Abstract
Background
Motoric Cognitive Risk Syndrome (MCR), slow gait speed (SG) and subjective cognitive decline (SCD) are known to be harbingers of dementia. MCR is known to be associated with a 3-fold increased risk of future dementia, while SG can precede cognitive impairment.
Objective
We aim to determine the prevalence and demographics of MCR, slow gait alone (SG-A) and subjective cognitive decline alone (SCD-A) in community-dwelling older adults and association with physical, functional, cognition and psychosocial factors.
Methods
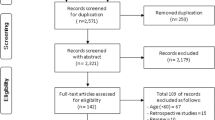
A total of 509 participants were classified into four groups according to presence of SG and/or SCD. Multinomial logistic regression was used to identify the factors associated with SG-A, SCD-A and MCR.
Results
The prevalence of MCR was 13.6%, SG-A 13.0% and SCD-A 35.0%. Prevalence of MCR doubled every decade in females with 27.7% of female ≥ 80 years old had MCR. Almost 4 in 10 had no SG or SCD (SG+SCD negative). MCR and SG-A groups were significantly older, had higher body mass index (BMI), lower education, lower global cognition scores especially in non-memory domains, higher prevalence of low grip strength and lower short physical performance battery scores than those with SCD-A and SG+SCD negative. In addition, the SG-A group had significantly higher prevalence of multi-morbidity and diabetes. The prevalence of pain, depression, frailty, social isolation and activity of daily living impairment were significantly higher in MCR. The global cognitive and functional scores for those with SCD-A were comparable to the SG+SCD negative group. The Malay ethnic group had the lowest prevalence of SCD but highest prevalence of SG. After adjusting for confounding factors, age, BMI, frailty status, instrumental activity of daily living, depression and pain remained significantly associated with MCR. For SG-A, age, BMI, education and number of chronic diseases remained significant.
Conclusion
Both MCR and SG-A are associated with global cognitive decline especially in the non-memory domains and lower functional scores. Gait speed is a good predictor of negative outcomes and should be considered as the ‘sixth’ vital sign. Long term prospective studies are needed to evaluate: i) the conversion to dementia in different ethnic groups and ii) effect of targeted physical and/or dual task exercise on delaying the conversion to dementia and/or improvement in physical measures and reduction of disability.


Similar content being viewed by others
References
Patterson C. World Alzheimer report 2018: the state of the art of dementia research: new frontiers. Alzheimer’s Disease International (ADI): London, UK. 2018:32–6.
Montero-Odasso M, Ismail Z, Livingston G. One third of dementia cases can be prevented within the next 25 years by tackling risk factors. The case “for” and “against”. Alzheimers Res Ther. 2020;12(1):81.
Ahmadi-Abhari S, Guzman-Castillo M, Bandosz P, Shipley MJ, Muniz-Terrera G, Singh-Manoux A, et al. Temporal trend in dementia incidence since 2002 and projections for prevalence in England and Wales to 2040: modelling study. Bmj. 2017;358:j2856.
Montero-Odasso M, Speechley M, Muir-Hunter SW, Pieruccini-Faria F, Sarquis-Adamson Y, Hachinski V, et al. Dual decline in gait speed and cognition is associated with future dementia: evidence for a phenotype. Age Ageing. 2020.
Si T, Xing G, Han Y. Subjective Cognitive Decline and Related Cognitive Deficits. Front Neurol. 2020;11:247.
Jessen F, Amariglio RE, Buckley RF, van der Flier WM, Han Y, Molinuevo JL, et al. The characterisation of subjective cognitive decline. Lancet Neurol. 2020;19(3):271–8.
Verghese J, Ayers E, Barzilai N, Bennett DA, Buchman AS, Holtzer R, et al. Motoric cognitive risk syndrome: Multicenter incidence study. Neurology. 2014;83(24):2278–84.
Maguire FJ, Killane I, Creagh AP, Donoghue O, Kenny RA, Reilly RB. Baseline Association of Motoric Cognitive Risk Syndrome With Sustained Attention, Memory, and Global Cognition. J Am Med Dir Assoc. 2018;19(1):53–8.
Shim H, Kim M, Won CW. Motoric cognitive risk syndrome is associated with processing speed and executive function, but not delayed free recall memory: The Korean frailty and aging cohort study (KFACS). Archives of gerontology and geriatrics. 2020;87:103990.
Doi T, Shimada H, Makizako H, Tsutsumimoto K, Verghese J, Suzuki T. Motoric Cognitive Risk Syndrome: Association with Incident Dementia and Disability. J Alzheimers Dis. 2017;59(1):77–84.
