Abstract
Objectives
Systematic reviews report dietary patterns may be associated with cognitive health in older adults. However, inconsistent findings have been reported and relevant research lacks large scale studies. This study aims to examine the associations of dietary patterns and cognitive function among older adults in an Australian ageing cohort.
Design
A population-based, cross-sectional analysis of the baseline phase of the Sydney Memory and Ageing Study, a well-characterised Australian ageing study.
Setting
The Sydney Memory and Ageing Study was initiated in 2005 to examine the clinical characteristics and prevalence of mild cognitive impairment (MCI).
Participants
Non-demented community-dwelling individuals from English-speaking background (N = 819) aged 70–90 recruited from two areas of Sydney, following a random approach to 8914 individuals on the electoral roll in the Sydney Memory and Ageing study.
Measurements
The Cancer Council of Victoria Food Frequency Questionnaire was used to assess dietary intake. Scores for Mediterranean diet, Dietary Approaches to Stop Hypertension (DASH) diet and the Dietary Guidelines Index (DGI 2013) were generated. Two patterns — a Prudent healthy and a Western dietary pattern — were derived using principal components analysis (PCA). Neuropsychological tests were used to assess global cognition and six cognitive domains. Multivariate linear modelling assessed the relationship between dietary patterns and cognitive domain scores.
Results
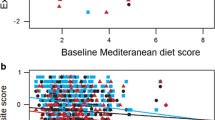
Mediterranean diet and DASH diet were both positively linked to visuospatial cognition (P=0.002 and P=0.001 respectively). Higher intake of legumes and nuts was related to better performance in global cognition (β=0.117; 95% CI:0.052, 0.181; P<0.001) and language and visuospatial cognitive domains.. The Prudent healthy diet was associated with better global cognition (β=0.307; 95% CI: 0.053, 0.562; P=0.019) in women and a Western diet was related to poorer global function (β=-0.242; 95% CI: -0.451,-0.034; P=0.023) and executive function (β=-0.325; 95% CI: -0.552,-0.099; P=0.005) in men.
Conclusion
In this analysis, higher adherence to the Mediterranean diet, DASH diet, Prudent healthy diet and greater consumption of legumes and nuts were associated with better cognition among older adults.
Similar content being viewed by others
References
Prince MJ, Comas-Herrera A, Knapp M, Guerchet MM, Karagiannidou M. World Alzheimer Report 2016 — Improving healthcare for people living with dementia: Coverage, quality and costs now and in the future. London: Alzheimer’s Disease International; 2016.
Canevelli M, Lucchini F, Quarata F, Bruno G, Cesari M. Nutrition and Dementia: Evidence for Preventive Approaches? Nutrients. 2016;8(3):144.
Yaffe K. Modifiable risk factors and prevention of dementia: What is the latest evidence? JAMA Intern Med. 2018;178(2):281–2.
Milte CM, McNaughton SA. Dietary patterns and successful ageing: a systematic review. Eur J Nutr. 2016;55(2):423–50.
Newby PK, Tucker KL. Empirically Derived Eating Patterns Using Factor or Cluster Analysis: A Review. Nutr Rev. 2004;62(5):177–203.
Radd-Vagenas S, Kouris-Blazos A, Singh MF, Flood VM. Evolution of Mediterranean diets and cuisine: concepts and definitions. Asia Pac J Clin Nutr. 2017;26(5):749–63.
Widmer RJ, Flammer AJ, Lerman LO, Lerman A. “The Mediterranean Diet, its Components, and Cardiovascular Disease”. Am J Med. 2015;128(3):229–38.
Matthews FE, Arthur A, Barnes LE, Bond J, Jagger C, Robinson L, et al. A two-decade comparison of prevalence of dementia in individuals aged 65 years and older from three geographical areas of England: results of the Cognitive Function and Ageing Study I and II. Lancet. 2013;382(9902):1405–12.
