Abstract
Background
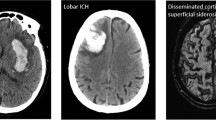
Intracerebral hemorrhage (ICH) is an infrequent complication of intravenous recombinant tissue plasminogen activator (rt-PA) for the treatment of acute stroke. However, such ICH is an important reason for withdrawal of care because of lack of adequate data regarding long-term patient outcomes.
Objective
To report the long-term outcomes in patients with post-thrombolytic ICH.
Methods
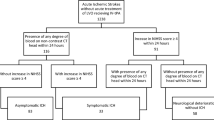
We analyzed patient data from a randomized, placebo-controlled trial in patients with ischemic stroke presenting within 3 h of symptom onset. Baseline clinical characteristics and outcomes defined by modified Rankin scale (mRS) were ascertained at 3, 6, and 12 months after treatment in patients who suffered from post-thrombolytic ICH. Favorable outcome was defined by mRS of 0–3 and unfavorable outcome by mRS of 4–6 at 1 year.
Results
A total of 48 patients suffered post-thrombolytic ICH in the trial. Fourteen patients had favorable outcomes and 34 patients had unfavorable outcomes. Clinical characteristics did not have an impact on patient outcomes at 12 months. Patients with unfavorable outcomes were more likely to have an National Institutes of Health Stroke Scale (NIHSS) score ≥20 at 7–10 days after treatment (64 vs. 7 %, p < 0.0009). Patients with unfavorable outcomes were more likely to have a worsening of NIHSS score of >4 points at 7–10 days from their baseline NIHSS (44 vs. 0 %, p = 0.0006).
Conclusion
Approximately 30 % of patients with post-thrombolytic ICH have favorable outcomes at 1 year which does not support early withdrawal of care. Ascertainment of NIHSS score and worsening of NIHSS score at 7–10 days may be necessary for accurate prognostic stratification.

Similar content being viewed by others
References
Adams H, Adams R, Del Zoppo G, et al. Guidelines for the early management of patients with ischemic stroke: 2005 guidelines update a scientific statement from the Stroke Council of the American Heart Association/American Stroke Association. Stroke. 2005;36(4):916–23.
Albers GW, Amarenco P, Easton JD, et al. Antithrombotic and thrombolytic therapy for ischemic stroke. The seventh ACCP conference on antithrombotic and thrombolytic therapy. Chest. 2004;126(3 Suppl):483S–512S.
The National Institute of Neurological Disorders, Stroke rt-PA Stroke Study Group. Tissue plasminogen activator for acute ischemic stroke. N Engl J Med. 1995;333(24):1581–7.
Qureshi AI, Chaudhry SA, Rodriguez GJ, et al. Outcome of the ‘drip-and-ship’ paradigm among patients with acute ischemic stroke: results of a statewide study. Cerebrovasc Dis Extra. 2012;2(1):1–8.
Wardlaw JM, Murray V, Berge E, et al. Thrombolysis for acute ischaemic stroke. Cochrane Database Syst Rev. 2009;(4):CD000213.
Clark WM, Wissman S, Albers GW, et al. Recombinant tissue-type plasminogen activator (Alteplase) for ischemic stroke 3 to 5 hours after symptom onset. The ATLANTIS Study: a randomized controlled trial. Alteplase thrombolysis for acute noninterventional therapy in ischemic stroke. JAMA. 1999;282(21):2019–26.
Hacke W, Kaste M, Fieschi C, et al. Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Second European-Australasian Acute Stroke Study Investigators. Lancet. 1998;352(9136):1245–51.
Hacke W, Donnan G, Fieschi C, et al. Association of outcome with early stroke treatment: pooled analysis of ATLANTIS, ECASS, and NINDS rt-PA stroke trials. Lancet. 2004;363(9411):768–74.
Lansberg MG, Albers GW, Wijman CA. Symptomatic intracerebral hemorrhage following thrombolytic therapy for acute ischemic stroke: a review of the risk factors. Cerebrovasc Dis. 2007;24(1):1–10.
