Abstract
Background
The purpose of this study was to investigate associations between right ventricular (RV) function and left ventricular (LV) diastolic function in patients with reduced LV ejection fraction (LVEF) and preserved LVEF.
Methods
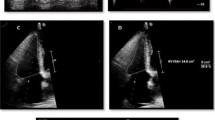
A total of 139 patients who had undergone echocardiography were recruited. LV diastolic function was determined as the ratio of mitral inflow E to mitral e′ lateral annular velocities (E/e′). RV function was determined as the RV index of myocardial performance (RIMP). Patients were divided into two groups: the preserved LVEF group (n = 100, LVEF ≥ 50%) and the reduced LVEF group (n = 39, LVEF < 50%).
Results
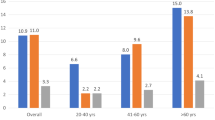
Associations between RV function and LV diastolic function in patients with reduced LVEF and preserved LVEF differed significantly. RIMP correlated significantly with E/e′ in patients with reduced LVEF (r = 0.47, p = 0.003), but not in those with preserved LVEF (r = 0.04, p = 0.68). An important finding of the multivariate regression analysis showed that RIMP was the only independent determinant of E/e′ in patients with reduced LVEF, whereas age and gender (not RIMP) was the independent determinant of E/e′ in patients with preserved LVEF.
Conclusions
Associations between RV function and LV diastolic function in patients with reduced LVEF and preserved LVEF differed significantly, and RV function showed a close correlation with LV diastolic function in patients with reduced LVEF, but not in those with preserved LVEF. Thus, these findings may well have clinical implications for better management of patients with reduced LVEF.


Similar content being viewed by others
References
Di Salvo TG, Mathier M, Semigran MJ, Dec GW. Preserved right ventricular ejection fraction predicts exercise capacity and survival in advanced heart failure. J Am Coll Cardiol. 1995;25(5):1143–53.
Gorcsan J 3rd, Murali S, Counihan PJ, Mandarino WA, Kormos RL. Right ventricular performance and contractile reserve in patients with severe heart failure. Assessment by pressure-area relations and association with outcome. Circulation. 1996;94(12):3190–7.
Kjaergaard J, Akkan D, Iversen KK, Kober L, Torp-Pedersen C, Hassager C. Right ventricular dysfunction as an independent predictor of short- and long-term mortality in patients with heart failure. Eur J Heart Fail. 2007;9(6–7):610–6.
Meyer P, Filippatos GS, Ahmed MI, et al. Effects of right ventricular ejection fraction on outcomes in chronic systolic heart failure. Circulation. 2010;121(2):252–8.
Mohammed SF, Hussain I, AbouEzzeddine OF, et al. Right ventricular function in heart failure with preserved ejection fraction: a community-based study. Circulation. 2014;130(25):2310–20.
Dohi K, Sugiura E, Ito M. Utility of strain-echocardiography in current clinical practice. J Echocardiogr. 2016;14(2):61–70.
Gavazzi A, Berzuini C, Campana C, et al. Value of right ventricular ejection fraction in predicting short-term prognosis of patients with severe chronic heart failure. J Heart Lung Transplant. 1997;16(7):774–85.
Nagueh SF, Smiseth OA, Appleton CP, et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2016;29(4):277–314.
Iglesias-Garriz I, Olalla-Gomez C, Garrote C, et al. Contribution of right ventricular dysfunction to heart failure mortality: a meta-analysis. Rev Cardiovasc Med. 2012;13(2–3):e62–9.
Matsumoto K, Tanaka H, Onishi A, et al. Bi-ventricular contractile reserve offers an incremental prognostic value for patients with dilated cardiomyopathy. Eur Heart J Cardiovasc Imaging. 2015;16(11):1213–23.
Galie N, Hinderliter AL, Torbicki A, et al. Effects of the oral endothelin-receptor antagonist bosentan on echocardiographic and doppler measures in patients with pulmonary arterial hypertension. J Am Coll Cardiol. 2003;41(8):1380–6.
Gurudevan SV, Malouf PJ, Auger WR, et al. Abnormal left ventricular diastolic filling in chronic thromboembolic pulmonary hypertension: true diastolic dysfunction or left ventricular underfilling? J Am Coll Cardiol. 2007;49(12):1334–9.
Motoji Y, Tanaka H, Fukuda Y, et al. Interdependence of right ventricular systolic function and left ventricular filling and its association with outcome for patients with pulmonary hypertension. Int J Cardiovasc Imaging. 2015;31(4):691–8.
Setaro JF, Cleman MW, Remetz MS. The right ventricle in disorders causing pulmonary venous hypertension. Cardiol Clin. 1992;10(1):165–83.
Klima UP, Guerrero JL, Vlahakes GJ. Myocardial perfusion and right ventricular function. Ann Thorac Cardiovasc Surg. 1999;5(2):74–80.
Voelkel NF, Quaife RA, Leinwand LA, et al. Right ventricular function and failure: report of a National Heart, Lung, and Blood Institute Working Group on cellular and molecular mechanisms of right heart failure. Circulation. 2006;114(17):1883–91.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Tsumugi Oki, Hidekazu Tanaka, Takamitsu Imanishi, Yuji Nakamachi, Jun Saegusa, Seiji Kawano, Ken-ichi Hirata, and Yoshihiro Nishimura declare that they have no conflict of interest.
Funding
Tsumugi Oki, Hidekazu Tanaka, Takamitsu Imanishi, Yuji Nakamachi, Jun Saegusa, Seiji Kawano, Ken-ichi Hirata, and Yoshihiro Nishimura declare that they receive no fundings.
Human rights statement
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1964 and later revisions.
Informed consent
Informed consent was obtained from all patients for being included in the study.
Rights and permissions
About this article
Cite this article
Oki, T., Tanaka, H., Imanishi, T. et al. Associations between left ventricular diastolic function and right ventricular function in patients with and without preserved left ventricular ejection fraction. J Echocardiogr 16, 81–86 (2018). https://doi.org/10.1007/s12574-017-0363-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12574-017-0363-3