Qiu C, von Strauss E, Backman L, Winblad B, Fratiglioni L. Twenty-year changes in dementia occurrence suggest decreasing incidence in central Stockholm, Sweden. Neurology. 2013;80(20):1888–94.
Christensen K, Thinggaard M, Oksuzyan A, Steenstrup T, Andersen-Ranberg K, Jeune B, et al. Physical and cognitive functioning of people older than 90 years: a comparison of two Danish cohorts born 10 years apart. Lancet. 2013;382(9903):1507–13.
Chen X, Maguire B, Brodaty H, O’Leary F. Dietary Patterns and Cognitive Health in Older Adults: A Systematic Review. J Alzheimers Dis. 2019;67(2):583–619.
Sachdev PS, Brodaty H, Reppermund S, Kochan NA, Trollor JN, Draper B, et al. The Sydney Memory and Ageing Study (MAS): methodology and baseline medical and neuropsychiatric characteristics of an elderly epidemiological non-demented cohort of Australians aged 70–90 years. International psychogeriatrics. 2010;22(8):1248–64.
Wechsler D. Wechsler Adult Intelligence Scale-III. San Antonio: The Psychological Corporation. 1997a.
Strauss E, Sherman EMS, Spreen O. A compendium of neuropsychological tests: Administration, norms, and commentary, 3rd ed. New York, NY, US: Oxford University Press; 2006. xvii, 1216-xvii, p.
Wechsler D. Wechsler Memory Scale. Third edition manual. San Antonio: The Psychological Corporation. 1997b.
Manna CBG, Filangieri CM, Borod JC, Alterescu K, Allison Bender H. Benton Visual Retention Test. In: Kreutzer J, DeLuca J, Caplan B, editors. Encyclopedia of Clinical Neuropsychology. Cham: Springer International Publishing; 2017. p. 1–4.
Kaplan E. The Boston Naming Test. Philadelphia: Lippincott Williams Wilkins. 2001.
Wechsler D. WAIS-R manual. New York: The Psychological Corporation. 1981.
Hodge A, Patterson AJ, Brown WJ, Ireland P, Giles G. The Anti Cancer Council of Victoria FFQ: relative validity of nutrient intakes compared with weighed food records in young to middle-aged women in a study of iron supplementation. Australian and New Zealand journal of public health. 2000;24(6):576–83.
Xinying P, Noakes M, Keogh J. Can a food frequency questionnaire be used to capture dietary intake data in a 4 week clinical intervention trial? Asia Pacific journal of clinical nutrition. 2004;13:318–23.
Petersen KS, Smith JM, Clifton PM, Keogh JB. Dietary intake in adults with type 1 and type 2 diabetes: validation of the Dietary Questionnaire for Epidemiological Studies version 2 FFQ against a 3-d weighed food record and 24-h urinalysis. The British journal of nutrition. 2015;114(12):2056–63.
Food Standards Australia New Zealand. NUTTAB 2010 — Australian Food Composition Tables. Canberra: FSANZ. 2011.
Trichopoulou A, Kyrozis A, Rossi M, Katsoulis M, Trichopoulos D, La Vecchia C, et al. Mediterranean diet and cognitive decline over time in an elderly Mediterranean population. Eur J Nutr. 2015;54(8):1311–21.
Trichopoulou A, Costacou T, Bamia C, Trichopoulos D. Adherence to a Mediterranean diet and survival in a Greek population. N Engl J Med. 2003;348(26):2599–608.
Panagiotakos DB, Pitsavos C, Arvaniti F, Stefanadis C. Adherence to the Mediterranean food pattern predicts the prevalence of hypertension, hypercholesterolemia, diabetes and obesity, among healthy adults; the accuracy of the MedDietScore. Prev Med. 2007;44(4):335–40.
Willett W, Stampfer MJ. Total energy intake: implications for epidemiologic analyses. Am J Epidemiol. 1986;124(1):17–27.
