Abstract
Purpose
Recent evidence associates sympathetic tone with severity of obstructive sleep apnea (OSA). Renal sympathetic denervation (RDN), by decreasing sympathetic tone, has the potential to decrease OSA severity. Small observational studies that assessed this hypothesis lacked precision. Hence, in this meta-analysis, we have attempted to pool available data from studies that have assessed the effect of RDN on OSA severity in patients with OSA.
Methods
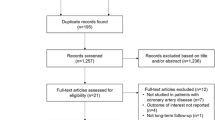
Medline, Embase, Cochrane central, Ovid, Cinahl, web of science, and conference abstracts were searched for eligible citations by two independent reviewers using key words “renal denervation,” “hypertension,” and “obstructive sleep apnea.” From a total of 2,863 identified citations, using meta-analysis of observational studies in epidemiology method, five studies were assessed eligible and included in the meta-analysis.
Results
All five studies followed an observational study design, involved patients with OSA and HTN, and reported an apnea-hypopnea index (AHI) 6 months post-RDN. Four were “before and after” studies and one compared continuous positive airway pressure with RDN. In the pooled analysis, involving 49 patients, RDN was associated with a significant reduction in mean AHI [weighted mean difference −9.61 (95 % CI −15.43 to −3.79, P = 0.001)] 6 months post-RDN. One study also reported improvement in oxygen desaturation index and Epworth sleepiness scale score 6 months post-RDN.
Conclusions
RDN is associated with significant improvement in OSA severity. However, our results need validation in RCTs that assess effect of RDN in patients with OSA, which can potentially broaden the clinical applicability of RDN.


Similar content being viewed by others
Reference
Duran J, Esnaola S, Rubio R, Iztueta A (2001) Obstructive sleep apnea-hypopnea and related clinical features in a population-based sample of subjects aged 30 to 70 yr. Am J Respir Crit Care Med 163:685e9
Punjabi NM (2008) The epidemiology of adult obstructive sleep apnea. Proc Am Thorac Soc 5:136e43
Flegal KM, Carroll MD, Kit BK, Ogden CL (2012) Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999–2010. JAMA 307:491–7
Young T, Skatrud J, Peppard PE (2004) Risk factors for obstructive sleep apnea in adults. JAMA 291:2013e6
Loke YK, Brown JW, Kwok CS, Niruban A, Myint PK (2012) Association of obstructive sleep apnea with risk of serious cardiovascular events: a systematic review and meta-analysis. Circ Cardiovasc Qual Outcome 5:720e8
Peppard PE, Young T, Palta M, Skatrud J (2000) Prospective study of the association between sleep-disordered breathing and hypertension. N Engl J Med 342:1378e84
Logan AG, Perlikowski SM, Mente A, Tisler A, Tkacova R, Niroumand M, Leung RS, Bradley TD (2001) High prevalence of unrecognized sleep apnoea in drug-resistant hypertension. J Hypertens 19:2271–7
Lloberes P, Lozano L, Sampol G, Romero O, Jurado MJ, Ríos J, Untoria MD, Tovar JL (2010) Obstructive sleep apnoea and 24-h blood pressure in patients with resistant hypertension. J Sleep Res 19:597–602
Kartali N, Daskalopoulou E, Geleris P, Chatzipantazi S, Tziomalos K, Vlachogiannis E, Karagiannis A (2013) The effect of continuous positive airway pressure therapy on blood pressure and arterial stiffness in hypertensive patients with obstructive sleep apnea. Sleep Breath. PMID: 24362941
Mancia G, De Backer G, Dominiczak A, Cifkova R, Fagard R, Germano G, Grassi G, Heagerty AM, Kjeldsen SE, Laurent S, Narkiewicz K, Ruilope L, Rynkiewicz A, Schmieder RE, Boudier HA, Zanchetti A (2007) 2007 guidelines for the management of arterial hypertension: the Task Force for the Management of Arterial Hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 25:1105–1187
Bradley TD, Floras JS (2009) Obstructive sleep apnoea and its cardiovascular consequences. Lancet 373:82–93
Tsioufis C, Kasiakogias A, Thomopoulos C, Manolis A, Stefanadis C (2010) Managing hypertension in obstructive sleep apnea: the interplay of continuous positive airway pressure, medication and chronotherapy. J Hypertens 28:875–882
