Abstract
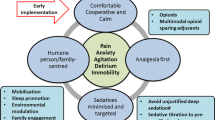
Adequate and appropriate analgesia and sedation is a crucial component in the care of critically ill patients. Implementation of a protocol for the assessment for adequate provision of sedation and analgesia is of paramount importance in the management of the critically ill patient. Both pharmacological and not pharmacological interventions play a role and influence outcomes. The assessment and prevention of delirium also influences outcomes and should be also routinely assessed and treated.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Society of Critical Care Medicine. Post-intensive care syndrome. 2013 [Internet] available from: http://www.myicucare.org/Adult-Support/Pages/Post-intensive-Care-Syndrome.aspx. Accessed 25 Mar 2014.
Samuelson KA, Lundberg D, Fridlund B. Stressful memories and psychological distress in adult mechanically ventilated intensive care patients—a 2-month follow-up study. Acta Anaesthesiol Scand. 2007;51:671–8.
Jones C, Bäckman C, Capuzzo M, Flaatten H, Rylander C, Griffiths RD. Precipitants of posttraumatic stress disorder following intensive care: a hypothesis generating study of diversity in care. Intensive Care Med. 2007;33:978–85.
Jones C, Griffiths RD, Humphris G, Skirrow PM. Memory, delusions, and the development of acute posttraumatic stress disorder-related symptoms after intensive care. Crit Care Med. 2001;29:573–80.
Wade DM, Howell DC, Weinman JA, Hardy RJ, Mythen MG, Brewin CR, et al. Investigating risk factors for psychological morbidity three months after intensive care: a prospective cohort study. Crit Care. 2012;16:R192.
Khitab A, Reid J, Bennett V, Adams GC, Balbuena L. Late onset and persistence of post-traumatic stress disorder symptoms in survivors of critical care. Can Respir J. 2013;20:429–33.
Sukantarat K, Greer S, Brett S, Williamson R. Physical and psychological sequelae of critical illness. Br J Health Psychol. 2007;12(Pt 1):65–74.
Lat I, McMillian W, Azocar R, In H, Agarwal S, Burke P, et al. The incidence of delirium is associated with longer ICU stay and fewer ventilator free days in surgical ICU patients. Crit Care Med. 2006;34:S483.
Ely EW, Shintani A, Truman B, Speroff T, Gordon SM, Harrell Jr FE, et al. Delirium as a predictor of mortality in mechanically ventilated patients in the intensive care unit. JAMA. 2004;291:1753–62.
Engel HJ, Needham DM, Morris PE, Gropper MA. ICU early mobilization: from recommendation to implementation at three medical centers. Crit Care Med. 2013;41(9 Suppl 1):S69–80.
Puthucheary Z, Rawal J, Ratnayake G, Harridge S, Montgomery H, Hart N. Neuromuscular blockade and skeletal muscle weakness in critically ill patients time to rethink the evidence? Am J Respir Crit Care Med. 2012;185:911–7.
Lipshutz AK, Gropper MA. Acquired neuromuscular weakness and early mobilization in the intensive care unit. Anesthesiology. 2013;118:202–15.
Balas MC, Vasilevskis EE, Olsen KM, Schmid KK, Shostrom V, Cohen MZ, et al. Effectiveness and safety of the awakening and breathing coordination, delirium monitoring/management, and early exercise/mobility bundle. Crit Care Med. 2014;42:1024–36.
Dale CR, Kannas DA, Fan VS, Daniel SL, Deem S, Yanez 3rd ND, et al. Improved analgesia, sedation and delirium protocol associated with decreased duration of delirium and mechanical ventilation. Ann Am Thorac Soc. 2014;11:367–74.
Reade MC, Finfer S. Sedation and delirium in the intensive care unit. N Engl J Med. 2014;370:444–54.
Barr J, Fraser GL, Puntillo K, Ely EW, Gélinas C, Dasta JF, et al. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. Crit Care Med. 2013;41:263–306.
Chanques G, Sebbane M, Barbotte E, Viel E, Eledjam JJ, Jaber S. A prospective study of pain at rest: incidence and characteristics of an unrecognized symptom in surgical and trauma versus medical intensive care unit patients. Anesthesiology. 2007;107:858–60.
Turner JS, Briggs SJ, Springhorn HE, Potgieter PD. Patients’ recollection of intensive care unit experiences. Crit Care Med. 1990;18:966–8.
Puntillo KA, White C, Morris AB, Perdue ST, Stanik-Hutt J, Thompson CL, et al. Patients’ perceptions and responses to procedural pain: results from Thunder Project II. Am J Crit Care. 2001;10:238–51.
