Abstract
Purpose
The aim of this study was to investigate the effectiveness of a planning intervention (specifying when, where, and how to act) and an implementation intention intervention (specifying the same in the format of an if-then plan) in increasing self-reported brushing in adolescents.
Methods
The study adopted a cluster randomized controlled trial design, and 1158 students in 48 schools were randomized to planning, implementation intention, or active control conditions. After baseline assessment, all participants received a leaflet containing information and recommendations on oral health and instructions on correct brushing behavior. After reading the leaflets, they were provided with a toothbrush and toothpaste plus a calendar in which to record their brushing. Participants in the planning condition and in the implementation intention condition also received instructions to form specific plans regarding brushing behavior. Self-reported brushing, perceived behavioral control, self-monitoring, intention, frequency of planning, oral health-related quality of life, and dental plaque and periodontal status were measured 1 and 6 months later.
Results
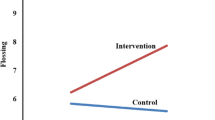
Both intervention conditions showed a significant improvement in the frequency of self-reported brushing, self-monitoring, frequency of planning, intention, perceived behavioral control, plaque index, periodontal health, and oral health-related quality of life compared to the control condition at both follow-ups. Comparing the two intervention conditions revealed that adolescents who received the implementation intention intervention had significantly greater improvement in the frequency of self-reported brushing, intention, frequency of planning, and periodontal health than those in planning condition.
Conclusions
Taken together, the findings suggest that forming implementation intentions as well as planning has the potential to increase dental self-reported brushing rates in adolescents, but that forming implementation intentions has the strongest impact on dental hygiene behavior and is, therefore, recommended.
Trial Registration Number
The trial was registered with the ClinicalTrials.gov database (NCT02066987) https://www.clinicaltrials.gov/ct2/show/NCT02066987.

Similar content being viewed by others
References
Petersen PE. World Health Organization global policy for improvement of oral health—World Health Assembly 2007. Int Dent J. 2008; 58(3): 115-121.
Ramsay P. The board of registration in dentistry. How to keep your dental practice out of trouble. J Mass Dent Soc. 2000; 49(2): 24-26.
Schüz B, Sniehotta FF, Wiedemann A, Seemann R. Adherence to a daily flossing regimen in university students: Effects of planning when, where, how and what to do in the face of barriers. J Clin Periodontol. 2006; 33(9): 612-619.
Ajzen I. The theory of planned behavior. Organ Behav Hum Decis Process. 1991; 50: 179-211.
Triandis HC. Interpersonal behavior. Monterey: Brooks/Cole; 1977.
Sheeran P, Orbell S. Do intentions predict condom use? Meta-analysis and examination of six moderator variables. Br J Soc Psychol. 1998; 37(2): 231-250.
Sheeran P. Intention—behavior relations: A conceptual and empirical review. Eur Rev Soc Psychol. 2002; 12: 1-36.
Webb TL, Sheeran P. Does changing behavioral intentions engender behavior change? A meta-analysis of the experimental evidence. Psychol Bull. 2006; 132: 249-268.
Gollwitzer PM, Sheeran P. Implementation intentions and goal achievement: A meta-analysis of effects and processes. Adv Exp Soc Psychol. 2006; 38: 69-119.
Sniehotta FF, Araújo Soares V, Dombrowski SU. Randomized controlled trial of a one-minute intervention changing oral self-care behavior. J Dent Res. 2007; 86(7): 641-645.
Webb TL, Sheeran P. How do implementation intentions promote goal attainment? A test of component processes. J Exp Soc Psychol. 2007; 43: 295-302.
Webb TL, Sheeran P. Mechanisms of implementation intention effects: the role of goal intentions, self-efficacy, and accessibility of plan components. Br J Soc Psychol. 2008; 47(Pt 3): 373-395.
Webb TL, Sheeran P. Identifying good opportunities to act: Implementation intentions and cue discrimination. Eur J Soc Psychol. 2004; 34: 407-419.
