Abstract
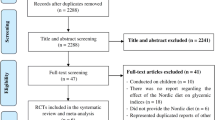
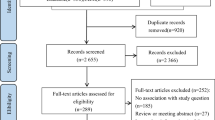
The purpose of this study was to study the effect of lifestyle intervention on the blood glucose control of women with gestational diabetes mellitus (GDM). A meta-analysis was conducted by including randomized controlled trials that compare any form of lifestyle intervention with the usual care. A search of PubMed, MEDLINE, Elsevier Science Direct, Springer, and Web of Science for studies published from 2000 to 2016 was undertaken to identify relevant studies. Methodological quality of the studies was assessed according to the Jadad scale. Random-effort models were used to analyze the weighted mean difference and its 95% confidence interval (CI). From 776 studies, 7 randomized controlled trials (RCTs) (3685 women) were selected for meta-analysis based on our inclusion and exclusion criteria. The evidence suggests that lifestyle, dietary, and activity intervention for women with GDM lowers the fasting plasma glucose (FPG) and 2-h postprandial glucose (2hPG). The reduction in FPG was observed to be statistically significant in the meta-analysis (4 RCTs; n = 1086; −0.16 [95% CI, −0.31 to −0.01]). The reduction in 2hPG was also observed to be statistically significant in the meta-analysis (3 RCTs; n = 849; −0.32 [95% CI, −0.61 to −0.03]). However, no effects of lifestyle interventions were identified in women with GDM in relation to body mass index and hemoglobin A1c. This meta-analysis provides further evidence that lifestyle intervention is associated with reducing FPG and 2hPG in women with GDM.



Similar content being viewed by others
References
Fauci AS, Braunwald E, Kaspe DL, Hauser SL, Longo DL, Larry Jameson J, et al. Harrison’s principles of internal medicine, 17th edition. Libr J. 2008;133(11):96.
Kim C, Newton KM, Knopp RH. Gestational diabetes and the incidence of type 2 diabetes - a systematic review. Diabetes Care. 2002;25(10):1862–8. doi:10.2337/diacare.25.10.1862.
Buchanan TA, Xiang AH, Page KA. Gestational diabetes mellitus: risks and management during and after pregnancy. Nat Rev Endocrinol. 2012;8(11):639–49. doi:10.1038/nrendo.2012.96.
Diagnosis and Classification of Diabetes Mellitus. Diabetes Care. 2012;36(Supplement_1):S67-S74. doi:10.2337/dc13-S067
Poolsup N, Suksomboon N, Amin M. Effect of treatment of gestational diabetes mellitus: a systematic review and meta-analysis. PLoS One. 2014;9(3):e92485. doi:10.1371/journal.pone.0092485.
Group HSCR, Metzger BE, Lowe LP, Dyer AR, Trimble ER, Chaovarindr U, et al. Hyperglycemia and adverse pregnancy outcomes. N Engl J Med. 2008;358(19):1991–2002. doi:10.1056/NEJMoa0707943.
Landon MB, Gabbe SG. Gestational diabetes mellitus. Obstet Gynecol. 2011;118(6):1379–93. doi:10.1097/AOG.0b013e31823974e2.
Jovanovic L, Pettitt DJ. Gestational diabetes mellitus. JAMA. 2001;286(20):2516–8.
Knowler WC, Barrett-Connor E, Fowler SE, Hamman RF, Lachin JM, Walker EA, et al. Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. New Engl J Med. 2002;346(6):393–403.
Tuomilehto J, Lindstrom J, Eriksson JG, Valle TT, Hamalainen H, Ilanne-Parikka P, et al. Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. New Engl J Med. 2001;344(18):1343–50. doi:10.1056/Nejm200105033441801.
Pan XR, Li GW, Hu YH, Wang JX, Yang WY, An ZX, et al. Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance. The Da Qing IGT and diabetes study. Diabetes Care. 1997;20(4):537–44.
Chiasson JL, Josse RG, Gomis R, Hanefeld M, Karasik A, Laakso M, et al. Acarbose for prevention of type 2 diabetes mellitus: the STOP-NIDDM randomised trial. Lancet. 2002;359(9323):2072–7. doi:10.1016/S0140-6736(02)08905-5.
