Abstract
Purpose
There is conflicting evidence regarding long-term effects of unilateral nephrectomy such as cardiovascular diseases. Excessive increase in blood pressure (BP) during exercise called “hypertensive response to exercise” may be a sign of unborn hypertension and increased cardiovascular risk. Decrease in glomerular filtration rate (GFR) in patients with unilateral nephrectomy may be associated with disturbance of circadian BP changes without affecting the absolute levels of BP. We aimed to investigate the circadian BP changes and hypertensive response to exercise in normotensive patients with preserved renal functions who had undergone unilateral nephrectomy for other causes rather than organ donation.
Methods
This study enrolled 32 patients (mean age 43.4 ± 9.9 years, male 15) with unilateral nephrectomy and 40 healthy controls (mean age 47 ± 6.1 years, male 17). All patients were undergone both office and ambulatory BP measurements and treadmill stress test.
Results
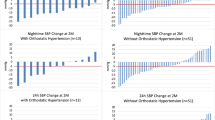
The median time since nephrectomy was 12 (9–22) years in the patient group. The median GFR of the patient group was lower than that of the controls without significance [85.1 (76.0–97.9) vs. 93.2 (84.5–104.9), respectively; p = 0.14]. There was no significant difference between groups in terms of office BP measurements, night time diastolic and systolic BP, mean arterial pressure (MAP), night/day time ratio of MAP in ambulatory BP measurements. The results of treadmill stress tests and hypertensive response to exercise ratios were also similar between the groups.
Conclusion
This study revealed that there was no increase in long-term cardiovascular risks one decade after unilateral nephrectomy based on circadian BP changes and hypertensive response to exercise in normotensive patients.
Similar content being viewed by others
References
Flanigan WJ, Burns RO, Takacs FJ, Merrill JP (1968) Serial studies of glomerular filtration rate and renal plasma flow in kidney transplant donors, identical twins, and allograft recipients. Am J Surg 116:788–794
Goldfarb DA, Matin SF, Braun WE et al (2001) Renal outcome 25 years after donor nephrectomy. J Urol 6:2043–2047
Yazawa M, Kido R, Shibagaki Y et al (2011) Kidney function, albuminuria and cardiovascular risk factors in post- perative living kidney donors: a single-center, cross-sectional study. Clin Exp Nephrol 15:514–521
Garg AX, Muirhead N, Knoll G et al (2006) Donor nephrectomy outcomes research (DONOR) network. Proteinuria and reduced kidney function in living kidney donors: a systematic review, meta-analysis, and meta-regression. Kidney Int 70:1801–1810
Garg AX, Meirambayeva A, Huang A et al (2012) Donor nephrectomy outcomes research network: cardiovascular disease in kidney donors: matched cohort study. BMJ 344:1–10
Mjqen G, Hallan S, Hartmann A et al (2014) Long-term risks for kidney donors. Kidney Int 86:162–167
Matthews CE, Pate RR, Jackson KL et al (1998) Exaggerated blood pressure response to dynamic exercise and risk of future hypertension. J Clin Epidemiol 51:29–35
Stewart KJ, Sung J, Silber HA et al (2004) Exaggerated exercise blood pressure is related to impaired endothelial vasodilator function. Am J Hypertens 17:314–320
Goto N, Uchida K, Morozumi K et al (2005) Circadian blood pressure rhythm is disturbed by nephrectomy. Hypertens Res 28:301–316
Mancia G, De Backer G, Dominiczak A et al (2007) Guidelines for the management of arterial hypertension: the Task force for the management of arterial hypertension of the european society of hypertension (ESH) and of the European society of cardiology (ESC). Eur Heart J 28:1462–1536
Levey AS, Stevens LA, Schmid CH et al (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150:604–612
O’Brien E, Coats A, Owens P et al (2003) Use and interpretation of ambulatory blood pressure monitoring: recommendations of the British hypertension society. BMJ 320:1128–1134
Kimura G (2001) Sodium, kidney, and circadian rhythm of blood pressure. Clin Exp Nephrol 5:13–18
