybrid platform. Talanta 171:115–123
Li L, Yuan Y, Chen Y, Zhang P, Bai Y, Bai L (2018) Aptamer based voltammetric biosensor for Mycobacterium tuberculosis antigen ESAT-6 using a nanohybrid material composed of reduced graphene oxide and a metal-organic framework. Microchim Acta 185(8):379
Zhang X, Feng Y, Yao Q, He F (2017) Selection of a new Mycobacterium tuberculosis H37Rv aptamer and its application in the construction of a SWCNT/aptamer/Au-IDE MSPQC H37Rv sensor. Biosens Bioelectron 98:261–266
Kim J, Gedi V, Lee SC, Cho JH, Moon JY, Yoon MY (2015) Advances in Anthrax Detection: Overview of Bioprobes and Biosensors. Appl Biochem Biotechnol 176(4):957–977
Klein F, Walker JS, Fitzpatrick DF, Lincoln RE, Mahlandt BG, Jones WI, Dobbs JP, Hendrix KJ (1966) Pathophysiology of Anthrax. J Infect Dis 116(2):123–138
Barth H, Aktories K, Popoff MR, Stiles BG (2004) Binary bacterial toxins: biochemistry, biology, and applications of common clostridium and bacillus proteins. Microbio Mol Biol Rev 68(3):373
Moayeri M, Leppla SH (2004) The roles of anthrax toxin in pathogenesis. Curr Opin Microbiol 7(1):19–24
Lahousse M, Park HC, Lee SC, Ha NR, Jung IP, Schlesinger SR, Shackelford K, Yoon MY, Kim SK (2018) Inhibition of anthrax lethal factor by ssDNA aptamers. Arch Biochem Biophys 646:16–23
Choi JS, Kim SG, Lahousse M, Park HY, Park HC, Jeong B, Kim J, Kim SK, Yoon MY (2011) Screening and Characterization of High-Affinity ssDNA Aptamers against Anthrax Protective Antigen. J Biomol Screen 16(2):266–271
Bruno JG, Carrillo MP (2012) Development of aptamer beacons for rapid presumptive detection of Bacillus spores. J Fluoresc 22(3):915–924
Oh BN, Lee S, Park HY, Baeg JO, Yoon MY, Kim J (2011) Sensitive fluorescence assay of anthrax protective antigen with two new DNA aptamers and their binding properties. Analyst 136(16):3384–3388
Kim DJ, Park HC, Sohn IY, Jung JH, Yoon OJ, Park JS, Yoon MY, Lee NE (2013) Electrical Graphene Aptasensor for ultra-sensitive detection of anthrax toxin with amplified signal transduction. Small 9(19):3352–3360
Lee SC, Gedi V, Ha NR, Cho JH, Park HC, Yoon MY (2015) Development of receptor-based inhibitory RNA aptamers for anthrax toxin neutralization. Int J Biol Macromol 77:293–302
Dong Y, Zhang T, Lin X, Feng J, Luo F, Gao H, Wu Y, Deng R, He Q (2020) Graphene/aptamer probes for small molecule detection: from in vitro test to in situ imaging. Microchim Acta 187(3):179
Karimi F, Dabbagh S (2019) Gel green fluorescence ssDNA aptasensor based on carbon nanotubes for detection of anthrax protective antigen. Int J Biol Macromol 140:842–850
Ivanovskii AL (2012) Graphene-based and graphene-like materials. Russ Chem Rev 81(7):571–605
Bradley KA, Mogridge J, Mourez M, Collier RJ, Young JAJN (2001) Identification of the cellular receptor for anthrax toxin. Nature 414(6860):225–229
Prasidthrathsint K, Stapleton JT (2019) Laboratory diagnosis and monitoring of viral hepatitis. Gastroenterol Clin North Am 48(2):259–279
Qu F, Liu Y, Kong R, You J (2017) A versatile DNA detection scheme based on the quenching of fluorescent silver nanoclusters by MoS2 nanosheets: application to aptamer-based determination of hepatitis B virus and of dopamine. Microchim Acta 184(11):4417–4424
Zheng H, Lang Y, Yu J, Han Z, Chen B, Wang Y (2019) Affinity binding of aptamers to agarose with DNA tetrahedron for removal of hepatitis B virus surface antigen. Colloids Surf B 178:80–86
