Abstract
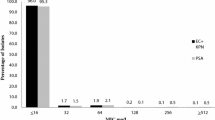
A variety of bacterial species are associated with acute respiratory tract infections, including Gram-positive, Gram-negative, and atypical pathogens. The most common pathogens include Streptococcus pneumoniae, Mycoplasma pneumoniae, Chlamydia pneumoniae, Legionella species, Haemophilus influenzae, and Moraxella catarrhalis. Because of cost considerations and specimen collection difficulties, primary care physicians seldom attempt to identify the causative pathogen. As a result treatment is necessarily empiric with agents including: the 13-lactams, macrolides, tetracyclines, and trimethoprim-sulfamethoxazole (TMP-SMX). However, antimicrobial resistance among the most common respiratory tract pathogens to these agents is increasing [1-5]. Specifically, the growing problem of multidrug resistant pneumococci has been the catalyst for the development of fluoroquinolones such as levofloxacin, gatifloxacin, which are effective against this resistant organism. However, there are reports of fluoroquinolone resistance emerging among pneumococci from a number of countries including: Canada, Spain, Hong Kong, Eastern and Central Europe, and Northern Ireland Figure 1. In Canada, Chen et al. [6] found that the prevalence of ciprofloxacin-resistant pneumococci (MIC >_ 4.ug/ml) increased from 0% in 1993 to 1.7% in 1997-1998 (p = 0.01). In adults, the prevalence increased from 0% in 1993 to 3.7% in 1998.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Preview
Unable to display preview. Download preview PDF.
Similar content being viewed by others
References
Low DE (2000) Trends and significance of antimicrobial resistance in respiratory pathogens. Opin Infect Dis 13: 145–153
Doern GV, Heilmann KP Huynh HK, Rhomberg PR, Coffman SL, Brueggemann AB (2001) Antimicrobial resistance among clinical isolates of Streptococcus pneumoniae in the United States during 1999–2000, including a comparison of resistance rates since 1994–1995. Antimicrob Agents Chemother 45(6): 1721–1729
Doern GV, Jones RN, Pfaller MA, Kugler K (1999) Haemophilus influenzae and Moraxella catarrhalis from patients with community-acquired respiratory tract infections: antimicrobial susceptibility patterns from the SENTRY antimicrobial Surveillance Program (United States and Canada, 1997). Antimicrob Agents Chemother 43(2): 385–389
Zhanel GG, Karlowsky JA, Low DE, Hoban DJ (2000) Antibiotic resistance in respiratory tract isolates of Haemophilus influenzae and Moraxella catarrhalis collected from across Canada in 1997–1998. J Antimicrob Chemother 45(5): 655–662
Pfaller MA, Ehrhardt AF, Jones RN (2001) Frequency of pathogen occurrence and antimicrobial susceptibility among community-acquired respiratory tract infections in the respiratory surveillance program study: microbiology from the medical office practice environment. Am J Med 111 Suppl 9A: 4S–12S
Chen D, McGeer A, de Azavedo JC, Low DE, The Canadian Bacterial Surveillance Network (1999) Decreased susceptibility of Streptococcus pneumoniae to fluoroquinolones in Canada. N Eng JMed 341(4): 233–239
Linares J, De La Campa AG, Pallares R (1999) Fluoroquinolone resistance in Streptococcus pneumoniae [letter]. N Engl J Med 341(20): 1546–1547
Ho PL, Que TL, Tsang DN, Ng TK, Chow KH, Seto WH (1999) Emergence of fluoroquinolone resistance among multiply resistant strains of Streptococcus pneumoniae in Hong Kong. Antimicrob Agents Chemother 43(5): 1310–1313
Ho PL, Yung RW, Tsang DN, Que TL, Ho M, Seto WH, Ng TK, Yam WC, Ng WW (2001) Increasing resistance of Streptococcus pneumoniae to fluoroquinolones: results of a Hong Kong multicentre study in 2000. JAntimicrob Chemother 48(5): 659–665
