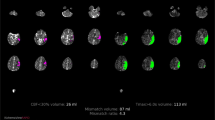
Abstract
Wake-up stroke (WUS) is a subgroup of ischemic stroke in which patients show no abnormality before sleep while wake up with neurological deficits. In addition to the uncertain onset, WUS patients have difficulty to receive prompt and effective thrombolytic or reperfusion therapy, leading to relatively poor prognosis. A number of researches have indicated that CT or MRI based thrombolysis and endovascular therapy might have benefits for WUS patients. This review article narratively discusses the pathogenesis, risk factors, imaging-based diagnosis and recanalization treatments of WUS with the purpose of expanding current treatment options for this group of stroke patients and exploring better therapeutic methods. The result showed that multimodal MRI or CT scan might be the best methods for extending the time window of WUS and, therefore, a large proportion of WUS patients could have favorable prognosis.
Similar content being viewed by others
References
Sun T, Xu Z, Diao SS, Zhang LL, Fang Q, Cai XY, Kong Y (2018) Safety and cost-effectiveness thrombolysis by diffusion-weighted imaging and fluid attenuated inversion recovery mismatch for wake-up stroke. Clin Neurol Neurosurg 170:47–52. https://doi.org/10.1016/j.clineuro.2018.04.027
Mackey J, Kleindorfer D, Sucharew H, Moomaw CJ, Kissela BM, Alwell K, Flaherty ML, Woo D, Khatri P, Adeoye O, Ferioli S, Khoury JC, Hornung R, Broderick JP (2011) Population-based study of wake-up strokes. Neurology 76(19):1662–1667. https://doi.org/10.1212/WNL.0b013e318219fb30
Serena J, Davalos A, Segura T, Mostacero E, Castillo J (2003) Stroke on awakening: looking for a more rational management. Cerebrovasc Dis (Basel, Switzerland) 16(2):128–133. https://doi.org/10.1159/000070592
Wouters A, Lemmens R, Dupont P, Thijs V (2014) Wake-up stroke and stroke of unknown onset: a critical review. Front Neurol 5:153. https://doi.org/10.3389/fneur.2014.00153
Kim TJ, Ko SB, Jeong HG, Lee JS, Kim CK, Kim Y, Nam K, Mo H, Joon An S, Choi HA, Yoon BW (2016) Nocturnal desaturation in the stroke unit is associated with wake-up ischemic stroke. Stroke 47(7):1748–1753. https://doi.org/10.1161/strokeaha.116.013266
Tanimoto A, Mehndiratta P, Koo BB (2014) Characteristics of wake-up stroke. J Stroke Cerebrovasc Dis 23(6):1296–1299. https://doi.org/10.1016/j.jstrokecerebrovasdis.2013.10.021
Spengos K, Tsivgoulis G, Manios E, Synetou M, Vassilopoulou S, Zakopoulos N, Vassilopoulos D, Vemmos KN (2005) Stroke etiology is associated with symptom onset during sleep. Sleep 28(2):233–238
Reid JM, Dai D, Cheripelli B, Christian C, Reidy Y, Gubitz GJ, Phillips SJ (2015) Differences in wake-up and unknown onset stroke examined in a stroke registry. Int J Stroke 10(3):331–335. https://doi.org/10.1111/ijs.12388
Okawa M, Amamoto T, Abe H, Yoshimura S, Higashi T, Inoue T (2015) Wake-up stroke in a young woman with rotational vertebral artery occlusion due to far-lateral cervical disc herniation. J Neurosurg Spine 23(2):166–169. https://doi.org/10.3171/2014.11.spine14393
Nishikawa H, Miya F, Kitano Y, Mori G, Shimizu S, Suzuki H (2017) Positional occlusion of vertebral artery due to cervical spondylosis as rare cause of wake-up stroke: report of two cases. World Neurosurg 98:877.e813–877.e821. https://doi.org/10.1016/j.wneu.2016.11.071
Hsieh SW, Lai CL, Liu CK, Hsieh CF, Hsu CY (2012) Obstructive sleep apnea linked to wake-up strokes. J Neurol 259(7):1433–1439. https://doi.org/10.1007/s00415-011-6370-9
Turin TC, Kita Y, Rumana N, Nakamura Y, Takashima N, Ichikawa M, Sugihara H, Morita Y, Hirose K, Okayama A, Miura K, Ueshima H (2013) Wake-up stroke: incidence, risk factors and outcome of acute stroke during sleep in a Japanese population. Takashima Stroke Registry 1988–2003. Eur Neurol 69(6):354–359. https://doi.org/10.1159/000346124
Siarnik P, Kollar B, Carnicka Z, Surda P, Klobucnikova K, Sykora M, Turcani P (2016) Association of sleep disordered breathing with wake-up acute ischemic stroke: a full polysomnographic study. J Clin Sleep Med JCSM 12(4):549–554. https://doi.org/10.5664/jcsm.5688
Koo BB, Bravata DM, Tobias LA, Mackey JS, Miech EJ, Matthias MS, Stahl SM, Sico JJ, Vaz Fragoso CA, Williams LS, Lampert R, Qin L, Yaggi HK (2016) Observational study of obstructive sleep apnea in wake-up stroke: the SLEEP TIGHT study. Cerebrovasc Dis (Basel, Switzerland) 41(5–6):233–241. https://doi.org/10.1159/000440736