Maggio M, Lauretani F. Prevalence, incidence, and clinical impact of cognitive-motoric risk syndrome in Europe, USA, and Japan: facts and numbers update 2019. J Cachexia Sarcopenia Muscle. 2019;10(5):953–5.
Beauchet O, Sekhon H, Schott AM, Rolland Y, Muir-Hunter S, Markle-Reid M, et al. Motoric Cognitive Risk Syndrome and Risk for Falls, Their Recurrence, and Postfall Fractures: Results From a Prospective Observational Population-Based Cohort Study. J Am Med Dir Assoc. 2019;20(10):1268–73.
Chhetri JK, Chan P, Vellas B, Cesari M. Motoric Cognitive Risk Syndrome: Predictor of Dementia and Age-Related Negative Outcomes. Frontiers in medicine. 2017;4:166.
Grande G, Triolo F, Nuara A, Welmer AK, Fratiglioni L, Vetrano DL. Measuring gait speed to better identify prodromal dementia. Exp Gerontol. 2019;124:110625.
Buracchio T, Dodge HH, Howieson D, Wasserman D, Kaye J. The trajectory of gait speed preceding mild cognitive impairment. Arch Neurol. 2010;67(8):980–6.
Dent E, Morley JE, Cruz-Jentoft AJ, Arai H, Kritchevsky SB, Guralnik J, et al. International Clinical Practice Guidelines for Sarcopenia (ICFSR): Screening, Diagnosis and Management. The journal of nutrition, health & aging. 2018;22(10):1148–61.
Morley JE, Malmstrom TK, Miller DK. A simple frailty questionnaire (FRAIL) predicts outcomes in middle aged African Americans. The journal of nutrition, health & aging. 2012;16(7):601–8.
Malmstrom TK, Morley JE. SARC-F: a simple questionnaire to rapidly diagnose sarcopenia. Journal of the American Medical Directors Association. 2013;14(8):531–2.
Allen N, Ames D, Ashby D, Bennetts K, Tuckwell V, West C. A brief sensitive screening instrument for depression in late life. Age Ageing. 1994;23(3):213–9.
Shelkey M, Wallace M. Katz Index of Independence in Activities of Daily Living. J Gerontol Nurs. 1999;25(3):8–9.
Lawton AR, 3rd, Mage RG. The synthesis of secretory IgA in the rabbit. I. Evidence for synthesis as an 11 S dimer. J Immunol. 1969;102(3):693–7.
Lubben J, Blozik E, Gillmann G, Iliffe S, von Renteln Kruse W, Beck JC, et al. Performance of an abbreviated version of the Lubben Social Network Scale among three European community-dwelling older adult populations. The Gerontologist. 2006;46(4):503–13.
Topolski TD, LoGerfo J, Patrick DL, Williams B, Walwick J, Patrick MB. The Rapid Assessment of Physical Activity (RAPA) among older adults. Preventing chronic disease. 2006;3(4):A118.
Chen LK, Woo J, Assantachai P, Auyeung TW, Chou MY, Iijima K, et al. Asian Working Group for Sarcopenia: 2019 Consensus Update on Sarcopenia Diagnosis and Treatment. Journal of the American Medical Directors Association. 2020.
Sekhon H, Allali G, Launay CP, Barden J, Szturm T, Liu-Ambrose T, et al. Motoric cognitive risk syndrome, incident cognitive impairment and morphological brain abnormalities: Systematic review and meta-analysis. Maturitas. 2019;123:45–54.
Blumen HM, Allali G, Beauchet O, Lipton RB, Verghese J. A Gray Matter Volume Covariance Network Associated with the Motoric Cognitive Risk Syndrome: A Multicohort MRI Study. J Gerontol A Biol Sci Med Sci. 2019;74(6):884–9.
Aguilar-Navarro SG, Mimenza-Alvarado AJ, Aguilar-Esquivel JE, Yeverino-Castro SG, Juarez-Cedillo T, Mejia-Arango S. Motoric Cognitive Risk Syndrome: Prevalence and Risk of Cognitive Impairment in a Population Studied in the Mexican Health and Aging Study 2012–2015. J Nutr Health Aging. 2019;23(3):227–31.
Shim H, Kim M, Won CW. Motoric cognitive risk syndrome is associated with processing speed and executive function, but not delayed free recall memory: The Korean frailty and aging cohort study (KFACS). Arch Gerontol Geriatr. 2020;87:103990.
van der Leeuw G, Ayers E, Blankenstein AH, van der Horst HE, Verghese J. The association between pain and prevalent and incident motoric cognitive risk syndrome in older adults. Arch Gerontol Geriatr. 2020;87:103991.