Kimura G, Brenner BM (1995) The renal basis for salt sensitivity in hypertension. In: Laragh JH, Brenner BM (eds) Hypertension: pathophysiology, diagnosis and management. Raven Press, New York, pp 1569–1588
Kimura G, Brenner BM (1997) Implications of linear pressure-natriuresis relationship and importance of sodium sensitivity in hypertension. J Hypertens 15:1055–1061
Krohn Arthur G, Ogden David A, Holmes Joseph H (1996) Renal function in 29 healthy adults before and after nephrectomy. JAMA 196:322–324
Edgren J, Laasonen L, Kock B, Brotherus JW, Pasternack A, Kuhlbäck B (1976) Kidney function and compensatory growth of the kidney in living kidney donors. Scand J Urol Nephrol 10:134–136
Hakim RM, Goldszer RC, Brenner BM (1984) Hypertension and proteinuria: long-term sequelae of uninephrectomy in humans. Kidney Int 25:930–936
Eberhard OK, Kliem V, Offner G et al (1997) Assessment of long-term risks for living related kidney donors by 24-h blood pressure monitoring and testing for microalbuminuria. Clin Transplant 11:415–419
Gatzka CD, Schobel HP, Klingbeil AU, Neumayer HH, Schmieder RE (1995) Normalization of circadian blood pressure profiles after renal transplantation. Transplantation 59:1270–1274
Buijsen JG, van Acker BA, Koomen GC, Koopman MG, Arisz L (1994) Circadian rhythm of glomerular filtration rate in patients after kidney transplantation. Nephrol Dial Transplant 9:1330–1333
Garg AX, Prasad GV, Thiessen-Philbrook HR et al (2008) Donor nephrectomy outcomes research (DONOR) network. Cardiovascular disease and hypertension risk in living kidney donors: an analysis of health administrative data in Ontario, Canada. Transplantation 86:399–406
Boudville N, Prasad GV, Knoll G et al (2006) Donor nephrectomy outcomes research (DONOR) network. Meta-analysis: risk for hypertension in living kidney donors. Ann Intern Med 145:185–196
Sobh M, Nabeeh A, el Din AS et al (1989) Long-term follow-up of the remaining kidney in living related kidney donors. Int Urol Nephrol 21:547–553
Tonelli M, Wiebe N, Culleton B et al (2006) Chronic kidney disease and mortality risk: a systematic review. J Am Soc Nephrol 17:2034–2047
Ibrahim HN, Rogers T, Tello A, Matas A (2006) The performance of three serum creatinine-based formulas in estimating GFR in former kidney donors. Am J Transplant 6:1479–1485
Tsai MY, Aras O, Sozen H et al (2004) Plasma homocysteine levels in living kidney donors before and after uninephrectomy. J Lab Clin Med 143:340–343
Scott JA, Coombes JS, Prins JB, Leano RL, Marwick TH, Sharman JE (2008) Patients with type 2 diabetes have exaggerated brachial and central exercise blood pressure: relation to left ventricular relative wall thickness. Am J Hypertens 21:715–721
Sharman JE, Hare JL, Thomas S et al (2011) Association of masked hypertension and left ventricular remodeling with the hypertensive response to exercise. Am J Hypertens 24:898–903
Kramer CK, Leitão CB, Canani LH, Ricardo ED, Pinto LC, Gross JL (2009) Blood pressure responses to exercise in type II diabetes mellitus patients with masked hypertension. J Hum Hypertens 23:620–622
Takeno K, Mita T, Nakayama S et al (2012) Masked hypertension, endothelial dysfunction, and arterial stiffness in type 2 diabetes mellitus: a pilot study. Am J Hypertens 25:165–170
Yilmaz BA, Caliskan Y, Yilmaz A et al (2015) Cardiovascular-renal changes after kidney donation: one-year follow-up study. Transplantation 99:760–764
Authors’ contributions
All of the authors contributed planning, conducting and reporting of the work. All contributors are responsible for the overall content as guarantors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Sultan Ozkurt, Yusuf Karavelioglu, Macit Kalcik and Ahmet Musmul declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Ozkurt, S., Karavelioglu, Y., Kalcik, M. et al. Assessment of long-term cardiovascular effects of unilateral nephrectomy. Int Urol Nephrol 49, 867–873 (2017). https://doi.org/10.1007/s11255-017-1553-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-017-1553-7