Abstract
Introduction
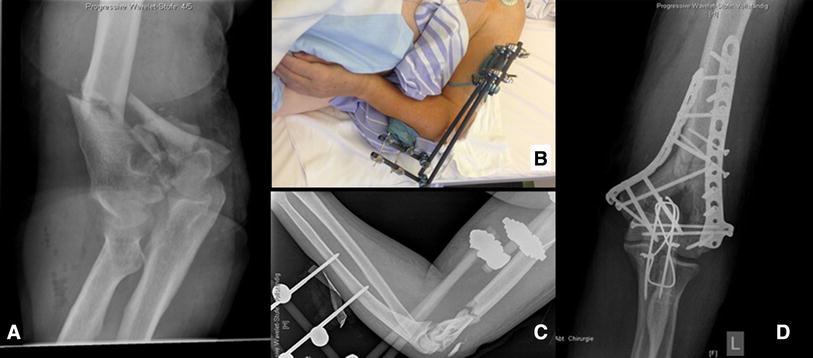
Fractures of the distal humerus are complex injuries that can be effectively treated with open reduction and internal fixation (ORIF). The new LCP distal humerus system allows angular stable fixation of these complex fractures with anatomically preshaped plates. The aim of the study was to evaluate operative reposition, fracture healing, and pain, function and patient satisfaction after open reduction with an angular stable fixation.
Methods
Fourteen patients with a mean age of 55.2 years (21–83) were treated with open reduction and angular stable internal fixation. Two patients were lost to follow up (1 died, one refused to be reevaluated). AO classification showed 12 C-fractures (1 × C 1.1; 1 × C 1.3; 4 × C 2.2; 4 × C 3.2; 2 × C 3.3) and 2 B-fracture (B 2.3 and B 3.3). 5 fractures were open fractures (4 × II°, 1 × I°). The clinical and radiographic follow up (Mayo elbow performance score (MEPS), Dash Score, elbow anterior–posterior and lateral view X-rays, and flexion and extension force as % of contralateral side at 90° flexion) were performed postoperatively. Mean follow up was 10 months.
Results
Radiographically, complete union was achieved in all patients. There were no cases of primary malposition or secondary dislocation. Complications were: (1) delayed union after olecranon osteotomy, (2) transient ulnar nerve irritation. Clinical MEPS results were good to excellent with a mean of 91 ± 11.7 points. The mean DASH Score was 18.5 ± 11.5 points. Mean flexion was 121 ± 20.9, mean extension deficit was 17.9° ± 10.3. Mean flexion force was 75.3% ± 26.7 and mean extension force was 70.7 % ± 24.9.
Conclusion
Treatment of supra-intercondylar fractures of the distal humerus is challenging. Anatomically preshaped angular stable implants facilitate operative reduction and stabilization of the fracture and may allow early postoperative rehabilitation. Clinical and radiological results are promising, with good range of motion and flexion and extension force.





Similar content being viewed by others
References
Brown RF, Morgan RG (1971) Intercondylar T-shaped fractures of the humerus. Results in ten cases treated by early mobilisation. J Bone Joint Surg Br 53:425–428
Horne G (1980) Supracondylar fractures of the humerus in adults. J Trauma 20:71–74
Imatani J, Ogura T, Morito Y, Hashizume H, Inoue H (2005) Custom AO small T plate for transcondylar fractures of the distal humerus in the elderly. J Shoulder Elbow Surg 14:611–615
John H, Rosso R, Neff U, Bodoky A, Regazzoni P, Harder F (1993) Distal humerus fractures in patients over 75 years of age. Long-term results of osteosynthesis. Helv Chir Acta 60:219–224
John H, Rosso R, Neff U, Bodoky A, Regazzoni P, Harder F (1994) Operative treatment of distal humeral fractures in the elderly. J Bone Joint Surg Br 76:793–796
Jupiter JB (1995) Complex fractures of the distal part of the humerus and associated complications. Instr Course Lect 44:187–198
Jupiter JB, Neff U, Holzach P, Allgower M (1985) Intercondylar fractures of the humerus. An operative approach. J Bone Joint Surg Am 67:226–239
Keon-Cohen BT (1966) Fractures at the elbow. J Bone Joint Surg Am 48:1623–1639
Korner J, Diederichs G, Arzdorf M, Lill H, Josten C, Schneider E, Linke B (2004) A biomechanical evaluation of methods of distal humerus fracture fixation using locking compression plates versus conventional reconstruction plates. J Orthop Trauma 18:286–293
Korner J, Lill H, Muller LP, Hessmann M, Kopf K, Goldhahn J, Gonschorek O, Josten C, Rommens PM (2005) Distal humerus fractures in elderly patients: results after open reduction and internal fixation. Osteoporos Int 16(Suppl 2):S73–S79
Korner J, Lill H, Muller LP, Rommens PM, Schneider E, Linke B (2003) The LCP-concept in the operative treatment of distal humerus fractures-biological, biomechanical and surgical aspects. Injury 34(Suppl 2):B20–B30
Letsch R, Schmit-Neuerburg KP, Sturmer KM, Walz M (1989) Intraarticular fractures of the distal humerus. Surgical treatment and results. Clin Orthop Relat Res:238–244
Miller WE (1964) Comminuted fractures of the distal end of the humerus in the adult. J Bone Joint Surg Am 46:644–657
Morrey BF (1993) Fractures and dislocations. In: Morrey BF (ed). The elbow and its disorders. 2nd ed. WB Sanndess, Philodelphia pp 293–329
O’Driscoll SW, Jupiter JB, Cohen MS, Ring D, McKee MD (2003) Difficult elbow fractures: pearls and pitfalls. Instr Course Lect 52:113–134
Pajarinen J, Björkenheim JM (2002) Operative treatment of type C intercondylar fractures of the distal humerus: results after a mean follow-up of 2 years in a series of 18 patients. J Shoulder Elbow Surg 11:48–52
Pereles TR, Koval KJ, Gallagher M, Rosen H (1997) Open reduction and internal fixation of the distal humerus: functional outcome in the elderly. J Trauma 43:578–584
Ring D, Gulotta L, Roy A, Jupiter JB (2003) Concomitant nonunion of the distal humerus and olecranon. J South Orthop Assoc 12:27–31
Ring D, Jupiter JB (1999) Complex fractures of the distal humerus and their complications. J Shoulder Elbow Surg 8:85–97
Ring D, Jupiter JB (2000) Fractures of the distal humerus. Orthop Clin North Am 31:103–113
Ring D, Jupiter JB, Gulotta L (2003) Articular fractures of the distal part of the humerus. J Bone Joint Surg Am 85:232–238
Riseborough EJ, Radin EL (1969) Intercondylar T fractures of the humerus in the adult. A comparison of operative and non-operative treatment in twenty-nine cases. J Bone Joint Surg Am 51:130–141
Sodergard J, Sandelin J, Bostman O (1992) Mechanical failures of internal fixation in T and Y fractures of the distal humerus. J Trauma 33:687–690
Sodergard J, Sandelin J, Bostman O (1992) Postoperative complications of distal humeral fractures. 27/96 adults followed up for 6 (2–10) years. Acta Orthop Scand 63:85–89
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Greiner, S., Haas, N.P. & Bail, H.J. Outcome after open reduction and angular stable internal fixation for supra-intercondylar fractures of the distal humerus: preliminary results with the LCP distal humerus system. Arch Orthop Trauma Surg 128, 723–729 (2008). https://doi.org/10.1007/s00402-007-0428-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-007-0428-2