Abstract
Aim
Postoperative scanning may help to identify patients with differentiated thyroid cancer (DTC); however, low dose I-131 can lead to stunning and suboptimal response to ablative therapy. The aim of this retrospective study is to compare postablative I-131 scintigraphy with post-thyroidectomy Tc-99m pertechnetate scintigraphy, serum thyroglobulin (Tg) and antithyroglobulin antibody (TgAb) levels in patients with DTC.
Methods
Patients who had undergone surgical thyroidectomy for DTC were evaluated retrospectively. All patients had undergone Tc-99m pertechnetate and postablative I-131 scans. Serum Tg and TgAb levels were measured in all subjects. Preablative pertechnetate scans of the thyroid bed were viewed blindly and then directly compared with postablative I-131 scans and Tc-99m pertechnetate scintigraphy was compared with serum Tg and TgAb levels.
Results
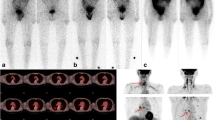
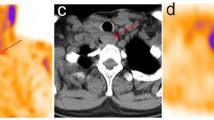
One hundred and seventy-four patients (146 women, 28 men) with a mean age of 48.7 ± 13.1 (range 12–84) years who had undergone surgical thyroidectomy for DTC were evaluated retrospectively. Of 174 patients, 6 (3 %) had negative I-131 and also Tc-99m pertechnetate scintigraphy results. Of the remaining 168 positive I-131 scans, 131 (75 %) were positive in at least one site on the pertechnetate scan, 19 (11 %) were considered to have equivocal uptake and 18 (11 %) were negative. For the per-site analysis, pertechnetate sites were considered to be accurately determined if they showed concordant uptake at sites that correlated precisely with those seen on the postablation I-131 scans. There were a total of 356 positive foci on I-131 scans. Of these, 273 foci (77 %) were unequivocally positive on pertechnetate scintigraphy, 41 (11 %) showed equivocal uptake and 42 (12 %) foci could not be detected. There were statistically significant differences (p < 0.0001) between the negative and positive foci in terms of Tg levels on pertechnetate sites.
Conclusions
A positive pertechnetate scan is, therefore, sufficient to guide progression to I-131 ablation in most patients. Pertechnetate scintigraphy may be of particular benefit if it is considered desirable to avoid use of I-131 in post-thyroidectomy remnant imaging. Tg level is an important parameter in the detection of remnant thyroid tissue in patients with DTC.



Similar content being viewed by others
References
Schlumberger MJ. Papillary and follicular thyroid carcinoma. N Engl J Med. 1998;338:297–306.
Pacini F, Schlumberger M, Dralle H, Elisei R, Smit JW, Wiersinga W, et al. European consensus for the management of patients with differentiated thyroid carcinoma of the follicular epithelium. Eur J Endocrinol. 2006;154:787–803.
Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, et al. Management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2006;16:109–42.
Brown RL. Standard and emerging therapeutic approaches for thyroid malignancies. Semin Oncol. 2008;35:298–308.
Kloos RT. Papillary thyroid cancer: medical management and follow-up. Curr Treat Options Oncol. 2005;6:323–38.
Bajén MT, Mañé S, Muñoz A, Garcia JR. Effect of a diagnostic dose of 185 MBq I-131 on postsurgical thyroid remnants. J Nucl Med. 2000;41:2038–42.
Verburg FA, Verkooijen RB, Stokkel MP, van Isselt JW. The success of 131I ablation in thyroid cancer patients is significantly reduced after a diagnostic activity of 40 MBq 131I. Nuklearmedizin. 2009;48:138–42.
Gulzar Z, Jana S, Young I, Bukberg P, Yen V, Naddaf S, et al. Neck and whole-body scanning with 5-mCi dose of (123)I as diagnostic tracer in patients with well-differentiated thyroid cancer. Endocr Pract. 2001;7:244–9.
Meller J, Becker W. The continuing importance of thyroid scintigraphy in the era of high-resolution ultrasound. Eur J Nucl Med Mol Imaging. 2002;29(Suppl 2):S425–38.
Luster M, Clarke SE, Dietlein M, Lassmann M, Lind P, Oyen WJ, et al. Guidelines for radioiodine therapy of differentiated thyroid cancer. Eur J Nucl Med Mol Imaging. 2008;35:1941–59.
Intenzo CM, Dam HQ, Manzone TA, Kim SM. Imaging of the thyroid in benign and malignant disease. Semin Nucl Med. 2012;42:49–61.
Lees W, Mansberg R, Roberts J, Towson J, Chua E, Turtle J. The clinical effects of thyroid stunning after diagnostic whole-body scanning with 185 MBq I-131. Eur J Nucl Med Mol Imaging. 2002;29:1421–7.
Muratet JP, Daver A, Minier JF, Larra F. Influence of scanning doses of iodine-131 on subsequent first ablative treatment outcome in patients operated on for differentiated thyroid carcinoma. J Nucl Med. 1998;39:1546–50.
Scott GC, Meier DA, Dickinson CZ. Cervical lymph node metastasis of thyroid papillary carcinoma imaged with fluorine-18-FDG, technetium-99m pertechnetate and iodine-131-sodium iodide. J Nucl Med. 1995;36:1843–5.
Carr HA, Temple TE, Staab EV. Early visualization of Tc-99m pertechnetate in metastatic thyroid cancer in a patient with Graves’ disease. J Nucl Med. 1971;12:40–2.
