Abstract
Background
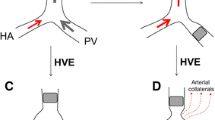
Preoperative portal vein embolization (PVE) is performed for right liver (RL) and sometimes left liver (LL) resection to prevent postoperative surgical complications.
Methods
We retrospectively reviewed 10 patients who underwent preoperative left PVE before LL resection for hepatobiliary malignancies along with 3 propensity score-matched control groups (n = 40 each).
Results
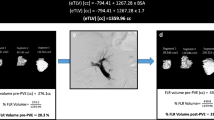
Mean patient age was 68.6 ± 6.9 years. Diagnoses included intrahepatic cholangiocarcinoma (n = 4), perihilar cholangiocarcinoma (n = 3), neuroendocrine carcinoma (n = 1), recurrent cholangiocarcinoma (n = 1), and inflammatory liver mass (n = 1). The reason for left PVE was a large LL >40 % of the total liver volume (TLV) with a major comorbidity or age > 70 years with a poor overall condition. All patients underwent preplanned operations, including LL resection at 1–3 weeks post PVE. The LL volume proportion of the TLV was 44.9 ± 1.7 and 40.7 ± 2.3 % before and after PVE; thus, 1–2 weeks post PVE, the kinetic shrinkage rate of the LL was 9.4 ± 3.3 %, and the kinetic growth rate of the RL was 7.6 ± 2.7 %. The overall surgical complication rates were 40, 50, and 39.2 % in the left PVE, large LL control, and all three control groups, respectively (p ≥ 0.727). In contrast, the adjusted rates of major complications were 0 % in the left PVE group versus 36.8 % (p = 0.040), 25.6 % (p = 0.123), and 15.8 % (p = 0.295) in the large-, medium-, and small-sized LL control groups, respectively.
Conclusions
Our experience indicates that left PVE is safe and induces atrophy of the LL effectively. We suggest that it can be a useful option to reduce the risk of postoperative complications in elderly high-risk patients.


Similar content being viewed by others
References
Yokoyama Y, Nagino M, Nimura Y (2007) Mechanisms of hepatic regeneration following portal vein embolization and partial hepatectomy: a review. World J Surg 31:367–374
Shindoh J, Truty MJ, Aloia TA et al (2013) Kinetic growth rate after portal vein embolization predicts posthepatectomy outcomes: toward zero liver-related mortality in patients with colorectal liver metastases and small future liver remnant. J Am Coll Surg 216:201–209
Lee SG, Hwang S (2005) How I do it: assessment of hepatic functional reserve for indication of hepatic resection. J Hepatobiliary Pancreat Surg 12:38–43
Hwang S, Ha TY, Song GW et al (2015) Quantified risk assessment for major hepatectomy via the indocyanine green clearance rate and liver volumetry combined with standard liver volume. J Gastrointest Surg 19:1305–1314
Hwang S, Ha TY, Ko GY et al (2015) Preoperative sequential portal and hepatic vein embolization in patients with hepatobiliary malignancy. World J Surg 39:2990–2998
Harimoto N, Yoshizumi T, Shimokawa M et al (2016) Sarcopenia is a poor prognostic factor following hepatic resection in patients 70 years of age and older with hepatocellular carcinoma. Hepatol Res (in press)
Sulpice L, Rayar M, Campillo B et al (2014) Advanced age remains an Achilles heel for liver resections. World J Surg 38:918–926
Schiergens TS, Lindenthaler A, Thomas MN et al (2016) Time-dependent impact of age and co-morbidities on long-term overall survival after liver resection. Liver Int (in press)
Oken MM, Creech RH, Tormey DC et al (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5:649–655
Kallogjeri D, Piccirillo JF, Spitznagel EL Jr et al (2012) Comparison of scoring methods for ACE-27: simpler is better. J Geriatr Oncol 3:238–245
Charlson ME, Pompei P, Ales KL et al (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Ko GY, Sung KB, Yoon HK et al (2003) Preoperative portal vein embolization with a new liquid embolic agent. Radiology 227:407–413
Yoo H, Ko GY, Gwon DI et al (2009) Preoperative portal vein embolization using an amplatzer vascular plug. Eur Radiol 19:1054–1061
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Yoon YI, Hwang S, Ko GY et al (2015) Balloon dilation of jejunal afferent loop functional stenosis following left hepatectomy and hepaticojejunostomy long time after pylorus-preserving pancreaticoduodenectomy: a case report. Korean J Hepatobiliary Pancreat Surg 19:66–70
Komori K, Nagino M, Nimura Y (2006) Hepatocyte morphology and kinetics after portal vein embolization. Br J Surg 93:745–751
Lee SG, Song GW, Hwang S et al (2010) Surgical treatment of hilar cholangiocarcinoma in the new era: the Asan experience. J Hepatobiliary Pancreat Sci 17:476–489
Hwang S, Lee SG, Ko GY et al (2009) Sequential preoperative ipsilateral hepatic vein embolization after portal vein embolization to induce further liver regeneration in patients with hepatobiliary malignancy. Ann Surg 249:608–616
Nagino M, Kamiya J, Nishio H et al (2006) Two hundred forty consecutive portal vein embolizations before extended hepatectomy for biliary cancer: surgical outcome and long-term followup. Ann Surg 243:364–372
Hayashi S, Baba Y, Ueno K et al (2007) Acceleration of primary liver tumor growth rate in embolized hepatic lobe after portal vein embolization. Acta Radiol 48:721–727
Yoo H, Kim JH, Ko GY et al (2011) Sequential transcatheter arterial chemoembolization and portal vein embolization versus portal vein embolization only before major hepatectomy for patients with hepatocellular carcinoma. Ann Surg Oncol 18:1251–1257
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hwang, S., Ko, GY., Kim, MH. et al. Preoperative Left Portal Vein Embolization for Left Liver Resection in High-Risk Hepatobiliary Malignancy Patients. World J Surg 40, 2758–2765 (2016). https://doi.org/10.1007/s00268-016-3618-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3618-7