Abstract
Background
First-line therapy of Cushing disease (CD) is transsphenoidal surgery (TSS) aimed to obtain a complete removal of the pituitary adenoma and remission of disease.
Purpose
To analyse the surgical outcome of patients with CD who underwent TSS in our Centre.
Methods
Retrospective analysis on patients with CD who underwent TSS between 1990 and 2016.
Results
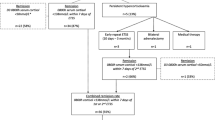
We analysed 102 TSS that included: 84 first TSS and 18 second and third TSS. The overall remission rate after surgery was 76.5%, with a significant higher percentage of remitted patients after the first TSS compared to the subsequent TSS (82% vs 50%, p = 0.014). The remission after the first TSS was significantly higher when performed by a dedicated surgical team (DST) (89.8% vs 71% p = 0.04) and when the immunohistochemical examination confirmed the adrenocorticotropic adenoma (87% vs 55%, p = 0.04). Neuroradiological findings influenced the surgical outcome in a non-significant manner. Post-TSS complications were reported in 32 patients, with no significant variation when TSS was performed by DST. In case of reintervention, remission of disease was obtained in 72.7% of microadenoma, while no remitted patients were observed in case of macroadenomas. The DST did not significantly improve the outcome.
Conclusion
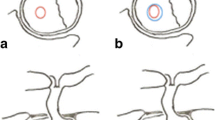
Cushing disease is characterized by a broad spectrum of neuroradiological presentation. Despite the availability of a DST make the TSS a safe and effective first-line treatment among all these patients, a precise pre-treatment evaluation is needed in order to define the aim of neurosurgery and to schedule the management of recurrent disease.


Similar content being viewed by others
References
Nieman LK, Biller BMK, Findling JW et al (2008) The diagnosis of Cushing’s syndrome: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 93:1526–1540. https://doi.org/10.1210/jc.2008-0125
Boscaro M, Arnaldi G (2009) Approach to the patient with possible Cushing’s syndrome. J Clin Endocrinol Metab 94:3121–3131. https://doi.org/10.1210/jc.2009-0612
Ferraù F, Korbonits M (2018) Metabolic syndrome in Cushing’s syndrome patients. Front Horm Res 49:85–103. https://doi.org/10.1159/000486002
Graversen D, Vestergaard P, Stochholm K et al (2012) Mortality in Cushing’s syndrome: a systematic review and meta-analysis. Eur J Intern Med 23:278–282. https://doi.org/10.1016/j.ejim.2011.10.013
Clayton RN, Jones PW, Reulen RC et al (2016) Mortality in patients with Cushing’s disease more than 10 years after remission: a multicentre, multinational, retrospective cohort study. Lancet Diabetes Endocrinol 4:569–576. https://doi.org/10.1016/S2213-8587(16)30005-5
Petersenn S, Beckers A, Ferone D et al (2015) Therapy of endocrine disease: outcomes in patients with Cushing’s disease undergoing transsphenoidal surgery: systematic review assessing criteria used to define remission and recurrence. Eur J Endocrinol 172:R227–R239. https://doi.org/10.1530/EJE-14-0883
Broersen LHA, Biermasz NR, van Furth WR et al (2018) Endoscopic vs. microscopic transsphenoidal surgery for Cushing’s disease: a systematic review and meta-analysis. Pituitary 21:524–534. https://doi.org/10.1007/s11102-018-0893-3
Bochicchio D, Losa M, Buchfelder M (1995) Factors influencing the immediate and late outcome of Cushing’s disease treated by transsphenoidal surgery: a retrospective study by the European Cushing’s Disease Survey Group. J Clin Endocrinol Metab 80:3114–3120. https://doi.org/10.1210/jcem.80.11.7593411
Chee GH, Mathias DB, James RA, Kendall-Taylor P (2001) Transsphenoidal pituitary surgery in Cushing’s disease: can we predict outcome? Clin Endocrinol (Oxf) 54:617–626. https://doi.org/10.1046/j.1365-2265.2001.01261.x