Krum H, Schlaich M, Whitbourn R, Sobotka PA, Sadowski J, Bartus K, Kapelak B, Walton A, Sievert H, Thambar S, Abraham WT, Esler M (2009) Catheter-based renal sympathetic denervation for resistant hypertension: a multicentre safety and proof-of-principle cohort study. Lancet 373:1275–1281
Schlaich MP, Sobotka PA, Krum H, Lambert E, Esler MD (2009) Renal sympathetic-nerve ablation for uncontrolled hypertension. N Engl J Med 361:932–934
Esler MD, Krum H, Sobotka PA, Schlaich MP, Schmieder RE, Bohm M (2010) Renal sympathetic denervation in patients with treatment-resistant hypertension (the Symplicity HTN-2 Trial): a randomised controlled trial. Lancet 376:1903–1909
Damascelli B, Patelli G, Tichá V, Della Rocca F, Lattuada S, Sala C, Albertoni A, D’Alessio A, Funaro A, Scotti L (2013) Catheter-based radiofrequency renal sympathetic denervation for resistant hypertension. J Vasc Interv Radiol 24:632–9
Witkowski A, Prejbisz A, Florczak E, Kądziela J, Śliwiński P, Bieleń P, Michałowska I, Kabat M, Warchoł E, Januszewicz M, Narkiewicz K, Somers VK, Sobotka PA, Januszewicz A (2011) Effects of renal sympathetic denervation on blood pressure, sleep apnea course, and glycemic control in patients with resistant hypertension and sleep apnea. Hypertension 58:559–65
Stroup DF, Berlin JA, Morton SC et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. Meta-analysis of observational studies in epidemiology (MOOSE) group. JAMA 283:2008e12
Deeks JJ, Higgins JPT, Altman DG (2008) Chapter 9. Analysing data and undertaking meta-analyses. In: Higgins JPT, Green S (eds) Cochrane handbook for systematic reviews of interventions. John Wiley & Sons, Chichester
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Egger M, Davey Smith G, Schneider M, Minder C (1997) Bias in meta-analysis detected by a simple, graphical test. BMJ 315:629–34
Schmiedel L, Traenkner A, Schmiedehausen N, Strasser RH, Schroetter H (2013) The failing effects of renal sympathetic denervation in patients with drug resistant hypertension and untreated obstructive sleep apnea. Eur Heart J 34:823–4
Thakur D, Zimmerman N, Rajebi H, Rajebi MR (2013) Renal sympathetic denervation and resistant hypertension. J Vasc Interv Radiol 24:145.e6–7
Zhao MM, Tan XX, Ding N, Zhang XL (2013) Comparison of efficacy between continuous positive airway pressure and renal artery sympathetic denervation by radiofrequency ablation in obstructive sleep apnea syndrome patients with hypertension. Zhonghua Yi Xue Za Zhi 93:1234–7
Schwab RJ, Gupta KB, Gefter WB, Metzger LJ, Hoffman EA, Pack AI (1995) Upper airway and soft tissue anatomy in normal subjects and patients with sleep-disordered breathing. Significance of the lateral pharyngeal walls. Am J Respir Crit Care Med 152:1673–89
Gaddam KK, Nishizaka MK, Pratt-Ubunama MN, Pimenta E, Aban I, Oparil S, Calhoun DA (2008) Characterization of resistant hypertension: association between resistant hypertension, aldosterone, and persistent intravascular volume expansion. Arch Intern Med 168:1159–1164
Hudgel DW, Harasick T (1990) Fluctuation in timing of upper airway and chest wall inspiratory muscle activity in obstructive sleep apnea. J Appl Physiol (1985) 69:443–50
Acknowledgments
None.
Ethical standards
In this systematic review, though uses data from published clinical studies, the authors’ were not directly involved in data collection from human subjects but used published data from the literature. The institutional review board of the Wright Center for Graduate Medical Education, Scranton, PA, USA approved the conduct of the study.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shantha, G.P.S., Pancholy, S.B. Effect of renal sympathetic denervation on apnea-hypopnea index in patients with obstructive sleep apnea: a systematic review and meta-analysis. Sleep Breath 19, 29–34 (2015). https://doi.org/10.1007/s11325-014-0991-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-014-0991-z