Libman R, Kwiakowski T, Lyden P, et al. Asymptomatic hemorrhagic transformation of cerebral infarction does not worsen long-term outcome. J Stroke Cerebrovasc Dis. 2005;14(2):50–4.
Zahuranec DB, Brown DL, Lisabeth LD, et al. Early care limitations independently predict mortality after intracerebral hemorrhage. Neurology. 2007;68(20):1651–7.
Saver JL. Hemorrhage after thrombolytic therapy for stroke: the clinically relevant number needed to harm. Stroke. 2007;38(8):2279–83.
Kwiatkowski TG, Libman RB, Frankel M, et al. Effects of tissue plasminogen activator for acute ischemic stroke at one year. National Institute of Neurological Disorders and Stroke Recombinant Tissue Plasminogen Activator Stroke Study Group. N Engl J Med. 1999;340(23):1781–7.
Patel SC, Levine SR, Tilley BC, et al. Lack of clinical significance of early ischemic changes on computed tomography in acute stroke. JAMA. 2001;286(22):2830–8.
Qureshi AI, Chaudhry SA, Sapkota BL, et al. Discharge destination as a surrogate for modified rankin scale defined outcomes at 3- and 12-months poststroke among stroke survivors. Arch Phys Med Rehabil. 2012;93(8):1408–13.
Barber PA, Demchuk AM, Zhang J, et al. Validity and reliability of a quantitative computed tomography score in predicting outcome of hyperacute stroke before thrombolytic therapy. ASPECTS Study Group. Alberta stroke programme early CT score. Lancet. 2000;355(9216):1670–4.
The NINDS t-PA Stroke Study Group. Intracerebral hemorrhage after intravenous t-PA therapy for ischemic stroke. Stroke. 1997;28(11):2109–18.
Barch C, Spilker J, Bratina P, et al. Nursing management of acute complications following rt-PA in acute ischemic stroke. The NINDS rt-PA Stroke Study Group. J Neurosci Nurs. 1997;29(6):367–72.
Sulter G, Steen C, De Keyser J. Use of the Barthel index and modified Rankin scale in acute stroke trials. Stroke. 1999;30(8):1538–41.
Mahoney FI, Barthel DW. Functional evaluation: the Barthel index. Md State Med J. 1965;14:61–5.
Dhamoon MS, Moon YP, Paik MC, et al. Long-term functional recovery after first ischemic stroke: the Northern Manhattan Study. Stroke. 2009;40(8):2805–11.
Donnan G, Davis S. ASK trial: predictors of good outcome. Cerebrovasc Dis. 1996;6:183.
Morris AD, Ritchie C, Grosset DG, et al. A pilot study of streptokinase for acute cerebral infarction. QJM. 1995;88(10):727–31.
del Zoppo GJ, von Kummer R, Hamann GF. Ischaemic damage of brain microvessels: inherent risks for thrombolytic treatment in stroke. J Neurol Neurosurg Psychiatry. 1998;65(1):1–9.
Del Zoppo GJ, Zeumer H, Harker LA. Thrombolytic therapy in stroke: possibilities and hazards. Stroke. 1986;17(4):595–607.
Rosenberg GA, Estrada EY, Dencoff JE. Matrix metalloproteinases and TIMPs are associated with blood-brain barrier opening after reperfusion in rat brain. Stroke. 1998;29(10):2189–95.
Montaner J, Alvarez-Sabín J, Molina C, et al. Matrix metalloproteinase expression after human cardioembolic stroke: temporal profile and relation to neurological impairment. Stroke. 2001;32(8):1759–66.
Heo JH, Lucero J, Abumiya T, et al. Matrix metalloproteinases increase very early during experimental focal cerebral ischemia. J Cereb Blood Flow Metab. 1999;19(6):624–33.
Molina CA, Montaner J, Abilleira S, et al. Time course of tissue plasminogen activator-induced recanalization in acute cardioembolic stroke: a case–control study. Stroke. 2001;32(12):2821–7.
Fisher M, Adams RD. Observations on brain embolism with special reference to the mechanism of hemorrhagic infarction. J Neuropathol Exp Neurol. 1951;10(1):92–4.