Biller BMK, Grossman AB, Stewart PM et al (2008) Treatment of adrenocorticotropin-dependent Cushing’s syndrome: a consensus statement. J Clin Endocrinol Metab 93:2454–2462. https://doi.org/10.1210/jc.2007-2734
Prevedello DM, Pouratian N, Sherman J et al (2008) Management of Cushing’s disease: outcome in patients with microadenoma detected on pituitary magnetic resonance imaging. J Neurosurg 109:751–759. https://doi.org/10.3171/JNS/2008/109/10/0751
Sala E, Ferrante E, Locatelli M et al (2014) Diagnostic features and outcome of surgical therapy of acromegalic patients: experience of the last three decades. Hormones 13:95–103. https://doi.org/10.1007/BF03401325
Rees DA, Hanna FWF, Davies JS et al (2002) Long-term follow-up results of transsphenoidal surgery for Cushing’s disease in a single centre using strict criteria for remission. Clin Endocrinol 56:541–551. https://doi.org/10.1046/j.1365-2265.2002.01511.x
Brichard C, Costa E, Fomekong E et al (2018) Outcome of transsphenoidal surgery for Cushing disease: a single-center experience over 20 years. World Neurosurg 119:e106–e117. https://doi.org/10.1016/j.wneu.2018.07.055
Fleseriu M, Hamrahian AH, Hoffman AR et al (2016) American Association of Clinical Endocrinologists and American College of Endocrinology Disease State Clinical review: diagnosis of recurrence in cushing disease. Endocr Pract 22:1436–1448. https://doi.org/10.4158/EP161512.DSCR
Arnaldi G, Angeli A, Atkinson AB et al (2003) Diagnosis and complications of Cushing’s syndrome: a consensus statement. J Clin Endocrinol Metab 88:5593–5602. https://doi.org/10.1210/jc.2003-030871
Ambrosi B, Barbetta L, Re T et al (1998) The one microgram adrenocorticotropin test in the assessment of hypothalamic-pituitary-adrenal function. Eur J Endocrinol 139:575–579
Molitch ME, Clemmons DR, Malozowski S et al (2011) Evaluation and treatment of adult growth hormone deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab 96:1587–1609. https://doi.org/10.1210/jc.2011-0179
Levi V, Bertani GA, Guastella C et al (2017) Microscopic versus endoscopic transsphenoidal surgery for pituitary adenoma: analysis of surgical safety in 221 consecutive patients. Clin Otolaryngol 42:466–469. https://doi.org/10.1111/coa.12631
Blevins LS, Christy JH, Khajavi M, Tindall GT (1998) Outcomes of therapy for Cushing’s disease due to adrenocorticotropin-secreting pituitary macroadenomas. J Clin Endocrinol Metab 83:63–67. https://doi.org/10.1210/jcem.83.1.4525
Swearingen B, Biller BM, Barker FG et al (1999) Long-term mortality after transsphenoidal surgery for Cushing disease. Ann Intern Med 130:821–824. https://doi.org/10.7326/0003-4819-130-10-199905180-00015
Shimon I, Ram Z, Cohen ZR, Hadani M (2002) Transsphenoidal surgery for Cushing’s disease: endocrinological follow-up monitoring of 82 patients. Neurosurgery 51:57–61. https://doi.org/10.1097/00006123-200207000-00008(discussion 61–62)
Honegger J, Schmalisch K, Beuschlein F et al (2012) Contemporary microsurgical concept for the treatment of Cushing’s disease: endocrine outcome in 83 consecutive patients. Clin Endocrinol (Oxf) 76:560–567. https://doi.org/10.1111/j.1365-2265.2011.04268.x
Hofmann BM, Fahlbusch R (2006) Treatment of Cushing’s disease: a retrospective clinical study of the latest 100 cases. Pituitary Surg Modern Approach 34:158–184. https://doi.org/10.1159/000091580
Alexandraki KI, Kaltsas GA, Isidori AM et al (2013) Long-term remission and recurrence rates in Cushing’s disease: predictive factors in a single-centre study. Eur J Endocrinol 168:639–648. https://doi.org/10.1530/EJE-12-0921
Feng M, Liu Z, Liu X et al (2018) Diagnosis and outcomes of 341 patients with Cushing’s disease following transsphenoid surgery: a single-center experience. World Neurosurg 109:e75–e80. https://doi.org/10.1016/j.wneu.2017.09.105
