Abstract
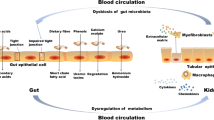
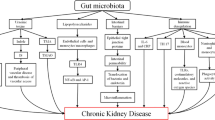
Kidney diseases are common and the incidence rate is increasing. Gut microbiota is involved in metabolic and immune regulation of the host. Genetic, alimentary and environmental disease factors may change gut flora and increase opportunistic and pathogenic bacteria, contributing to immune or non-immune mediated kidney diseases including IgA nephropathy and diabetic nephropathy. Additionally, bacterial metabolites may be a source of uremic toxins. Thus, identification of diversity, composition, and metabolic and immunologic features of gut bacteria in chronic kidney diseases may help understand pathogenetic mechanism and develop therapy for diseases.
Similar content being viewed by others
References
Qin J, Li R, Raes J, Arumuqam M, Burqdorf KS, Manichanh C, et al. A human gut microbial gene catalogue established by metagenomic sequencing. Nature 2010;464:59–65.
Kiryluk K, Moldoveanu Z, Sanders JT, Eison TM, Suzuki H, Julian BA, et al. Aberrant glycosylation of IgA1 is inherited in both pediatric IgA nephropathy and Henoch-Schönlein purpura nephritis. Kidney Int 2011;80:79–87.
Kiryluk K, Li Y, Scolari F, Sanna-Cherchi S, Choi M, Verbitsky M, et al. Discovery of new risk loci for IgA nephropathy implicates genes involved in immunity against intestinal pathogens. Nat Genet 2014;46:1187–1196.
Ambruzs JM, Walker PD, Larsen CP. The histopathologic spectrum of kidney biopsies in patients with inflammatory bowel disease. Clin J Am Soc Nephrol 2014;9:265–270.
Rosanna C. The intestine-renal connection in IgA nephropathy. Nephrol Dial Transplant 2015;30:360–366.
Anders HJ, Andersen K, Stecher B. The intestinal microbiota, a leaky gut, and abnormal immunity in kidney disease. Kidney Int 2013;83:1010–1016.
Krishnamurthy VM, Wei G, Baird BC, Murtauqh M, Chonchol MB, Raphael KL, et al. High dietary fiber intake is associated with decreased inflammation and allcause mortality in patients with chronic kidney disease. Kidney Int 2012;81:300–306.
Ryu M, Kullkarni OP, Radomska E, Miosge N, Gross O, Anders HJ. Bacterial CpG-DNA accelerates Alport glomerulosclerosis by inducing an M1 macrophage phenotype and tumor necrosis factor-a-mediated podocyte loss. Kidney Int 2011;79:189–198.
Neal MD, Jia H, Eyer B, Good M, Guerriero CJ, Sodhi CP, et al. Discovery and validation of a new class of small molecule Tolllike receptor 4 (TLR-4) inhibitors. PLoS One 2013;8:e65779.
Vaziri ND, Wong J, Pahl M, Piceno YM, Yuan J, DeSantis TZ, et al. Chronic kidney disease alters the componsition of intestinal microbial flora. Kidney Int 2013;83:308–315.
Aronov PA, Luo FJ, Plummer NS, Quan Z, Holmes S, Hostetter TH, et al. Colonic contribution to uremic solutes. J Am Soc Nephrol 2011;22:1769–1776.
Lin CJ, Chen HH, Pan CF, Chuang CK, Wang TJ, Sun FJ, et al. p-Cresylsulfate and indoxyl sulfate level at different stages of chronic kidney disease. J Clin Lab Anal 2011;25:191–197.
Niwa T. Role of indoxyl sulfate in the progression of chronic kidney disease and cardiovascular disease: experimental and clinical effects of oral sorbent AST-120. Ther Apher Dial 2011;15:120–124.
Wang F, Zhang P, Jiang H, Cheng S. Gut bacterial translocation contributes to microinflammation in experimental uremia. Dig Dis Sci 2012;57:2856–2862.
Acknowledgements
We sincerely thank Zheng ZH for his critical review and editing of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xie, A., Sheng, J. & Zheng, F. Intestinal Microbiota and Kidney Diseases. Chin. J. Integr. Med. 24, 406–408 (2018). https://doi.org/10.1007/s11655-017-2927-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-017-2927-5