Diniz DL, Barreto PR, Bruin PF (1992) Bruin VM (2016) Wake-up stroke: clinical characteristics, sedentary lifestyle, and daytime sleepiness. Rev Assoc Med Bras 62(7):628–634. https://doi.org/10.1590/1806-9282.62.07.628
Kim JS, Kim S, Lee SH, Lee HY, Lee SY, Im KB (2018) Increased risk of ischemic stroke during sleep in apneic patients. J Clin Neurol (Seoul, Korea) 14(2):174–178. https://doi.org/10.3988/jcn.2018.14.2.174
Brown DL, Li C, Chervin RD, Case E, Garcia NM, Tower SD, Lisabeth LD (2018) Wake-up stroke is not associated with sleep-disordered breathing in women. Neurol Clin Pract 8(1):8–14. https://doi.org/10.1212/cpj.0000000000000412
Xiao Z, Xie M, You Y, Wu H, Zhou G, Li M (2018) Wake-up stroke and sleep-disordered breathing: a meta-analysis of current studies. J Neurol 265(6):1288–1294. https://doi.org/10.1007/s00415-018-8810-2
Fu X, Li J, Wu JJ, Chen J, Huang JY, Mao CJ, Chen R, Liu CF (2019) Reduced cortical arousability to nocturnal apneic episodes in patients with wake-up ischemic stroke. Sleep Med. https://doi.org/10.1016/j.sleep.2019.09.007
Barreto PR, Diniz DLO, Lopes JP, Barroso MC, Daniele T, de Bruin PFC, de Bruin VMS (2019) Obstructive sleep apnea and wake-up stroke—a 12 months prospective longitudinal study. J Stroke Cerebrovasc dis. https://doi.org/10.1016/j.jstrokecerebrovasdis.2019.104564
Mohammad Y, Almutlaq A, Al-Ruwaita A, Aldrees A, Alsubaie A, Al-Hussain F (2019) Stroke during sleep and obstructive sleep apnea: there is a link. Neurol Sci 40(5):1001–1005. https://doi.org/10.1007/s10072-019-03753-2
Man H, Xu Y, Zhao Z, Zhang S, Lv R, Chi X, Li X, Zhang Z (2019) The coexistence of a patent foramen ovale and obstructive sleep apnea may increase the risk of wake-up stroke in young adults. Technol Health Care 27(S1):23–30. https://doi.org/10.3233/thc-199004
Hacke W, Kaste M, Bluhmki E, Brozman M, Davalos A, Guidetti D, Larrue V, Lees KR, Medeghri Z, Machnig T, Schneider D, von Kummer R, Wahlgren N, Toni D (2008) Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med 359(13):1317–1329. https://doi.org/10.1056/nejmoa0804656
National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group (1995) Tissue plasminogen activator for acute ischemic stroke. N Engl J Med 333(24):1581–1587. https://doi.org/10.1056/nejm199512143332401
Kang DW, Kwon JY, Kwon SU, Kim JS (2012) Wake-up or unclear-onset strokes: are they waking up to the world of thrombolysis therapy? Int J Stroke 7(4):311–320. https://doi.org/10.1111/j.1747-4949.2012.00779.x
Silva GS, Lima FO, Camargo EC, Smith WS, Singhal AB, Greer DM, Ay H, Lev MH, Harris GJ, Halpern EF, Sonni S, Koroshetz W, Furie KL (2010) Wake-up stroke: clinical and neuroimaging characteristics. Cerebrovasc Dis (Basel, Switzerland) 29(4):336–342. https://doi.org/10.1159/000278929
Breuer L, Huttner HB, Dorfler A, Schellinger PD, Kohrmann M (2010) Wake up stroke: overview on diagnostic and therapeutic options for ischemic stroke on awakening. Fortschr Neurol Psychiatr 78(2):101–106. https://doi.org/10.1055/s-0028-1109985
Huisa BN, Raman R, Ernstrom K, Tafreshi G, Stemer A, Meyer BC, Hemmen T (2010) Alberta Stroke Program Early CT Score (ASPECTS) in patients with wake-up stroke. J Stroke Cerebrovasc Dis 19(6):475–479. https://doi.org/10.1016/j.jstrokecerebrovasdis.2010.03.003
Koton S, Tanne D, Bornstein NM (2012) Ischemic stroke on awakening: patients’ characteristics, outcomes and potential for reperfusion therapy. Neuroepidemiology 39(3–4):149–153. https://doi.org/10.1159/000341242
Denny MC, Boehme AK, Dorsey AM, George AJ, Yeh AD, Albright KC, Martin-Schild S (2014) Wake-up strokes are similar to known-onset morning strokes in severity and outcome. J Neurol Neurol Disord. https://doi.org/10.15744/2454-4981.1.102
Nadeau JO, Fang J, Kapral MK, Silver FL, Hill MD (2005) Outcome after stroke upon awakening. Can J Neurol Sci Le journal canadien des sciences neurologiques 32(2):232–236
Bornstein NM, Gur AY, Fainshtein P, Korczyn AD (1999) Stroke during sleep: epidemiological and clinical features. Cerebrovasc Dis (Basel, Switzerland) 9(6):320–322. https://doi.org/10.1159/000016005
Barreto AD, Martin-Schild S, Hallevi H, Morales MM, Abraham AT, Gonzales NR, Illoh K, Grotta JC, Savitz SI (2009) Thrombolytic Therapy for patients who wake-up with stroke. Stroke 40(3):827
Barreto AD, Fanale CV, Alexandrov AV, Gaffney KC, Vahidy FS, Nguyen CB, Sarraj A, Rahbar M, Grotta JC, Savitz SI (2016) Prospective, open-label safety study of intravenous recombinant tissue plasminogen activator in wake-up stroke. Ann Neurol 80(2):211–218. https://doi.org/10.1002/ana.24700