Puntillo KA. Pain experiences of intensive care unit patients. Heart Lung. 1990;19:526–33.
Schelling G, Stoll C, Haller M, Briegel J, Manert W, Hummel T, et al. Health-related quality of life and posttraumatic stress disorder in survivors of the acute respiratory distress syndrome. Crit Care Med. 1998;26:651–9.
Ahlers SJ, van der Veen AM, van Dijk M, Tibboel D, Knibbe CA. The use of the Behavioral Pain Scale to assess pain in conscious sedated patients. Anesth Analg. 2010;110:127–33.
Gélinas C, Johnston C. Pain assessment in the critically ill ventilated adult: validation of the Critical-Care Pain Observation Tool and physiologic indicators. Clin J Pain. 2007;23:497–505.
Payen JF, Bosson JL, Chanques G, Mantz J, Labarere J, DOLOREA Investigators. Pain assessment is associated with decreased duration of mechanical ventilation in the intensive care unit: a post hoc analysis of the DOLOREA study. Anesthesiology. 2009;111:1308–16.
Chanques G, Viel E, Constantin JM, Jung B, de Lattre S, Carr J, et al. The measurement of pain in intensive care unit: comparison of 5 self-report intensity scales. Pain. 2010;151:711–21.
Memis D, Inal MT, Kavalci G, Sezer A, Sut N. Intravenous paracetamol reduced the use of opioids, extubation time, and opioid-related adverse effects after major surgery in intensive care unit. J Crit Care. 2010;25:458–62.
Liu LL, Gropper MA. Postoperative analgesia and sedation in the adult intensive care unit. A guide to drug selection. Drugs. 2003;63:755–67.
Strøm T, Martinussen T, Toft P. A protocol of no sedation for critically ill patients receiving mechanical ventilation: a randomised trial. Lancet. 2010;375:475–80.
Murdoch S, Cohen A. Intensive care sedation: a review of current British practice. Intensive Care Med. 2000;26:922–8.
Battershill AJ, Keating GM. Remifentanil: a review of its analgesic and sedative use in the intensive care unit. Drugs. 2006;66:365–85.
Dahaba AA, Grabner T, Rehak PH, List WF, Metzler H. Remifentanil versus morphine analgesia and sedation for mechanically ventilated critically ill patients: a randomized double blind study. Anesthesiology. 2004;101:640–6.
Martin J, Franck M, Fischer M, Spies C. Sedation and analgesia in German intensive care units: how is it done in reality? Results of a patient-based survey of analgesia and sedation. Intensive Care Med. 2006;32:1137–42.
Pickering G, Loriot MA, Libert F, Eschalier A, Beaune P, Dubray C. Analgesic effect of acetaminophen in humans: first evidence of a central serotonergic mechanism. Clin Pharmacol Ther. 2006;79:371–8.
Peduto VA, Ballabio M, Stefanini S. Efficacy of propacetamol in the treatment of postoperative pain. Morphine sparing effect in orthopedic surgery. Italian Collaborative Group on Propacetamol. Acta Anaesthesiol Scand. 1998;42:293–8.
Tuman KJ, McCarthy RJ, March RJ, DeLaria GA, Patel RV, Ivankovich AD. Effects of epidural anesthesia and analgesia on coagulation and outcome after major vascular surgery. Anesth Analg. 1991;73:696–704.
Ryan P, Schweitzer SA, Woods RJ. Effect of epidural and general anaesthesia compared with general anaesthesia alone in large bowel anastomoses. A prospective study. Eur J Surg. 1992;158:45–9.
Stevens RA, Mikat-Stevens M, Flanigan R, Waters WB, Furry P, Sheikh T, et al. Does the choice of anesthetic technique affect the recovery of bowel function after radical prostatectomy? Urology. 1998;52:213–8.
Bauer C, Hentz JG, Ducrocq X, Meyer N, Oswald-Mammosser M, Steib A, et al. Lung function after lobectomy: a randomized, double-blinded trial comparing thoracic epidural ropivacaine/sufentanil and intravenous morphine for patient-controlled analgesia. Anesth Analg. 2007;105:238–44.
Flisberg P, Törnebrandt K, Walther B, Lundberg J. Pain relief after esophagectomy: thoracic epidural analgesia is better than parenteral opioids. J Cardiothorac Vasc Anesth. 2001;15:282–7.
Grass JA. The role of epidural anesthesia and analgesia in postoperative outcome. Anesthesiol Clin North America. 2000;18:407–28.
Schweinger JW. The pathophysiology, diagnosis and management for flail chest injury and pulmonary contusion: a review. Review course lectures. Anesth Analg. 2001;92:S86–93.