Coustan DR. Can a dietary supplement prevent gestational diabetes mellitus? Diabetes Care. 2013;36(4):777–9. doi:10.2337/dc12-2505.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gotzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate health care interventions: explanation and elaboration. Ann Intern Med. 2009;151(4):W65–94.
Alejandro R, Jadad M, Andrew Moore R, RCJ DC, Reynolds DDJG DJM, HJM DM. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17:1–12.
Thalheimer W CS. How to calculate effect sizes from published research: a simplified methodology. 2002
Higgins JTS, Deeks JJ, Altman DG. Measuring inconsistency in meta-analyses. BMJ. 2003;327:557.
Higgins JTS, Deeks JJ, Altman DG. Quantifying heterogeneity in a metaanalysis. Stat Med. 2002;21:1539.
Egger MSG, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629.
Elnour AA, El Mugammar IT, Jaber T, Revel T, McElnay JC. Pharmaceutical care of patients with gestational diabetes mellitus. J Eval Clin Pract. 2008;14(1):131–40.
Hu G, Tian HG, Zhang FX, Liu HK, Zhang CP, Zhang S, et al. 3Tianjin gestational diabetes mellitus prevention program study design, methods, and 1-year interim report on the feasibility of lifestyle intervention program. Diabetes Res Clin Pr. 2012;98(3):508–17. doi:10.1016/j.diabres.2012.09.015.
Yang XL, Tian HG, Zhang FX, Zhang CP, Li Y, Leng JH, et al. A randomised translational trial of lifestyle intervention using a 3-tier shared care approach on pregnancy outcomes in Chinese women with gestational diabetes mellitus but without diabetes. J Transl Med. 2014;12 doi:10.1186/S12967-014-0290-2.
Perez-Ferre N, Del Valle L, Torrejon MJ, Barca I, Calvo MI, Matia P, et al. 5 diabetes mellitus and abnormal glucose tolerance development after gestational diabetes: a three-year, prospective, randomized, clinical-based, Mediterranean lifestyle interventional study with parallel groups. Clin Nutr. 2015;34(4):579–85. doi:10.1016/j.clnu.2014.09.005.
Youngwanichsetha S, Phumdoung S, Ingkathawornwong T. 7 the effects of mindfulness eating and yoga exercise on blood sugar levels of pregnant women with gestational diabetes mellitus. Applied nursing research : ANR. 2014;27(4):227–30. doi:10.1016/j.apnr.2014.02.002.
Landon MB, Spong CY, Thom E, Carpenter MW, Ramin SM, Casey B, et al. 8 a multicenter, randomized trial of treatment for mild gestational diabetes. N Engl J Med. 2009;361(14):1339–48. doi:10.1056/NEJMoa0902430.
Cao X, Wang Z, Yang C, Mo X, Xiu L, Li Y, et al. 10 comprehensive intensive therapy for Chinese gestational diabetes benefits both newborns and mothers. Diabetes Technol Ther. 2012;14(11):1002–7. doi:10.1089/dia.2012.0142.
Agarwal MM, Dhatt GS, Punnose J, Koster G. Gestational diabetes: dilemma caused by multiple international diagnostic criteria. Diabetic medicine : a journal of the British Diabetic Association. 2005;22(12):1731–6. doi:10.1111/j.1464-5491.2005.01706.x.
Streuling I, Beyerlein A, von Kries R. Can gestational weight gain be modified by increasing physical activity and diet counseling? A meta-analysis of interventional trials. Am J Clin Nutr. 2010;92(4):678–87. doi:10.3945/ajcn.2010.29363.
Olson CM. A call for intervention in pregnancy to prevent maternal and child obesity. Am J Prev Med. 2007;33(5):435–6. doi:10.1016/j.amepre.2007.07.028.
Olson CM. Achieving a healthy weight gain during pregnancy. Annu Rev Nutr. 2008;28:411–23. doi:10.1146/annurev.nutr.28.061807.155322.
Birdsall KM, Vyas S, Khazaezadeh N, Oteng-Ntim E. Maternal obesity: a review of interventions. Int J Clin Pract. 2009;63(3):494–507. doi:10.1111/j.1742-1241.2008.01910.x.
Gardner B, Wardle J, Poston L, Croker H. Changing diet and physical activity to reduce gestational weight gain: a meta-analysis. Obes Rev. 2011;12(7):E602–E20. doi:10.1111/j.1467-789X.2011.00884.x.