Seyhan M, Mackenrodt D, Gunreben I, Müllges W, Haeusler KG, Pham M, Kleinschnitz C, Kraft P (2020) Should IV thrombolysis be given in patients with suspected ischemic stroke but unknown symptom onset and without diffusion-weighted imaging lesion?—results of a case-control study. J Stroke Cerebrovasc Dis 29(2):104515. https://doi.org/10.1016/j.jstrokecerebrovasdis.2019.104515
Thomalla G, Boutitie F, Fiebach JB, Simonsen CZ, Nighoghossian N, Pedraza S, Lemmens R, Roy P, Muir KW, Ebinger M, Ford I, Cheng B, Galinovic I, Cho TH, Puig J, Thijs V, Endres M, Fiehler J, Gerloff C (2017) Stroke with unknown time of symptom onset: baseline clinical and magnetic resonance imaging data of the first thousand patients in WAKE-UP (efficacy and safety of mri-based thrombolysis in wake-up stroke: a randomized, doubleblind, placebo-controlled trial). Stroke 48(3):770–773. https://doi.org/10.1161/strokeaha.116.015233
Kim YJ, Kim BJ, Kwon SU, Kim JS, Kang DW (2016) Unclear-onset stroke: daytime-unwitnessed stroke vs. wake-up stroke. Int J Stroke 11(2):212–220. https://doi.org/10.1177/1747493015616513
Manawadu D, Bodla S, Jarosz J, Keep J, Kalra L (2013) A case-controlled comparison of thrombolysis outcomes between wake-up and known time of onset ischemic stroke patients. Stroke 44(8):2226–2231. https://doi.org/10.1161/strokeaha.111.000757
Aghaebrahim A, Leiva-Salinas C, Jadhav AP, Jankowitz B, Zaidi S, Jumaa M, Urra X, Amorim E, Zhu G, Giurgiutiu DV, Horev A, Reddy V, Hammer M, Wechsler L, Wintermark M, Jovin T (2015) Outcomes after endovascular treatment for anterior circulation stroke presenting as wake-up strokes are not different than those with witnessed onset beyond 8 hours. J Neurointervent Surg 7(12):875–880. https://doi.org/10.1136/neurintsurg-2014-011316
Nogueira RG, Jadhav AP, Haussen DC, Bonafe A, Budzik RF, Bhuva P, Yavagal DR, Ribo M, Cognard C, Hanel RA, Sila CA, Hassan AE, Millan M, Levy EI, Mitchell P, Chen M, English JD, Shah QA, Silver FL, Pereira VM, Mehta BP, Baxter BW, Abraham MG, Cardona P, Veznedaroglu E, Hellinger FR, Feng L, Kirmani JF, Lopes DK, Jankowitz BT, Frankel MR, Costalat V, Vora NA, Yoo AJ, Malik AM, Furlan AJ, Rubiera M, Aghaebrahim A, Olivot JM, Tekle WG, Shields R, Graves T, Lewis RJ, Smith WS, Liebeskind DS, Saver JL, Jovin TG (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med 378(1):11–21. https://doi.org/10.1056/NEJMoa1706442
Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, McTaggart RA, Torbey MT, Kim-Tenser M, Leslie-Mazwi T, Sarraj A, Kasner SE, Ansari SA, Yeatts SD, Hamilton S, Mlynash M, Heit JJ, Zaharchuk G, Kim S, Carrozzella J, Palesch YY, Demchuk AM, Bammer R, Lavori PW, Broderick JP, Lansberg MG (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378(8):708–718. https://doi.org/10.1056/NEJMoa1713973
Ma H, Campbell BCV, Parsons MW, Churilov L, Levi CR, Hsu C, Kleinig TJ, Wijeratne T, Curtze S, Dewey HM, Miteff F, Tsai CH, Lee JT, Phan TG, Mahant N, Sun MC, Krause M, Sturm J, Grimley R, Chen CH, Hu CJ, Wong AA, Field D, Sun Y, Barber PA, Sabet A, Jannes J, Jeng JS, Clissold B, Markus R, Lin CH, Lien LM, Bladin CF, Christensen S, Yassi N, Sharma G, Bivard A, Desmond PM, Yan B, Mitchell PJ, Thijs V, Carey L, Meretoja A, Davis SM, Donnan GA (2019) Thrombolysis guided by perfusion imaging up to 9 hours after onset of stroke. N Engl J Med 380(19):1795–1803. https://doi.org/10.1056/nejmoa1813046
Campbell BCV, Ma H, Ringleb PA, Parsons MW, Churilov L, Bendszus M, Levi CR, Hsu C, Kleinig TJ, Fatar M, Leys D, Molina C, Wijeratne T, Curtze S, Dewey HM, Barber PA, Butcher KS, De Silva DA, Bladin CF, Yassi N, Pfaff JAR, Sharma G, Bivard A, Desmond PM, Schwab S, Schellinger PD, Yan B, Mitchell PJ, Serena J, Toni D, Thijs V, Hacke W, Davis SM, Donnan GA (2019) Extending thrombolysis to 4.5–9 h and wake-up stroke using perfusion imaging: a systematic review and meta-analysis of individual patient data. Lancet (London, England) 394(10193):139–147. https://doi.org/10.1016/s0140-6736(19)31053-0
Krebs S, Posekany A, Ferrari J, Lang W, Sommer P, Gattringer T, Boehme C, Sykora M (2019) Intravenous thrombolysis in wake-up stroke: real-world data from the Austrian Stroke Unit Registry. Eur J Neurol 26(5):754–759. https://doi.org/10.1111/ene.13884
