Abstract
Objective
To prospectively assess the cost of patients in an adult intensive care unit (ICU) using bottom-up costing methodology and evaluate the usefulness of “severity of illness” scores in estimating ICU cost.
Methods and design
A prospective study costing 64 consecutive admissions over a 2-month period in a mixed medical/surgical ICU.
Results
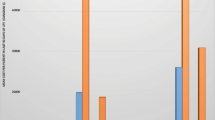
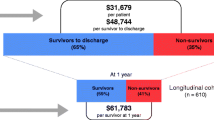
The median daily ICU cost (interquartile range, IQR) was €2,205 (€1,932–€3,073), and the median total ICU cost (IQR) was €10,916 (€4,294–€24,091). ICU survivors had a lower median daily ICU cost at €2,164 per day, compared with €3,496 per day for ICU non-survivors (P = 0.08). The requirements for continuous haemodiafiltration, blood products and anti-fungal agents were associated with higher daily and overall ICU costs (P = 0.002). Each point increase in SAPS3 was associated with a €305 (95% CI €31–€579) increase in total ICU cost (P = 0.029). However, SAPS3 accounted for a small proportion of the variance in this model (R 2 = 0.08), limiting its usefulness as a stand-alone predictor of cost in clinical practice. A model including haemodiafiltration, blood products and anti-fungal agents explained 54% of the variance in total ICU cost.
Conclusion
This bottom-up costing study highlighted the considerable individual variation in costs between ICU patients and identified the major factors contributing to cost. As the requirement for expensive interventions was the main driver for ICU cost, “severity of illness” scores may not be useful as stand-alone predictors of cost in the ICU.


Similar content being viewed by others
Abbreviations
- APACHE II:
-
Acute Physiology and Chronic Health Evaluation Score II
- CI:
-
Confidence interval
- CT:
-
Computed tomography scan
- CXR:
-
Chest X-ray
- FFP:
-
Fresh frozen plasma
- ICU:
-
Intensive care unit
- IQR:
-
Interquartile range
- MRI:
-
Magnetic resonance imaging
- NICE:
-
National Institute for Clinical Excellence
- NIV:
-
Non-invasive ventilation
- SAPS 3:
-
Simplified Acute Physiology Score 3
- SD:
-
Standard deviation
- SOFA:
-
Sequential Organ Failure Assessment Score
- U/S:
-
Ultrasound scan
References
Chalfin DB, Cohen IL, Lambrinos J (1995) The economics and cost–effectiveness of critical care medicine. Intensive Care Med 21:952–961
Bams JL, Miranda DR (1985) Outcome and costs of intensive care. A follow-up study on 238 ICU-patients. Intensive Care Med 11:234–241
Bekes C, Fleming S, Scott E (1988) Reimbursement for intensive care services under diagnosis-related groups. Crit Care Med 16:478–481
Chassin MR (1982) Costs and outcomes of medical intensive care. Med Care 20:165–179
Coulton CJ, McClish D, Doremus H, Powell S, Smookler S, Jackson DL (1985) Implications of DRG payments for medical intensive care. Med Care 23:977–985
Ridley S, Biggam M, Stone P (1991) Cost of intensive therapy. A description of methodology and initial results. Anaesthesia 46:523–530
Ridley S, Biggam M, Stone P (1993) A cost–benefit of intensive therapy. Anaesthesia 48:14–19
Singer M, Myers G, Hall G, Cohen SL, Armstrong RF (1994) The cost of intensive care. A comparison on one unit between 1988 and 1991. Intensive Care Med 20:542–549
Loes O, Smith-Erichsen N, Lind B (1987) Intensive care: cost and benefit. Acta Anaesthesiol Scand 31:3–19
Health Division of Statistics Canada (1982) Canadian workload measurement system-diagnostic radiology. A schedule of unit values for diagnostic radiology, 1982–1983. Workload Measurement, Institutional Statistics Section, Health Division, Statistics Canada, Ottawa, Canada
Sznajder M, Aegerter P, Launois R, Merliere Y, Guidet CubRea B (2001) A cost–effectiveness analysis of stays in intensive care units. Intensive Care Med 27:146–153
Chaix C, Durand-Zaleski I, Alberti C, Brun-Buisson C (1999) A model to compute the medical cost of patients in intensive care. Pharmacoeconomics 15:573–582
Heyland DK, Konopad E, Noseworthy TW, Johnston R, Gafni A (1998) Is it ‘worthwhile’ to continue treating patients with a prolonged stay (>14 days) in the ICU? An economic evaluation. Chest 114:192–198
Negrini D, Sheppard L, Mills GH, Jacobs P, Rapoport J, Bourne RS, Guidet B, Csomos A, Prien T, Anderson G, Edbrooke DL (2006) International Programme for Resource Use in Critical Care (IPOC)—a methodology and initial results of cost and provision in four European countries. Acta Anaesthesiol Scand 50:72–79
Golestanian E, Scruggs JE, Gangnon RE, Mak RP, Wood KE (2007) Effect of interhospital transfer on resource utilization and outcomes at a tertiary care referral center. Crit Care Med 35:1470–1476
Rawlins M, Culyer AJ (2004) National Institute for Clinical Excellence and its value judgments. BMJ 329:224–227
Devlin N, Parkin D (2004) Does NICE have a cost effectiveness threshold and what other factors influence its decisions? A binary choice analysis. Health Econ 13:437–452
Dakin H, Devlin N, Odeyemi I (2006) Yes, no or “yes, but”? A multinomial model of NICE decision-making. Health Policy 77:352–367
Appleby J, Devlin N, Parkin D (2007) NICE’s cost effectiveness threshold. BMJ 335:358–359
Mason J, Drummond M, Torrance G (1993) Some guidelines on the use of cost effectiveness league tables. BMJ 306:570–572
Acknowledgments
The authors would like to thank Dr. J. Boylan for his valuable advice in preparing this manuscript. The authors acknowledge financial support from Dr. Canavan from the UK Department of Health via the National Institute for Health Research (NIHR) comprehensive Biomedical Research Centre award to Guy’s and St Thomas’ NHS Foundation Trust in partnership with King’s College London and King’s College Hospital NHS Foundation Trust.
Conflict of interest statement
None
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
McLaughlin, A.M., Hardt, J., Canavan, J.B. et al. Determining the economic cost of ICU treatment: a prospective “micro-costing” study. Intensive Care Med 35, 2135–2140 (2009). https://doi.org/10.1007/s00134-009-1622-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-009-1622-1