Nagai K, Appelbaum PC, Davies TA, Kelly LM, Hoellman DB, Andrasevic AT, Drukalska L, Hryniewicz W, Jacobs MR, Kolman J et al (2002) Susceptibilities to telithromycin and six other agents and prevalence of macrolide resistance due to L4 ribosomal protein mutation among 992 pneumococci from 10 Central and Eastern European countries. Antimicrob Agents Chemother 46(2): 371–377
Goldsmith CE, Moore JE, Murphy PG, Ambler JE (1998) Increased incidence of ciprofloxacin resistance in penicillin-resistant pneumococci in Northern Ireland [letter; comment]. JAntimicrob Chemother 41(3): 420–421
Brueggemann AB, Coffman SL, Rhomberg P, Huynh H, Almer L, Nilius A, Flamm R, Doern GV (2002) Fluoroquinolone Resistance in Streptococcus pneumoniae in United States since 1994–1995. Antimicrob Agents Chemother 46(3): 680–688
Sahm DF, Peterson DE, Critchley IA, Thornsberry C (2000) Analysis of ciprofloxacin activity against Streptococcus pneumoniae after 10 years of use in the United States. Antimicrob Agents Chemother 44(9): 2521–2524
Sahm DF, Karlowsky JA, Kelly LJ, Critchley IA, Jones ME, Thornsberry C, Mauriz Y, Kahn J (2001) Need for annual surveillance of antimicrobial resistance in Streptococcus pneumoniae in the United States: 2-year longitudinal analysis. Antimicrob Agents Chemother 45(4): 1037–1042
Centers for Disease Control (2001) Resistance of Streptococcus pneumoniae to fluoroquinolonesUnited States, 1995–1999. Morbid Mortal Weekly Rep 50(37): 800–804
Alou L, Ramirez M, Garcia-Rey C, Prieto J, de Lencastre H (2001) Streptococcus pneumoniae isolates with reduced susceptibility to ciprofloxacin in Spain: clonal diversity and appearance of ciprofloxacin-resistant epidemic clones. Antimicrob Agents Chemother 45(10): 2955–2957
Perez-Trallero E, Fernandez-Mazarrasa C, Garcia-Rey C, Bouza E, Aguilar L, Garcia-de-Lomas J, Baquero F (2001) Antimicrobial susceptibilities of 1,684 Streptococcus pneumoniae and 2,039 Streptococcus pyogenes isolates and their ecological relationships: results of a 1-year (1998–1999) multicenter surveillance study in Spain. Antimicrob Agents Chemother 45(12): 3334–3340
McGee L, Goldsmith CE, Kingman KP (2002) Fluoroquinolone resistance among clinical isolates of Streptococcus pneumoniae belonging to international multiresistant clones. J Antimicrob Chemother 49(1): 173–176
Deeks SL, Palacio R, Ruvinsky R, Kertesz DA, Hortal M, Rossi A, Spika JS, Di Fabio JL (1999) Risk factors and course of illness among children with invasive penicillin-resistant Streptococcus pneumoniae. The Streptococcus pneumoniae Working Group. Pediatrics 103(2): 409–413
Straus WL, Qazi SA, Kundi Z, Nomani NK, Schwartz B (1998) Antimicrobial resistance and clinical effectiveness of co-trimoxazole versus amoxycillin for pneumonia among children in Pakistan: randomised controlled trial. Pakistan Co-trimoxazole Study Group. Lancet 352(9124): 270–274
Davies BI, Maesen FP, Baur C (1986) Ciprofloxacin in the treatment of acute exacerbations of chronic bronchitis. Eur J Clin Microbial 5(2): 226–231
Hoogkamp-Korstanje JA, Klein SJ (1986) Ciprofloxacin in acute exacerbations of chronic bronchitis. JAntimicrob Chemother 18(3): 407–413
Maesen FP, Davies BI, Geraedts WH, Baur C (1987) The use of quinolones in respiratory tract infections. Drugs 34 Suppl 1: 74–79
Thys JP (1988) Quinolones in the treatment of bronchopulmonary infections. Rev Infect Dis 10 Suppl 1: S212—S217
Weiss K, Restieri C, Laverdiere M, McGeer A, Davidson RJ, Kilburn L, Bast DJ, de Azavedo J, Low DE (2001) A nosocomial outbreak of fluoroquinolone-resistant Streptococcus pneumoniae. Clin Inf Dis 33(4): 517–522
