Abstract
Background
Cardiovascular dysfunction (CVD) is a major cause of mortality and morbidity in hyperthyroidism. CVD and its reversibility after total thyroidectomy (TT) are not adequately addressed. This prospective case–control study evaluates the effect of hyperthyroidism on myocardium and its reversibility after TT.
Materials and methods
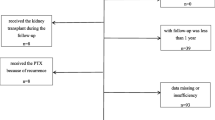
Surgical candidates of new onset hyperthyroidism, Group A (n = 41, age < 60 years) was evaluated with 2D Echocardiography, serum n-terminal probrain natriuretic peptide (NT-proBNP) at the time of diagnosis (Point A), after achieving euthyroidism (Point B) with antithyroid drugs, and 3 months after TT (Point C). 20 patients with nontoxic benign thyroid nodules undergoing TT served as controls (Group B).
Results
Both groups were age and sex matched. Group A (n = 41) comprises Graves disease (n = 22) and Toxic Multinodular goiter (n = 19). At point A, CVD was evident in 26/41(63.4 %), pulmonary hypertension (PHT) in 24/41(58.5 %)—mild in 17/41(41.4 %) and moderate in 7/41(17 %)—dilated cardiomyopathy (DCM) in 8/41(19.5 %), heart failure in 4/41(9.7 %), and NT-proBNP elevated in 28/41(68.3 %). At point B, recovery was observed in PHT 19/26(73.1 %), DCM 4/8(50 %), heart failure 4/4(100 %), NT-proBNP in 3/28(10.7 %). At Point C, further improvement occurred in PHT 23/24(95.8 %), DCM 7/8(87.5 %), heart failure 4/4(100 %), and NT-proBNP in 24/28(85.7 %).
Conclusion
Pulmonary hypertension is completely reversible at 3 months after TT and is the most common cardiac event in Hyperthyroidism. Various parameters of CVD improved consistently after surgical cure. NT-proBNP levels correlated well with the severity and duration of CVD and hence can be an objective tool in monitoring of hyperthyroid cardiac dysfunction.



Similar content being viewed by others
References
Brandt F, Green A, Hegedüs L et al (2011) A critical review and meta-analysis of the association between overt hyperthyroidism and mortality. Eur J Endocrinol 165:491–497
Cordova-Alvelais L, Verdejo-Paris J, Cárdenas-Loaeza M (1979) Cardiopatiatirotoxica. Archivos de Cardiología de México 49:1046–1054
Wang Y-Y, Jiao B, Guo W-G et al (2010) Excessive thyroxine enhances susceptibility to apoptosis and decreases contractility of cardiomyocytes. Mol Cell Endocrinol 320(1–2):67–75
Ghandour A, Reust C (2011) Hyperthyroidism: a stepwise approach to treatment. J Fam Pract 60:388–395
Palitzsch KD (2008) Prevention and multimodal therapy of hyperthyroidism. Internist (Berl) 49:1428–1436
Petersen P, Hansen JM (1988) Stroke in thyrotoxicosis with atrial fibrillation. Stroke 19:15–18
Anakwue RC, Onwubere BJ, Ikeh V et al (2015) Echocardiographic assessment of left ventricular function in thyrotoxicosis and implications for the therapeutics of thyrotoxic cardiac disease. Ther Clin Risk Manag 11:189–200. doi:10.2147/TCRM.S68752
Forfar JC, Matthews DM, Toft AD (1984) Delayed recovery of left ventricular function after antithyroid treatment. Further evidence for reversible abnormalities of contractility in hyperthyroidism. Br Heart J 52(2):215–222
Mercé J, Ferrás S, Oltra C (2005) Cardiovascular abnormalities in hyperthyroidism: a prospective Doppler echocardiographic study. Am J Med 118:126–131
Marvisi M, Zambrelli P, Brianti M et al (2006) Pulmonary hypertension is frequent in hyperthyroidism and normalizes after therapy. Eur J Intern Med 17(4):267–271