Dabrh AMA, Singh Ospina NM, Nofal AA et al (2016) Predictors of biochemical remission and recurrence after surgical and radiation treatments of cushing disease: a systematic review and meta-analysis. Endocr Pract 22:466–475. https://doi.org/10.4158/EP15922.RA
Prete A, Corsello SM, Salvatori R (2017) Current best practice in the management of patients after pituitary surgery. Ther Adv Endocrinol Metab 8:33–48. https://doi.org/10.1177/2042018816687240
Ciric I, Zhao J-C, Du H et al (2012) Transsphenoidal surgery for Cushing disease: experience with 136 patients. Neurosurgery 70:70–81. https://doi.org/10.1227/NEU.0b013e31822dda2c
Yamada S, Inoshita N, Fukuhara N et al (2015) Therapeutic outcomes in patients undergoing surgery after diagnosis of Cushing’s disease: a single-center study. Endocr J 62:1115–1125. https://doi.org/10.1507/endocrj.15-0463
Shirvani M, Motiei-Langroudi R, Sadeghian H (2016) Outcome of microscopic transsphenoidal surgery in Cushing disease: a case series of 96 patients. World Neurosurg 87:170–175. https://doi.org/10.1016/j.wneu.2015.11.046
Chandler WF, Barkan AL, Hollon T et al (2016) Outcome of transsphenoidal surgery for Cushing disease: a single-center experience over 32 years. Neurosurgery 78:216–223. https://doi.org/10.1227/NEU.0000000000001011
Keskin FE, Ozkaya HM, Bolayirli M et al (2017) Outcomes of primary transsphenoidal surgery in Cushing disease: experience of a tertiary center. World Neurosurg 106:374–381. https://doi.org/10.1016/j.wneu.2017.07.014
Cebula H, Baussart B, Villa C et al (2017) Efficacy of endoscopic endonasal transsphenoidal surgery for Cushing’s disease in 230 patients with positive and negative MRI. Acta Neurochir (Wien) 159:1227–1236. https://doi.org/10.1007/s00701-017-3140-1
Fahlbusch R, Buchfelder M, Müller OA (1986) Transsphenoidal surgery for Cushing’s disease. J R Soc Med 79:262–269. https://doi.org/10.1177/014107688607900504
Patil CG, Veeravagu A, Prevedello DM et al (2008) Outcomes after repeat transsphenoidal surgery for recurrent Cushing’s disease. Neurosurgery 63:266–270. https://doi.org/10.1227/01.NEU.0000313117.35824.9F(discussion 270–271)
Acknowledgements
We thank Prof. Bruno Ambrosi for providing us some of the missing data and his expertise in the field of Cushing disease. We also thank endocrine nurse specialists of Endocrinology Unit, Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico of Milan for their professionalism in executing endocrine dynamic test.
Funding
This study was supported by the Associazione Italiana Ricerca sul Cancro (Grant IG 2017-20594 to G. Mantovani), Ricerca Corrente Funds from the Italian Ministry of Health, and Progetti di Ricerca di Interesse Nazionale (PRIN) (Grant 2015ZHKFTA to G. Mantovani).
Author information
Authors and Affiliations
Contributions
ALS analysed the data, and wrote certain paragraphs (Materials and methods and Results) of manuscript. GD, ES, GC, and, RI and GR collected the data and draft the study protocol required by the Ethics Committee. ML, GC, GB, GM analysed the data and provided intellectual input. GM, MA, CG, and revised the project and critically reviewed the manuscript. EF designed the study and wrote the remaining paragraphs. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the Ethics Committee of Fondazione IRCCS Ca’ Granda Ospedale Maggiore Policlinico of Milan (Comitato Etico Milano Area 2, number 651_2019).
Informed consent
Subjects gave their written informed consent for the use of their clinical data for research purposes.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
M. Arosio and E. Ferrante are co-last authors.
Rights and permissions
About this article
Cite this article
Serban, A.L., Del Sindaco, G., Sala, E. et al. Determinants of outcome of transsphenoidal surgery for Cushing disease in a single-centre series. J Endocrinol Invest 43, 631–639 (2020). https://doi.org/10.1007/s40618-019-01151-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-019-01151-1