Ghanbari K, Roushani M (2018) A nanohybrid probe based on double recognition of an aptamer MIP grafted onto a MWCNTs-Chit nanocomposite for sensing hepatitis C virus core antigen. Sens Actuators B Chem 258:1066–1071
Pleshakova OT, Kaysheva LA, Shumov DI, Ziborov SV, Bayzyanova MJ, Konev AV, Uchaikin FV, Archakov IA, Ivanov DY (2019) Detection of Hepatitis C Virus Core Protein in Serum Using Aptamer-Functionalized AFM Chips. Micromachines 10 (2)
Huang R, Xi Z, Deng Y, He N (2016) Fluorescence based Aptasensors for the determination of hepatitis B virus e antigen. Sci Rep 6(1):31103
Park JH, Jee MH, Kwon OS, Keum SJ, Jang SK (2013) Infectivity of hepatitis C virus correlates with the amount of envelope protein E2: development of a new aptamer-based assay system suitable for measuring the infectious titer of HCV. Virology 439(1):13–22
Ghanbari K, Roushani M, Azadbakht A (2017) Ultra-sensitive aptasensor based on a GQD nanocomposite for detection of hepatitis C virus core antigen. Anal Biochem 534:64–69
Madhombiro M, Cha R, Sawyer J, Przybyla S, Burstein G, Morse GD (2019) Why do young adults living with HIV perform poorly on combined antiretroviral therapy (CART)? a Zimbabwean perspective. Future Virol 14(4):211–217
Zeng J, Li X, Yuan H, Ma M, Li D, Ma J, Liao S Screening ssDNA aptamers against HIV P24 antigen using agarose beads as carriers. In: BIO Web of Conferences, 2017. EDP Sciences, p 03009
Zhang K, Yang Q, Huang W, Wang K, Zhu X, Xie M (2019) Detection of HIV-1 ribonuclease H activity in single-cell by using RNA mimics green fluorescent protein based biosensor. Sens Actuators B Chem 281:439–444
Fatin MF, Rahim Ruslinda A, Gopinath SCB, Arshad MKM, Hashim U, Lakshmipriya T, Tang T-H, Kamarulzaman A (2019) Co-ordinated split aptamer assembly and disassembly on Gold nanoparticle for functional detection of HIV-1 tat. Process Biochem 79:32–39
Wang L, Zhou H, Liu B, Zhao C, Fan J, Wang W, Tong C (2017) Fluorescence assay for ribonuclease H based on Nonlabeled substrate and DNAzyme assisted cascade amplification. Anal Chem 89(20):11014–11020
Deng X, Wang C, Gao Y, Li J, Wen W, Zhang X, Wang S (2018) Applying strand displacement amplification to quantum dots-based fluorescent lateral flow assay strips for HIV-DNA detection. Biosens Bioelectron 105:211–217
DeStefano JJ, Alves Ferreira-Bravo I (2018) A highly sensitive aptamer-based HIV reverse transcriptase detection assay. J Virol Methods 257:22–28
Chang CC, Chen CY, Chuang TL, Wu TH, Wei SC, Liao H, Lin CW (2016) Aptamer-based colorimetric detection of proteins using a branched DNA cascade amplification strategy and unmodified gold nanoparticles. Biosens Bioelectron 78:200–205
Wang H, Liang G (2015) Epidemiology of Japanese encephalitis: past, present, and future prospects. Ther Clin Risk Manag 11:435–448
Whitley RJ (1990) Viral Encephalitis. N Engl J Med 323(4):242–250
Ray D, Shah A, Tilgner M, Guo Y, Zhao YW, Dong HP, Deas TS, Zhou YS, Li HM, Shi PY (2006) West Nile Virus 5’-Cap Structure Is Formed by Sequential Guanine N-7 and Ribose 2’-O Methylations by Nonstructural Protein 5. J Virol 80(17):8362–8370
Han SR, Lee SW (2017) Inhibition of Japanese encephalitis virus (JEV) replication by specific RNA aptamer against JEV methyltransferase. Biochem Biophys Res Commun 483(1):687–693
Kang J, Lee MS, Watowich SJ, Gorenstein DG (2007) Combinatorial selection of a RNA thioaptamer that binds to Venezuelan equine encephalitis virus capsid protein. FEBS Lett 581(13):2497–2502