Furlanis G, Ajcevic M, Buoite Stella A, Cillotto T, Caruso P, Ridolfi M, Cova MA, Naccarato M, Manganotti P (2019) Wake-up stroke: thrombolysis reduces ischemic lesion volume and neurological deficit. J Neurol. https://doi.org/10.1007/s00415-019-09603-7
Caruso P, Naccarato M, Furlanis G, Ajčević M, Stragapede L, Ridolfi M, Polverino P, Ukmar M, Manganotti P (2018) Wake-up stroke and CT perfusion: effectiveness and safety of reperfusion therapy. Neurol Sci 39(10):1705–1712. https://doi.org/10.1007/s10072-018-3486-z
Feil K, Reidler P, Kunz WG, Kupper C, Heinrich J, Laub C, Muller K, Voglein J, Liebig T, Dieterich M, Kellert L (2020) Addressing a real-life problem: treatment with intravenous thrombolysis and mechanical thrombectomy in acute stroke patients with an extended time window beyond 4.5 h based on computed tomography perfusion imaging. Eur J Neurol 27(1):168–174. https://doi.org/10.1111/ene.14051
Cortijo E, Garcia-Bermejo P, Calleja AI, Perez-Fernandez S, Gomez R, del Monte JM, Reyes J, Arenillas JF (2014) Intravenous thrombolysis in ischemic stroke with unknown onset using CT perfusion. Acta Neurol Scand 129(3):178–183. https://doi.org/10.1111/ane.12160
Morelli N, Rota E, Iafelice I, Petracca F, Magnacavallo A, Michieletti E, Guidetti D (2014) Parenchyma, pipes, perfusion and penumbra imaging: the multimodal CT in wake-up stroke basilar thrombosis. Eur Neurol 71(3–4):155–156. https://doi.org/10.1159/000355469
Hill MD, Kenney C, Dzialowski I, Boulanger JM, Demchuk AM, Barber PA, Watson TW, Weir NU, Buchan AM (2013) Tissue Window in Stroke Thrombolysis study (TWIST): a safety study. Can J Neurol Sci Le journal canadien des sciences neurologiques 40(1):17–20
Parsons MW, Pepper EM, Chan V, Siddique S, Rajaratnam S, Bateman GA, Levi CR (2005) Perfusion computed tomography: prediction of final infarct extent and stroke outcome. Ann Neurol 58(5):672–679. https://doi.org/10.1002/ana.20638
Campbell BCV, Majoie C, Albers GW, Menon BK, Yassi N, Sharma G, van Zwam WH, van Oostenbrugge RJ, Demchuk AM, Guillemin F, White P, Davalos A, van der Lugt A, Butcher KS, Cherifi A, Marquering HA, Cloud G, Macho Fernandez JM, Madigan J, Oppenheim C, Donnan GA, Roos Y, Shankar J, Lingsma H, Bonafe A, Raoult H, Hernandez-Perez M, Bharatha A, Jahan R, Jansen O, Richard S, Levy EI, Berkhemer OA, Soudant M, Aja L, Davis SM, Krings T, Tisserand M, San Roman L, Tomasello A, Beumer D, Brown S, Liebeskind DS, Bracard S, Muir KW, Dippel DWJ, Goyal M, Saver JL, Jovin TG, Hill MD, Mitchell PJ (2019) Penumbral imaging and functional outcome in patients with anterior circulation ischaemic stroke treated with endovascular thrombectomy versus medical therapy: a meta-analysis of individual patient-level data. Lancet Neurol 18(1):46–55. https://doi.org/10.1016/s1474-4422(18)30314-4
Roveri L, La Gioia S, Ghidinelli C, Anzalone N, De Filippis C, Comi G (2013) Wake-up stroke within 3 hours of symptom awareness: imaging and clinical features compared to standard recombinant tissue plasminogen activator treated stroke. J Stroke Cerebrovasc Dis 22(6):703–708. https://doi.org/10.1016/j.jstrokecerebrovasdis.2011.10.003
Kim JT, Park MS, Nam TS, Choi SM, Kim BC, Kim MK, Cho KH (2011) Thrombolysis as a factor associated with favorable outcomes in patients with unclear-onset stroke. Eur J Neurol 18(7):988–994. https://doi.org/10.1111/j.1468-1331.2011.03351.x
Kohrmann M, Juttler E, Fiebach JB, Huttner HB, Siebert S, Schwark C, Ringleb PA, Schellinger PD, Hacke W (2006) MRI versus CT-based thrombolysis treatment within and beyond the 3 h time window after stroke onset: a cohort study. Lancet Neurol 5(8):661–667. https://doi.org/10.1016/s1474-4422(06)70499-9
Schellinger PD, Thomalla G, Fiehler J, Kohrmann M, Molina CA, Neumann-Haefelin T, Ribo M, Singer OC, Zaro-Weber O, Sobesky J (2007) MRI-based and CT-based thrombolytic therapy in acute stroke within and beyond established time windows: an analysis of 1210 patients. Stroke 38(10):2640–2645. https://doi.org/10.1161/strokeaha.107.483255
Thomalla G, Cheng B, Ebinger M, Hao Q, Tourdias T, Wu O, Kim JS, Breuer L, Singer OC, Warach S, Christensen S, Treszl A, Forkert ND, Galinovic I, Rosenkranz M, Engelhorn T, Kohrmann M, Endres M, Kang DW, Dousset V, Sorensen AG, Liebeskind DS, Fiebach JB, Fiehler J, Gerloff C (2011) DWI-FLAIR mismatch for the identification of patients with acute ischaemic stroke within 4.5 h of symptom onset (PRE-FLAIR): a multicentre observational study. Lancet Neurol 10(11):978–986. https://doi.org/10.1016/s1474-4422(11)70192-2
