Abstract
Background
The literature has investigated barriers to reporting adverse events in surgery, but with less emphasis on near misses. No attempt was made to categorise near misses by type and reportability. This paper attempts to fill these two gaps in the literature.
Methods
A mixed methodology approach was adopted. A sample of 16 laparoscopic surgeries were observed followed by a questionnaire distributed among professionals dealing with laparoscopies. Non-parametric tests and mediation–moderation analysis were used to compare responses and identify causal factors.
Results
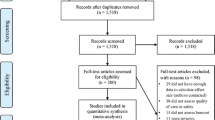
A total of 469 near misses were observed, and classified into two categories: reportable events and common events. Among 23 observed reportable events, only 9 events were reported. Out of 300 distributed questionnaires, we received 178 valid responses (response rate 59%). The professionals strongly disagreed that reporting near misses (Mean 4.09, STD 0.95) and adverse events (4.17, 1.02) makes little contribution to the quality of surgery. However, the results show that professionals were more willing to disclose adverse events than near misses, Heavy workload, privacy, lack of support, and fear from disciplinary actions negatively affected professionals’ willingness to report near misses.
Discussion
Error reporting should aim to promote safety, knowledge sharing and education. It is important to differentiate near misses that should be reported from voluntary reported events. Hospital’s management might award professionals who frequently report errors and provide solutions, Quality rather than quantity of reports should be emphasised with flexibility in the way near misses are reported.
Conclusion
The outcome of this study has benefits of understanding the attitudes of surgical professionals towards error reporting. It provides healthcare management with tool for enhancing safety and providing suitable training for their professionals.
Similar content being viewed by others
References
Kohn LT, Corrigan JM, Donaldson MS (2000) To err is human: building a safer health system. A report of the Committee on Quality of Health Care in America, Institute of Medicine. National Academy Press, Washington, DC
Francis N, Curtis N, Conti J, Foster J, Bonjer H, Hanna G (2018) EAES classification of intraoperative adverse events in laparoscopic surgery. Surg Endosc 32:3822–3829
Abe T, Murai S, Nasuhara Y, Shinohara N (2019) Characteristics of Medical Adverse Events/Near Misses Associated With Laparoscopic/Thoracoscopic Surgery: A Retrospective Study Based on the Japanese National Database of Medical Adverse Events. J Patient Saf 15:343
Bosma E, Veen E, Roukema J (2011) Incidence, nature and impact of error in surgery. Br J Surg 98:1654–1659
Soydemir D, Seren Intepeler S, Mert H (2017) Barriers to medical error reporting for physicians and nurses. West J Nurs Res 39:1348–1363
Uribe CL, Schweikhart SB, Pathak DS, Marsh GB, Fraley RR (2002) Perceived barriers to medical-error reporting: an exploratory investigation. J Healthc Manag 47:263
Gawande AA, Thomas EJ, Zinner MJ, Brennan TA (1999) The incidence and nature of surgical adverse events in Colorado and Utah in 1992. Surgery 126:66–75
Eva K, Regher G (2000) An organisation with a memory: report of an expert group on learning from adverse events in the NHS. Department of Health, Norwich, UK
Tang FI, Sheu SJ, Yu S, Wei IL, Chen CH (2007) Nurses relate the contributing factors involved in medication errors. J Clin Nurs 16:447–457
White A, Skelton M, Mushtaq F, Pike T, Mon-Williams M, Lodge J, Wilkie R (2015) Inconsistent reporting of minimally invasive surgery errors. Ann R Coll Surg Engl 97:608–612
Heard GC, Sanderson PM, Thomas RD (2012) Barriers to adverse event and error reporting in anesthesia. Anesth Analg 114:604–614
Shanafelt TD, Balch CM, Bechamps G, Russell T, Dyrbye L, Satele D, Collicott P, Novotny PJ, Sloan J, Freischlag J (2010) Burnout and medical errors among American surgeons. Ann Surg 251:995–1000
Al-Hakim L, Wang M, Xiao J, Gyomber D, Sengupta S (2019) Hierarchical task analysis for identification of interrelationships between ergonomic, external disruption, and internal disruption in complex laparoscopic procedures. Surg Endosc 33:3673–3687
Bonrath E, Zevin B, Dedy N, Grantcharov T (2013) Error rating tool to identify and analyse technical errors and events in laparoscopic surgery. Br J Surg 100:1080–1088
