Abstract
Two well-studied conditions of peripheral neuropathic pain are postherpetic neuralgia (PHN) and painful diabetic peripheral neuropathy (DPN). Several pregabalin trials for peripheral neuropathic pain have been conducted in the West, but limited data are available for Japan. As ethnicity may influence health risks, differences may be evident in safety data from pregabalin trials in Japan and in the West.
The objectives of this review were to compare large pooled safety data from randomized controlled trials evaluating pregabalin for the treatment of PHN or DPN in the West with data from two (one PHN, N = 371; one DPN, N = 314) similar trials in Japan. Longer-term safety data from Japanese open-label extension studies were also reviewed in these neuropathic pain populations. Published and unpublished Pfizer-supported pregabalin trials were identified and sourced from internal Pfizer records.
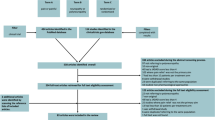
A PubMed search to check for inclusiveness was conducted on 2 November 2011 using the following criteria: ‘diabetic peripheral neuropathy’ OR ‘postherpetic neuralgia’ OR ‘neuropathic pain’ AND ‘pregabalin’, with limits set for clinical and randomized controlled trials published in English. Five PHN trials (N= 1250) and nine DPN trials (N = 2554) were identified as suitable for inclusion based on methodological comparability. Descriptive safety data from the original trials were reviewed and the most commonly reported adverse events (AEs; dizziness, somnolence, peripheral oedema and weight gain) were identified to be of primary interest. The majority of AEs were of mild to moderate severity in Japanese and Western populations. The most commonly reported AE data (all-causality) with pregabalin (regardless of dose) in Japan (dizziness: PHN = 31.1%; DPN = 24.6%, and somnolence: PHN = 28.6%; DPN = 25.7%) were compared with pooled data from the Western trials (dizziness: PHN = 24.9%; DPN = 23.0%, and somnolence: PHN=15.1%; DPN=13.4%). Further assessment of these pooled AE (all-causality) data showed that dizziness and somnolence appeared early in the course of pregabalin treatment, but resolved before the end of the treatment in the majority of PHN and DPN patients (maximum duration of trials was 13 weeks).
The slightly higher incidence of dizziness and somnolence in the two Japanese trials than that seen in the Western trials may reflect an increased exposure to pregabalin per fixed dose due to the lower mean bodyweight of the Japanese versus Western populations (on a mg/kg basis). However, of the participants who experienced these AEs (all-causality), the proportion who withdrew from the trials in Japan (dizziness: PHN = 23.5%; DPN = 18.2%, and somnolence: PHN = 10.3%; DPN = 10.9%) were comparable with the proportion who withdrew from trials in the West (dizziness: PHN= 16.0%; DPN = 29.3%, and somnolence: PHN = 19.4%; DPN = 34.2%). In Japan, 12.5% (PHN) and 15.1% (DPN) of patients experienced peripheral oedema as an AE (all-causality) compared with 8.8% (PHN) and 10.3% (DPN) in the West. Weight gain as an AE (all-causality) was experienced in 11.7% (PHN) and 13.4% (DPN) of patients in Japan compared with 3.8% (PHN) and 7.0% (DPN) in the West, but stabilized with continued treatment. Despite the lower mean bodyweight in Japanese versus Western patients, the PHN and DPN patients in Japan had stable blood glucose and HbA1c levels throughout the trials.
The results of this review indicate safety outcomes in pregabalin trials are comparable between patients in Japan and those in the West. While managing peripheral neuropathic pain with pregabalin treatment, all patients should be observed closely for the incidence of dizziness and somnolence, especially at the beginning of treatment. These patients should also be monitored for evidence of peripheral oedema and weight gain during stable treatment, regardless of the source of neuropathic pain.