Tian X, Li C, Huang A, Xia S, Lu S, Shi Z, Lu L, Jiang S, Yang Z, Wu Y, Ying T (2020) Potent binding of 2019 novel coronavirus spike protein by a SARS coronavirus-specific human monoclonal antibody. Emerg Microbes Infect 9(1):382–385
Song Yl, Song J, Wei XY, Huang MJ, Sun M, Zhu L, Lin BQ, Shen HC, Zhu Z, Yang CY (2020) Discovery of Aptamers Targeting Receptor-Binding Domain of the SARS-CoV-2 Spike Glycoprotein. Anal Chem 14(92):9895–9900
Ung COL (2020) Community pharmacist in public health emergencies: quick to action against the coronavirus 2019-nCoV outbreak. Res Social Adm Pharm 16(4):583–586
Hui DS, E IA, Madani TA, Ntoumi F, Kock R, Dar O, Ippolito G, McHugh TD, Memish ZA, Drosten C, Zumla A, Petersen E (2020) The continuing 2019-nCoV epidemic threat of novel coronaviruses to global health—The latest 2019 novel coronavirus outbreak in Wuhan, China. Int J Infect Dis 91:264–266
Wrapp D, Wang N, Corbett KS, Goldsmith JA, Hsieh C-L, Abiona O, Graham BS, McLellan JS (2020) Cryo-EM structure of the 2019-nCoV spike in the prefusion conformation. Science 367(6483):1260
Nik Kamarudin NAA, Mohammed NA, Mustaffa KMF (2017) Aptamer technology: adjunct therapy for malaria. Biomedicines 5(1):1
World Health Organization (2020) World malaria report 2019
Fatih FA, Staines HM, Siner A, Ahmed MA, Woon LC, Pasini EM, Kocken CHM, Singh B, Cox-Singh J, Krishna S (2013) Susceptibility of human Plasmodium knowlesi infections to anti-malarials. Malar J 12(1):425
Tun KM, Imwong M, Lwin KM, Win AA, Hlaing TM, Hlaing T, Lin K, Kyaw MP, Plewes K, Faiz MA, Dhorda M, Cheah PY, Pukrittayakamee S, Ashley EA, Anderson TJC, Nair S, McDew-White M, Flegg JA, Grist EPM, Guerin P, Maude RJ, Smithuis F, Dondorp AM, Day NPJ, Fo N, White NJ, Woodrow CJ (2015) Spread of artemisinin-resistant Plasmodium falciparum in Myanmar: a cross-sectional survey of the K13 molecular marker. Lancet Infect Dis 15(4):415–421
Figueroa-Miranda G, Feng L, Shiu SC, Dirkzwager RM, Cheung YW, Tanner JA, Schöning MJ, Offenhäusser A, Mayer D (2018) Aptamer-based electrochemical biosensor for highly sensitive and selective malaria detection with adjustable dynamic response range and reusability. Sens Actuators B Chem 255:235–243
Wang WX, Cheung YW, Dirkzwager RM, Wong WC, Tanner JA, Li HW, Wu Y (2017) Specific and sensitive detection of Plasmodium falciparum lactate dehydrogenase by DNA-scaffolded silver nanoclusters combined with an aptamer. Analyst 142(5):800–807
Godonoga M, Lin TY, Oshima A, Sumitomo K, Tang MSL, Cheung YW, Kinghorn AB, Dirkzwager RM, Zhou C, Kuzuya A, Tanner JA, Heddle JG (2016) A DNA aptamer recognising a malaria protein biomarker can function as part of a DNA origami assembly. Sci Rep 6:21266
Dirkzwager RM, Liang S, Tanner JA (2016) Development of aptamer-based point-of-care diagnostic devices for malaria using three-dimensional printing rapid prototyping. ACS Sens 1(4):420–426
Kenry GA, Zhang X, Zhang H, Lim CT (2016) Highly sensitive and selective aptamer-based fluorescence detection of a malarial biomarker using single-layer MoS2 Nanosheets. ACS Sens 1(11):1315–1321
Singh NK, Thungon PD, Estrela P, Goswami P (2019) Development of an aptamer-based field effect transistor biosensor for quantitative detection of Plasmodium falciparum glutamate dehydrogenase in serum samples. Biosens Bioelectron 123:30–35
