Abstract
Aim
Obstetric anal sphincter injuries are a significant risk factor for faecal incontinence. Correct identification and successful primary repair are important. The aim of this study was to review the outcome of all patients, with an obstetric anal sphincter injury, referred to our unit.
Method
This is a retrospective review of 1495 patients over a 12-year period. All had a third or fourth degree tear and were referred at 4-months postpartum.
Results
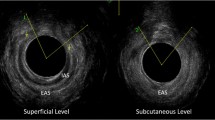
Endoanal ultrasonography demonstrated residual sphincter defect in 792 (53%) and normal sphincters, with no evidence of repair, in 661 (44%). The majority of injuries involved both the external and internal sphincters (n = 501). Significant reductions in resting pressure and voluntary squeeze pressures were seen when those with a sphincter defect were compared to those with intact sphincters. However, there was no significant difference in the mean (SD) Cleveland Clinic faecal incontinence scores (5.8 (5.8) and 4.3 (5.5), p = 0.8).
Conclusion
Third and fourth degree tears appear to be over diagnosed. Primary repair appears to be unsuccessful in the majority of cases. There appears to be poor correlation between objective and subjective assessment of sphincter function.

Similar content being viewed by others
References
Sultan AH (1999) Clinical focus: perineal injury and faecal incontinence after childbirth. Editorial: obstetric perineal injury and anal incontinence. Clinical Risk 5:193–196
Savoye-Collet C, Savoye G, Koning E, Sassi A, Leroi AM, Dacher JN (2003) Endosonography in the evaluation of anal function after primary repair of a third-degree obstetric tear. Scand J Gastroenterol 38(11):1149–1153
Soerensen MM, Buntzen S, Bek KM, Laurberg S (2013) Complete obstetric anal sphincter tear and risk of long-term fecal incontinence: a cohort study. Dis Colon rectum 56(8):992–1001
Fitzpatrick M, Behan M, O'Connell PR, O'Herlihy C (2000) A randomized clinical trial comparing primary overlap with approximation repair of third-degree obstetric tears. Am J Obstet Gynecol 183(5):1220–1224
Gynaecologists RCoOa (2015) Third and fourth degree perineal tears, management (green top guideline number 29). Third edition. Royal College of Obstetricians and Gynaecologists Publications
Starck M, Bohe M, Valentin L (2006) The extent of endosonographic anal sphincter defects after primary repair of obstetric sphincter tears increases over time and is related to anal incontinence. Ultrasound Obstet Gynecol 27(2):188–197
Sultan AH, Kamm MA, Hudson CN, Bartram CI (1994) Third degree obstetric anal sphincter tears: risk factors and outcome of primary repair. BMJ 308(6933):887–891
Rockwood TH, Church JM, Fleshman JW, Kane RL, Mavrantonis C, Thorson AG et al (1999) Patient and surgeon ranking of the severity of symptoms associated with fecal incontinence: the fecal incontinence severity index. Dis Colon rectum 42(12):1525–1532
Poen AC, Felt-Bersma RJ, Dekker GA, Deville W, Cuesta MA, Meuwissen SG (1997) Third degree obstetric perineal tears: risk factors and the preventive role of mediolateral episiotomy. Br J Obstet Gynaecol 104(5):563–566
Samuelsson E, Ladfors L, Wennerholm UB, Gareberg B, Nyberg K, Hagberg H (2000) Anal sphincter tears: prospective study of obstetric risk factors. BJOG 107(7):926–931
Matzel KE, Stadelmaier U, Hohenfellner M, Gall FP (1995) Electrical stimulation of sacral spinal nerves for treatment of faecal incontinence. Lancet 346(8983):1124–1127
Boyle DJ, Murphy J, Gooneratne ML, Grimmer K, Allison ME, Chan CL et al (2011) Efficacy of sacral nerve stimulation for the treatment of fecal incontinence. Dis Colon rectum 54(10):1271–1278
Glasgow SC, Lowry AC (2012) Long-term outcomes of anal sphincter repair for fecal incontinence: a systematic review. Dis Colon rectum 55(4):482–490
Andrews V, Sultan AH, Thakar R, Jones PW (2006) Occult anal sphincter injuries—myth or reality? BJOG 113(2):195–200
Scheer I, Thakar R, Sultan AH (2009) Mode of delivery after previous obstetric anal sphincter injuries (OASIS)—a reappraisal? Int Urogynecol J Pelvic Floor Dysfunct 20(9):1095–1101
Fernando RJ, Sultan AH, Kettle C, Thakar R (2013) Methods of repair for obstetric anal sphincter injury. Cochrane Database Syst Rev 12:CD002866
Sultan AH, Monga AK, Kumar D, Stanton SL (1999) Primary repair of obstetric anal sphincter rupture using the overlap technique. Br J Obstet Gynaecol 106(4):318–323
Soerensen MM, Bek KM, Buntzen S, Hojberg KE, Laurberg S (2008) Long-term outcome of delayed primary or early secondary reconstruction of the anal sphincter after obstetrical injury. Dis Colon rectum 51(3):312–317
Authors contributions
All authors contributed to the collection of data, analysis of data and construction of manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there are no conflicts of interest.
Funding
No funding was received for this research.
Additional information
What does this paper add to the literature?
This paper demonstrates the high failure rate of primary sphincter repair following obstetric injury and suggests an over diagnosis of this complication.
Rights and permissions
About this article
Cite this article
Thomas, G.P., Gould, L.E., Casunuran, F. et al. A retrospective review of 1495 patients with obstetric anal sphincter injuries referred for assessment of function and endoanal ultrasonography. Int J Colorectal Dis 32, 1321–1325 (2017). https://doi.org/10.1007/s00384-017-2851-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00384-017-2851-3