Davidson R, Cavalcanti R, Brunton JL, Bast DJ, de Azavedo JC, Kibsey P, Fleming C, Low DE (2002) Resistance to levofloxacin and failure of treatment of pneumococcal pneumonia. N Engl J Med 346(10): 747–750
Empey PE, Jennings HR, Thornton AC, Rapp RP, Evans ME (2001) Levofloxacin failure in a patient with pneumococcal pneumonia. Ann Pharmacother 35(6): 687–690
Kays MB, Smith DW, Wack ME, Denys GA (2002) Levofloxacin treatment failure in a patient with fluoroquinolone-resistant Streptococcus pneumoniae pneumonia. Pharmacotherapy 22(3): 395–399
Lee BL, Kimbrough RC, Jones SR, Mills J, Sande MA (1991) Infectious complications with respiratory pathogens despite ciprofloxacin therapy. N Engl J Med 325(7): 520–521
Cooper B, Lawlor M (1989) Pneumococcal bacteremia during ciprofloxacin therapy for pneumococcal pneumonia [see comments]. Am J Med 87(4): 475
Perez-Trallero E, Garcia-Arenzana JM, Jimenez JA, Peris A (1990) Therapeutic failure and selection of resistance to quinolones in a case of pneumococcal pneumonia treated with ciprofloxacin. Eur J Clin Microbial Infect Dis 9(12): 905–906
Gordon JJ, Kauffman CA (1990) Superinfection with Streptococcus pneumoniae during therapy with ciprofloxacin. Am J Med 89(3): 383–384
Pollack M (2000) Pseudomona aeruginosa. In: GL Mandell, JE Bennett, R Daim (eds): Mandell,Douglas, and Bennett’s principles and practise of infectious diseases. Toronto: Churchill Livingstone, 2310–2335
Chandler JR (1968) Malignant external otitis. Laryngoscope 78(8): 1257–1294
Rubin J, Yu VL (1988) Malignant external otitis: insights into pathogenesis, clinical manifestations, diagnosis, and therapy. Am J Med 85(3): 391–398
Zaky DA, Bentley DW, Lowy K, Betts RF, Douglas RG Jr (1976) Malignant external otitis: a severe form of otitis in diabetic patients. Am J Med 61(2): 298–302
Damiani JM, Damiani KK, Kinney SE (1979) Malignant external otitis with multiple cranial nerve involvement. Am J Otol 1(2): 115–120
Rubin J, Curtin HD, Yu VL, Kamerer DB (1990) Malignant external otitis: utility of CT in diagnosis and follow-up. Radiology 174(2): 391–394
Giamarellou H (1992) Malignant otitis externa: the therapeutic evolution of a lethal infection. J Antimicrob Chemother 30(6): 745–751
Morrison GA, Bailey CM (1988) Relapsing malignant otitis externa successfully treated with ciprofloxacin. J Laryngol Otol 102(10): 872–876
Lang R, Goshen S, Kitzes-Cohen R, Sade J (1990) Successful treatment of malignant external otitis with oral ciprofloxacin: report of experience with 23 patients. J Infect Dis 161(3): 537–540
Sade J, Lang R, Goshen S, Kitzes-Cohen R (1989) Ciprofloxacin treatment of malignant external otitis. Am J Med 87(5A): 138S–141S
Rubin J, Stoehr G, Yu VL, Muder RR, Matador A, Kamerer DB (1989) Efficacy of oral ciprofloxacin plus rifampin for treatment of malignant external otitis. Arch Otolaryngol Head Neck Surg 115(9): 1063–1069
Bluestone CD (2001) Efficacy of ofloxacin and other ototopical preparations for chronic suppurative otitis media in children. Pediatr Infect Dis J 20(1): 111–115
Bluestone CD (2000) Clinical course, complications and sequelae of acute otitis media. Pediatr Infect Dis J 19(5 Suppl): S37–S46
Kenna MA, Bluestone CD (1986) Microbiology of chronic suppurative otitis media in children. Pediatr Infect Dis 5(2): 223–225
Goldblatt EL, Dohar J, Nozza RJ, Nielsen RW, Goldberg T, Sidman JD, Seidlin M (1998) Topical ofloxacin versus systemic amoxicillin/clavulanate in purulent otorrhea in children with tympanostomy tubes. Int J Pediatr Otorhinolaryngol 46(1–2): 91–101
Dohar JE, Gamer ET, Nielsen RW, Biel MA, Seidlin M (1999) Topical ofloxacin treatment of otorrhea in children with tympanostomy tubes. Arch Otolaryngol Head Neck Surg 125(5): 537–545