Gollwitzer PM. Implementation intentions: Strong effects of simple plans. Am Psychol. 1999; 54(7): 493-503.
Oettingen G, Hönig G, Gollwitzer PM. Effective self-regulation of goal attainment. Int J Educ Res. 2000; 33: 28.
Sheeran P, Milne S, Webb TL, et al. Implementation intentions and health behaviour: Bibliothek der Universität Konstanz. 2005.
Hagger MS, Luszczynska A. Implementation intention and action planning interventions in health contexts: State of the research and proposals for the way forward. Appl Psychol Health Well Being. 2014; 6(1): 1-47.
Campbell MK, Piaggio G, Elbourne DR, Altman DG, Group C. Consort 2010 statement: Extension to cluster randomised trials. BMJ. 2012; 345: e5661.
Poyato-Ferrera M, Segura-Egea JJ, Bullon-Fernandez P. Comparison of modified Bass technique with normal toothbrushing practices for efficacy in supragingival plaque removal. Int J Dent Hyg. 2003; 1(2): 110-114.
Pakpour AH, Sniehotta FF. Perceived behavioural control and coping planning predict dental brushing behaviour among Iranian adolescents. J Clin Periodontol. 2012; 39(2): 132-137.
Pakpour AH, Hidarnia A, Hajizadeh E, Plotnikoff RC. Action and coping planning with regard to dental brushing among Iranian adolescents. Psychol, Health Med. 2012; 17(2): 176-187.
Pakpour AH, Yekaninejad MS, Zarei F, Hashemi F, Steele MM, Varni JW. The PedsQL Oral Health Scale in Iranian children: Reliability and validity. Int J Paediatr Dentist / British Paedodontic Soc Int Assoc Dentistry Children. 2011; 21(5): 342-352.
Turesky S, Gilmore ND, Glickman I. Reduced plaque formation by the chloromethyl analogue of victamine C. J Periodontol. 1970; 41(1): 41-43.
Ainamo J, Barmes D, Beagrie G, Cutress T, Martin J, Sardo-Infirri J. Development of the World Health Organization (WHO) community periodontal index of treatment needs (CPITN). Int Dent J. 1982; 32(3): 281-291.
Benjamini Y, Hochberg Y. Controlling the false discovery rate: A practical and powerful approach to multiple testing. J R Stat Soc Ser B Stat Methodol. 1995; 57: 289-300.
Schüz B, Wiedemann AU, Mallach N, Scholz U. Effects of a short behavioural intervention for dental flossing: Randomized-controlled trial on planning when, where and how. J Clin Periodontol. 2009; 36(6): 498-505.
Pakpour AH, Hidarnia A, Hajizadeh E, Kumar S, Harrison AP. The status of dental caries and related factors in a sample of Iranian adolescents. Med Oral, Patol Oral y Cirugia Bucal. 2011; 16(6): e822-827.
Rothman AJ. Toward a theory-based analysis of behavioral maintenance. Health Psychol. 2000; 19(1 Suppl): 64-69.
Acknowledgments
The authors thank the schools, teachers, and children involved in the study. This study was funded by the Qazvin University of medical sciences, via a grant to Amir H Pakpour.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Authors’ Statement of Conflict of Interest and Adherence to Ethical Standards
Amir H. Pakpour, Maryam Gholami, Paul Gellert, Mir Saeed Yekaninejad, Stephan U. Dombrowski, and Thomas L. Webb declare that they have no conflict of interests. All procedures were carried out in compliance with the Helsinki Declaration. The study was approved by both the Ethics Committee of Qazvin University of Medical Sciences and the Organization for Education at Qazvin. All participants and their parents provided informed consent prior to participation, and all information about the participants was kept strictly confidential.
About this article
Cite this article
Pakpour, A.H., Gholami, M., Gellert, P. et al. The Effects of Two Planning Interventions on the Oral Health Behavior of Iranian Adolescents: A Cluster Randomized Controlled Trial. ann. behav. med. 50, 409–418 (2016). https://doi.org/10.1007/s12160-015-9767-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-015-9767-3