Abstract
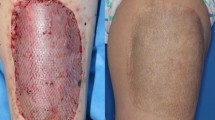
Split thickness skin graft (STSG) is a key method in the reconstructive ladder for covering skin defects used widely by surgeons from all specialties. The donor site is often a source of delayed healing, associated with considerable pain and discomfort even more than the recipient wound. The aim of this prospective randomized controlled study was to compare Helicoll® (EnColl Corp., Fremont, CA, USA), a type I pure collagen dressing, to OpSite® (Smith & Nephew, USA) dressing and to Scarlet Red® (Kendall HealthCare, USA) dressing in the treatment of standardized STSG donor sites. Thirty patients, over a 3-month period, underwent various reconstructive procedures, necessitating the use of STSGs. Following a simple randomized clinical protocol, the analysis of data included donor site pain, healing time of the donor site, initial absorption of the applied dressing and rate of infection with the three different dressings to form the basis of this paper. Patients in the Helicoll group reported significantly less pain, less infection rate and required no dressing change when compared with the OpSite (Johnson & Johnson, Langhorne, PA, USA) or the Scarlet Red groups. Healing time of the donor site in the Helicoll group was shorter than that in the Scarlet Red group; however, it was comparable to the OpSite group. This study indicates that Helicoll, as a donor site dressing, is successful in providing pain-free mobility with a measurable healing rate.













Similar content being viewed by others
References
Davies JW (1983) Synthetic materials for covering burn wounds: progress towards perfection. Part I. Short term dressing materials. Burns Incl Therm Inj 10(2):94–103
Hickerson WL, Kealey GP, Smith DJ Jr, Thomson PD (1994) A prospective comparison of a new synthetic donor site dressing versus an impregnated gauze dressing. J Burn Care Rehabil 15(4):359–363
Feldman DL, Rogers A, Karpinski RH (1991) A prospective trial comparing Biobrane, Duoderm and xeroform for skin graft donor sites. Surg Gynecol Obstet 173(1):1–5
Kilinc H, Sensoz O, Ozdemir R, Unlu RE, Baran C (2001) Which dressing for split-thickness skin graft donor sites? Ann Plast Surg 46(4):409–414
Friedman GD, Capozzi A, Pennisi VR (1974) Care of the split-thickness skin graft donor site. J Trauma 14(2):163–167
Person K, Salemark L (2000) How to dress donor sites of split thickness skin grafts: a prospective, randomised study of four dressings. Scand J Plast Reconstr Surg Hand Surg 34(1):55–59
Brady SC, Snelling CF, Chow G (1980) Comparison of donor site dressings. Ann Plast Surg 5(3):238–243
Winter GD (1962) Formation of the scab and the rate of epithelization of superficial wounds in the skin of the young domestic pig. J Wound Care 4(8):366–367, discussion 368–371
Lawrence JE, Blake GB (1991) A comparison of calcium alginate and scarlet red dressings in the formation of the scab and the rate of epithelization of superficial wounds in the skin of the young domestic pig healing of split thickness skin graft donor sites. Br J Plast Surg 44(4):247–249
Barnett A, Berkowitz RL, Mills R, Vistnes LM (1983) Comparison of synthetic adhesive moisture vapor permeable and fine mesh gauze dressings for split-thickness skin graft donor sites. Am J Surg 145(3):379–381
Ponten B, Nordgaard JO (1976) The use of collagen film (Cutycol) as a dressing for donor areas in split skin grafting. Scand J Plast Reconstr Surg 10(3):237–240
Prasad JK, Feller I, Thomson PD (1987) A prospective controlled trial of Biobrane versus scarlet red on skin graft donor areas. J Burn Care Rehabil 8(5):384–386
James JH, Watson AC (1975) The use of OpSite, a vapour permeable dressing, on skin graft donor sites. Br J Plast Surg 28(2):107–110
Weber RS, Hankins P, Limit one E et al (1995) Split-thickness skin graft donor site management. A randomized prospective trial comparing a hydrophilic polyurethane absorbent foam dressing with a petrolatum gauze dressing. Arch Otolaryngol Head Neck Surg 121(10):1145–1149
Gunasekaran S, Kwolek M, Dhanikachalam A (2006) A comparative second-degree burn treatment trial collagen dressing vs. silver sulphadiazine alone. Presented at the 31st Annual Meeting of Society of Biomaterials, Pittsburgh, PA, USA.
