Abstract
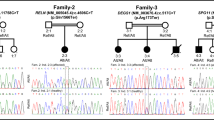
Mutations in the SLC26A4 gene at the DFNB4 locus are responsible for Pendred syndrome and non-syndromic hereditary hearing loss (DFNB4). This study included 80 nuclear families with two or more siblings segregating presumed autosomal recessive hearing loss. All deaf persons tested negative for mutations in GJB2 at the DFNB1 locus and were, therefore, screened for autozygosity by descent (ABD) using short tandem repeat polymorphisms (STRPs) that flanked SLC26A4. In 12 families, homozygosity for STRPs suggested possible ABD in this genomic region. Affected individuals in five families had a positive perchlorate discharge test. Sequence analysis of SLC26A4 identified ten mutations in eight families (T420I, 1197delT, G334V, R409H, T721M, R79X, S448L, L597S, 965insA and L445W), of which, four are novel (T420I, G334V, 965insA and R79X). These results imply that Pendred syndrome is the most prevalent form of syndromic hereditary hearing loss in Iran.
Similar content being viewed by others
Abbreviations
- HHL:
-
Hereditary hearing loss
- DFNB4:
-
Autosomal recessive non-syndromic hearing loss locus 4
- STRP:
-
Short tandem repeat polymorphisms
- SLC26A4:
-
Solute carrier family 26, member 4
- ABD:
-
Autozygosity by descent
- PDS:
-
Pendred syndrome
- GJB2:
-
Gap junction protein
- EVA:
-
Enlarged vestibular aqueduct
References
Campbell C, Cucci RA, Prasad S et al (2001) Pendred syndrome, DFNB4, and PDS/SLC26A4 identification of eight novel mutations and possible genotype–phenotype correlations. Hum Mutat 17:403–411
Coyle B, Reardon W, Herbrick JA et al (1998) Molecular analysis of the PDS gene in Pendred syndrome. Hum Mol Genet 7(7):1105–1112
Fugazzola L, Mannavola D, Cerutti N et al (2000) Molecular analysis of the Pendred’s syndrome gene and magnetic resonance imaging studies of the inner ear are essential for the diagnosis of true Pendred’s syndrome. J Clin Endocrinol Metab 85(7):2469–2475
Green GE, Scott DA, McDonald JM et al (1999) Carrier rates in the midwestern United States for GJB2 mutations causing inherited deafness. JAMA 281(23):2211–2216
Li XC, Everett LA, Lalwani AK et al (1998) A mutation in PDS causes non-syndromic recessive deafness. Nat Genet 18:215–217
Park HJ, Shaukat S, Liu XZ et al (2003) Origins and frequencies of SLC26A4 (PDS) mutations in east and south Asians: global implications for the epidemiology of deafness. J Med Genet 40(4):242–248
Reardon W (1992) Genetic deafness. J Med Genet 29:521–526
Reardon W, Coffey R, Chowdhury T et al (1999) Prevalence, age of onset, and natural history of thyroid disease in Pendred syndrome. J Med Genet 36(8):595–598
Scott DA, Wang R, Kreman TM et al (1999) The Pendred syndrome gene encodes a chloride–iodide transport protein. Nat Genet 21:440–443
The Pendred/BOR Homepage, Molecular Otolaryngology Research Laboratory, University of Iowa Hospitals and Clinics, Department of Otolaryngology—Head and Neck Surgery, 200 Hawkins Drive, Iowa City, IA 52246. Home page at: http://www.healthcare.uiowa.edu/labs/pendredandbor
Yang T, Vidarsson H, Rodrigo-Blomqvist S et al (2007) Transcriptional control of SLC26A4 Is involved in Pendred syndrome and nonsyndromic enlargement of vestibular aqueduct (DFNB4). Am J Hum Genet 80:1055–1063
Acknowledgements
We would like to thank our patients and their families for their cooperation in this research. This study was supported in part by grant no. 801 from the Genetic Research Center (University of Social Welfare and Rehabilitation Sciences), grant no. 35301 from the Research Institute for Endocrine Science (Beheshti University) and the NIDCD (RJHS, R01-DC02842).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kahrizi, K., Mohseni, M., Nishimura, C. et al. Identification of SLC26A4 gene mutations in Iranian families with hereditary hearing impairment. Eur J Pediatr 168, 651–653 (2009). https://doi.org/10.1007/s00431-008-0809-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-008-0809-8