Abstract
Introduction
Infection is a common complication of open fractures potentially leading to nonunion, functional loss, and even amputation. Perioperative antibiotic prophylaxis (PAP) is standard practice for infection prevention in the management of open fractures. However, optimal duration of PAP remains controversial. The objectives were to assess whether PAP duration is independently associated with infection in open fractures and if administration of PAP beyond the commonly-recommended limit of 72 h has any effect on the infection rate.
Materials and methods
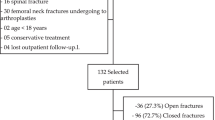
Over a 14-year period from 2003 to 2017, 530 skeletally-mature patients with operatively-treated, non-pathologic, long-bone open fractures were treated at one institution. Twenty-eight patients were excluded because of death or loss to follow-up and the remaining 502 patients (with 559 open fractures) who completed a 24-month follow-up were included in this retrospective study. The outcome was fracture-related infection (FRI), defined by the criteria of a recent consensus definition. A logistic generalized estimating equations regression model was conducted, including PAP duration and variables selected by a least absolute shrinkage and selection operator (LASSO) method, to assess the association between PAP duration and FRI. Propensity score analysis using a 72-h cut-off was performed to further cope with confounding.
Results
PAP duration, adjusted for the LASSO selected predictors, was independently associated with FRI (OR: 1.11 [95%CI, 1.04–1.19] for every one-day increase in PAP duration, p = 0.003). PAP duration longer than 72 h did not significantly increase the odds for FRI compared to shorter durations (p = 0.06, analysis adjusted for propensity score).
Conclusions
This study found no evidence that administration of prophylactic antibiotics beyond 72 h in patients with long-bone open fractures is warranted. Analyses adjusted for known confounders even revealed a higher risk for FRI for longer PAP. However, this effect cannot necessarily be considered as causal and further research is needed.

Similar content being viewed by others
References
Metsemakers WJ, Kuehl R, Moriarty TF, Richards RG, Verhofstad MHJ, Borens O, Kates S, Morgenstern M (2018) Infection after fracture fixation: current surgical and microbiological concepts. Injury 49(3):511–522
Papakostidis C, Kanakaris NK, Pretel J, Faour O, Morell DJ, Giannoudis PV (2011) Prevalence of complications of open tibial shaft fractures stratified as per the Gustilo–Anderson classification. Injury 42(12):1408–1415
Gustilo RB, Anderson JT (1976) Prevention of infection in the treatment of one thousand and twenty-five open fractures of long bones: retrospective and prospective analyses. J Bone Jt Surg Am 58(4):453–458
Gustilo RB, Mendoza RM, Williams DN (1984) Problems in the management of type III (severe) open fractures: a new classification of type III open fractures. J Trauma 24(8):742–746
Dunkel N, Pittet D, Tovmirzaeva L, Suva D, Bernard L, Lew D, Hoffmeyer P, Uckay I: Short duration of antibiotic prophylaxis in open fractures does not enhance risk of subsequent infection. Bone Joint J 2013, 95-b(6):831–837.
Kortram K, Bezstarosti H, Metsemakers WJ, Raschke MJ, Van Lieshout EMM, Verhofstad MHJ (2017) Risk factors for infectious complications after open fractures; a systematic review and meta-analysis. Int Orthop 41(10):1965–1982
Zalavras CG (2017) Prevention of infection in open fractures. Infect Dis Clin North Am 31(2):339–352
Zalavras CG, Marcus RE, Levin LS, Patzakis MJ (2007) Management of open fractures and subsequent complications. J Bone Jt Surg Am 89(4):884–895
Puetzler J, Zalavras C, Moriarty TF, Verhofstad MHJ, Kates SL, Raschke MJ, Rosslenbroich S, Metsemakers WJ (2019) Clinical practice in prevention of fracture-related infection: an international survey among 1197 orthopaedic trauma surgeons. Injury 50(6):1208–1215
Obremskey W, Molina C, Collinge C, Nana A, Tornetta P 3rd, Sagi C, Schmidt A, Probe R, Ahn J, Browner BD (2014) Current practice in the management of open fractures among orthopaedic trauma surgeons. Part A: initial management. A survey of orthopaedic trauma surgeons. J Orthop Trauma 28(8):e198–202
Gumbel D, Matthes G, Napp M, Lange J, Hinz P, Spitzmuller R, Ekkernkamp A (2016) Current management of open fractures: results from an online survey. Arch Orthop Trauma Surg 136(12):1663–1672
Dellinger EP, Caplan ES, Weaver LD, Wertz MJ, Droppert BM, Hoyt N, Brumback R, Burgess A, Poka A, Benirschke SK et al (1988) Duration of preventive antibiotic administration for open extremity fractures. Arch Surg 123(3):333–339
Carsenti-Etesse H, Doyon F, Desplaces N, Gagey O, Tancrede C, Pradier C, Dunais B, Dellamonica P (1999) Epidemiology of bacterial infection during management of open leg fractures. Eur J Clin Microbiol Infect Dis 18(5):315–323
Chang Y, Bhandari M, Zhu KL, Mirza RD, Ren M, Kennedy SA, Negm A, Bhatnagar N, Naji FN, Milovanovic L et al (2019) Antibiotic prophylaxis in the management of open fractures: a systematic survey of current practice and recommendations. JBJS Rev 7(2):e1