Ogata J, Yutani C, Imakita M, et al. Hemorrhagic infarct of the brain without a reopening of the occluded arteries in cardioembolic stroke. Stroke. 1989;20(7):876–83.
Tanne D, Kasner SE, Demchuk AM, et al. Markers of increased risk of intracerebral hemorrhage after intravenous recombinant tissue plasminogen activator therapy for acute ischemic stroke in clinical practice: the Multicenter rt-PA Stroke Survey. Circulation. 2002;105(14):1679–85.
Larrue V, von Kummer RR, Müller A, et al. Risk factors for severe hemorrhagic transformation in ischemic stroke patients treated with recombinant tissue plasminogen activator: a secondary analysis of the European-Australasian Acute Stroke Study (ECASS II). Stroke. 2001;32(2):438–41.
Hill MD, Buchan AM, Investigators CAfSESC. Thrombolysis for acute ischemic stroke: results of the Canadian Alteplase for stroke effectiveness study. CMAJ. 2005;172(10):1307–12.
Kase CS, Furlan AJ, Wechsler LR, et al. Cerebral hemorrhage after intra-arterial thrombolysis for ischemic stroke: the PROACT II trial. Neurology. 2001;57(9):1603–10.
Dubey N, Bakshi R, Wasay M, et al. Early computed tomography hypodensity predicts hemorrhage after intravenous tissue plasminogen activator in acute ischemic stroke. J Neuroimaging. 2001;11(2):184–8.
Gilligan AK, Markus R, Read S, et al. Baseline blood pressure but not early computed tomography changes predicts major hemorrhage after streptokinase in acute ischemic stroke. Stroke. 2002;33(9):2236–42.
Ribo M, Montaner J, Molina CA, et al. Admission fibrinolytic profile is associated with symptomatic hemorrhagic transformation in stroke patients treated with tissue plasminogen activator. Stroke. 2004;35(9):2123–7.
Selim M, Fink JN, Kumar S, et al. Predictors of hemorrhagic transformation after intravenous recombinant tissue plasminogen activator: prognostic value of the initial apparent diffusion coefficient and diffusion-weighted lesion volume. Stroke. 2002;33(8):2047–52.
Fiorelli M, Bastianello S, von Kummer R, et al. Hemorrhagic transformation within 36 hours of a cerebral infarct: relationships with early clinical deterioration and 3-month outcome in the European Cooperative Acute Stroke Study I (ECASS I) cohort. Stroke. 1999;30(11):2280–4.
Berger C, Fiorelli M, Steiner T, et al. Hemorrhagic transformation of ischemic brain tissue: asymptomatic or symptomatic? Stroke. 2001;32(6):1330–5.
Molina CA, Alvarez-Sabín J, Montaner J, et al. Thrombolysis-related hemorrhagic infarction: a marker of early reperfusion, reduced infarct size, and improved outcome in patients with proximal middle cerebral artery occlusion. Stroke. 2002;33(6):1551–6.
Gebel JM, Sila CA, Sloan MA, et al. Thrombolysis-related intracranial hemorrhage: a radiographic analysis of 244 cases from the GUSTO-1 trial with clinical correlation. Global utilization of streptokinase and tissue plasminogen activator for occluded coronary arteries. Stroke. 1998;29(3):563–9.
Brown DL, Barsan WG, Lisabeth LD, et al. Survey of emergency physicians about recombinant tissue plasminogen activator for acute ischemic stroke. Ann Emerg Med. 2005;46(1):56–60.
Appelros P, Nydevik I, Viitanen M. Poor outcome after first-ever stroke: predictors for death, dependency, and recurrent stroke within the first year. Stroke. 2003;34(1):122–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Norby, K.E., Siddiq, F., Adil, M.M. et al. Long-Term Outcomes of Post-Thrombolytic Intracerebral Hemorrhage in Ischemic Stroke Patients. Neurocrit Care 18, 170–177 (2013). https://doi.org/10.1007/s12028-012-9803-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12028-012-9803-0