Fung TT, Chiuve SE, McCullough ML, Rexrode KM, Logroscino G, Hu FB. Adherence to a DASH-style diet and risk of coronary heart disease and stroke in women. Archives of internal medicine. 2008;168(7):713–20.
Berendsen AAM, Kang JH, van de Rest O, Feskens EJM, de Groot L, Grodstein F. The Dietary Approaches to Stop Hypertension Diet, Cognitive Function, and Cognitive Decline in American Older Women. J Am Med Dir Assoc. 2017;18(5):427–32.
Siervo M, Lara J, Chowdhury S, Ashor A, Oggioni C, Mathers JC. Effects of the Dietary Approach to Stop Hypertension (DASH) diet on cardiovascular risk factors: a systematic review and meta-analysis. The British journal of nutrition. 2015;113(1):1–15.
Saneei P, Salehi-Abargouei A, Esmaillzadeh A, Azadbakht L. Influence of Dietary Approaches to Stop Hypertension (DASH) diet on blood pressure: a systematic review and meta-analysis on randomized controlled trials. Nutr Metab Cardiovasc Dis. 2014;24(12):1253–61.
Thorpe MG, Milte CM, Crawford D, McNaughton SA. A Revised Australian Dietary Guideline Index and Its Association with Key Sociodemographic Factors, Health Behaviors and Body Mass Index in Peri-Retirement Aged Adults. Nutrients. 2016;8(3):160.
Thorpe MG, Milte CM, Crawford D, McNaughton SA. A comparison of the dietary patterns derived by principal component analysis and cluster analysis in older Australians. International Journal of Behavioral Nutrition and Physical Activity. 2016;13(1):30.
Peterson RA. A Meta-Analysis of Variance Accounted for and Factor Loadings in Exploratory Factor Analysis. Marketing Letters. 2000;11(3):261–75.
Mazza E, Fava A, Ferro Y, Moraca M, Rotundo S, Colica C, et al. Impact of legumes and plant proteins consumption on cognitive performances in the elderly. J Transl Med. 2017;15(1):109.
Rabassa M, Zamora-Ros R, Palau-Rodriguez M, Tulipani S, Minarro A, Bandinelli S, et al. Habitual Nut Exposure, Assessed by Dietary and Multiple Urinary Metabolomic Markers, and Cognitive Decline in Older Adults: The InCHIANTI Study. Mol Nutr Food Res. 2019:e1900532.
O’Brien J, Okereke O, Devore E, Rosner B, Breteler M, Grodstein F. Long-term intake of nuts in relation to cognitive function in older women. J Nutr Health Aging. 2014;18(5):496–502.
Neergaard JS, Dragsbæk K, Christiansen C, Nielsen HB, Brix S, Karsdal MA, et al. Metabolic Syndrome, Insulin Resistance, and Cognitive Dysfunction: Does Your Metabolic Profile Affect Your Brain? Diabetes. 2017;66(7):1957–63.
Spielman LJ, Gibson DL, Klegeris A. Unhealthy gut, unhealthy brain: The role of the intestinal microbiota in neurodegenerative diseases. Neurochem Int. 2018;120:149–63.
Gardener SL, Rainey-Smith SR, Barnes MB, Sohrabi HR, Weinborn M, Lim YY, et al. Dietary patterns and cognitive decline in an Australian study of ageing. Mol Psychiatry. 2015;20(7):860–6.
Valls-Pedret C, Sala-Vila A, Serra-Mir M, Corella D, de la Torre R, Martinez-Gonzalez MA, et al. Mediterranean diet and age-related cognitive decline: A randomized clinical trial. JAMA Intern Med. 2015;175(7):1094–103. doi:https://doi.org/10.0001/jamainternmed.2015.1668. Published online May, 2015.Corrected November, 8.
Tangney CC, Li H, Wang Y, Barnes L, Schneider JA, Bennett DA, et al. Relation of DASH- and Mediterranean-like dietary patterns to cognitive decline in older persons. Neurology. 2014;83(16):1410–6.