Lee S, Song KM, Jeon W, Jo H, Shim YB, Ban C (2012) A highly sensitive aptasensor towards Plasmodium lactate dehydrogenase for the diagnosis of malaria. Biosens Bioelectron 35(1):291–296
Jeon W, Lee S, Dh M, Ban C (2013) A colorimetric aptasensor for the diagnosis of malaria based on cationic polymers and gold nanoparticles. Anal Biochem 439 (1):11–16
Cheung YW, Dirkzwager RM, Wong WC, Costa JDN, Tanner JA (2018) Aptamer-mediated Plasmodium-specific diagnosis of malaria. Biochimie 145:131–136
Dirkzwager R, Kinghorn A, Richards J, Tanner J (2015) APTEC: Aptamer-tethered enzyme capture as a novel rapid diagnostic test for malaria. Chem Commun 51:4697–4700
Cheung YW, Kwok J, Law AW, Watt RM, Kotaka M, Tanner JAJPotNAoS (2013) Structural basis for discriminatory recognition of Plasmodium lactate dehydrogenase by a DNA aptamer. Proc Natl Acad Sci USA 110 (40):15967–15972
Jain P, Das S, Chakma B, Goswami P (2016) Aptamer-graphene oxide for highly sensitive dual electrochemical detection of Plasmodium lactate dehydrogenase. Anal Biochem 514:32–37
Fraser LA, Kinghorn AB, Dirkzwager RM, Liang S, Cheung YW, Lim B, Shiu SCC, Tang MSL, Andrew D, Manitta J, Richards JS, Tanner JA (2018) A portable microfluidic Aptamer-Tethered Enzyme Capture (APTEC) biosensor for malaria diagnosis. Biosens Bioelectron 100:591–596
Birch CM, Hou HW, Han J, Niles JC (2015) Identification of malaria parasite-infected red blood cell surface aptamers by inertial microfluidic SELEX (I-SELEX). Sci Rep 5(1):11347
Aryanyijuka N (2018) Non-invasive mobile phone diagnosis of malaria supported by an in vivo technique using aptamers conjugated with acridine orange. Makerere University
Tonelli RR, Colli W, Alves MJ (2012) Selection of binding targets in parasites using phage-display and aptamer libraries in vivo and in vitro. Front Immunol 3:419
Lo NC, Gurarie D, Yoon N, Coulibaly JT, Bendavid E, Andrews JR, King CH (2018) Impact and cost-effectiveness of snail control to achieve disease control targets for schistosomiasis. Proc Nat Acad Sci 115(4):E584
Gryseels B, Polman K, Clerinx J, Kestens L (2006) Human schistosomiasis. Lancet 368(9541):1106–1118
Colley DG, Bustinduy AL, Secor WE, King CH (2014) Human schistosomiasis. Lancet 383(9936):2253–2264
Mangano VD, Bianchi C, Ouedraogo M, Kabore Y, Corran P, Silva N, Sirima SB, Nebie I, Bruschi F, Modiano D (2020) Antibody response to Schistosoma haematobium and other helminth species in malaria-exposed populations from Burkina Faso. Acta Trop 205:105381
Long Y, Qin Z, Duan M, Li S, Wu X, Lin W, Li J, Zhao Z, Liu J, Xiong D, Huang Y, Hu X, Yang C, Ye M, Tan W (2016) Screening and identification of DNA aptamers toward Schistosoma japonicum eggs via SELEX. Sci Rep 6(1):24986
Moss WJ (2017) Measles. Lancet 390(10111):2490–2502
Basetti S, Hodgson J, Rawson TM, Majeed A (2017) Scarlet fever: a guide for general practitioners. London J Prim Care (Abingdon) 9(5):77–79
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Zhang, T., Lu, Y., Deng, S., Deng, R. (2021). Aptamers for the Diagnosis of Infectious Diseases. In: Dong, Y. (eds) Aptamers for Medical Applications. Springer, Singapore. https://doi.org/10.1007/978-981-33-4838-7_8
Download citation
DOI: https://doi.org/10.1007/978-981-33-4838-7_8
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-33-4837-0
Online ISBN: 978-981-33-4838-7
eBook Packages: Chemistry and Materials ScienceChemistry and Material Science (R0)