Abstract
Introduction and hypothesis
The objective of this study was to evaluate the effect of vaginal packing following pelvic floor surgery with regard to post-operative pain, bleeding and infection. This was a double-blind randomised study of women undergoing vaginal hysterectomy and/or pelvic floor repair at a tertiary urogynaecology unit.
Methods
The primary outcome of day 1 post-operative pain was assessed using the short-form McGill Pain score. Secondary outcomes were haematological and infective morbidity, evaluated using changes in full blood count, and cultures of midstream urine and high vaginal swabs. A transvaginal ultrasound scan to exclude pelvic haematoma was performed at 6 weeks in all women who underwent vaginal hysterectomy with or without a pelvic floor repair.
Results
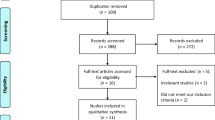
In total, 190 women were recruited: mean age 58.3 years (27–91 years), mean body mass index 27.4 kg/m2 and median parity 3. Women were randomised into the ‘pack’ (n = 86) and ‘no pack’ (n = 87) arms with no demographic differences between the groups. No statistically significant differences in the post-operative pain scores or secondary outcome measures were demonstrated. Incidence of haematoma formation (14.8 % no pack, 7.3 % pack, p = 0.204) was not statistically significant. There were three clinically significant complications in the no pack group and none in the pack group.
Conclusions
This is the first study to examine pain in association with post-operative vaginal packing. There is no evidence to suggest that packing increases pain scores or post-operative morbidity. A trend towards increased haematoma and significant complications was seen in the no pack group. As vaginal packing does no harm and may be of some benefit it may be argued that packing should be recommended as routine clinical practice.


Similar content being viewed by others
References
Kelleher CJ, Cardozo LD, Khullar V, Salvatore S (1997) A new questionnaire to assess the quality of life of urinary incontinent women. Br J Obstet Gynaecol 104:1374–1379
Kapoor DS, Thakar R, Sultan AH, Oliver R (2009) Conservative versus surgical management of prolapse: what dictates patient choice? Int Urogynecol J Pelvic Floor Dysfunct 20(10):1157–1161
Olsen AL, Smith VJ, Bergstrom JO, Colling JC, Clark AL (1997) Epidemiology of surgically managed pelvic organ prolapse and urinary incontinence. Obstet Gynecol 89(4):501–506
Sutton C (1997) Hysterectomy: a historical perspective. Baillieres Clin Obstet Gynaecol 11(1):1–22
Senn N (1895) The early history of vaginal hysterectomy. JAMA XXV(12):476–482
Kalogirou D, Antoniou G, Karakitsos P, Zioris C, Salampasis C (1996) Comparison of abdominal and vaginal hysterectomy. Study of complications. Clin Exp Obstet Gynecol 23(3):161–167
Conturso R, Radaelli L, Turtulici P, Alegente G, De Lalla F (1989) Prophylactic mezlocillin in vaginal hysterectomy: a prospective, randomized study. J Chemother 1(4 Suppl):1033–1034
Engel K, Schmidt W, Sonntag HG, Kees F (1989) Comparative clinical and pharmacokinetic aspects of cefotetan versus cefoxitin plus metronidazole in vaginal hysterectomy. J Chemother 1(4 Suppl):1053–1056
Bolling DR Jr, Plunkett GD (1973) Prophylactic antibiotics for vaginal hysterectomies. Obstet Gynecol 41(5):689–692
Kauer FM, Wijma J, Manson WL (1990) Vaginal hysterectomy: cefuroxime, metronidazole or both? Pharm Weekbl Sci 12(6A):284–288
Harris WJ (1995) Early complications of abdominal and vaginal hysterectomy. Obstet Gynecol Surv 50:795–805
Schneider J, Benito R (1988) Extensive gynecologic surgical procedures upon patients more than 75 years of age. Surg Gynecol Obstet 167:497–500
Kjølhede P, Halili S, Löfgren M (2011) Vaginal cleansing and postoperative infectious morbidity in vaginal hysterectomy. A register study from the Swedish National Register for Gynecological Surgery. Acta Obstet Gynecol Scand 90(1):63–71
Batista CS, Osako T, Clemente EM, Batista FC, Osako MT (2012) Observational evaluation of preoperative, intraoperative, and postoperative characteristics in 117 Brazilian women without uterine prolapse undergoing vaginal hysterectomy. Int J Womens Health 4:505–510
Dane C, Dane B, Cetin A, Yayla M (2009) Sonographically diagnosed vault hematomas following vaginal hysterectomy and its correlation with postoperative morbidity. Infect Dis Obstet Gynecol 2009:91708
Thomson AJ, Farquharson RG (2000) Vault haematoma and febrile morbidity after vaginal hysterectomy. Hosp Med 61(8):535–538
Moustafa M, Elgonaid WE, Massouh H, Beynon WG (2008) Evaluation of closure versus non-closure of vaginal vault after vaginal hysterectomy. J Obstet Gynaecol 28(8):791–794
Wood C, Maher P, Hill D (1997) Bleeding associated with vaginal hysterectomy. Aust N Z J Obstet Gynaecol 37(4):457–461
Daly LE, Bourke GJ (2000) Interpretation and uses of medical statistics, 3rd edn. Wiley, New York
Melzack R (1987) The short-form McGill Pain Questionnaire. Pain 30(2):191–197
Strand LI, Ljunggren AE, Bogen B, Ask T, Johnsen TB (2008) The Short-Form McGill Pain Questionnaire as an outcome measure: test-retest reliability and responsiveness to change. Eur J Pain 12(7):917–925
Tincello DG (1998) Ultrasound detection of vault haematoma following vaginal hysterectomy. Br J Obstet Gynaecol 105(12):1336–1337
Dubin MR, Pletcher SD (2009) Postoperative packing after septoplasty: is it necessary? Otolaryngol Clin North Am 42(2):279–285
Bajaj Y, Kanatas AN, Carr S, Sethi N, Kelly G (2009) Is nasal packing really required after septoplasty? Int J Clin Pract 63(5):757–759
Guyuron B (1989) Is packing after septorhinoplasty necessary? A randomized study. Plast Reconstr Surg 84(1):41–44, discussion 45–6
Bugten V, Nordgård S, Skogvoll E, Steinsvåg S (2006) Effects of nonabsorbable packing in middle meatus after sinus surgery. Laryngoscope 116(1):83–88
Glavind K, Mørup L, Madsen H, Glavind J (2007) A prospective, randomised, controlled trial comparing 3 hour and 24 hour postoperative removal of bladder catheter and vaginal pack following vaginal prolapse surgery. Acta Obstet Gynecol Scand 86(9):1122–1125
Acknowledgments
Mr. John Bidmead, Dr. Marcus Naef, Ms. Salma Ayis, Dr. Maria Grazia Matarazzo.
Funding
None.
Conflicts of interest
G. Thiagamoorthy: Has received funding from Astellas to attend conferences. Has received an IUGA FRN grant to set up a multicentre research project. A. Khalil: None. L. Cardozo: During the last year received funding for research, lecturing and/or advice/consultancies from Allergan, Astellas, Ethicon, Merck, Pfizer & Teva. S. Srikrishna: None. D. Robinson: During the last year received funding for research, lecturing and/or advice/consultancies from Allergan, Astellas, Ferring & Pfizer.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thiagamoorthy, G., Khalil, A., Cardozo, L. et al. The value of vaginal packing in pelvic floor surgery: a randomised double-blind study. Int Urogynecol J 25, 585–591 (2014). https://doi.org/10.1007/s00192-013-2264-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-013-2264-y