Lebouvier T, Chen Y, Duriez P, Pasquier F, Bordet R. Antihypertensive agents in Alzheimer’s disease: beyond vascular protection. Expert Rev Neurother. 2020;20(2):175–87.
Imamura F, Micha R, Wu JHY, de Oliveira Otto MC, Otite FO, Abioye AI, et al. Effects of Saturated Fat, Polyunsaturated Fat, Monounsaturated Fat, and Carbohydrate on Glucose-Insulin Homeostasis: A Systematic Review and Meta-analysis of Randomised Controlled Feeding Trials. PLOS Medicine. 2016;13(7):e1002087.
Julibert A, Bibiloni MdM, Tur JA. Dietary fat intake and metabolic syndrome in adults: A systematic review. Nutrition, Metabolism and Cardiovascular Diseases. 2019;29(9):887–905.
Olsson E, Karlstrom B, Kilander L, Byberg L, Cederholm T, Sjogren P. Dietary patterns and cognitive dysfunction in a 12-year follow-up study of 70 year old men. J Alzheimers Dis. 2015;43(1):109–19.
Haring B, Wu C, Mossavar-Rahmani Y, Snetselaar L, Brunner R, Wallace RB, et al. No Association between Dietary Patterns and Risk for Cognitive Decline in Older Women with 9-Year Follow-Up: Data from the Women’s Health Initiative Memory Study. J Acad Nutr Diet. 2016;116(6):921–30.e1.
Ronksley PE, Brien SE, Turner BJ, Mukamal KJ, Ghali WA. Association of alcohol consumption with selected cardiovascular disease outcomes: a systematic review and meta-analysis. BMJ. 2011;342:d671.
Mostofsky E, Chahal HS, Mukamal KJ, Rimm EB, Mittleman MA. Alcohol and Immediate Risk of Cardiovascular Events: A Systematic Review and Dose-Response Meta-Analysis. Circulation. 2016;133(10):979–87.
Santangelo C, Vari R, Scazzocchio B, De Sanctis P, Giovannini C, D’Archivio M, et al. Anti-inflammatory Activity of Extra Virgin Olive Oil Polyphenols: Which Role in the Prevention and Treatment of Immune-Mediated Inflammatory Diseases? Endocr Metab Immune Disord Drug Targets. 2018;18(1):36–50.
Sabia S, Elbaz A, Britton A, Bell S, Dugravot A, Shipley M, et al. Alcohol consumption and cognitive decline in early old age. Neurology. 2014;82(4):332–9.
Acknowledgements
Participants, staff and investigators of the Sydney Memory and Ageing Study are gratefully acknowledged.
Funding
Funding: Sydney Memory and Ageing Study received funding from the National Health and Medical Research Council (NHMRC) Australia.
Author information
Authors and Affiliations
Contributions
Author contributions: XC designed the research protocol, conducted data analysis, drafted the protocol and report, including creating reference list and tables. ZXL was responsible for technical support on statistical analysis, interpreting results and providing comments on manuscript. PS and NK were responsible for project design, data collection and study coordination, critical revision of manuscript. FOL provided support on dietary pattern score construction, data analysis, interpretation of results, critical revision of manuscript and approval of report. HB was responsible for designing the research protocol, interpreting results, critical revision and final approval of report. All authors reviewed the final draft.
Corresponding author
Ethics declarations
Conflict of interest: Henry Brodaty is an Advisory Board member for Nutricia. None declared by other authors.
Declaration: This study complies with the current laws of Australia where research was performed.
Ethical standards: The study was approved by the Ethics Committees of the University of New South Wales and the South Eastern Sydney and Illawarra Area Health Service.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Chen, X., Liu, Z., Sachdev, P.S. et al. Dietary Patterns and Cognitive Health in Older Adults: Findings from the Sydney Memory and Ageing Study. J Nutr Health Aging 25, 255–262 (2021). https://doi.org/10.1007/s12603-020-1536-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-020-1536-8