Wei XE, Zhou J, Li WB, Zhao YW, Li MH, Li YH (2017) MRI based thrombolysis for FLAIR-negative stroke patients within 4.5-6 h after symptom onset. J Neurol Sci 372:421–427. https://doi.org/10.1016/j.jns.2016.11.010
Emeriau S, Serre I, Toubas O, Pombourcq F, Oppenheim C, Pierot L (2013) Can diffusion-weighted imaging-fluid-attenuated inversion recovery mismatch (positive diffusion-weighted imaging/negative fluid-attenuated inversion recovery) at 3 Tesla identify patients with stroke at < 4.5 hours? Stroke 44(6):1647–1651. https://doi.org/10.1161/strokeaha.113.001001
Kim BJ, Kim HJ, Lee DH, Kwon SU, Kim SJ, Kim JS, Kang DW (2014) Diffusion-weighted image and fluid-attenuated inversion recovery image mismatch: unclear-onset versus clear-onset stroke. Stroke 45(2):450–455. https://doi.org/10.1161/strokeaha.113.002830
Tortuyaux R, Ferrigno M, Dequatre-Ponchelle N, Djelad S, Cordonnier C, Henon H, Leys D (2019) Cerebral ischaemia with unknown onset: outcome after recanalization procedure. Revue neurologique. https://doi.org/10.1016/j.neurol.2019.05.004
Galinovic I, Boutitie F, Fiebach JB, Villringer K, Cheng B, Ebinger M, Endres M, Fiehler J, Ford I, Thijs V, Lemmens R, Muir KW, Nighoghossian N, Pedraza S, Simonsen CZ, Roy P, Gerloff C, Thomalla G (2019) Post-hoc analysis of outcome of intravenous thrombolysis in infarcts of infratentorial localization in the WAKE-UP trial. Front Neurol 10:983. https://doi.org/10.3389/fneur.2019.00983
Lee H, Lee EJ, Ham S, Lee HB, Lee JS, Kwon SU, Kim JS, Kim N, Kang DW (2020) Machine learning approach to identify stroke within 4.5 hours. Stroke. https://doi.org/10.1161/strokeaha.119.027611
Thomalla G, Simonsen CZ, Boutitie F, Andersen G, Berthezene Y, Cheng B, Cheripelli B, Cho TH, Fazekas F, Fiehler J, Ford I, Galinovic I, Gellissen S, Golsari A, Gregori J, Gunther M, Guibernau J, Hausler KG, Hennerici M, Kemmling A, Marstrand J, Modrau B, Neeb L, Perez de la Ossa N, Puig J, Ringleb P, Roy P, Scheel E, Schonewille W, Serena J, Sunaert S, Villringer K, Wouters A, Thijs V, Ebinger M, Endres M, Fiebach JB, Lemmens R, Muir KW, Nighoghossian N, Pedraza S, Gerloff C (2018) MRI-guided thrombolysis for stroke with unknown time of onset. N Engl J Med. https://doi.org/10.1056/NEJMoa1804355
Mourand I, Milhaud D, Arquizan C, Lobotesis K, Schaub R, Machi P, Ayrignac X, Eker OF, Bonafe A, Costalat V (2016) Favorable bridging therapy based on DWI-FLAIR mismatch in patients with unclear-onset stroke. AJNR Am J Neuroradiol 37(1):88–93. https://doi.org/10.3174/ajnr.A4574
Caliandro P, Reale G, Tartaglione T, Rossini PM (2016) The challenge of basilar artery occlusion wake-up stroke: too late for intravenous thrombolysis? Neurol Sci 37(7):1137–1140. https://doi.org/10.1007/s10072-016-2539-4
Aoki J, Sakamoto Y, Kimura K (2016) Intravenous thrombolysis increases the rate of dramatic recovery in patients with acute stroke with an unknown onset time and negative FLAIR MRI. J Neuroimaging 26(4):414–419. https://doi.org/10.1111/jon.12323
Jakubicek S, Krebs S, Posekany A, Ferrari J, Szabo J, Siarnik P, Lang W, Sykora M (2019) Modified DWI-FLAIR mismatch guided thrombolysis in unknown onset stroke. J Thromb Thromb 47(2):167–173. https://doi.org/10.1007/s11239-018-1766-3
Huisa BN, Liebeskind DS, Raman R, Hao Q, Meyer BC, Meyer DM, Hemmen TM (2013) Diffusion-weighted imaging-fluid attenuated inversion recovery mismatch in nocturnal stroke patients with unknown time of onset. J Stroke Cerebrovasc Dis 22(7):972–977. https://doi.org/10.1016/j.jstrokecerebrovasdis.2012.01.004
Odland A, Saervoll P, Advani R, Kurz MW, Kurz KD (2015) Are the current MRI criteria using the DWI-FLAIR mismatch concept for selection of patients with wake-up stroke to thrombolysis excluding too many patients? Scandinavian journal of trauma, resuscitation and emergency medicine 23:22. https://doi.org/10.1186/s13049-015-0101-7
Bardutzky J, Shen Q, Bouley J, Sotak CH, Duong TQ, Fisher M (2005) Perfusion and diffusion imaging in acute focal cerebral ischemia: temporal vs. spatial resolution. Brain Res 1043(1–2):155–162. https://doi.org/10.1016/j.brainres.2005.02.073
Cheng Q, Xu X, Zu Q, Lu S, Yu J, Liu X, Wang B, Shi H, Teng G, Liu S (2016) High b value DWI in evaluation of the hyperacute cerebral ischemia at 3T: a comparative study in an embolic canine stroke model. Exp Ther Med 12(2):951–956. https://doi.org/10.3892/etm.2016.3403