Simon BJ, Cushman J, Barraco R, Lane V, Luchette FA, Miglietta M, et al. Pain management guidelines for blunt thoracic trauma. Trauma. 2005;59:1256–67.
Hall RI, MacLaren C, Smith MS, McIntyre AJ, Allen CT, Murphy JT, et al. Light versus heavy sedation after cardiac surgery: myocardial ischemia and the stress response. Maritime Heart Centre and Dalhousie University. Anesth Analg. 1997;85:971–8.
Kress JP, Pohlman AS, O’Connor MF, Hall JB. Daily interruption of sedative infusions in critically ill patients undergoing mechanical ventilation. N Engl J Med. 2000;342:1471–7.
Ramsay MA, Savege TM, Simpson BR, Goodwin R. Controlled sedation with alphaxalone-alphadolone. Br Med J. 1974;2:656–9.
Riker RR, Picard JT, Fraser GL. Prospective evaluation of the Sedation-Agitation Scale for adult critically ill patients. Crit Care Med. 1999;27:1325–9.
Sessler CN, Gosnell MS, Grap MJ, Brophy GM, O’Neal PV, Keane KA, et al. The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002;166:1338–44.
Ely EW, Truman B, Shintani A, Thomason JW, Wheeler AP, Gordon S, et al. Monitoring sedation status over time in ICU patients: reliability and validity of the Richmond Agitation-Sedation Scale (RASS). JAMA. 2003;289:2983–91.
Riker RR, Fraser GL, Simmons LE, Wilkins ML. Validating the Sedation-Agitation Scale with the Bispectral Index and Visual Analog Scale in adult ICU patients after cardiac surgery. Intensive Care Med. 2001;27:853–8.
De Deyne C, Struys M, Decruyenaere J, Creupelandt J, Hoste E, Colardyn F. Use of continuous bispectral EEG monitoring to assess depth of sedation in ICU patients. Intensive Care Med. 1998;24:1294–8.
Nasraway Jr SASA, Wu EC, Kelleher RM, Yasuda CM, Donnelly AM. How reliable is the Bispectral Index in critically ill patients? A prospective, comparative, single blinded observer study. Crit Care Med. 2002;30:1483–7.
Weatherburn C, Endacott R, Tynan P, Bailey M. The impact of bispectral index monitoring on sedation administration in mechanically ventilated patients. Anaesth Intensive Care. 2007;35:204–8.
Ely EW, Truman B, Manzi DJ, Sigl JC, Shintani A, Bernard GR. Consciousness monitoring in ventilated patients: bispectral EEG monitors arousal not delirium. Intensive Care Med. 2004;30:1537–43.
Deogaonkar A, Gupta R, DeGeorgia M, Sabharwal V, Gopakumaran B, Schubert A. Bispectral Index monitoring correlates with sedation scales in brain-injured patients. Crit Care Med. 2004;32:2403–6.
Jacobs JR, Reves JG, Glass PS. A rationale and technique for continuous infusions in anesthesia. Int Anesthesiol Clin. 1991;29:23–38.
Kress JP, Hall JB. Sedation in the mechanically ventilated patient. Crit Care Med. 2006;34:2541–6.
Pandharipande P, Shintani A, Peterson J, Pun BT, Wilkinson GR, Dittus RS. Lorazepam is an independent risk factor for transitioning to delirium in intensive care unit patients. Anesthesiology. 2006;104:21–6.
Wilson KC, Reardon C, Theodore AC, Farber HW. Propylene glycol toxicity: a severe iatrogenic illness in ICU patients receiving IV benzodiazepines: a case series and prospective, observational pilot study. Chest. 2005;128:1674–81.
Devlin JW, Lau AK, Tanios MA. Propofol-associated hypertriglyceridemia and pancreatitis in the intensive care unit: an analysis of frequency and risk factors. Pharmacotherapy. 2005;25:348–52.
Kam PC, Cardone D. Propofol infusion syndrome. Anaesthesia. 2007;62:690–701.
Corbett SM, Moore J, Rebuck JA, Rogers FB, Greene CM. Survival of propofol infusion syndrome in a head-injured patient. Crit Care Med. 2006;34:2479–83.
Vasile B, Rasulo F, Candiani A, Latronico N. The pathophysiology of propofol infusion syndrome. A simple name for a complex syndrome. Intensive Care Med. 2003;29:1417–25.
Lang BC, Yang J, Wang Y, Luo Y, Kang Y, Liu J, Zhang WS. An improved design of water-soluble propofol prodrugs characterized by rapid onset of action. Anesth Analg. 2014;118:745–54.
