Abstract
Background
It is unknown if ulcerative colitis (UC) duration has an impact on outcomes of ileal pouch anal anastomosis (IPAA). The aim of the study was to compare the long-term IPAA outcomes based on preoperative UC duration.
Methods
All patients with pathologically confirmed UC who underwent IPAA were included from a prospectively maintained pouch database (1983–2017).Patient’s cohort was stratified according to UC duration:< 5 years,5–10 years,10–20 years,> 20 years. UC duration was defined as time interval from date of preoperative diagnosis to colectomy date. The main outcome was Kaplan-Meier pouch survival. Secondary outcomes were pouch function and quality of life.
Results
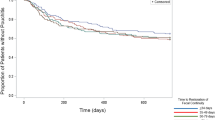
Out of 4502 IPAAs (1983–2016), 2797 patients were included. Treated with biologics versus 12% with UC duration > 20 years were 41% patients with UC duration < 5 years. Treated with steroids compared to shortest (34%,p < 0.001) were 54% patients with the longest disease. A total of 65% of patients with shortest disease had IPAAs performed mostly in 3 stages. Anastomotic separation and pelvic sepsis were more prevalent among shortest compared to longest disease groups. Rates of pouch-targeted fistulas, anastomotic strictures, and pouchitis were highest in longest disease group. Pouch survival was similar between groups. Multivariate analysis did not show a significant association between UC duration and pouch failure [1.05(0.97–1.1), p = 0.23].Longer UC duration was associated with increased odds of pouchitis [1.2(1.1, 1.3), p < 0.001]. Biologics agents were shown to be protective against pouchitis.
Conclusions
Preoperative UC duration does not increase pouch failure risk. Longer preoperative UC duration increases the pouchitis risk. Biologic agents and three-staged IPAA are protective against pouchitis and septic complications in long-term among patients with UC.


Similar content being viewed by others
References
Feagan BG, Reinisch W, Rutgeerts P, Sandborn WJ, Yan S, Eisenberg D, Bala M, Johanns J, Olson A, Hanauer SB (2007) The effects of infliximab therapy on health-related quality of life in ulcerative colitis patients. Am.J.Gastroenterol. 102(4):794–802
Choy MC, Seah D, Gorelik A, An YK, Chen CY, Macrae FA, Sparrow MP, Connell WR, Moore GT, Radford-Smith G, Van Langenberg DR, De Cruz P (2018) Predicting response after infliximab salvage in acute severe ulcerative colitis. J Gastroenterol Hepatol 33(7):1347–1352
Gibson DJ, Heetun ZS, Redmond CE, Nanda KS, Keegan D, Byrne K et al (2015) An accelerated infliximab induction regimen reduces the need for early colectomy in patients with acute severe ulcerative colitis. Clin Gastroenterol Hepatol 13(2):330–335.e1
Dayan B, Turner D (2012) Role of surgery in severe ulcerative colitis in the era of medical rescue therapy. World JGastroenterol 18(29):3833–3838
Saha SK, Panwar R, Kumar A, Pal S, Ahuja V, Dash NR, Makharia G, Sahni P (2018) Early colectomy in steroid-refractory acute severe ulcerative colitis improves operative outcome. Int J Color Dis 33(1):79–82
Randall J, Singh B, Warren BF, Travis SP, Mortensen NJ, George BD (2010) Delayed surgery for acute severe colitis is associated with increased risk of postoperative complications. Br J Surg 97(3):404–409
Fazio VW, Kiran RP, Remzi FH, Coffey JC, Heneghan HM, Kirat HT, Manilich E, Shen B, Martin ST (2013) Ileal pouch anal anastomosis: analysis of outcome and quality of life in 3707 patients. Ann Surg 257(4):679–685
Fazio VW, O'Riordain MG, Lavery IC, Church JM, Lau P, Strong SA et al (1999) Long-term functional outcome and quality of life after stapled restorative proctocolectomy. Ann.Surg. 230(4):575–584 discussion 584-6
Delaney CP, Fazio VW, Remzi FH, Hammel J, Church JM, Hull TL, Senagore AJ, Strong SA, Lavery IC (2003 Aug) Prospective, age-related analysis of surgical results, functional outcome, and quality of life after ileal pouch-anal anastomosis. Ann.Surg. 238(2):221–228
Kolehmainen S, Lepistö A, Färkkilä M (2019) Impact of anti-TNF-alpha therapy on colectomy rate and indications for colectomy in ulcerative colitis: comparison of two patient cohorts from 2005 to 2007 and from 2014 to 2016. Scand J Gastroenterol 28:1–5
Macaluso FS, Cavallaro F, Felice C, Mazza M, Armuzzi A, Gionchetti P, Vecchi M, Orlando A (2019) Risk factors and timing for colectomy in chronically active refractory ulcerative colitis: a systematic review. Dig Liver Dis 51(5):613–620
Gröne J, Lorenz EM, Seifarth C, Seeliger H, Kreis ME, Mueller MH (2018) Timing of surgery in ulcerative colitis in the biologic therapy era-the patient's perspective. Int J Color Dis 33(10):1429–1435
Remzi FH, Lavryk OA, Ashburn JH, Hull TL, Lavery IC, Dietz DW, Kessler H, Church JM (2017) Restorative proctocolectomy: an example of how surgery evolves in response to paradigm shifts in care. Color Dis 11:1003–1012
Gu J, Stocchi L, Remzi F, Kiran RP (2013) Factors associated with postoperative morbidity, reoperation and readmission rates after laparoscopic total abdominal colectomy for ulcerative colitis. Color Dis 15(9):1123–1129
Fasen GS, Pandian TK, Pavey ES, Dozois EJ, Boostrom SY (2015) Long-term outcome of IPAA in patients presenting with fulminant ulcerative colitis: a matched cohort study. World J Surg 39(10):2590–2594
Bewtra M, Kilambi V, Fairchild AO, Siegel CA, Lewis JD, Johnson FR (2014) Patient preferences for surgical versus medical therapy for ulcerative colitis. Inflamm Bowel Dis 20(1):103–114
Author information
Authors and Affiliations
Contributions
All authors participated in conception and design of the study, acquisition of data, analysis and interpretation of data, drafting and revising the manuscript, and approval of the published version.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lavryk, O.A., Stocchi, L., Hull, T.L. et al. Impact of preoperative duration of ulcerative colitis on long-term outcomes of restorative proctocolectomy. Int J Colorectal Dis 35, 41–49 (2020). https://doi.org/10.1007/s00384-019-03449-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-019-03449-1