Abstract
Background
Endoscopic submucosal dissection (ESD) is a technically demanding procedure associated with a higher risk of complications. This study aimed to assess the difficulties and outcomes experienced by endoscopists beginning to perform ESD.
Methods
This prospective study investigated course participants in an ESD training workshop. The participants were asked at the end of the workshop about the ease of using various ESD knives, the occurrence of complications and their management, the procedural time, and the outcomes for the swine used for the procedure.
Results
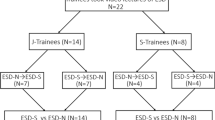
For this study, 24 endoscopists were trained in performing gastric and esophageal ESD techniques using a porcine model. The mean size of the specimen retrieved was 2.66 ± 1.18 cm. The mean procedural times were 52.09 ± 24.67 min for gastric ESD and 32.50 ± 8.45 min for esophageal ESD. During gastric ESD, 15 participants (65.22%) encountered perforations, whereas bleeding occurred during 13 ESDs (56.52%). There were two procedure-related mortalities. Significantly, a higher proportion of perforations were encountered with the use of noninsulated knives. The perforated and nonperforated groups did not show a difference in prior endoscopic experience (P = 0.335). The majority of the participants agreed that the swine model is appropriate for simulating both human gastric (96%) and esophageal (96%) ESD.
Conclusions
The ESD procedure is technically challenging and associated with a high rate of complications for beginners. The use of noninsulated knives may increase the risk of perforations during the learning curve for gastric ESD, and future prospective trials must evaluate their use. The development of training models may augment the acquisition of skills in low-volume centers but will not replace a standardized patient-based training program.


Similar content being viewed by others
References
Chiu PW, Chan KF, Lee YT, Sung JJ, Lau JY, Ng EK (2008) Endoscopic submucosal dissection used for treating early neoplasia of the foregut using a combination of knives. Surg Endosc 22:777–783
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Yamamichi N, Tateishi A, Shimizu Y, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2006) Endoscopic submucosal dissection of esophageal squamous cell neoplasms. Clin Gastroenterol Hepatol 4:688–694
Kakushima N, Fujishiro M, Kodashima S, Muraki Y, Tateishi A, Omata M (2006) A learning curve for endoscopic submucosal dissection of gastric epithelial neoplasms. Endoscopy 38:991–995
Imagawa A, Okada H, Kawahara Y, Takenaka R, Kato J, Kawamoto H, Fujiki S, Takata R, Yoshino T, Shiratori Y (2006) Endoscopic submucosal dissection for early gastric cancer: results and degrees of technical difficulty as well as success. Endoscopy 38:987–990
Tanaka S, Oka S, Kaneko I, Hirata M, Mouri R, Kanao H, Yoshida S, Chayama K (2007) Endoscopic submucosal dissection for colorectal neoplasia: possibility of standardization. Gastrointest Endosc 66:100–107
Kodama M, Kakegawa T (1998) Treatment of superficial cancer of the esophagus: a summary of responses to a questionnaire on superficial cancer of the esophagus in Japan. Surgery 123:432–439
Oka S, Tanaka S, Kaneko I, Mouri R, Hirata M, Kawamura T, Yoshihara M, Chayama K (2006) Advantage of endoscopic submucosal dissection compared with EMR for early gastric cancer. Gastrointest Endosc 64:877–883
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Yamamichi N, Tateishi A, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2007) Outcomes of endoscopic submucosal dissection for colorectal epithelial neoplasms in 200 consecutive cases. Clin Gastroenterol Hepatol 5:678–683
Okabayashi T, Gotoda T, Kondo H, Ono H, Oda I, Fujishiro M, Yachida S (2000) Usefulness of indigo carmine chromoendoscopy and endoscopic clipping for accurate preoperative assessment of proximal gastric cancer. Endoscopy 32:S62
Uedo N, Iishi H, Tatsuta M, Yamada T, Ogiyama H, Imanaka K, Sugimoto N, Higashino K, Ishihara R, Narahara H, Ishiguro S (2005) A novel videoendoscopy system by using autofluorescence and reflectance imaging for diagnosis of esophagogastric cancers. Gastrointest Endosc 62:521–528
Participants of the Paris Workshop (2003) The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach, and colon: November 30 to December 1, 2002. Gastrointest Endosc 58:S3–S43
Gotoda T, Yanagisawa A, Sasako M, Ono H, Nakanishi Y, Shimoda T, Kato Y (2000) Incidence of lymph node metastasis from early gastric cancer: estimation with a large number of cases at two large centers. Gastric Cancer 3:219–225
Gotoda T (2005) A large endoscopic resection by endoscopic submucosal dissection procedure for early gastric cancer. Clin Gastroenterol Hepatol 3:S71–S73
Inoue H, Satoh Y, Kazawa T, Sugaya S, Usui S, Satodate H, Kudo S (2004) Endoscopic submucosal dissection using a newly developed triangle-tip knife. Stomach Intest 39:73–75
Kodashima S, Fujishiro M, Yahagi N, Kakushima N, Ichinose M, Omata M (2006) Endoscopic submucosal dissection for gastric neoplasia: experience with the flex-knife. Acta Gastroenterol Belg 69:224–229
Fujishiro M, Yahagi N, Kakushima N, Kodashima S, Muraki Y, Ono S, Kobayashi K, Hashimoto T, Yamamichi N, Tateishi A, Shimizu Y, Oka M, Ogura K, Kawabe T, Ichinose M, Omata M (2006) Successful nonsurgical management of perforation complicating endoscopic submucosal dissection of gastrointestinal epithelial neoplasms. Endoscopy 38:1001–1006
Nelson DB, Bosco JJ, Curtis WD, Faigel DO, Kelsey PB, Leung JW, Mills MR, Smith P, Tarnasky PR, VanDam J, Wang KK, Wassef WY (1999) ASGE technology evaluation report: endoscopy simulators, May 1999. American Society for Gastrointestinal Endoscopy. Gastrointest Endosc 50:935–937
Sedlack R, Petersen B, Binmoeller K, Kolars J (2003) A direct comparison of ERCP teaching models. Gastrointest Endosc 57:886–890
Acknowledgments
We express our deepest appreciation for all the overseas faculties from Japan involved in organizing the ESD workshop including Professor Haruhiro Inoue, Digestive Disease Centre, Showa University; Dr. Takuji Gotoda, National Cancer Center Hospital; Dr Noriya Uedo, Osaka Medical Center for Cancer and Cardiovascular Diseases; and Dr. Naohisa Yahagi, Toranomon Hospital. We also thank Olympus Co. Ltd., Hong Kong, and Olympus Tokyo, Japan, for sponsoring the training workshop.
Disclosures
Anthony Y. B. Teoh, Philip W. Y. Chiu, Simon K. H. Wong, Joseph J. Y. Sung, James Y. W. Lau, and Enders K. W. Ng have no conflicts of interest or financial ties to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Teoh, A.Y.B., Chiu, P.W.Y., Wong, S.K.H. et al. Difficulties and outcomes in starting endoscopic submucosal dissection. Surg Endosc 24, 1049–1054 (2010). https://doi.org/10.1007/s00464-009-0724-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-009-0724-8