Whitelaw B, Gayle C. Gestational diabetes. Obstetrics, Gynaecology & Reproductive Medicine. 2011;21(2):41–6. doi:10.1016/j.ogrm.2010.11.001.
JF C. Effects of diet and exercise on insulin resistance during pregnancy. Metab Syndr Relat Disord. 2006;4:84–90.
Oken E, Taveras EM, Popoola FA, Rich-Edwards JW, MW G. Television, walking, and diet: associations with postpartum weight retention. Am J Prev Med. 2007;32:305–11.
Fraser RBFF, Lawrence GF. Insulin sensitivity in third trimester pregnancy. A randomized study of dietary effects. Br J Obstet Gynaecol. 1988;95(3):223–9.
Qiu C, Williams MA, Vadachkoria S, Frederick IO, DA L. Increased maternal plasma leptin in early pregnancy and risk of gestational diabetes mellitus. Obstet Gynecol. 2004;103(3):519–25.
Yu LC. Kang, Zhang Yanwu, Ma Liangkun, Li Rongrong, fang W. Effects of medical nutritional intervention on clinical outcome of gestational diabetes mellitus: a metaanalysis. Chinese Journal of Clinical Nutrition. 2015;23(6):341–50.
Rasekaba TM, Furler J, Blackberry I, Tacey M, Gray K, Lim K. Telemedicine interventions for gestational diabetes mellitus: a systematic review and meta-analysis. Diabetes Res Clin Pract. 2015;110(1):1–9. doi:10.1016/j.diabres.2015.07.007.
Carolan-Olah MC. Educational and intervention programmes for gestational diabetes mellitus (GDM) management: an integrative review. Collegian. 2016;23(1):103–14. doi:10.1016/j.colegn.2015.01.001.
Russo LM, Nobles C, Ertel KA, Chasan-Taber L, Whitcomb BW. Physical activity interventions in pregnancy and risk of gestational diabetes mellitus: a systematic review and meta-analysis. Obstet Gynecol. 2015;125(3):576–82. doi:10.1097/AOG.0000000000000691.
Chasan-Taber L. Lifestyle interventions to reduce risk of diabetes among women with prior gestational diabetes mellitus. Best practice & research Clinical obstetrics & gynaecology. 2015;29(1):110–22. doi:10.1016/j.bpobgyn.2014.04.019.
Falavigna M, Schmidt MI, Trujillo J, Alves LF, Wendland ER, Torloni MR, et al. Effectiveness of gestational diabetes treatment: a systematic review with quality of evidence assessment. Diabetes Res Clin Pr. 2012;98(3):396–405. doi:10.1016/j.diabres.2012.09.002.
Hartling L, Dryden DM, Guthrie A, Muise M, Vandermeer B, Donovan L. Benefits and harms of treating gestational diabetes mellitus: a systematic review and meta-analysis for the U.S. preventive services task force and the National Institutes of Health Office of medical applications of research. Ann Intern Med. 2013;159(2):123–9. doi:10.7326/0003-4819-159-2-201307160-00661.
Rogozinska E, Chamillard M, Hitman GA, Khan KS, Thangaratinam S. meta Nutritional manipulation for the primary prevention of gestational diabetes mellitus: a meta-analysis of randomised studies. PLoS One. 2015;10(2):e0115526. doi:10.1371/journal.pone.0115526.
Acknowledgements
My deepest gratitude goes first and foremost to Professor Xia Wang, my supervisor, for her constant encouragement and guidance. She has walked me through all the stages of the writing of this paper. Without her consistent and illuminating instruction, this thesis could not have reached its present form. I also owe my sincere gratitude to my friends Baihui Zhang who gave me their help and time in listening to me and helping me work out my problems during the difficult course of the thesis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
(1) Statement of human rights
Ethical approval: All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
(2) Statement on the welfare of animals
This article does not contain any studies with animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Electronic supplementary material
ESM 1
(DOC 43 kb).
Rights and permissions
About this article
Cite this article
Guo, W., Zhang, B. & Wang, X. Lifestyle interventions for gestational diabetes mellitus to control blood glucose: a meta-analysis of randomized studies. Int J Diabetes Dev Ctries 38, 26–35 (2018). https://doi.org/10.1007/s13410-017-0553-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-017-0553-6