Abstract
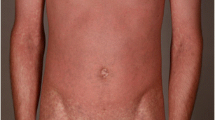
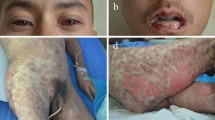
Exanthematous (also known as morbilliform) drug reactions are one of the most common cutaneous adverse drug reactions (CADRs). Clinically, exanthematous reactions appear as erythematous macules and papules, sometimes accompanied by pruritus and low-grade fever, appearing days to weeks after culprit drug administration. While the pathogenesis of exanthematous drug reactions remains to be fully elucidated, it is thought to be a form of delayed T-cell hypersensitivity reaction. The list of offending agents is broad, and almost any medication may cause an exanthematous drug eruption. However, antibiotics are common offending agents. Diagnosis is clinical; identifying warning signs and symptoms of a more severe cutaneous adverse reaction is critical. Treatment of exanthematous drug eruptions is primarily supportive, providing symptomatic relief if symptoms are present. Further study is indicated for learning more about the pathophysiological mechanisms, role of systemic therapy, and role of desensitization for future use of the causative medications.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
Abbreviations
- AGEP:
-
Acute generalized exanthematous pustulosis
- BUN:
-
Blood urea nitrogen
- CADR:
-
Cutaneous adverse drug reaction
- CBC:
-
Complete blood count
- DIHS:
-
Drug-induced hypersensitivity syndrome
- DRESS:
-
Drug reaction with eosinophilia and systemic symptoms
- EBV:
-
Epstein–Barr virus
- FDE:
-
Fixed drug eruption
- HIV:
-
Human immunodeficiency virus
- HLA:
-
Human leukocyte antigen
- IHC:
-
Immunohistochemistry
- IL:
-
Interleukin
- MHC:
-
Major histocompatibility complex
- NSAIDs:
-
Nonsteroidal anti-inflammatory drugs
- p–i:
-
Pharmacologic interaction of drugs with immune receptors
- SCAR:
-
Severe cutaneous adverse reaction
- SDRIFE:
-
Symmetrical drug-related intertriginous and flexural exanthem
- SJS:
-
Stevens–Johnson syndrome
- SLE:
-
Systemic lupus erythematosus
- TEN:
-
Toxic epidermal necrolysis
- TMP-SMX:
-
Trimethoprim–sulfamethoxazole
References
Amstutz U, Shear NH, Rieder MJ, Hwang S, Fung V, Nakamura H, et al. Recommendations for HLA-B*15:02 and HLA-A*31:01 genetic testing to reduce the risk of carbamazepine-induced hypersensitivity reactions. Epilepsia. 2014;55(4):496–506.
Barbaud AM, Bene MC, Schmutz JL, Ehlinger A, Weber M, Faure GC. Role of delayed cellular hypersensitivity and adhesion molecules in amoxicillin-induced morbilliform rashes. Arch Dermatol. 1997;133(4):481–6.
Bigby M. Rates of cutaneous reactions to drugs. Arch Dermatol. 2001;137(6):765–70.
Carlson JA, Perlmutter A, Tobin E, Richardson D, Rohwedder A. Adverse antibiotic-induced eruptions associated with Epstein-Barr virus infection and showing Kikuchi-Fujimoto disease-like histology. Am J Dermatopathol. 2006;28(1):48–55.
Christiansen C, Dreborg S, Pichler WJ, Ekeli H. Macular exanthema appearing 5 days after X-ray contrast medium administration. Eur Radiol. 2002;12(Suppl 3):S94–7.
Cohen AD, Friger M, Sarov B, Halevy S. Which intercurrent infections are associated with maculopapular cutaneous drug reactions? A case-control study. Int J Dermatol. 2001;40(1):41–4.
Coopman SA, Johnson RA, Platt R, Stern RS. Cutaneous disease and drug reactions in HIV infection. N Engl J Med. 1993;328(23):1670–4.
Crowson AN, Magro CM. Recent advances in the pathology of cutaneous drug eruptions. Dermatol Clin. 1999;17(3):537–60.
deShazo RD, Kemp SF. Allergic reactions to drugs and biologic agents. JAMA. 1997;278(22):1895–906.
Dilek N, Ozkol HU, Akbas A, Kilinc F, Dilek AR, Saral Y, et al. Cutaneous drug reactions in children: a multicentric study. Postepy Dermatol Alergol. 2014;31(6):368–71.
Fan WL, Shiao MS, Hui RC, Su SC, Wang CW, Chang YC, et al. HLA association with drug-induced adverse reactions. J Immunol Res. 2017;2017:3186328.
Fitzpatrick JE, High WA, Kyle WL. Chapter 3-Morbilliform eruptions. In: Fitzpatrick JE, High WA, Kyle WL, editors. Urgent care dermatology: symptom-based diagnosis. Amsterdam: Elsevier; 2018. p. 31–50.
Hanson SG, Nigro JF. Pediatric dermatology. Med Clin N Am. 1998;82(6):1381–403.