Gunasekaran S, Rajendran MK, Swaminathan T, Dhawan S (2003) Modified collagen for burns enhances healing rate possibly by cell signaling. Presented at the American Society for Dermatologic Surgery Annual Meeting.
Salisbury RE, Wilmore DW, Silverstein P, Pruitt BA Jr (1973) Biological dressings for skin graft donor sites. Arch Surg 106(5):705–706
Leicht P, Siim E, Sorensen B (1989) Treatment of donor sites—Duoderm or Omiderm? Burns Incl Therm Inj 15(1):7–10
Vanstraelen P (1992) Comparison of calcium sodium alginate (KALTOSTAT) and porcine xenograft (E-Z DERM) in the healing of split-thickness skin graft donor sites. Burns 18(2):145–148
Chang H, Wind S, Kerstein MD (1996) Moist wound healing. Dermatol Nurs 8(3):174–176
Innes ME, Umraw N, Fish JS, Gomez M, Cartotto RC (2001) The use of silver coated dressings on donor site wounds: a prospective, controlled matched pair study. Burns 27(6):621–627
Varma SK, Henderson HP, Hankins CL (1991) Calcium alginate as a dressing for mini skin grafts (skin soup). Br J Plast Surg 44(1):55–56
Feldman DL (1991) Which dressing for split-thickness skin graft donor sites? Ann Plast Surg 27(3):288–291
Attwood AI (1989) Calcium alginate dressing accelerates split skin graft donor site healing. Br J Plast Surg 42(4):373–379
Bettinger D, Gore D, Humphries Y (1995) Evaluation of calcium alginate for skin graft donor sites. J Burn Care Rehabil 16(1):59–61
Disa JJ, Alizadeh K, Smith JW, Hu Q, Cordeiro PG (2001) Evaluation of a combined calcium sodium alginate and bio-occlusive membrane dressing in the management of split-thickness skin graft donor sites. Ann Plast Surg 46(4):405–408
Freshwater MF, Su CT, Hopes JE (1978) A comparison of polyurethane foam dressing and fine mesh gauze in the healing of donor sites. Plast Reconstr Surg 61(2):275–276
Tan ST, Roberts RH, Blake GB (1993) Comparing Duo DERM E with scarlet red in the treatment of split skin graft donor sites. Br J Plast Surg 46(1):79–81
Dinner MI, Peters CR, Sherer J (1979) Use of a semipermeable polyurethane membrane as a dressing for split-skin graft donor sites. Plast Reconstr Surg 64(1):112–114
Klein RL, Rothmann BF, Marshall R (1984) Biobrane—a useful adjunct in the therapy of outpatient burns. J Pediatr Surg 19(6):846–847
Zapata-Sirvent R, Hansbrough JF, Carroll W, Johnson R, Wakimoto A (1985) Comparison of Biobrane and Scarlet Red dressings for treatment of donor site wounds. Arch Surg 120(6):743–745
Horch RE, Stark GB (1998) Comparison of the effect of a collagen dressing and a polyurethane dressing on the healing of split thickness skin graft (STSG) donor sites. Scand J Plast Reconstruct Surg Hand Surg 32(4):407–413
Dyson M, Young SR, Hart J, Lynch JA, Lang S (1992) Comparison of the effects of moist and dry conditions on the process of angiogenesis during dermal repair. J Invest Dermatol 99(6):729–733
Young T, Fowler A (1998) Nursing management of skin grafts and donor sites. Br J Nurs 7(6):324–326, 328, 330 passim
Acknowledgements
This study has been conducted solely for research purposes and this study was not sponsored by any product distributor or manufacturer. Accordingly, there have been no conflicts of interest in this research study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Dhanraj, P. A Clinical Study Comparing Helicoll with Scarlet Red and OpSite in the Treatment of Split Thickness Skin Graft Donor Sites—A Randomized Controlled Trial. Indian J Surg 77 (Suppl 2), 385–392 (2015). https://doi.org/10.1007/s12262-013-0850-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-013-0850-3