Verma N, Singh-Wadhwa S, Arvela OM. Metastatic thyroid cancer visualized on technetium pertechnetate and iodine-131 scintigraphy. Clin Nucl Med. 2002;27:610.
Vieras F. Preoperative scintigraphic detection of cervical metastases from thyroid carcinoma with technetium-99m pertechnetate. Clin Nucl Med. 1985;10:567–9.
Khammash NF, Halkar RK, Abdel-Dayem HM. The use of technetium-99m pertechnetate in postoperative thyroid carcinoma. A comparative study with iodine-131. Clin Nucl Med. 1988;13:17–22.
Kueh SS, Roach PJ, Schembri GP. Role of Tc-99m pertechnetate for remnant scintigraphy post-thyroidectomy. Clin Nucl Med. 2010;35:671–4.
Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiate thyroid cancer. Thyroid. 2009;19:1167–214.
Sawka AM, Thephamongkhol K, Brouwers M, Thabane L, Browman G, Gerstein HC. A systematic review and metaanalysis of the effectiveness of radioactive iodine remnant ablation for well-differentiated thyroid cancer. J Clin Endocrinol Metab. 2004;89:3668–76.
Sawka AM, Brierley JD, Tsang RW, Thabane L, Rotstein L, Gafni A, et al. An updated systematic review and commentary examining the effectiveness of radioactive iodine remnant ablation in well-differentiated thyroid cancer. Endocrinol Metab Clin North Am. 2008;37:457–80.
Kim S, Wei JP, Braveman JM, Brams DM. Predicting outcome and directing therapy papillary thyroid carcinoma. Arch Surg. 2004;139:390–4.
Sanders LE, Cady B. Differentiated thyroid cancer: reexamination of risk groups and outcome of treatment. Arch Surg. 1998;133:419–25.
Bilimoria KY, Bentrem DJ, Ko CY, Stewart AK, Winchester DP, Talamonti MS, et al. Extent of surgery affects survival for papillary thyroid cancer. Ann Surg. 2007;246:375–81.
Soh EY, Clark OH. Surgical considerations and approach to thyroid cancer. Endocrinol Metab Clin North Am. 1996;25:115–39.
Sywak M, Cornford L, Roach P, Stalberg P, Sidhu S, Delbridge L. Routine ipsilateral level VI lymphadenectomy reduces postoperative thyroglobulin levels in papillary thyroid cancer. Surgery. 2006;140:1000–7.
Neshandar Asli I, Siahkali AS, Shafie B, Javadi H, Assadi M. Prognostic value of basal serum thyroglobulin levels, but not basal antithyroglobulin antibody (tgab) levels, in patients with differentiated thyroid cancer. Mol Imaging Radionucl Ther. 2014;23(2):54–9.
Giovanella L, Suriano S, Ricci R, Ceriani L, Anton Verburg F. Postsurgıcal thyroid remnant estimation by Tc-99m pertechnetate scintigraphy predicts radioiodine ablation effectiveness in patients with differentiated thyroid carcinoma. Head Neck. 2011;33(4):552–6.
Caglar M, Tuncel M, Alpar R. Value of technetium scintigraphy and iodine uptake measurement during follow-up of differentiated thyroid cancer. Ann Nucl Med. 2004;18:479–82.
Reynolds JC. Percent I-131 uptake and post-therapy I-131 scans: their role in the management of thyroid cancer. Thyroid. 1997;7:281–4.
Souza Rosario PW, Barroso AL, Rezende LL, Padrão EL, Fagundes TA, Pena GC, et al. Post I-131 therapy scanning in patients with thyroid cancer metastases: an unnecessary cost or a relevant contribution? Clin Nucl Med. 2004;29:795–8.
Thomas DL, Menda Y, Bushnell DA. A comparison between diagnostic I-123 and posttherapy I-131 scans in the detection of remnant and loco regional thyroid disease. Clin Nucl Med. 2009;34:745–8.
Al-Nahhas A, Khan S, Gogbashian A, Banti E, Rampin L, Rubello D. Review. 18F-FDG PET in the diagnosis and follow-up of thyroid malignancy. In Vivo. 2008;22:109–14.
Zanotti-Fregonara P, Hindié E, Keller I, Calzada-Nocaudie M, Devaux JY. Scintigraphic visualization of glossal thyroid tissue during the follow-up of thyroid cancer patients. Clin Nucl Med. 2007;32:911–4.
Geerlings JA, van Zuijlen A, Lohmann EM, Smit JW, Stokkel MP. The value of I-131 SPECT in the detection of recurrent differentiated thyroid cancer. Nucl Med Commun. 2010;31:417–22.
Grewal RK, Tuttle RM, Fox J, Borkar S, Chou JF, Gonen K, et al. The effect of posttherapy I-131 SPECT/CT on risk classification and management of patients with differentiated thyroid cancer. J Nucl Med. 2010;51:1361–7.
Acknowledgments
This study was supported by Akdeniz University Scientific Research Projects Unit.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Aydin, F., Sipahi, M., Budak, E.S. et al. Role of Tc-99m pertechnetate for remnant scintigraphy, post-thyroidectomy, and serum thyroglobulin and antithyroglobulin antibody levels in the patients with differentiated thyroid cancer. Ann Nucl Med 30, 60–67 (2016). https://doi.org/10.1007/s12149-015-1031-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-015-1031-1