Abstract
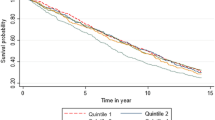
The association of mortality risk and insomnia disorder with daytime impairments has been plausible. The purpose of this study was to evaluate the strength of evidence for this relationship. We performed a comprehensive literature search for clinical Cohort trials including annual cumulative time-to-event data that evaluated the risk of mortality in insomnia disorder patients with daytime impairments. We used pooled hazard ratio (HR) as the main outcome measure and Kaplan-Meier survive curve to display outcome measures. The weighted cumulative mortality of 4.5% for patients with insomnia disorder was higher than that of 2.6% for those without insomnia (p<0.001). Higher risk of mortality presented in patients with insomnia disorder when compared to those without insomnia (HR = 1.66, 95% CI = 1.25–2.19, p<0.001). Patients with duration of more than 10 years were at a greater risk of annual cumulative mortality (R2 = 0.891, p<0.001). Insomnia disorder with daytime impairments increased the risk of mortality, and patients with duration of more than 10 years were at a greater risk of annual cumulative mortality.



Similar content being viewed by others
References
Association AP. Diagnostic and Statistical Manual of Mental Disorders (DSM-5). W ashington, DC. London, England; 2013.
Riemann D, Nissen C, Palagini L, Otte A, Perlis ML, Spiegelhalder K. The neurobiology, investigation, and treatment of chronic insomnia. Lancet Neurol. 2015;14(5):547–58.
Irwin MR. Why sleep is important for health: a psychoneuroimmunology perspective. Annu Rev Psychol. 2015;66:143–72.
Irwin MR, Olmstead R, Carroll JE. Sleep disturbance, sleep duration, and inflammation: a systematic review and meta-analysis of cohort studies and experimental sleep deprivation. Biol Psychiatry. 2016;80(1):40–52.
Allen RP. Article reviewed: mortality associated with sleep duration and insomnia. Sleep Med. 2002;3(4):373–5.
Li Y, Zhang X, Winkelman JW, Redline S, Hu FB, Stampfer M, et al. Association between insomnia symptoms and mortality: a prospective study of U.S. men. Circulation. 2014;129(7):737–46.
Lu JL, Freire AX, Molnar MZ, Kalantar-Zadeh K, Kovesdy CP. Association of Chronic Insomnia with Mortality and Adverse Renal Outcomes. Mayo Clin Proc. 2018;93(11):1563–70.
Li LJ, Yang Y, Guan BY, Chen Q, Wang AX, Wang YJ, et al. Insomnia is associated with increased mortality in patients with first-ever stroke: a 6-year follow-up in a Chinese cohort study. Stroke Vasc Neurol. 2018;3(4):197–202.
Vgontzas AN, Liao D, Pejovic S, Calhoun S, Karataraki M, Basta M, et al. Insomnia with short sleep duration and mortality: the Penn State cohort. Sleep. 2010;33(9):1159–64.
Lovato N, Lack L. Insomnia and mortality: A meta-analysis. Sleep Med Rev. 2019;43:71–83.
The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. at http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp.)
Tierney JF, Stewart LA, Ghersi D, et al. Practical methods for incorporating summary time-to-event data into meta-analysis. Trials. 2007;8:16.
Sivertsen B, Pallesen S, Glozier N, et al. Midlife insomnia and subsequent mortality: the Hordaland health study. BMC Public Health. 2014;14:720.
Leigh L, Hudson IL, Byles JE. Sleeping difficulty, disease and mortality in older women: a latent class analysis and distal survival analysis. J Sleep Res. 2015;24(6):648–57.
Parthasarathy S, Vasquez MM, Halonen M, Bootzin R, Quan SF, Martinez FD, et al. Persistent insomnia is associated with mortality risk. Am J Med. 2015;128(3):268–75 e262.
Choi JW, Song JS, Lee YJ, Won TB, Jeong DU. Increased mortality in relation to insomnia and obstructive sleep apnea in Korean patients studied with nocturnal Polysomnography. J Clin Sleep Med. 2017;13(1):49–56.
Bertisch SM, Pollock BD, Mittleman MA, et al. Insomnia with objective short sleep duration and risk of incident cardiovascular disease and all-cause mortality: Sleep Heart Health Study. Sleep 2018;41(6).
Lallukka T, Podlipskyte A, Sivertsen B, et al. Insomnia symptoms and mortality: a register-linked study among women and men from Finland. Norway and Lithuania J Sleep Res. 2016;25(1):96–103.
Grandner MA, Buxton OM, Jackson N, Sands-Lincoln M, Pandey A, Jean-Louis G. Extreme sleep durations and increased C-reactive protein: effects of sex and ethnoracial group. Sleep. 2013;36(5):769–779E.
Zee PC, Badr MS, Kushida C, Mullington JM, Pack AI, Parthasarathy S, et al. Strategic opportunities in sleep and circadian research: report of the joint task force of the Sleep Research Society and American Academy of sleep medicine. Sleep. 2014;37(2):219–27.
Irwin MR, Cole SW. Reciprocal regulation of the neural and innate immune systems. Nat Rev Immunol. 2011;11(9):625–32.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
All authors declare that they have no conflicts of interest to disclose.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jiang, B., He, D., Guo, Z. et al. Insomnia Disorder Increases the Risk of Mortality: Pooled Analysis of Annual Cumulative Time-to-Event Data. Psychiatr Q 91, 1431–1437 (2020). https://doi.org/10.1007/s11126-020-09768-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11126-020-09768-9