Abstract
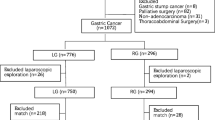
Robotic gastrectomy (RG) is increasingly performed based on expected benefits in short-term outcomes. However, it is still unclear if RG has any advantages over laparoscopic gastrectomy (LG). A retrospective cohort study was performed in patients who underwent minimally invasive gastrectomy between January 2012 and January 2020. A total of 366 patients were enrolled and short-term outcomes were compared between RG and LG. Propensity score matching was conducted to reduce selection bias based on age, sex, body mass index, performance status, physical status, clinical T, clinical N, clinical M, tumor location, neoadjuvant chemotherapy, type of gastrectomy, and extent of lymphadenectomy. A propensity score-matching algorithm was used to select 93 patients for each group. Estimated blood loss was smaller (0 vs. 37 mL, P = 0.001), length of hospital stay was shorter (10 vs. 12 days, P = 0.012), and the time until starting a soft diet was shorter (3 vs. 4 days, P = 0.001) in RG compared to LG. The overall complication rate was also lower in RG (9.7% vs 14.0%), but the difference was not significant. There was no mortality in either group. Total gastrectomy was an independent risk factor for postoperative complications. RG can be safely performed with a similar complication rate to that in LG and may permit faster postoperative recovery and a shorter hospital stay.



Similar content being viewed by others
References
Sakuramoto S, Sasako M, Yamaguchi T et al (2007) Adjuvant chemotherapy for gastric cancer with S-1, an oral fluoropyrimidine. N Engl J Med 357:1810–1820
Al-Batran SE, Homann N, Pauligk C et al (2019) Perioperative chemotherapy with fluorouracil plus leucovorin, oxaliplatin, and docetaxel versus fluorouracil or capecitabine plus cisplatin and epirubicin for locally advanced, resectable gastric or gastro-oesophageal junction adenocarcinoma (FLOT4): a randomised, phase 2/3 trial. Lancet 393:1948–1957
Pucher PH, Aggarwal R, Qurashi M et al (2014) Meta-analysis of the effect of postoperative in-hospital morbidity on long-term patient survival. Br J Surg 101:1499–1508
Saito T, Kurokawa Y, Miyazaki Y et al (2015) Which is a more reliable indicator of survival after gastric cancer surgery: postoperative complication occurrence or C-reactive protein elevation? J Surg Oncol 112:894–899
Inaki N, Etoh T, Ohyama T et al (2015) A multi-institutional, prospective, phase ii feasibility study of laparoscopy-assisted distal gastrectomy with D2 lymph node dissection for locally advanced gastric cancer (JLSSG0901). World J Surg 39:2734–2741
Lee HJ, Hyung WJ, Yang HK et al (2019) Short-term outcomes of a multicenter randomized controlled trial comparing laparoscopic distal gastrectomy with D2 lymphadenectomy to open distal gastrectomy for locally advanced gastric cancer (KLASS-02-RCT). Ann Surg 270:983–991
Katai H, Mizusawa J, Katayama H et al (2020) Survival outcomes after laparoscopy-assisted distal gastrectomy versus open distal gastrectomy with nodal dissection for clinical stage IA or IB gastric cancer (JCOG0912): a multicentre, non-inferiority, phase 3 randomised controlled trial. Lancet Gastroenterol Hepatol 5:142–151
Kim W, Kim HH, Han SU et al (2016) Decreased morbidity of laparoscopic distal gastrectomy compared with open distal gastrectomy for stage i gastric cancer: short-term outcomes from a multicenter randomized controlled trial (KLASS-01). Ann Surg 263:28–35
Yoshida K, Honda M, Kumamaru H et al (2018) Surgical outcomes of laparoscopic distal gastrectomy compared to open distal gastrectomy: a retrospective cohort study based on a nationwide registry database in Japan. Ann Gastroenterol Surg 2:55–64
Hiki N, Honda M, Etoh T et al (2017) Higher incidence of pancreatic fistula in laparoscopic gastrectomy. Real-world evidence from a nationwide prospective cohort study. Gastric Cancer 21:162–170
Okabe H, Obama K, Tsunoda S et al (2019) Feasibility of robotic radical gastrectomy using a monopolar device for gastric cancer. Surg Today 49:820–827
Kim HI, Han SU, Yang HK et al (2016) Multicenter prospective comparative study of robotic versus laparoscopic gastrectomy for gastric adenocarcinoma. Ann Surg 263:103–109
Uyama I, Suda K, Nakauchi M et al (2019) Clinical advantages of robotic gastrectomy for clinical stage I/II gastric cancer: a multi-institutional prospective single-arm study. Gastric Cancer 22:377–385