Similar content being viewed by others
References
Ben-Menachem E. Pregabalin pharmacology and its relevance to clinical practice. Epilepsia 2004; 45 Suppl. 6: 13–8
European Medicines Agency. European Public Assessment Report (EPAR) for Lyrica [online]. Available from URL: http://www.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Summary_for_the_public/human/000546/WC500046603.pdf [Accessed 2011 Apr 27]
Pfizer Inc. Highlights of prescribing information [online]. Available from URL: http://www.pfizer.com/files/products/uspi_lyrica.pdf [Accessed 2011 Jan]
Bockbrader HN, Radulovic LL, Posvar EL, et al. Clinical pharmacokinetics of pregabalin in healthy volunteers. J Clin Pharmacol 2010 Aug; 50(8): 941–50
Brodie MJ, Wilson EA, Wesche DL, et al. Pregabalin drug interaction studies: lack of effect on the pharmacokinetics of carbamazepine, phenytoin, lamotrigine, and valproate in patients with partial epilepsy. Epilepsia 2005 Sep; 46(9): 1407–13
Ogawa S, Suzuki M, Arakawa A, et al. Long-term efficacy and safety of pregabalin in patients with postherpetic neuralgia: results of a 52-week, open-label, flexible-dose study. Masui 2010 Aug; 59(8): 961–70
Satoh J, Yagihashi S, Baba M, et al. Efficacy and safety of pregabalin for treating neuropathic pain associated with diabetic peripheral neuropathy: a 14 week, randomized, double-blind, placebo-controlled trial. Diabet Med 2011 Jan; 28(1): 109–16
News Blaze. Pfizer’s Lyrica® (Pregabalin) capsules CV receives approval for treatment of peripheral neuropathic pain in Japan [online]. Available from URL: http://newsblaze.com/story/2010102814380200001.pnw/topstory.html [Accessed 2011 May 17]
Opstelten W, Mauritz JW, de Wit NJ, et al. Herpes zoster and postherpetic neuralgia: incidence and risk indicators using a general practice research database. Fam Pract 2002 Oct; 19(5): 471–5
Gialloreti LE, Merito M, Pezzotti P, et al. Epidemiology and economic burden of herpes zoster and post-herpetic neuralgia in Italy: a retrospective, population-based study. BMC Infect Dis 2010 Aug 3; 10: 230
Sampathkumar P, Drage LA, Martin DP. Herpes zoster (shingles) and postherpetic neuralgia. Mayo Clin Proc 2009 Mar; 84(3): 274–80
Schmader KE. Epidemiology and impact on quality of life of postherpetic neuralgia and painful diabetic neuropathy. Clin J Pain 2002 Nov–Dec; 18(6): 350–4
Kazuo H, Kazunori H, Keiichi N. Bridging the gap between pain research and treatment — update review: postherpetic neuralgia: diagnosis and treatment. Pain Clinic 2004; 25(2): 158–65
Ziegler D. Treatment of diabetic neuropathy and neuropathic pain: how far have we come? Diabetes Care 2008 Feb; 31 Suppl. 2: S255–61
Kawano M, Omori Y, Katayama S, et al. A questionnaire for neurological symptoms in patients with diabetes: cross-sectional multicenter study in Saitama Prefecture, Japan. Diabetes Res Clin Pract 2001 Oct; 54(1): 41–7
Ogawa S, Suzuki M, Arakawa A, et al. Evaluation of the efficacy and safety of pregabalin in the treatment of post-herpetic neuralgia: a randomized, double-blind, multicenter, placebo-controlled study. J Japan Soc Pain Clin 2010; 17(2): 141–52
van Seventer R, Feister HA, Young Jr JP, et al. Efficacy and tolerability of twice-daily pregabalin for treating pain and related sleep interference in postherpetic neuralgia: a 13-week, randomized trial. Curr Med Res Opin 2006 Feb; 22(2): 375–84
Tolle T, Freynhagen R, Versavel M, et al. Pregabalin for relief of neuropathic pain associated with diabetic neuropathy: a randomized, double-blind study. Eur J Pain 2008 Feb; 12(2): 203–13
Zaccara G, Gangemi P, Perucca P, et al. The adverse event profile of pregabalin: a systematic review and meta-analysis of randomized controlled trials. Epilepsia 2011 Apr; 52(4): 826–36
Stommel M, Schoenborn CA. Variations in BMI and prevalence of health risks in diverse racial and ethnic populations. Obesity (Silver Spring) 2010 Sep; 18(9): 1821–6
World Health Organization. Appropriate body-mass index for Asian populations and its implications for policy and intervention strategies. Lancet 2004 Jan 10; 363(9403): 157–63
Freynhagen R, Strojek K, Griesing T, et al. Efficacy of pregabalin in neuropathic pain evaluated in a 12-week, randomised, double-blind, multicentre, placebo-controlled trial of flexible- and fixed-dose regimens. Pain 2005 Jun; 115(3): 254–63