Hausermann P, Harr T, Bircher AJ. Baboon syndrome resulting from systemic drugs: is there strife between SDRIFE and allergic contact dermatitis syndrome? Contact Dermat. 2004;51(5–6):297–310.
Hertl M, Merk HF. Lymphocyte activation in cutaneous drug reactions. J Investig Dermatol. 1995;105(1 Suppl):95S–8S.
Hirsch LJ, Arif H, Nahm EA, Buchsbaum R, Resor SR Jr, Bazil CW. Cross-sensitivity of skin rashes with antiepileptic drug use. Neurology. 2008;71(19):1527–34.
Hoetzenecker W, Nageli M, Mehra ET, Jensen AN, Saulite I, Schmid-Grendelmeier P, et al. Adverse cutaneous drug eruptions: current understanding. Semin Immunopathol. 2016;38(1):75–86.
Justiniano H, Berlingeri-Ramos AC, Sanchez JL. Pattern analysis of drug-induced skin diseases. Am J Dermatopathol. 2008;30(4):352–69.
Lackmann GM, Schmidt B, Niehues T. Exanthema simulating measles without measles virus? Allergic reaction to a non-nucleoside reverse transcriptase inhibitor in an HIV infected boy treated with HAART. Hautarzt. 2003;54(8):765–6.
Lerch M, Pichler WJ. The immunological and clinical spectrum of delayed drug-induced exanthems. Curr Opin Allergy Clin Immunol. 2004;4(5):411–9.
Naranjo CA, Busto U, Sellers EM, Sandor P, Ruiz I, Roberts EA, et al. A method for estimating the probability of adverse drug reactions. Clin Pharmacol Ther. 1981;30(2):239–45.
Oberholzer B, Hoigne R, Hartmann K, Capaul R, Egli A, Wymann R, et al. Incidence of drug side effects by symptoms and syndromes. From the experiences of the comprehensive hospital drug monitoring and the Swiss Drug Side Effect Center. As an example: allergic and pseudo-allergic reactions with mild analgesics and NSAID. Ther Umsch. 1993;50(1):13–9.
Ónodi-Nagy K, Kinyó Á, Meszes A, Garaczi E, Kemény L, Bata-Csörgő Z. Amoxicillin rash in patients with infectious mononucleosis: evidence of true drug sensitization. Allergy Asthma Clin Immunol. 2015;11(1):1. https://doi.org/10.1186/1710-1492-11-1. PMID: 25784943; PMCID: PMC4362637.
Pichler WJ, Naisbitt DJ, Park BK. Immune pathomechanism of drug hypersensitivity reactions. J Allergy Clin Immunol. 2011;127(3 Suppl):S74–81.
Roujeau JC. Immune mechanisms in drug allergy. Allergol Int. 2006;55(1):27–33.
Scherer K, Brockow K, Aberer W, Gooi JH, Demoly P, Romano A, et al. Desensitization in delayed drug hypersensitivity reactions—an EAACI position paper of the Drug Allergy Interest Group. Allergy. 2013;68(7):844–52.
Shin HT, Chang MW. Drug eruptions in children. Curr Probl Pediatr. 2001;31(7):207–34.
Sonntag MR, Zoppi M, Fritschy D, Maibach R, Stocker F, Sollberger J, et al. Exanthema during frequent use of antibiotics and antibacterial drugs (penicillin, especially aminopenicillin, cephalosporin and cotrimoxazole) as well as allopurinol. Results of the Berne comprehensive hospital drug monitoring program. Schweiz Med Wochenschr. 1986;116(5):142–5.
Stern RS. Clinical practice. Exanthematous drug eruptions. N Engl J Med. 2012;366(26):2492–501.
Stokes SC, Tankersley MS. HIV: practical implications for the practicing allergist-immunologist. Ann Allergy Asthma Immunol. 2011;107(1):1–9.
van der Linden PD, van der Lei J, Vlug AE, Stricker BH. Skin reactions to antibacterial agents in general practice. J Clin Epidemiol. 1998;51(8):703–8.
Waldman R, Whitaker-Worth D, Grant-Kels JM. Cutaneous adverse drug reactions: kids are not just little people. Clin Dermatol. 2017;35(6):566–82.
Warrington RJ, Silviu-Dan F, Magro C. Accelerated cell-mediated immune reactions in penicillin allergy. J Allergy Clin Immunol. 1993;92(4):626–8.
Yawalkar N, Egli F, Hari Y, Nievergelt H, Braathen LR, Pichler WJ. Infiltration of cytotoxic T cells in drug-induced cutaneous eruptions. Clin Exp Allergy. 2000;30(6):847–55.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2022 Springer Nature Switzerland AG
About this chapter
Cite this chapter
Gabel, C., Kroshinsky, D. (2022). Exanthematous Drug Eruptions. In: Lee, H.Y., Creamer, D. (eds) Drug Eruptions. Updates in Clinical Dermatology. Springer, Cham. https://doi.org/10.1007/978-3-031-09388-3_7
Download citation
DOI: https://doi.org/10.1007/978-3-031-09388-3_7
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-031-09387-6
Online ISBN: 978-3-031-09388-3
eBook Packages: MedicineMedicine (R0)