Howell A-M, Burns EM, Hull L, Mayer E, Sevdalis N, Darzi A (2017) International recommendations for national patient safety incident reporting systems: an expert Delphi consensus-building process. BMJ Qual Saf 26:150–163
Weissman JS, Rothschild JM, Bendavid E, Sprivulis P, Cook EF, Evans RS, Kaganova Y, Bender M, David-Kasdan J, Haug P (2007) Hospital workload and adverse events. Med Care 45:448–455
Ro H (2012) Moderator and mediator effects in hospitality research. Int J Hosp Manag 31:952–961
Satava R (2005) The nature of surgical error: a cautionary tale and a call to reason. Surg Endosc 19:1014–1016
Cuschieri A (2005) Reducing errors in the operating room: surgical proficiency and quality assurance of execution. Surg Endosc 19:1022–1027
Rosner B, Glynn RJ, Lee MLT (2006) The Wilcoxon signed rank test for paired comparisons of clustered data. Biometrics 62:185–192
Baron RM, Kenny DA (1986) The moderator–mediator variable distinction in social psychological research: conceptual, strategic, and statistical considerations. J Pers Soc Psychol 51:1173
Hayes AF (2017) Introduction to mediation, moderation, and conditional process analysis: a regression-based approach. Guilford Publications, New York
Bonrath EM, Gordon LE, Grantcharov TP (2015) Characterising ‘near miss’ events in complex laparoscopic surgery through video analysis. BMJ Qual Saf 24:516–521
Gallagher TH, Waterman AD, Ebers AG, Fraser VJ, Levinson W (2003) Patients’ and physicians’ attitudes regarding the disclosure of medical errors. JAMA 289:1001–1007
Frenkel DN, Liebman CB (2004) Words that heal. Ann Intern Med 140:482–483
Eadie A (2012) Medical error reporting should it be mandatory in Scotland? J Forensic Leg Med 19:437–441
Weissman JS, Annas CL, Epstein AM, Schneider EC, Clarridge B, Kirle L, Gatsonis C, Feibelmann S, Ridley N (2005) Error reporting and disclosure systems: views from hospital leaders. JAMA 293:1359–1366
WHO (2005) World alliance for patient safety: WHO draft guidelines for adverse event reporting and learning systems: from information to action. World Health Organization
Donn SM, McDonnell WM (2012) When bad things happen: adverse event reporting and disclosure as patient safety and risk management tools in the neonatal intensive care unit. Am J Perinatol 29:65–70
Al-Hakim L, Sengupta S, Xiao J (2017) Ergonomics perspective for identifying and reducing internal operative flow disruption for laparoscopic urological surgery. Surg Endosc 31:5043–5056
Wiegmann DA, ElBardissi AW, Dearani JA, Daly RC, Sundt TM (2007) Disruptions in surgical flow and their relationship to surgical errors: An exploratory investigation. Surgery 142:658–665
Etchells E, O’Neill C, Bernstein M (2003) Patient safety in surgery: error detection and prevention. World J Surg 27:936–941
Cannon MD, Edmondson AC (2005) Failing to learn and learning to fail (intelligently): how great organizations put failure to work to innovate and improve. Long Range Plan 38:299–319
Hemingway MW, O’Malley C, Silvestri S (2015) Safety culture and care: a program to prevent surgical errors. AORN J 101:404–415
Vincent C, Moorthy K, Sarker S, Chang A, Darzi A (2004) Systems approaches to surgical Quality and safety: from concept to measurement. Ann Surg 239:475–482
Acknowledgements
The authors would like to acknowledge the support of Professor Jian’an Wang, President of the Second Affiliated Hospital of Zhejiang University Medical School (SAHZU), Hangzhou, China, Professor Jiaquan Xiao, Director of the Urology Department, Dr Kai Sun, Department of Anesthesiology, Ms Mingli Yang, Director of Foreign Affair at SAHZU, and Ms Desleigh de Jonge, Research Fellow at the School of Health and Rehabilitation Sciences, The University of Queensland. Our acknowledgement and appreciation extended to all professionals who involved in the observational study and responded to our questionnaires.
Funding
No funding was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosure
Drs Yan, Wang, and Al-Hakim have no conflicts of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yan, M., Wang, M. & Al-Hakim, L. Barriers to reporting near misses and adverse events among professionals performing laparoscopic surgeries: a mixed methodology approach. Surg Endosc 35, 7015–7026 (2021). https://doi.org/10.1007/s00464-020-08215-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-08215-x