Abstract
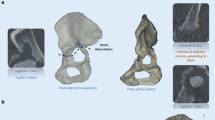
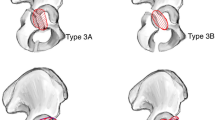
Acetabular bone defects determine the type of acetabular revision surgery. In order to avoid complications, preoperative planning must include patient evaluation, detailed imaging assessment of the bone defects, defect classification, and the proposed surgical reconstruction. Diagnosis of osteolysis and aseptic loosening is made based on serial radiographs, but potential difficulties in the presurgical evaluation require imaging techniques such as the use of Computed Tomography (CT) and Magnetic Resonance Imaging (MRI) to supplement information for radiographic assessment. Because of the complexity of acetabular revision surgery, the bone defects must be classified preoperatively in order to prepare the appropriate surgical technique. The definitive bone defects are evaluated intraoperatively after removal of the failed cup. A good bone defect classification system must be based on imaging findings, it must be validated by documented low rates of interobserver and intraobserver error prior before being accepted into routine usage, and it must be a guide to the surgeon that will facilitate choosing the right surgical technique.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Harris WH. Wear and periprosthetic osteolysis: the problem. Clin Orthop Relat Res. 2001;393:66–70.
Schmalzried TP, Guttman D, Grecula M, Amstutz HC. The relationship between the design, physician, and articular wear of acetabular components inserted without cement and the development of pelvic osteolysis. J Bone Joint Surg Am. 1994;76-A(5):677–88.
Schmalzried TP, Kwong OM, Jasty M, Sedlacek RC, Haire TC, O’Connor DO, Bragdon CR, Kabo JM, Malcolm AJ, Harris WH. The machanism of loosening and cemented acetabular components and total hip arthroplasty: analysis of specimens retrieved at autopsy. Clin Orthop Relat Res. 1991;274:60–78.
Schmalzried TP, Jasty M, Harris WH. Periprosthetic bone loss in total hip arthroplasty. Polyethylene wear debris and the concept of the effective joint space. J Bone Joint Surg Am. 1992;74-A(6):849–63.
Ries MD, Link TM. Monitoring and risk of progression of osteolysis after total hip arthroplasty. In: Pagnano MW, Hart RA, editors. AAOS instructional course lectures. 2013;62:207–14.
Stamenkov R, Howie D, Taylor J, Findlay D, McGee M, Kourlis G, Carbone A, Burwell M. Measurement of bone defects adjacent to acetabular components of hip replacement. Clin Orthop Relat Res. 2003;412:117–24.
Kitamura N, Naudie DD, Leung SB, Hooper RH Jr, Engh CA Sr. Diagnostic features of pelvic osteolysis associated with stable acetabulat component inserted without cement as part of a total hip replacement. J Bone Joint Surg Am. 2005;87-A(7):1542–50.
Maloney WJ, Paposky W, Engh CA, Rubash H. Surgical treatment of pelvic osteolysis. Clin Orthop Relat Res. 2001;393:78–84.
Kobayashi A, Freeman MAR, Bonfield W, Kadoya Y, Yamac T. Number of polyethylene particles and osteolysis in total joints replacements. A quantitative study using a tissue-digestion method. J Bone Joint Surg Br. 1997;79-B(5):844–8.
Maloney WJ, Smith RL. Periprosthetic osteolysis in total hip arthroplasty. The role of particulate wear debris. J Bone Joint Surg Am. 1995;77-A(9):1448–61.
Spangehl MJ, Masri BA, O’Connell JX, Duncan CP. Prospective analysis of preoperative and intraoperative investigation for the diagnosis of infection at the sites of two hundred and two revisión total hip arthroplasties. J Bone Joint Surg Am. 1999;81-A(5):672–83.
Alexander DP, Frew N. Preoperative optimisation of anaemia for primary total hip arthroplasty: a systemic review. Hip Int. 2017;27(6):515–22.
Gombotz H, Rehak PH, Shander A, Hofmann A. Blood use in elective surgery: the Austrian benchmark study. Transfusion. 2007;47(8):1468–80.
