Abstract
Background
Symptomatic new lesions that appear after gamma knife radiosurgery (GKRS) for brain metastases have not been thoroughly described.
Methods
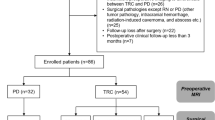
Among 238 patients who underwent a single session of GKRS without whole-brain radiotherapy or surgery for brain metastases between 2009 and 2014, a total of 165 (69.3%) patients underwent follow-up magnetic resonance imaging (MRI). Their electrical health records were reviewed retrospectively. The median age was 68 years, and 62.4% patients were men. The median number of brain metastases was 2. The most frequent primary organ site was the lung (71.5%). Then, we evaluated predictors for the symptoms of new lesions.
Results
New lesions and leptomeningeal dissemination were observed in 101 (61.2%) and 23 (14.2%) patients, respectively. The median number of new lesions was 2; moreover, 20 of 101 patients (19.8%) with new lesions had tumours with the largest diameters of > 1 cm. Among 101 patients with new lesions, 13 were symptomatic (12.9%). Patients with larger new lesions (> 1 cm of the largest diameter) experienced symptoms more frequently (odds ratio 7.6, P < 0.01). Symptoms resolved after salvage GKRS in seven of 11 patients who abided by the recommended follow-up MRI schedule. No significant risk factors were found for symptoms of new lesions.
Conclusions
The incidence of symptomatic new lesions that appeared after GKRS was low, and more than half of the patients showed improvements in their symptoms after salvage GKRS. However, careful MRI-based assessments and salvage GKRS are critical for the quality of life.


Similar content being viewed by others
References
Aoyama H, Shirato H, Tago M, Nakagawa K, Toyoda T, Hatano K, Kenjyo M, Oya N, Hirota S, Shioura H, Kunieda E, Inomata T, Hayakawa K, Katoh N, Kobashi G (2006) Stereotactic radiosurgery plus whole-brain radiation therapy vs stereotactic radiosurgery alone for treatment of brain metastases: a randomized controlled trial. JAMA 295:2483–2491
Chang EL, Wefel JS, Hess KR, Allen PK, Lang FF, Kornguth DG, Arbuckle RB, Swint JM, Shiu AS, Maor MH, Meyers CA (2009) Neurocognition in patients with brain metastases treated with radiosurgery or radiosurgery plus whole-brain irradiation: a randomised controlled trial. Lancet Oncol 10:1037–1044
Chernov MF, Nakaya K, Izawa M, Hayashi M, Usuba Y, Kato K, Muragaki Y, Iseki H, Hori T, Takakura K (2007) Outcome after radiosurgery for brain metastases in patients with low Karnofsky performance scale (KPS) scores. Int J Radiat Oncol Biol Phys 67:1492–1498
Cho KR, Lee MH, Kong DS, Seol HJ, Nam DH, Sun JM, Ahn JS, Ahn MJ, Park K, Kim ST, Lim DH, Lee JI (2015) Outcome of gamma knife radiosurgery for metastatic brain tumors derived from non-small cell lung cancer. J Neuro-Oncol 125:331–338
Elliott RE, Rush SC, Morsi A, Mehta N, Spriet J, Narayana A, Donahue B, Parker EC, Golfinos JG (2011) Local control of newly diagnosed and distally recurrent, low-volume brain metastases with fixed-dose (20 Gy) gamma knife radiosurgery. Neurosurgery 68:921–931
Hanssens P, Karlsson B, Vashu R, Yeo TT, Beute G (2012) Salvage treatment of distant recurrent brain metastases with gamma knife surgery. Acta Neurochir 154:285–290
Hanssens P, Karlsson B, Yeo TT, Chou N, Beute G (2011) Detection of brain micrometastases by high-resolution stereotactic magnetic resonance imaging and its impact on the timing of and risk for distant recurrences. J Neurosurg 115:499–504
Kano H, Kondziolka D, Lobato-Polo J, Zorro O, Flickinger JC, Lunsford LD (2010) T1/T2 matching to differentiate tumor growth from radiation effects after stereotactic radiosurgery. Neurosurgery 66:486–491