Hoff WS, Bonadies JA, Cachecho R, Dorlac WC (2011) East Practice Management Guidelines Work Group: update to practice management guidelines for prophylactic antibiotic use in open fractures. J Trauma 70(3):751–754
Nanchahal J, Nayagam S, Khan U, Moran C, Barrett S, Sanderson F, Pallisher I (2009) Standards for the management of open fractures of the lower limb. The Royal Society of Medicine Press Ltd, UK
Obremskey WT, Metsemakers WJ, Schlatterer DR, Tetsworth K, Egol K, Kates S, McNally M, Gibbons J, Kenny P, Stangl P et al (2020) Musculoskeletal infection in orthopaedic trauma: assessment of the 2018 international consensus meeting on musculoskeletal infection. J Bone Jt Surg Am (Epub ahead of print)
Messner J, Papakostidis C, Giannoudis PV, Kanakaris NK (2017) Duration of administration of antibiotic agents for open fractures: meta-analysis of the existing evidence. Surg Infect (Larchmt) 18(8):854–867
Pape HC, Lefering R, Butcher N, Peitzman A, Leenen L, Marzi I, Lichte P, Josten C, Bouillon B, Schmucker U et al (2014) The definition of polytrauma revisited: an international consensus process and proposal of the new 'Berlin definition'. J Trauma Acute Care Surg 77(5):780–786
Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, Prokuski L, Sirkin MS, Ziran B, Henley B et al (2007) Fracture and dislocation classification compendium—2007: orthopaedic trauma association classification, database and outcomes committee. J Orthop Trauma 21(10 Suppl):S1–133
Declercq P, Nijs S, D'Hoore A, Van Wijngaerden E, Wolthuis A, de Buck van Overstraeten A, Wauters J, Spriet I (2016) Augmented renal clearance in non-critically ill abdominal and trauma surgery patients is an underestimated phenomenon: a point prevalence study. J Trauma Acute Care Surg 81(3):468–477
Udy AA, Varghese JM, Altukroni M, Briscoe S, McWhinney BC, Ungerer JP, Lipman J, Roberts JA (2012) Subtherapeutic initial beta-lactam concentrations in select critically ill patients: association between augmented renal clearance and low trough drug concentrations. Chest 142(1):30–39
Declercq P, Gijsen M, Meijers B, Schetz M, Nijs S, D'Hoore A, Wauters J, Spriet I (2018) Reliability of serum creatinine-based formulae estimating renal function in non-critically ill surgery patients: focus on augmented renal clearance. J Clin Pharm Ther 45(5):695–706
Metsemakers WJ, Morgenstern M, McNally MA, Moriarty TF, McFadyen I, Scarborough M, Athanasou NA, Ochsner PE, Kuehl R, Raschke M et al (2018) Fracture-related infection: a consensus on definition from an international expert group. Injury 49(3):505–510
Yuan M, Lin Y (2006) Model selection and estimation in regression with grouped variables. J R Stat Soc Series B (Statistical Methodology) 68(1):49–67
Rosenbaum PR, Rubin DB (1983) The central role of the propensity score in observational studies for causal effects. Biometrika 70(1):41–55
Hauser CJ, Adams CA Jr, Eachempati SR (2006) Surgical Infection Society guideline: prophylactic antibiotic use in open fractures: an evidence-based guideline. Surg Infect (Larchmt) 7(4):379–405
Patzakis MJ, Harvey JP Jr, Ivler D (1974) The role of antibiotics in the management of open fractures. J Bone Jt Surg Am 56(3):532–541
Stennett CA, O'Hara NN, Sprague S, Petrisor B, Jeray KJ, Leekha S, Yimgang DP, Joshi M, O'Toole RV, Bhandari M et al (2020) Effect of extended prophylactic antibiotic duration in the treatment of open fracture wounds differs by level of contamination. J Orthop Trauma 34(3):113–120
Gustilo RB (1995) Interobserver agreement in the classification of open fractures of the tibia. The results of a survey of two hundred and forty-five orthopaedic surgeons. J Bone Jt Surg Am 77(8):1291–1292
Author information
Authors and Affiliations
Contributions
We confirm that all the authors contributed significantly to one or more aspects of the study: its design, data acquisition and analysis and interpretation of data. The manuscript has been read and approved by all named authors. We further confirm that the order of authors listed in the manuscript has been approved by all of us.
Corresponding author
Ethics declarations
Conflict of interest
Prof. WJ. Metsemakers is a consultant for DePuy Synthes. He received speaker fees from DePuy Synthes, BoneSupport and ZiomerBiomet. Prof. S. Nijs is a consultant for DePuy Synthes, Materialise and ZimmerBiomet. All the above are outside the submitted work. All the other authors declare that they have no conflict of interest.
Ethical approval
This is a retrospective case–control study involving human data. It is conducted at the University Hospitals Leuven, which is a designated level I trauma referral center in Belgium. The study time period was January 2003 to January 2017 and the protocol was approved by the hospital’s Ethics Committee (S58022, OG032).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Declercq, P., Zalavras, C., Nijssen, A. et al. Impact of duration of perioperative antibiotic prophylaxis on development of fracture-related infection in open fractures. Arch Orthop Trauma Surg 141, 235–243 (2021). https://doi.org/10.1007/s00402-020-03474-8
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-020-03474-8