Agro AS, Garner ET, Wright JW, III, Caballeros dE, I, Villeda B, Seidlin M (1998) Clinical trial of ototopical ofloxacin for treatment of chronic suppurative otitis media. Clin Ther 20(4): 744–759
Kaga K, Ichimura K (1998) A preliminary report: clinical effects of otic solution of ofloxacin in infantile myringitis and chronic otitis media. Int J Pediatr Otorhinolaryngol 42(3): 199–205
Tong MC, Woo JK, van Hasselt CA (1996) A double-blind comparative study of ofloxacin otic drops versus neomycin-polymyxin B-hydrocortisone otic drops in the medical treatment of chronic suppurative otitis media. JLaryngol Otol 110(4): 309–314
Hickner JM, Bartlett JG, Besser RE, Gonzales R, Hoffman JR, Sande MA (2001) Principles of appropriate antibiotic use for acute rhinosinusitis in adults: background. Ann Emerg Med 37(6): 703–710
Gwaltney JM Jr (1996) Acute community-acquired sinusitis. Clin Infect Dis 23(6): 1209–1223
Lindbaek M, Hjortdahl P, Johnsen UL (1996) Randomised, double blind, placebo controlled trial of penicillin V and amoxycillin in treatment of acute sinus infections in adults. BMJ 313(7053): 325–329
Axelsson A, Chidekel N, Grebelius N, Jensen C (1970) Treatment of acute maxillary sinusitis. A comparison of four different methods. Acta Otolaryngol 70(1): 71–76
Gananca M, Trabulsi LR (1973) The therapeutic effects of cyclacillin in acute sinusitis: in vitro and in vivo correlations in a placebo-controlled study. Curr Med Res Opin 1(6): 362–368
Stalman W, van Essen GA, van der GY, de Melker RA (1997) The end of antibiotic treatment in adults with acute sinusitis-like complaints in general practice? A placebo-controlled double-blind randomized doxycycline trial. Br J Gen Pract 47(425): 794–799
van Buchem FL, Knottnerus JA, Schrijnemaekers VJ, Peeters MF (1997) Primary-care-based randomised placebo-controlled trial of antibiotic treatment in acute maxillary sinusitis [see comments]. Lancet 349(9053): 683–687
Antimicrobial treatment guidelines for acute bacterial rhinosinusitis Sinus, Allergy Health Partnership (2000) Otolaryngol Head Neck Surg 123(1 Pt 2): 5–31
Brook I, Gooch WM, III, Jenkins SG, Pichichero ME, Reiner SA, Sher L, Yamauchi T (2000) Medical management of acute bacterial sinusitis. Recommendations of a clinical advisory committee on pediatric and adult sinusitis. Ann Otol Rhinol Laryngol Suppl 182: 2–20
Clifford K, Huck W, Shan M, Tosiello R, Echols RM, Heyd A (1999) Double-blind comparative trial of ciprofloxacin versus clarithromycin in the treatment of acute bacterial sinusitis. Sinusitis Infection Study Group. Ann Otol Rhinol Laryngol 108(4): 360–367
Johnson PA, Rodriguez HP, Wazen JJ, Huck W, Shan M, Tosiello R, Heyd A, Echols RM (1999) Ciprofloxacin versus cefuroxime axetil in the treatment of acute bacterial sinusitis. Sinusitis Infection Study Group. J Otolaryngol 28(1): 3–12
Weis M, Hendrick K, Tillotson G, Gravelle K (1998) Multicenter comparative trial of ciprofloxacin versus cefuroxime axetil in the treatment of acute rhinosinusitis in a primary care setting. Rhinosinusitis Investigation Group. Clin Ther 20(5): 921–932
Klein GL, Whalen E, Echols RM, Heyd A (1998) Ciprofloxacin versus cefuroxime axetil in the treatment of adult patients with acute bacterial sinusitis. J Otolaryngol 27(1): 10–16
Rakkar S, Roberts K, Towe BF, Flores SM, Heyd A, Warner J (2001) Moxifloxacin versus amoxicillin clavulanate in the treatment of acute maxillary sinusitis: a primary care experience. Int J Clin Pract 55(5): 309–315