Davis SM, Donnan GA, Parsons MW, Levi C, Butcher KS, Peeters A, Barber PA, Bladin C, De Silva DA, Byrnes G, Chalk JB, Fink JN, Kimber TE, Schultz D, Hand PJ, Frayne J, Hankey G, Muir K, Gerraty R, Tress BM, Desmond PM (2008) Effects of alteplase beyond 3 h after stroke in the Echoplanar Imaging Thrombolytic Evaluation Trial (EPITHET): a placebo-controlled randomised trial. Lancet Neurol 7(4):299–309. https://doi.org/10.1016/s1474-4422(08)70044-9
Reid E, Graham D, Lopez-Gonzalez MR, Holmes WM, Macrae IM, McCabe C (2012) Penumbra detection using PWI/DWI mismatch MRI in a rat stroke model with and without comorbidity: comparison of methods. J Cereb Blood Flow Metab 32(9):1765–1777. https://doi.org/10.1038/jcbfm.2012.69
Mishra NK, Albers GW, Davis SM, Donnan GA, Furlan AJ, Hacke W, Lees KR (2010) Mismatch-based delayed thrombolysis. A meta-analysis. Stroke 41(1):e25–e33. https://doi.org/10.1161/strokeaha.109.566869
Amiri H, Bluhmki E, Bendszus M, Eschenfelder CC, Donnan GA, Leys D, Molina C, Ringleb PA, Schellinger PD, Schwab S, Toni D, Wahlgren N, Hacke W (2016) European cooperative acute stroke study-4: extending the time for thrombolysis in emergency neurological deficits ECASS-4: ExTEND. Int J Stroke 11(2):260–267. https://doi.org/10.1177/1747493015620805
Thomalla G, Schwark C, Sobesky J, Bluhmki E, Fiebach JB, Fiehler J, Zaro Weber O, Kucinski T, Juettler E, Ringleb PA, Zeumer H, Weiller C, Hacke W, Schellinger PD, Rother J (2006) Outcome and symptomatic bleeding complications of intravenous thrombolysis within 6 hours in MRI-selected stroke patients: comparison of a German multicenter study with the pooled data of ATLANTIS, ECASS, and NINDS tPA trials. Stroke 37(3):852–858. https://doi.org/10.1161/01.str.0000204120.79399.72
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL (2018) 2018 guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. https://doi.org/10.1161/str.0000000000000158
Heiss WD, Zaro Weber O (2017) Validation of MRI determination of the penumbra by PET measurements in ischemic stroke. J Nucl Med 58(2):187–193. https://doi.org/10.2967/jnumed.116.185975
Hansen MB, Nagenthiraja K, Ribe LR, Dupont KH, Østergaard L, Mouridsen K (2016) Automated estimation of salvageable tissue: comparison with expert readers. J Magn Reson Imaging 43(1):220–228. https://doi.org/10.1002/jmri.24963
Lansberg MG, Straka M, Kemp S, Mlynash M, Wechsler LR, Jovin TG, Wilder MJ, Lutsep HL, Czartoski TJ, Bernstein RA, Chang CW, Warach S, Fazekas F, Inoue M, Tipirneni A, Hamilton SA, Zaharchuk G, Marks MP, Bammer R, Albers GW (2012) MRI profile and response to endovascular reperfusion after stroke (DEFUSE 2): a prospective cohort study. Lancet Neurol 11(10):860–867. https://doi.org/10.1016/s1474-4422(12)70203-x
Albers GW, Thijs VN, Wechsler L, Kemp S, Schlaug G, Skalabrin E, Bammer R, Kakuda W, Lansberg MG, Shuaib A, Coplin W, Hamilton S, Moseley M, Marks MP (2006) Magnetic resonance imaging profiles predict clinical response to early reperfusion: the diffusion and perfusion imaging evaluation for understanding stroke evolution (DEFUSE) study. Ann Neurol 60(5):508–517. https://doi.org/10.1002/ana.20976
Scheldeman L, Wouters A, Dupont P, Cheng B, Ebinger M, Endres M, Fiebach JB, Gerloff C, Muir KW, Nighoghossian N, Pedraza S, Simonsen CZ, Boutitie F, Thomalla G, Lemmens R (2019) Total mismatch in diffusion negative patients in the WAKE-UP trial. Int J Stroke 14(7):Np20–Np22. https://doi.org/10.1177/1747493019875238
Iosif C, Oppenheim C, Trystram D, Domigo V, Meder JF (2008) MR imaging-based decision in thrombolytic therapy for stroke on awakening: report of 2 cases. AJNR Am J Neuroradiol 29(7):1314–1316. https://doi.org/10.3174/ajnr.A1069
Cho AH, Sohn SI, Han MK, Lee DH, Kim JS, Choi CG, Sohn CH, Kwon SU, Suh DC, Kim SJ, Bae HJ, Kang DW (2008) Safety and efficacy of MRI-based thrombolysis in unclear-onset stroke A preliminary report. Cerebrovasc Dis (Basel, Switzerland) 25(6):572–579. https://doi.org/10.1159/000132204
Kang DW, Sohn SI, Hong KS, Yu KH, Hwang YH, Han MK, Lee J, Park JM, Cho AH, Kim HJ, Kim DE, Cho YJ, Koo J, Yun SC, Kwon SU, Bae HJ, Kim JS (2012) Reperfusion therapy in unclear-onset stroke based on MRI evaluation (RESTORE): a prospective multicenter study. Stroke 43(12):3278–3283. https://doi.org/10.1161/strokeaha.112.675926
Ebinger M, Scheitz JF, Kufner A, Endres M, Fiebach JB, Nolte CH (2012) MRI-based intravenous thrombolysis in stroke patients with unknown time of symptom onset. Eur J Neurol 19(2):348–350. https://doi.org/10.1111/j.1468-1331.2011.03504.x