Siu CW, Zhang XH, Yung C et al (2007) Hemodynamic changes in hyperthyroidism-related pulmonary hypertension: a prospective echocardiographic study. J Clin Endocrinol Metab 92(5):1736–1742
Armigliato M, Paolini R, Aggio S et al (2006) Hyperthyroidism as a cause of pulmonary arterial hypertension: a prospective study. Angiology 57(5):600–606
Suk JH, Cho KI, Lee SH et al (2011) Prevalence of echocardiographic criteria for the diagnosis of pulmonary hypertension in patients with Graves’ disease: before and after antithyroid treatment. J Endocrinol Invest 34(8):e229–e234. doi:10.3275/7573 Epub 2011 Mar 7
Nakchbandi IA, Wirth JA, Inzucchi SE (1999) Pulmonary hypertension caused by Graves’ thyrotoxicosis: normal pulmonary hemodynamics restored by (131) I treatment. Chest 116:1483–1485
Frost L, Vestergaard P, Mosekilde L (2004) Hyperthyroidism and Risk of atrial fibrillation or flutter—a population-based study. Arch Intern Med 164:1675–1678
Vlase H, Lungu G, Vlase L (1991) Cardiac disturbances in thyrotoxicosis: diagnosis, incidence, clinical features and management. Endocrinologie 29(3–4):155–160
El Hattaoui M, Charei N, Mouniri M, et al. (2009) Cardiothyrotoxicosis in the young adult in Marrakech. A report of 36 cases. Ann Cardiol Angeiol (Paris) 58(3):135–138. doi:10.1016/j.ancard.2008.07.006
Roffi M, Cattaneo F, Topol EJ (2003) Thyrotoxicosis and the cardiovascular system: subtle but serious effects. Clevel Clin J Med 70(1):57–63
Oliveros-Ruiz L, Vallejo M, Canseco LFD et al. (2013) Determinants of thyrotoxic cardiomyopathy recovery. Biomed Res Int 2013. doi:10.1155/2013/452709
Umpierrez GE, Challapalli S, Patterson C (1995) Congestive heart failure due to reversible cardiomyopathy in patients with hyperthyroidism. Am J Med Sci 310:99–102
Li X, Yang X, Wang Y et al (2014) The prevalence and prognostic effects of subclinical thyroid dysfunction in dilated cardiomyopathy patients: a single-center cohort study. J Card Fail 20(7):506–512. doi:10.1016/j.cardfail.2014.05.002
Aziz F, Cheveli P (2012) Hyperthyroid-induced cardiomyopathy in an adult: a case report. Int J Cardiol 10(2):1
Ebisawa K, Ikeda U, Murata M et al (1994) Irreversible cardiomyopathy due to thyrotoxicosis. Cardiology 84:274–277
Abassi Z, Karram T, Ellaham S et al (2004) Implications of the natriuretic peptide system in the pathogenesis of heart failure: diagnostic and therapeutic importance. Pharmacol Ther 102(3):223–241
Kato Keiko, Murakami Hitomi, Isozaki Osamu et al (2009) Serum concentrations of BNP and ANP in patients with thyrotoxicosis. Endocr J 56(1):17–27
Acknowledgments
We would like to thank Dr. Ravi, MD, DM, HOD of department of cardiology, and Dr. Gomathi, MD cardiologist, RGGGH and MMC, Chennai, for their valuable guidance in assessing the various echographic parameters. We would like to acknowledge Dr. Srinivasa Raman, MD, Director, Anderson Diagnostic services, for his excellent lab supports.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Muthukumar, S., Sadacharan, D., Ravikumar, K. et al. A Prospective Study on Cardiovascular Dysfunction in Patients with Hyperthyroidism and Its Reversal After Surgical Cure. World J Surg 40, 622–628 (2016). https://doi.org/10.1007/s00268-015-3352-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3352-6