Wong C, Burry L, Molino-Carmona S, Leo M, Tessler J, Hynes P, et al. Analgesic and sedative pharmacology in the intensive care unit. Dynamics. 2004;15:23–6.
Ip Yam PC, Forbes A, Kox WJ. Clonidine in the treatment of alcohol withdrawal in the intensive care unit. Br J Anaesth. 1992;68:106–8.
Maccioli GA. Dexmedetomidine to facilitate drug withdrawal. Anesthesiology. 2003;98:575–7.
Jakob SM, Ruokonen E, Grounds RM, Sarapohja T, Garratt C, Pocock SJ, et al. Dexmedetomidine vs midazolam or propofol for sedation during prolonged mechanical ventilation. JAMA. 2012;307:1151–60.
Patil N, Weinhouse GL. Randomized controlled trial of dexmedetomidine to treat intensive care unit delirium. Crit Care Med. 2006;34:A1.
Szumita PM, Baroletti SA, Anger KE, Wechsler ME. Sedation and analgesia in the intensive care unit: evaluating the role of dexmedetomidine. Am J Health Syst Pharm. 2007;64:37–44.
Riker RR, Shehabi Y, Bokesch PM, Ceraso D, Wisemandle W, Koura F, et al. Dexmedetomidine vs midazolam for sedation of critically ill patients: a randomized trial. JAMA. 2009;301:489–99.
Pandharipande PP, Pun BT, Herr DL, Maze M, Girard TD, Miller RR, et al. Effect of sedation with dexmedetomidine vs lorazepam on acute brain dysfunction in mechanically ventilated patients: the MENDS randomized controlled trial. JAMA. 2007;298:2644–53.
Inouye SK, Bogardus Jr ST, Charpentier PA, Leo-Summers L, Acampora D, Holford TR, et al. A multicomponent intervention to prevent delirium in hospitalized older patients. N Engl J Med. 1999;340:669–76.
Marcantonio ER, Flacker JM, Wright RJ, Resnick NM. Reducing delirium after hip fracture: a randomized trial. J Am Geriatr Soc. 2001;49:516–22.
Hopkins RO, Weaver LK, Pope D, Orme JF, Bigler ED, Larson-Lohr V. Neuropsychological sequelae and impaired health status in survivors of acute respiratory distress syndrome. Am J Respir Crit Care Med. 1999;160:50–6.
Pandharipande P, Cotton BA, Shintani A, Thompson J, Costabile S, Truman Pun B, et al. Motoric subtypes of delirium in mechanically ventilated surgical and trauma intensive care patients. Intensive Care Med. 2007;33:1726–31.
Ely EW, Inouye SK, Bernard GR, Gordon S, Francis J, May L, et al. Delirium in mechanically ventilated patients: validity and reliability of the confusion assessment method for the intensive care unit (CAM-ICU). JAMA. 2001;286:2703–10.
Bergeron N, Dubois MJ, Dumont M, Dial S, Skrobik Y. Intensive care delirium screening checklist: evaluation of a new screening tool. Intensive Care Med. 2001;27:859–64.
Inouye SK, Rushing JT, Foreman MD, Palmer RM, Pompei P. Does delirium contributes to poor hospital outcomes? A three site epidemiological study. J Gen Intern Med. 1998;13:234–42.
Milbrandt EB, Deppen S, Harrison PL, Shintani AK, Speroff T, Stiles RA, et al. Costs associated with delirium. Crit Care Med. 2004;32:955–62.
Pun BT, Gordon SM, Peterson JF, Shintani AK, Jackson JC, Foss J, et al. Large scale implementation of sedation and delirium monitoring in the intensive care unit: a report from two medical centers. Crit Care Med. 2005;33:1199–205.
Tesar GE, Murray GB, Cassem NH. Use of high-dose intravenous haloperidol in the treatment of agitated cardiac patients. J Clin Psychopharmacol. 1985;5:344–7.
Devlin JW, Roberts RJ, Fong JJ, Skrobik Y, Riker RR, Hill NS. Efficacy and safety of quetiapine in critically ill patients with delirium: a prospective, multicenter, randomized, double-blind, placebo-controlled pilot study. Crit Care Med. 2010;38:419–27.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2016 Springer International Publishing Switzerland
About this chapter
Cite this chapter
Alli, S., Azocar, R.J. (2016). Analgesia and Sedation. In: O'Donnell, J., Nácul, F. (eds) Surgical Intensive Care Medicine. Springer, Cham. https://doi.org/10.1007/978-3-319-19668-8_11
Download citation
DOI: https://doi.org/10.1007/978-3-319-19668-8_11
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-19667-1
Online ISBN: 978-3-319-19668-8
eBook Packages: MedicineMedicine (R0)