Lassalle L, Turc G, Tisserand M, Charron S, Roca P, Lion S, Legrand L, Edjlali M, Naggara O, Meder JF, Mas JL, Baron JC, Oppenheim C (2016) ASPECTS (Alberta Stroke Program Early CT Score) assessment of the perfusion-diffusion mismatch. Stroke 47(10):2553–2558. https://doi.org/10.1161/strokeaha.116.013676
Ogata T, Nagakane Y, Christensen S, Ma H, Campbell BC, Churilov L, Olivot JM, Desmond PM, Albers GW, Davis SM, Donnan GA (2011) A topographic study of the evolution of the MR DWI/PWI mismatch pattern and its clinical impact: a study by the EPITHET and DEFUSE Investigators. Stroke 42(6):1596–1601. https://doi.org/10.1161/strokeaha.110.609016
Guo C, Bai Q, Zhao Z, Zhang J (2019) Recombinant tissue-type plasminogen activator study of wake-up ischemic strokes guided by rapid MRI. Cerebrovasc Dis (Basel, Switzerland) 48(1–2):85–90. https://doi.org/10.1159/000503379
Ho KC, Speier W, Zhang H, Scalzo F, El-Saden S, Arnold CW (2019) A machine learning approach for classifying ischemic stroke onset time from imaging. IEEE Trans Med Imaging 38(7):1666–1676. https://doi.org/10.1109/tmi.2019.2901445
Legrand L, Tisserand M, Turc G, Edjlali M, Calvet D, Trystram D, Roca P, Naggara O, Mas J-L, Méder J-F, Baron J-C, Oppenheim C (2016) Fluid-attenuated inversion recovery vascular hyperintensities–diffusion-weighted imaging mismatch identifies acute stroke patients most likely to benefit from recanalization. Stroke 47(2):424
Legrand L, Turc G, Edjlali M, Beaumont M, Gautheron V, Ben Hassen W, Charron S, Trystram D, Boulouis G, Bourcier R, Benzakoun J, Naggara O, Clarencon F, Bracard S, Oppenheim C (2019) Benefit from revascularization after thrombectomy according to FLAIR vascular hyperintensities-DWI mismatch. Eur Radiol 29(10):5567–5576. https://doi.org/10.1007/s00330-019-06094-y
Duchaussoy T, Budzik JF, Norberciak L, Colas L, Pasquini M, Verclytte S (2019) Synthetic T2 mapping is correlated with time from stroke onset: a future tool in wake-up stroke management? Eur Radiol 29(12):7019–7026. https://doi.org/10.1007/s00330-019-06270-0
Legge J, Graham A, Male S, Copeland D, Lee R, Goyal N, Zand R (2017) Fluid-attenuated inversion recovery (FLAIR) signal intensity can identify stroke within 6 and 8 hours. J Stroke Cerebrovasc Dis 26(7):1582–1587. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.02.030
Cheng B, Boutitie F, Nickel A, Wouters A, Cho TH, Ebinger M, Endres M, Fiebach JB, Fiehler J, Galinovic I, Puig J, Thijs V, Lemmens R, Muir KW, Nighoghossian N, Pedraza S, Simonsen CZ, Gerloff C, Thomalla G (2020) Quantitative signal intensity in fluid-attenuated inversion recovery and treatment effect in the WAKE-UP trial. Stroke 51(1):209–215. https://doi.org/10.1161/strokeaha.119.027390
Kao HW, Tsai FY, Hasso AN (2012) Predicting stroke evolution: comparison of susceptibility-weighted MR imaging with MR perfusion. Eur Radiol 22(7):1397–1403. https://doi.org/10.1007/s00330-012-2387-4
Tsai JP, Albers GW (2017) Wake-up stroke: current understanding. Top Magn Resonan Imaging TMRI 26(3):97–102. https://doi.org/10.1097/rmr.0000000000000126
Parsons MW, Christensen S, McElduff P, Levi CR, Butcher KS, De Silva DA, Ebinger M, Barber PA, Bladin C, Donnan GA, Davis SM (2010) Pretreatment diffusion- and perfusion-MR lesion volumes have a crucial influence on clinical response to stroke thrombolysis. J Cereb Blood Flow Metab 30(6):1214–1225. https://doi.org/10.1038/jcbfm.2010.3
Kidwell CS, Chalela JA, Saver JL et al (2004) Comparison of mri and ct for detection of acute intracerebral hemorrhage. JAMA 292(15):1823–1830. https://doi.org/10.1001/jama.292.15.1823
Greer DM, Koroshetz WJ, Cullen S, Gonzalez RG, Lev MH (2004) Magnetic resonance imaging improves detection of intracerebral hemorrhage over computed tomography after intra-arterial thrombolysis. Stroke 35(2):491–495. https://doi.org/10.1161/01.str.0000114201.11353.c5
Edgell RC, Vora NA (2012) Neuroimaging markers of hemorrhagic risk with stroke reperfusion therapy. Neurology 79(13 Suppl 1):S100–S104. https://doi.org/10.1212/WNL.0b013e3182695848
Kuruvilla A, Norris GM, Xavier AR (2011) Acute endovascular recanalization therapy in wake-up stroke. J Neurol Sci 300(1–2):148–150. https://doi.org/10.1016/j.jns.2010.10.019
Bracco S, Tassi R, Gennari P, Grazzini I, Leonini S, D’Andrea P, Martini G, Cerase A (2013) Wake-up (or wake-up for) stroke: a treatable stroke. Neuroradiol J 26(5):573–578. https://doi.org/10.1177/197140091302600511
