Abstract
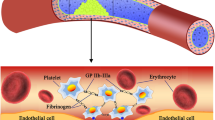
Vascular injury triggers two intertwined processes, platelet deposition and coagulation, and can lead to the formation of an intravascular clot (thrombus) that may grow to occlude the vessel. Formation of the thrombus involves complex biochemical, biophysical, and biomechanical interactions that are also dynamic and spatially-distributed, and occur on multiple spatial and temporal scales. We previously developed a spatial-temporal mathematical model of these interactions and looked at the interplay between physical factors (flow, transport to the clot, platelet distribution within the blood) and biochemical ones in determining the growth of the clot. Here, we extend this model to include reduction of the advection and diffusion of the coagulation proteins in regions of the clot with high platelet number density. The effect of this reduction, in conjunction with limitations on fluid and platelet transport through dense regions of the clot can be profound. We found that hindered transport leads to the formation of smaller and denser clots compared to the case with no protein hindrance. The limitation on protein transport confines the important activating complexes to small regions in the interior of the thrombus and greatly reduces the supply of substrates to these complexes. Ultimately, this decreases the rate and amount of thrombin production and leads to greatly slowed growth and smaller thrombus size. Our results suggest a possible physical mechanism for limiting thrombus growth.











Similar content being viewed by others
References
Adolph, R., Steed, D. L., Vorp, D. A., Webster, M. W., Kameneva, M. V., & Watkins, S. C. (1997). Cellular content and permeability of intraluminal thrombus in abdominal aortic aneurysm. J. Vasc. Surg., 25, 916–926.
Andre, P., Delaney, S. M., LaRocca, T., Vincent, D., DeGuzman, F., Jurek, M., Koller, B., Phillips, D. R., & Conley, P. B. (2003). P2Y12 regulates platelet adhesion/activation, thrombus growth, and thrombus stability in injured arteries. J. Clin. Invest., 112, 398–406.
Brass, L. F., Wannemacher, K. M., Ma, P., & Stalker, T. J. (2011). Regulating thrombus growth and stability to achieve an optimal response to injury. J. Thromb. Haemost., 9(1), 66–75.
Buddai, S. K., Layzer, J. M., Lu, G., Rusconi, C. P., Sullenger, B. A., Monroe, D. M., & Krishnaswamy, S. (2009). An anticoagulant RNA aptamer that inhibits proteinase-cofactor interactions within prothrombinase. J. Biol. Chem., 285, 5212–5223.
Celi, A., Merrill-Skoloff, G., Gross, P., Falati, S., Sim, D. S., Flaumenhaft, R., Furie, B. C., & Furie, B. (2003). Thrombus formation: Direct real-time observation and digital analysis of thrombus assembly in a living mouse by confocal and widefield intravital microscopy. J. Thromb. Haemost., 1, 60–68.
Clague, D. S., & Phillips, R. J. (1996). Hindered diffusion of spherical macromolecules through dilute fibrous media. Phys. Fluids, 8, 1720–1731.
Clague, D. S., & Phillips, R. J. (1997). A numerical calculation of the hydraulic permeability of three-dimensional disordered fibrous media. Phys. Fluids, 9, 1562–1572.
Colace, T. V., Muthard, R. W., & Diamond, S. L. (2012). Thrombus growth and embolism on tissue factor-bearing collagen surfaces under flow: role of thrombin with and without fibrin. Arterioscler. Thromb. Vasc. Biol., 32(6), 1466–1476.
Crowl, L., & Fogelson, A. L. (2011). Analysis of mechanisms for platelet near-wall excess under arterial blood flow conditions. J. Fluid Mech., 676, 348–375.
Crowl, L. M., & Fogelson, A. L. (2010). Computational model of whole blood exhibiting lateral platelet motion induced by red blood cells. Int. J. Numer. Methods Biomed. Eng., 26, 471–487.
Deen, W. M. (1997). Hindered transport of large molecules in liquid-filled pores. AIChE J., 33, 1409–1425.
Dill, K., & Bromberg, S. (2010). Molecular driving forces: statistical thermodynamics in biology, chemistry, physics, and nanoscience (2nd ed.). New York: Garland Science.
Eckstein, E. C., Tilles, A. W., & Millero, J.F., III (1988). Conditions for the occurrence of large near-wall excesses of small particles during blood flow. Microvasc. Res., 36, 31–39.
Fogelson, A. L., & Guy, R. D. (2008). Immersed-boundary-type models of intravascular platelet aggregation. Comput. Methods Appl. Mech. Eng., 197, 2087–2104.
Fogelson, A. L., & Guy, R. D. (2004). Platelet-wall interactions in continuum models of platelet aggregation: formulation and numerical solution. Math. Med. Biol., 21, 293–334.
Fogelson, A. L., Hussain, Y. H., & Leiderman, K. (2012). Blood clot formation under flow: the importance of factor xi depends strongly on platelet count. Biophys. J., 102, 10–18.
Fogelson, A. L., & Tania, N. (2005). Coagulation under flow: the influence of flow-mediated transport on the initiation and inhibition of coagulation. Pathophysiol. Haemost. Thromb., 34, 91–108.
Furie, B., & Furie, B. C. (2005). Thrombus formation in vivo. J. Clin. Invest., 115(12), 3355–3362.
Happel, J., & Brenner, H. (1983). Low Reynolds number hydrodynamics. Hague: Nijhoff.
Hathcock, J. J., & Nemerson, Y. (2004). Platelet deposition inhibits tissue factor activity: In vitro clots are impermeable to Factor Xa. Blood, 104(1), 123–127.