Dunne JR, Malone D, Tracy JK, Gannon C, Napolitano LM. Perioperative anemia: an independent risk factor for infection, mortality, and resource utilization in surgery. J Surg Res. 2002;102(2):237–44.
Bedair H, Yang J, Dwyer MK, McCarthy JC. Preoperative erytropoietin alpha reduces postoperative transfusions in THA and TKA by my not be cost-effective. Clin Orthop Relat Res. 2015;473(2):590–6.
Welton KL, Jesse MK, Kraeutler MJ, Garabekyan T, Mei-Dan O. The anteroposterior pelvic radiograph. Acetabular and femoral measurements and relation to hip pathologies. J Bone Joint Surg Am. 2018;100-A:76–85.
Masri BA, Masterson EL, Duncan CP. The classification and radiographic evaluation of bone loss in revision hip arthroplasty. Orthop Clin North Am. 1998;28(2):219–27.
Judet R, Judet J, Letournel E. Fractures of the acetabulum: classification and surgical approaches for open reduction, preliminary report. J Bone Joint Surg Am. 1964;46-A:1615–46.
Claus AM, Engh CA Jr, Sychterz CJ, Xenos JS, Orishimo KF, Engh CA Sr. Radiographic definition of pelvic osteolysis following total hip arthroplasty. J Bone Joint Surg Am. 2003;85-A(8):1519–26.
Shon WY, Gupta S, Biswal S, Han SH, Hong SJ, Moon JG. Pelvic osteolysis relationship to radiographs and polyethylene wear. J Arthroplasty. 2009;24(5):743–50.
Puri L, Wixson RL, Stern SH, Kohli J, Hendrix RW, Stulberg SD. Use of helical computed tomography for the assessment of acetabular osteolysis after total hip arthroplasty. J Bone Joint Surg Am. 2002;84-A(4):609–14.
Southwell DG, Bechtold JE, Lew WD, Schmidt AH. Improving the detection of acetabular osteolysis using oblique radiographs. J Bone Joint Surg Br. 1999;81-B(2):289–95.
Zimlich RH, Fehring TK. Underestimation of pelvic osteolysis: the value of the iliac oblique radiograph. J Arthroplasty. 2000;15(6):796–801.
Robertson DD, Magid D, Poss R, Fishman EK, Brooker AF, Sledge CB. Enhanced computed tomographic techniques for the evaluation of total hip arthroplasty. J Arthroplasty. 1989;4(3):271–6.
Claus AM, Totterman SM, Sychterz CJ, Tamez-Peña JG, Looney RJ, Engh CA Sr. Computed tomography to assess pelvic lysis after total hip replacement. Clin Orthop Relat Res. 2004;422:167–74.
Walde TA, Weiland DE, Leung SB, Kitamura N, Sychterz CJ, Engh CA Jr, Claus AM, Potter HG, Engh CA Sr. Comparison of CT, MRI, and radiographs in assessing pelvic osteolysis. A cadaveric study. Clin Orthop Relat Res. 2005;437:138–44.
Garcia-Cimbrelo E, Tapia M, Martin-Hervas C. Multislice computed tomography for evaluating acetabular defects in revision THA. Clin Orthop Relat Res. 2007;463(Oct):138–43.
Leung S, Naudie D, Kitamura N, Walde T, Engh CA. Computed tomography in the assessment of periacetabular osteolysis. J Bone Joint Surg Am. 2005;87(3):592–7.
Lee MJ, Kim S, Lee SA, Song HT, Huh YM, Kim DH, Han SH, Suh JS. Overcoming artifacts from metallic orthopedic implants at high-field-strength MR imaging and multi-detector CT. Radiographics. 2007;27(3):791–803.
Chen CA, Chen W, Goodman SB, Hargreaves BA, Koch KM, Lu W, Brau AC, Draper CE, Delp SL, Gold GE. New MR imaging methods for metallic implants in the knee: artifacts corection and clinical impact. J Magn Reson Imaging. 2011;33(5):1121–7.