Suda K, Man-I M, Ishida Y et al (2015) Potential advantages of robotic radical gastrectomy for gastric adenocarcinoma in comparison with conventional laparoscopic approach: a single institutional retrospective comparative cohort study. Surg Endosc 29:673–685
Wang WJ, Li HT, Yu JP et al (2019) Severity and incidence of complications assessed by the Clavien-Dindo classification following robotic and laparoscopic gastrectomy for advanced gastric cancer: a retrospective and propensity score-matched study. Surg Endosc 33:3341–3354
Clavien PA, Barkun J, de Oliveira ML et al (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Obama K, Okabe H, Hosogi H et al (2011) Feasibility of laparoscopic gastrectomy with radical lymph node dissection for gastric cancer: from a viewpoint of pancreas-related complications. Surgery 149:15–21
Brierley D, Gospodarowics M et al (2020) TNM classification of malignant tumours. Wiley Blackwell, New Jersey
Japanese Gastric Cancer Association (2020) Japanese gastric cancer treatment guidelines 2018. Gastric Cancer. https://doi.org/10.1007/s10120-020-01042-y
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Okabe H, Obama K, Kan T et al (2010) Medial approach for laparoscopic total gastrectomy with splenic lymph node dissection. J Am Coll Surg 211:e1-6
Okabe H, Obama K, Tsunoda S et al (2014) Advantage of completely laparoscopic gastrectomy with linear stapled reconstruction: a long-term follow-up study. Ann Surg 259:109–116
Okabe H, Obama K, Tanaka E et al (2013) Laparoscopic proximal gastrectomy with a hand-sewn esophago-gastric anastomosis using a knifeless endoscopic linear stapler. Gastric Cancer 16:268–274
Tsunoda S, Okabe H, Obama K et al (2014) Short-term outcomes of totally laparoscopic total gastrectomy: experience with the first consecutive 112 cases. World J Surg 38:2662–2667
Hikage M, Tokunaga M, Makuuchi R et al (2017) Comparison of surgical outcomes between robotic and laparoscopic distal gastrectomy for cT1 gastric cancer. World J Surg 42:1803–1810
Kong Y, Cao S, Liu X et al (2020) Short-term clinical outcomes after laparoscopic and robotic gastrectomy for gastric cancer: a propensity score matching analysis. J Gastrointest Surg 24:531–539
Ye SP, Shi J, Liu DN et al (2020) Robotic- versus laparoscopic-assisted distal gastrectomy with D2 lymphadenectomy for advanced gastric cancer based on propensity score matching: short-term outcomes at a high-capacity center. Sci Rep 10:6502
Chen K, Pan Y, Zhang B et al (2017) Robotic versus laparoscopic Gastrectomy for gastric cancer: a systematic review and updated meta-analysis. BMC Surg 17:93
Hoshino N, Murakami K, Hida K et al (2020) Robotic versus laparoscopic surgery for gastric cancer: an overview of systematic reviews with quality assessment of current evidence. Updates Surg 72:573–582
Etoh T, Honda M, Kumamaru H et al (2017) Morbidity and mortality from a propensity score-matched, prospective cohort study of laparoscopic versus open total gastrectomy for gastric cancer: data from a nationwide web-based database. Surg Endosc 32:2766–2773
Yang K, Cho M, Roh CK et al (2019) Robotic spleen-preserving splenic hilar lymph node dissection during total gastrectomy for gastric cancer. Surg Endosc 33:2357–2363
Sano T, Sasako M, Yamamoto S et al (2004) Gastric cancer surgery: morbidity and mortality results from a prospective randomized controlled trial comparing D2 and extended para-aortic lymphadenectomy–Japan Clinical Oncology Group study 9501. J Clin Oncol 22:2767–2773
Obama K, Kim YM, Kang DR et al (2018) Long-term oncologic outcomes of robotic gastrectomy for gastric cancer compared with laparoscopic gastrectomy. Gastric Cancer 21:285–295
Yu J, Huang C, Sun Y et al (2019) Effect of laparoscopic vs open distal gastrectomy on 3-year disease-free survival in patients with locally advanced gastric cancer: the class-01 randomized clinical trial. JAMA 321:1983–1992
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Hiroshi Okabe, Hideki Sunagawa, Masashi Saji, Kenjiro Hirai, Shigeo Hisamori, Shigeru Tsunoda, and Kazutaka Obama declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were approved by the Institutional Review Board of each participating hospital and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Okabe, H., Sunagawa, H., Saji, M. et al. Comparison of short-term outcomes between robotic and laparoscopic gastrectomy for gastric cancer: a propensity score-matching analysis. J Robotic Surg 15, 803–811 (2021). https://doi.org/10.1007/s11701-020-01182-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11701-020-01182-4