Koiso T, Yamamoto M, Kawabe T, Watanabe S, Sato Y, Higuchi Y, Yamamoto T, Matsumura A, Kasuya H (2016) Follow-up results of brain metastasis patients undergoing repeat gamma knife radiosurgery. J Neurosurg 125(Suppl 1):2–10
Jamal-Hanjani M, Spicer J (2012) Epidermal growth factor receptor tyrosine kinase inhibitors in the treatment of epidermal growth factor receptor-mutant non-small cell lung cancer metastatic to the brain. Clin Cancer Res 18:938–944
Matsunaga S, Shuto T, Kawahara N, Suenaga J, Inomori S, Fujino H (2011) Gamma knife surgery for brain metastases from colorectal cancer. Clinical article. J Neurosurg 114:782–789
Regine WF, Huhn JL, Patchell RA, St Clair WH, Strottmann J, Meigooni A, Sanders M, Young AB (2002) Risk of symptomatic brain tumor recurrence and neurologic deficit after radiosurgery alone in patients with newly diagnosed brain metastases: results and implications. Int J Radiat Oncol Biol Phys 52:333–338
Rush S, Elliott RE, Morsi A, Mehta N, Spriet J, Narayana A, Donahue B, Parker EC, Golfinos JG (2011) Incidence, timing, and treatment of new brain metastases after gamma knife surgery for limited brain disease: the case for reducing the use of whole-brain radiation therapy. J Neurosurg 115:37–48
Sawrie SM, Guthrie BL, Spencer SA, Nordal RA, Meredith RF, Markert JM, Cloud GA, Fiveash JB et al (2008) Predictors of distant brain recurrence for patients with newly diagnosed brain metastases treated with stereotactic radiosurgery alone. Int J Radiat Oncol Biol Phys 70:181–186
Serizawa T, Higuchi Y, Ono J, Matsuda S, Nagano O, Iwadate Y, Saeki N (2006) Gamma knife surgery for metastatic brain tumors without prophylactic whole-brain radiotherapy: results in 1000 consecutive cases. J Neurosurg 105(suppl):86–90
Serizawa T, Saeki N, Higuchi Y, Ono J, Iuchi T, Nagano O, Yamaura A (2005) Gamma knife surgery for brain metastases: indications for and limitations of a local treatment protocol. Acta Neurochir 147:721–726
Sheehan JP, Yen CP, Nguyen J, Rainey JA, Dassoulas K, Schlesinger DJ (2011) Timing and risk factors for new brain metastasis formation in patients initially treated only with gamma knife surgery. Clinical article. J Neurosurg 114:763–768
Thng CH, Tay KH, Chan LL, Lim EH, Khoo BK, Huin EL, Tan KP (1999) Magnetic resonance imaging of brain metastases: magnetisation transfer or triple dose gadolinium? Ann Acad Med Singap 28:1529–1533
Yamamoto M, Ide M, Si N, Urakawa Y (2002) Gamma knife radiosurgery for numerous brain metastases: is this a safe treatment? Int J Radiat Oncol Biol Phys 53:1279–1283
Yamamoto M, Kawabe T, Higuchi Y, Sato Y, Nariai T, Watanabe S, Barfod BE, Kasuya H (2014) Validity of prognostic grading indices for brain metastasis patients undergoing repeat radiosurgery. World Neurosurg 82:1242–1249
Yamamoto M, Kawabe T, Sato Y, Higuchi Y, Nariai T, Watanabe S, Kasuya H (2014) Stereotactic radiosurgery for patients with multiple brain metastases: a case-matched study comparing treatment results for patients with 2-9 versus 10 or more tumors. J Neurosurg 121(suppl):16–25
Yamamoto M, Serizawa T, Shuto T, Akabane A, Higuchi Y, Kawagishi J, Yamanaka K, Sato Y, Jokura H, Yomo S, Nagano O, Kenai H, Moriki A, Suzuki S, Kida Y, Iwai Y, Hayashi M, Onishi H, Gondo M, Sato M, Akimitsu T, Kubo K, Kikuchi Y, Shibasaki T, Goto T, Takanashi M, Mori Y, Takakura K, Saeki N, Kunieda E, Aoyama H, Momoshima S, Tsuchiya K (2014) Stereotactic radiosurgery for patients with multiple brain metastases (JLGK0901): a multi-institutional prospective observational study. Lancet Oncol 15:387–395
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Nakazaki, K., Nishigaki, M. Evaluation of new lesions and symptoms after gamma knife radiosurgery for brain metastases: a retrospective cohort study. Acta Neurochir 160, 1461–1471 (2018). https://doi.org/10.1007/s00701-018-3524-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-018-3524-x