Abstract
Introduction
The treatment for a majority of solid organ tumors is surgical resection; 10–20 % of patients suffer a perioperative complication. Perioperative complications may contribute to cancer recurrence. This study examined the relationship between postoperative complications and risk-adjusted patient overall survival.
Methods
Data from 2003 to 2009 were linked from our clinical cancer registry, the National Surgery Quality Improvement Project (NSQIP), and medical records. Patients who had tumor extirpation for cure were included. The NSQIP was used to identify complications. Patients with a complication were matched to patients without a complication. χ 2 tests and Cox proportional hazard regression models were used.
Results
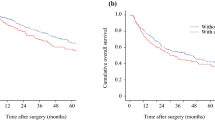
A total of 415 patients were included for survival analysis. The hazard ratio (HR) for mortality associated with having a complication was 2.17. The HR for mortality after 200 days postoperatively was 2.47. Infectious complications were associated with the highest association with increased mortality (HR = 3.56). Noninfectious complications were not associated with an increased risk of mortality.
Conclusions
This study investigated the relationship of surgical infectious complications in cancer patients with long-term survival for patients who had a number of different types of cancer. After taking into account the site, histology, and stage of the cancer, we found that patients with infectious complications had earlier death.
Similar content being viewed by others
References
El-Tamer MB, Ward BM, Schifftner T, et al. Morbidity and mortality following breast cancer surgery in women: national benchmarks for standards of care. Ann Surg. 2007;245(5):665–71.
Longo WE, Virgo KS, Johnson FE, et al. Risk factors for morbidity and mortality after colectomy for colon cancer. Dis Colon Rectum. 2000;43(1):83–91.
Begg CB, Riedel ER, Bach PB et al. Variations in morbidity after radical prostatectomy. N Engl J Med. 2002;346(15):1138–44.
Grivennikov SI, Greten FR, Karin M. Immunity, inflammation, and cancer. Cell. 2010;140(6): 883–99.
Balkwill F, Mantovani A. Inflammation and cancer: back to Virchow? Lancet. 2001;357(9255):539–45.
Walker KG, Bell SW, Rickard MJ, et al. Anastomotic leakage is predictive of diminished survival after curative resection for colorectal cancer. Ann Surg. 2004;240(2):255–9.
Law WL, Choi HK, Lee YM, Ho JW. The impact of postoperative complications on long-term outcomes following curative resection for colorectal cancer. Ann Surg Oncol. 2007;14(9):2559–66.
Hirai T, Yamashita Y, Mukaida H, et al. Poor prognosis in esophageal cancer patients with postoperative complications. Surg Today. 1998;28(6):576–9.
Roxburgh CS, Salmond JM, Horgan PG, et al. Comparison of the prognostic value of inflammation-based pathologic and biochemical criteria in patients undergoing potentially curative resection for colorectal cancer. Ann Surg. 2009;249(5):788–93.
Roxburgh CS, Platt JJ, Leitch EF, et al. Relationship between preoperative comorbidity, systemic inflammatory response, and survival in patients undergoing curative resection for colorectal cancer. Ann Surg Oncol. 2011;18(4):997–1005.
Law WL, Choi HK, Lee YM, et al. Anastomotic leakage is associated with poor lone-term outcome in patients after curative colorectal resection for malignancy. J Gastrointest Surg. 2007;11(1):8–15.
Bell SW, Walker KG, Rickard MJ, et al. Anastomotic leakage after curative anterior resection results in a higher prevalence of local recurrence. Br J Surg. 2003;90(10):1261–6.
Change SC, Lin JK, Yang SH, et al. Long-term outcome of anastomosis leakage after curative resection for mid and low rectal cancer. Hepatogastroenterology. 2003;50(54):1898–902.
Tachibna M, Tabara H, Kotoh T, et al. Prognostic significance of perioperative blood transfusions in resectable thoracic esophageal cancer. Am J Gastroenterol. 1999;94(3):757–65.
Swicher SG, Homes EC, Hunt KK, et al. Perioperative blood transfusions and decreased long-term survival in esophageal cancer. J Thorac Cardiovasc Surg. 1996;112(2):341–8.
Ito H, Are C, Gonen M, et al. Effect of postoperative morbidity on long-term survival after hepative resection for metastatic colorectal cancer. Ann Surg. 2008;247(6):994–1002.
Farid SG, Aldouri A, Morris-Stiff G, et al. Correlation between postoperative infective complications and long-term outcomes after hepatic resection for colorectal liver metastasis. Ann Surg. 2010;251(1):91–100.
Gomez D, Morris-Stiff G, Wyatt J, et al. Surgical technique and systemic inflammation influences long-term disease-free survival following hepatic resection for colorectal metastasis. J Surg Oncol. 2008;98(5):371–6.
Lerut T, Moons J, Coosemans W, et al. Postoperative complications after transthoracic esophagectomy for cancer of the esophagus and gastroesophageal junction are correlated with early cancer recurrence: role of systematic grading of complications using the modified Clavien classification. Ann Surg. 2009;250(5):798–807.
Lagarde SM, de Boer JD, ten Kate FJ, et al. Postoperative complications after esophagectomy for adenocarcinoma of the esophagus are related to timing of death due to recurrence. Ann Surg. 2008;247(1):71–6.
Folkman J. Role of angiogenesis in tumor growth and metastasis. Semin Oncol. 2002;29(6 Suppl 16):15–8.
Smyth MJ, Dunn GP, Schreiber RD. Cancer immunosurveillance and immunoediting: the roles of immunity in suppressing tumor development and shaping tumor immunogenicity. Adv Immunol. 2006;90:1–50.
Roxburgh CS, McMillan DC. Role of systemic inflammatory response in predicting survival in patients with primary operable cancer. Future Oncol. 2010;6(1):149–63.
Rakoff-Nahoum S. Why cancer and inflammation? Yale J Biol Med. 2006;79(3–4):123–30.
Acknowledgment
This study was supported in part by the Huntsman Cancer Foundation support of the Clinical Cancer Research database.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Scaife, C.L., Hartz, A., Pappas, L. et al. Association Between Postoperative Complications and Clinical Cancer Outcomes. Ann Surg Oncol 20, 4063–4066 (2013). https://doi.org/10.1245/s10434-013-3267-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-013-3267-0