Hemker, H. C., & Kessels, H. (1991). Feedback mechanisms in coagulation. Haemostasis, 21, 189–196.
Jackson, S. P. (2007). The growing complexity of platelet aggregation. Blood, 109, 5087–5095.
Jesty, J., & Nemerson, Y. (1995). The pathways of blood coagulation. In E. Beutler, M. Lichtman, & B. Coller (Eds.), Williams hematology (5th ed.) (pp. 1227–1238). New York: McGraw-Hill.
Jordan, R. E., Oosta, G. M., Gardner, W. T., & Rosenberg, R. D. (1980). The kinetics of hemostatic enzyme-antithrombin interactions in the presence of low molecular weight heparin. J. Biol. Chem., 255, 10081–10090.
Kamath, P., & Krishnaswamy, S. (2008). Fate of membrane-bound reactants and products during the activation of human prothrombin by prothrombinase. J Biol Chem, 283, 30164–30173.
Keener, J. P., Sircar, S., & Fogelson, A. L. (2011). Kinetics of swelling gels. SIAM J. Appl. Math., 71, 854–875.
Kosto, K. B., & Deen, W. M. (2004). Diffusivities of macromolecules in composite hydrogels. AIChE J., 50, 2648–2658.
Kuharsky, A. L., & Fogelson, A. L. (2001). Surface-mediated control of blood coagulation: the role of binding site densities and platelet deposition. Biophys. J., 80, 1050–1074.
Leiderman, K., & Fogelson, A. L. (2011). Grow with the flow: a spatial-temporal model of platelet deposition and blood coagulation under flow. Math. Med. Biol., 28, 47–84.
Leiderman, K., Miller, L. A., & Fogelson, A. L. (2008). The effects of spatial inhomogeneities on flow through the endothelial surface layer. J. Theor. Biol., 252, 313–325.
LeVeque, R. J. (1996). High-resolution conservative algorithms for advection in incompressible flow. SIAM J. Numer. Anal., 33, 627–665.
Mann, K. G., Nesheim, M. E., Church, W. R., Haley, P., & Krishnaswamy, S. (1990). Surface-dependent reactions of the vitamin K-dependent enzyme complexes. Blood, 76, 1–16.
Neeves, K. B., Illing, D. A., & Diamond, S. L. (2010). Thrombin flux and wall shear rate regulate fibrin fiber deposition state during polymerization under flow. Biophys. J., 98(7), 1344–1352.
Nicholson, C. (2001). Diffusion and related transport mechanisms in brain tissue. Rep. Prog. Phys., 64, 815–884.
Okorie, U., Denney, W. S., Chatterjee, M. S., Neeves, K. B., & Diamond, S. L. (2008). Determination of surface tissue factor thresholds that trigger coagulation at venous and arterial shear rates: amplification of 100 fM circulating tissue factor by flow. Blood, 111(7), 3507–3513.
oude Egbrink, M. G. A., Tangelder, G. J., Slaaf, D. W., & Reneman, R. S. (1988). Thromboembolic reaction following wall punction in arterioles and venules of the rabbit mesentery. Thromb. Haemost., 59, 23–28.
Pluen, A., Boucher, Y., Ramanujan, S., McKee, T. D., Gohongi, T., di Tomaso, E., Brown, E. B., Izumi, Y., Campbell, R. B., Berk, D. A., & Jain, R. K. (2001). Role of tumor-host interactions in interstitial diffusion of macromolecules: cranial vs. subcutaneous tumors. Proc. Natl. Acad. Sci. USA, 98, 4628–4633.
Sahimi, M. (2010). Flow and transport in porous media and fractured rock. Weinheim: Wiley-VCH.
Seligsohn, U. (2009). Factor XI deficiency in humans. J. Thromb. Haemost., 7, 84–87.
Stalker, T. J., Traxler, E. A., Diamond, S. L., & Brass, L. F. (2011). Development of a stable thrombotic core with limited access to plasma proteins during thrombus formation in vivo. Abstract 53rd ASH annual meeting and exposition, December 2011.
Steiakakis, E., Gamvroudis, C., & Alevios, G. (2012). Kozeny–Carman equation and hydraulic conductivity of compacted clayey soils. Geomaterials, 2, 37–41.
Tilles, A. W., & Eckstein, E. C. (1987). The near-wall excess of platelet-sized particles in blood flow: its dependence on hematocrit and wall shear rate. Microvasc. Res., 33, 211.
Torquato, S. (2002). Random heterogeneous materials: microstructure and macroscopic properties. New York: Springer.
Vaiyapuri, S., Jones, C. I., Sasikumar, P., Moraes, L. A., Munger, S. J., Wright, J. R., Ali, M. S., Sage, T., Kaiser, W. J., Tucker, K. L., Stain, C. J., Bye, A. P., Jones, S., Oviedo-Orta, E., Simon, A. M., Mahaut-Smith, M. P., & Gibbins, J. M. (2012). Gap junctions and connexin hemichannels underpin hemostasis and thrombosis. Circulation, 125(20), 2479–2491.
Zhao, H., & Shaqfeh, E. S. G. (2011). Shear-induced platelet margination in a microchannel. Phys. Rev. E, 83, 061924.
Acknowledgements
This work was supported by NSF RTG Grant DMS-0943760, by NSF Grant DMS-0540779 and by NIGMS Grant R01-GM090203. The authors are very grateful to Jim Keener for numerous helpful discussions.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Leiderman, K., Fogelson, A.L. The Influence of Hindered Transport on the Development of Platelet Thrombi Under Flow. Bull Math Biol 75, 1255–1283 (2013). https://doi.org/10.1007/s11538-012-9784-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11538-012-9784-3