Hayter CL, Koff MF, Shah KKM, Miller TT, Potter HG. MRI after arthroplasty: comparison of MAVRiC and conventional fast spin-echo techniques. AJR Am J Roentgenol. 2011;197(3):W405–11.
Hayter CL, Koff MF, Porter HG. Magnetic resonance imaging of the postoperative hip. J Magn Reson Imaging. 2012;35(5):1013–25.
Potter HG, Nestor BJ, Sofka CM, Ho ST, Peters SL, Salvati EA. Magnetic resonance imaging after total hip arthroplasty: evaluation of periprosthetic soft tissue. J Bone Joint Surg Am. 2004;86-A(9):1947–54.
Cooper HJ, Ranawat AS, HGF P, Foo LF, Jawetz ST, Ranawat CS. Magnetic resonance imaging in diagnosis and management of hip pain after total hip arthroplasty. J Arthroplasty. 2009;24(5):661–7.
Hayter CL, Potter HG, Su EP. Imaging of metal-on-metal resurfacing. Orthop Clin North Am. 2011;42(2):195–205.
Williams DH, Greidanus NV, Masri BA, Duncan CP, Garbuz DS. Prevalence of pseudotumor in asymptomatic patients after metal-on-metal hip arthroplasty. J Bone Joint Surg Am. 2011;93-A(23):2164–71.
Eftekhar NS, Nercessian O. Intrapelvic migration of total hip prostheses: operative treatment. J Bone Joint Surg. 1989;71-A(10):1480–6.
Frandsen PA, Andersen E, Madsen F, Skjodt T. Garden’s classification of femoral neck fractures: an assessment of inter-observer variation. J Bone Joint Surg Br. 1988;70-B(4):588–90.
D’Antonio JA, Capello WN, Borden LS, Bargar WL, Bierbaum BF, Boettcher WG, Steinberg ME, Stulberg SH, Wedge JH. Classification and management of acetabular abnormalities in total hip arthroplasty. Clin Orthop Relat Res. 1989;243:126–37.
Paprosky WG, Perona PG, Lawrence JM. Acetabular defect classification and surgical reconstruction in revision arthroplasty: a 6-year follow-up evaluation. J Arthroplasty. 1994;9(1):33–44.
Gross AE, Duncan CP, Garbuz D, Mohamed EMZ. Revision arthroplasty of the acetabulum in association with loss of bone stock. J Bone Joint Surg Am. 1998;80-A(3):440–51.
Berry DJ, Lewallen DG, Hanssen AD, Cabanela ME. Pelvic discontinuity in revision total hip arthroplasty. J Bone Joint Surg Am. 1999;81-A(12):1692–702.
Saleh KJ, Holtzman J, Gafni A, Saleh L, Jaroszynski G, Wong P, Woodgate I, Davis A, Gross AE. Development, test reliability and validation of a classification for revision hip arthroplasty. J Orthop Res. 2001;19(1):50–6.
Paprosky WG, Weeden SH, Howling JW Jr. Component removal in revision total hip arthroplasty. Clin Orthop Relat Res. 2001;393:181–93.
Peters CL, Erickson JA, Dunn HK. Revision of well-fixed cementless acetabular components for polyethylene failure. Clin Orthop Relat Res. 2003;414:129–35.
Mitchell PA, Masri BA, Garbuz DS, , Greidanus NV, Wilson D, Duncan CP. Removal of well-fixed, ccementless, acetabular components in revisión hip arthroplasty. J Bone Joint Surg Br 2000;85-B(7):949–952.
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Cite this chapter
García-Rey, E. (2019). Bone Defects in Acetabular Revision Surgery. Imaging and Classifications. In: García-Rey, E., García-Cimbrelo, E. (eds) Acetabular Revision Surgery in Major Bone Defects. Springer, Cham. https://doi.org/10.1007/978-3-319-98596-1_2
Download citation
DOI: https://doi.org/10.1007/978-3-319-98596-1_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-98595-4
Online ISBN: 978-3-319-98596-1
eBook Packages: MedicineMedicine (R0)