Kuntze Soderqvist A, Andersson T, Wahlgren N, Kaijser M (2016) Mechanical thrombectomy in acute ischemic stroke-patients with wake-up stroke and the elderly may benefit as well. J Stroke Cerebrovasc Dis 25(9):2276–2283. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.05.019
Rifino N, Filizzolo MG, Sangalli D, Basilico P, Mantero V, Scaccabarozzi C, Salmaggi A (2019) Thrombectomy for wake-up stroke in a patient with mild symptoms and in an adolescent. Can J Neurol Sci Le journal canadien des sciences neurologiques. https://doi.org/10.1017/cjn.2019.299
Rangel-Castilla L, Siddiqui AH (2019) Azygous anterior cerebral artery acute occlusion managed with endovascular mechanical thrombectomy: 2-dimensional operative video. Oper Neurosurg (Hagerstown, Md) 16(4):514–515. https://doi.org/10.1093/ons/opy183
Alsahli K, Cheung AK, Wijesuriya N, Cordato D, Zagami AS, Wenderoth JD, Chiu AH, Tay K, Cappelen-Smith C (2019) Thrombectomy in stroke of unknown onset, wake up stroke and late presentations: australian experience from 2 comprehensive stroke centres. J Clin Neurosci 59:136–140. https://doi.org/10.1016/j.jocn.2018.10.114
Kahles T, Garcia-Esperon C, Zeller S, Hlavica M, Anon J, Diepers M, Nedeltchev K, Remonda L (2016) Mechanical thrombectomy using the new eric retrieval device is feasible, efficient, and safe in acute ischemic stroke: a swiss stroke center experience. AJNR Am J Neuroradiol 37(1):114–119. https://doi.org/10.3174/ajnr.A4463
Jung S, Gralla J, Fischer U, Mono ML, Weck A, Ludi R, Heldner MR, Findling O, El-Koussy M, Brekenfeld C, Schroth G, Mattle HP, Arnold M (2013) Safety of endovascular treatment beyond the 6-h time window in 205 patients. Eur J Neurol 20(6):865–871. https://doi.org/10.1111/ene.12069
Nakiri GS, Castro-Afonso LH, Monsignore LM, Dias FA, Alessio-Alves FF, Fabio SR, Camilo MR, Cougo-Pinto PT, Leite JP, Pontes-Neto OM, Abud DG (2017) Experience on mechanical thrombectomy for acute stroke treatment in a Brazilian University Hospital. J Stroke Cerebrovasc Dis 26(3):532–537. https://doi.org/10.1016/j.jstrokecerebrovasdis.2016.11.128
Konstas AA, Minaeian A, Ross IB (2017) Mechanical thrombectomy in wake-up strokes: a case series using alberta stroke program early CT score (ASPECTS) for patient selection. J Stroke Cerebrovasc Dis 26(7):1609–1614. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.02.024
Stampfl S, Ringleb PA, Haehnel S, Rocco A, Herweh C, Hametner C, Pham M, Moehlenbruch M, Bendszus M, Rohde S (2013) Recanalization with stent-retriever devices in patients with wake-up stroke. AJNR Am J Neuroradiol 34(5):1040–1043. https://doi.org/10.3174/ajnr.A3357
Bhuva P, Yoo AJ, Jadhav AP, Jovin TG, Haussen DC, Bonafe A, Budzik RJ, Yavagal DR, Hanel RA, Hassan AE, Ribo M, Cognard C, Sila CA, Morgan PM, Zhang Y, Shields R, Smith W, Saver JL, Liebeskind DS, Nogueira RG (2019) Noncontrast computed tomography alberta stroke program early CT score may modify intra-arterial treatment effect in DAWN. Stroke 50(9):2404–2412. https://doi.org/10.1161/strokeaha.118.024583
Santos T, Carvalho A, Cunha AA, Rodrigues M, Gregorio T, Paredes L, Costa H, Roriz JM, Pinho J, Veloso M, Castro S, Barros P, Ribeiro M (2019) NCCT and CTA-based imaging protocol for endovascular treatment selection in late presenting or wake-up strokes. J Neurointervent Surg 11(2):200–203. https://doi.org/10.1136/neurintsurg-2018-014051
Jadhav AP, Aghaebrahim A, Jankowitz BT, Haussen DC, Budzik RF, Bonafe A, Bhuva P, Yavagal DR, Hanel RA, Hassan AE, Ribo M, Cognard C, Sila CA, Zhang Y, Smith WS, Saver JL, Liebeskind DS, Nogueira RG, Jovin TG (2019) Benefit of endovascular thrombectomy by mode of onset: secondary analysis of the DAWN trial. Stroke 50(11):3141–3146. https://doi.org/10.1161/strokeaha.119.025795
Li X, Wu L, Xie H, Bao Y, He D, Luo X (2020) Endovascular treatment for ischemic stroke beyond the time window: a meta-analysis. Acta Neurol Scand 141(1):3–13. https://doi.org/10.1111/ane.13161
Hiraga A (2012) Can we extend thrombolytic treatment for wake-up stroke? Neuroepidemiology 39(3–4):154–155. https://doi.org/10.1159/000341747
Funding
This work was supported by the grant of Clinical Research Innovation Plan of Shanghai General Hospital (Grant No. CTCCR-2018B03).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Zhang, YL., Zhang, JF., Wang, XX. et al. Wake-up stroke: imaging-based diagnosis and recanalization therapy. J Neurol 268, 4002–4012 (2021). https://doi.org/10.1007/s00415-020-10055-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-020-10055-7