Sabatowski R, Galvez R, Cherry DA, et al. Pregabalin reduces pain and improves sleep and mood disturbances in patients with post-herpetic neuralgia: results of a randomised, placebo-controlled clinical trial. Pain 2004 May; 109(1–2): 26–35
Dworkin RH, Corbin AE, Young Jr JP, et al. Pregabalin for the treatment of postherpetic neuralgia: a randomized, placebo-controlled trial. Neurology 2003 Apr 22; 60(8): 1274–83
Richter RW, Portenoy R, Sharma U, et al. Relief of painful diabetic peripheral neuropathy with pregabalin: a randomized, placebo-controlled trial. J Pain 2005 Apr; 6(4): 253–60
Lesser H, Sharma U, LaMoreaux L, et al. Pregabalin relieves symptoms of painful diabetic neuropathy: a randomized controlled trial. Neurology 2004 Dec 14; 63(11): 2104–10
Rosenstock J, Tuchman M, LaMoreaux L, et al. Pregabalin for the treatment of painful diabetic peripheral neuropathy: a double-blind, placebo-controlled trial. Pain 2004 Aug; 110(3): 628–38
Arezzo JC, Rosenstock J, Lamoreaux L, et al. Efficacy and safety of pregabalin 600 mg/d for treating painful diabetic peripheral neuropathy: a double-blind placebo-controlled trial. BMC Neurol 2008 Sep 16; 8: 33
Semel D, Murphy TK, Zlateva G, et al. Evaluation of the safety and efficacy of pregabalin in older patients with neuropathic pain: results from a pooled analysis of 11 clinical studies. BMC Fam Pract 2010; 11: 85
Sharma U, Griesing T, Emir B, et al. Time to onset of neuropathic pain reduction: a retrospective analysis of data from nine controlled trials of pregabalin for painful diabetic peripheral neuropathy and postherpetic neuralgia. Am J Ther 2010 Nov–Dec; 17(6): 577–85
Freeman R, Durso-Decruz E, Emir B. Efficacy, safety, and tolerability of pregabalin treatment for painful diabetic peripheral neuropathy: findings from seven randomized, controlled trials across a range of doses. Diabetes Care 2008 Jul; 31(7): 1448–54
Pfizer Inc. Protocol A0081071: a randomized double-blind, placebo-controlled, parallel-group, multi-center trial of pregabalin versus placebo in the treatment of neuropathic pain associated with diabetic peripheral neuropathy [online]. Available from URL: http://www.clinicalstudyresults.org/documents/company-study_3972_0.pdf [Accessed 2011 May 17]
Pfizer Inc. Protocol A0081030: a 14 week, double-blind, randomized, placebo-controlled, multi-center study to evaluate the safety and efficacy of pregabalin (150 mg–600 mg day) using a flexible, optimized dose schedule in patients with painful diabetic peripheral neuropathy (DPN) [online]. Available from URL: http://www.clinicalstudyresults.org/documents/company-study_2504_0.pdf [Accessed 2011 May 17]
Seino Y, Nanjo K, Tajima N, et al. Report of the Committee on the Classification and Diagnostic Criteria of Diabetes Mellitus. J Diabet Invest 2010; 1(5): 212–28
Satoh J, Yagihashi S, Baba M, et al. Efficacy and safety evaluation of pregabalin treatment over 52 weeks in patients with diabetic neuropathic pain extended after a phase III double-blind placebo-controlled trial. J Diabet Invest 2011; 2(6): 457–63
Acknowledgements
The studies included within this pooled analysis were all sponsored and funded by Pfizer Inc. All authors contributed to the writing, reviewing, preparation and interpretation of the data, and approval of the manuscript. They were also involved in the decision to submit the paper for publication. Setsuro Ogawa has received consultancy fees or lecture fees from Janssen, Hisamitsu, Pfizer, Nippon Shinyaku and Showa Yakuhin Kakou. Jo Satoh has received research funding, lecture fees and consultancy fees from Astellas, Banyu, Daiichi-Sankyo, Dainippon-Sumitomo, Eli Lilly, Novo Nordisk, Ono, Pfizer, Sanofi-Aventis and Takeda. Akio Arakawa, Tamotsu Yoshiyama and Makoto Suzuki are employees of Pfizer. Medical writing support was provided by Brenda Meyer, PhD, of UBC Scientific Solutions and funded by Pfizer Inc.
The Medical Dictionary for Regulatory Activities (MedDRA®) trademark is owned by the International Federation of Pharmaceutical Manufacturers and Associations (IFPMA) on behalf of the International Conference on Harmonisation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ogawa, S., Satoh, J., Arakawa, A. et al. Pregabalin Treatment for Peripheral Neuropathic Pain. Drug Saf 35, 793–806 (2012). https://doi.org/10.1007/BF03261976
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF03261976