Doi T, Verghese J, Shimada H, Makizako H, Tsutsumimoto K, Hotta R, et al. Motoric Cognitive Risk Syndrome: Prevalence and Risk Factors in Japanese Seniors. J Am Med Dir Assoc. 2015;16(12):1103 e21–5.
Kyrönlahti SM, Stenholm S, Raitanen J, Neupane S, Koskinen S, Tiainen K. Educational Differences in Decline in Maximum Gait Speed in Older Adults over an 11-year Follow-up. J Gerontol A Biol Sci Med Sci. 2020.
Fritz S, Lusardi M. White paper: “walking speed: the sixth vital sign”. J Geriatr Phys Ther. 2009;32(2):46–9.
Topiwala A, Suri S, Allan C, Zsoldos E, Filippini N, Sexton CE, et al. Subjective Cognitive Complaints Given in Questionnaire: Relationship With Brain Structure, Cognitive Performance and Self-Reported Depressive Symptoms in a 25-Year Retrospective Cohort Study. Am J Geriatr Psychiatry. 2020.
Caramelli P, Beato RG. Subjective memory complaints and cognitive performance in a sample of healthy elderly. Dement Neuropsychol. 2008;2(1):42–5.
Nester C, Ayers E, Rabin L, Verghese J. Non-memory subjective cognitive concerns predict incident motoric cognitive risk syndrome. Eur J Neurol. 2020.
Merchant RA, Chan YH, Lim JY, Morley JE. Prevalence of Metabolic Syndrome and Association with Grip Strength in Older Adults: Findings from the HOPE Study. Diabetes Metab Syndr Obes. 2020;13:2677–86.
Callisaya ML, Ayers E, Barzilai N, Ferrucci L, Guralnik JM, Lipton RB, et al. Motoric Cognitive Risk Syndrome and Falls Risk: A Multi-Center Study. J Alzheimers Dis. 2016;53(3):1043–52.
Shim H, Kim M, Won CW. Motoric Cognitive Risk Syndrome Using Three-Item Recall Test and Its Associations with Fall-Related Outcomes: The Korean Frailty and Aging Cohort Study. Int J Environ Res Public Health. 2020;17(10).
Sekhon H, Allali G, Beauchet O. The association of anxio-depressive disorders and depression with motoric cognitive risk syndrome: results from the baseline assessment of the Canadian longitudinal study on aging. Geroscience. 2019;41(4):409–18.
Buchman AS, Shah RC, Leurgans SE, Boyle PA, Wilson RS, Bennett DA. Musculoskeletal pain and incident disability in community-dwelling older adults. Arthritis Care Res (Hoboken). 2010;62(9):1287–93.
Shen S, Zeng X, Xu L, Chen L, Liu Z, Chu J, et al. Association between motoric cognitive risk syndrome and frailty among older Chinese adults. BMC Geriatr. 2020;20(1):110.
Hardy R, Cooper R, Aihie Sayer A, Ben-Shlomo Y, Cooper C, Deary IJ, et al. Body mass index, muscle strength and physical performance in older adults from eight cohort studies: the HALCyon programme. PLoS One. 2013;8(2):e56483.
Sathyan S, Wang T, Ayers E, Verghese J. Genetic basis of motoric cognitive risk syndrome in the Health and Retirement Study. Neurology. 2019;92(13):e1427–e34.
Sheng C, Yang K, Wang X, Li H, Li T, Lin L, et al. Advances in Non-Pharmacological Interventions for Subjective Cognitive Decline: A Systematic Review and Meta-Analysis. J Alzheimers Dis. 2020.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest: All authors declare no conflict of interest.
Ethical standards: The study protocol was approved by the local National Healthcare Group (NHG) Domain Specific Review Board (DSRB) whose requirements are based on Declaration of Helsinki and the ethical principles in the Belmont Report. All participants signed a consent form.
Electronic Supplementary Material
Rights and permissions
About this article
Cite this article
Merchant, R.A., Goh, J., Chan, Y.H. et al. Slow Gait, Subjective Cognitive Decline and Motoric Cognitive Risk Syndrome: Prevalence and Associated Factors in Community Dwelling Older Adults. J Nutr Health Aging 25, 48–56 (2021). https://doi.org/10.1007/s12603-020-1525-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12603-020-1525-y