Burke T, Villanueva C, Mariano H Jr, Huck W, Orchard D, Haverstock D, Heyd A, Church D (1999) Comparison of moxifloxacin and cefuroxime axetil in the treatment of acute maxillary sinusitis. Sinusitis Infection Study Group. Clin Ther 21(10): 1664–1677
Sher LD, McAdoo MA, Bettis RB, Turner MA, Li NF, Pierce PF (2002) A multicenter, random-ized, investigator-blinded study of 5- and 10-day gatifloxacin versus 10-day amoxicillin/clavulanate in patients with acute bacterial sinusitis. Clin Ther 24(2): 269–281
Lasko B, Lau CY, Saint-Pierre C, Reddington JL, Martel A, Anstey RJ (1998) Efficacy and safety of oral levofloxacin compared with clarithromycin in the treatment of acute sinusitis in adults: a multicentre, double-blind, randomized study. The Canadian Sinusitis Study Group. J Int Med Res 26(6): 281–291
Adelglass J, DeAbate CA, McElvaine P, Fowler CL, LoCocco J, Campbell T (1999) Comparison of the effectiveness of levofloxacin and amoxicillin-clavulanate for the treatment of acute sinusitis in adults. Otolaryngol Head Neck Surg 120(3): 320–327
Adelglass J, Jones TM, Ruoff G, Kahn JB, Wiesinger BA, Rielly-Gauvin K, Siu CO (1998) A multicenter, investigator-blinded, randomized comparison of oral levofloxacin and oral clarithromycin in the treatment of acute bacterial sinusitis. Pharmacotherapy 18(6): 1255–1263
Barry AL, Fuchs PC, Brown SD (2001) In vitro activities of three nonfluorinated quinolones against representative bacterial isolates. Antimicrob Agents Chemother 45(6): 1923–1927
Yan SS, Fox ML, Holland SM, Stock F, Gill VJ, Fedorko DP (2000) Resistance to multiple fluoroquinolones in a clinical isolate of Streptococcus pyogenes: identification of gyrA and parC and specification of point mutations associated with resistance. Antimicrob Agents Chemother 44(11): 3196–3198
Anthonisen NR, Manfreda J, Warren CP, Hershfield ES, Harding GK, Nelson NA (1987) Antibiotic therapy in exacerbations of chronic obstructive pulmonary disease. Ann Intern Med 106(2): 196–204
Murphy TF, Sethi S, Niederman MS (2000) The role of bacteria in exacerbations of COPD. A constructive view. Chest 118(1): 204–209
Murphy TF, Sethi S (1992) Bacterial infection in chronic obstructive pulmonary disease. Am Rev Respir Dis 146(4): 1067–1083
Saint S, Bent S, Vittinghoff E, Grady D (1995) Antibiotics in chronic obstructive pulmonary disease exacerbations. A meta-analysis [see comments]. JAMA 273(12): 957–960
Ball P (1995) Epidemiology and treatment of chronic bronchitis and its exacerbations. Chest 108(2 Suppl): 43S–52S
Fagon JY, Chastre J, Trouillet JL, Domart Y, Dombret MC, Bornet M, Gibert C (1990) Characterization of distal bronchial microflora during acute exacerbation of chronic bronchitis. Use of the protected specimen brush technique in 54 mechanically ventilated patients. Am Rev Respir Dis 142(5): 1004–1008
Monso E, Ruiz J, Rosell A, Manterola J, Fiz J, Morera J, Ausina V (1995) Bacterial infection in chronic obstructive pulmonary disease. A study of stable and exacerbated outpatients using the protected specimen brush. Am J Respir Crit Care Med 152(4 Pt 1): 1316–1320
Baiter MS, Hyland RH, Low DE, Renzi PM (1994) Recommendations on the management of chronic bronchitis. CMAJ 151(Suppl 10): 7–23
Schaberg T, Ballin I, Huchon G, Bassaris H, Hampel B, Reimnitz P (2001) A multinational, multicentre, non-blinded, randomized study of moxifloxacin oral tablets compared with co-amoxiclav oral tablets in the treatment of acute exacerbation of chronic bronchitis. J Int Med Res 29(4): 314–328
DeAbate CA, Mathew CP, Warner JH, Heyd A, Church D (2000) The safety and efficacy of short course (5-day) moxifloxacin versus azithromycin in the treatment of patients with acute exacerbation of chronic bronchitis. Respir Med 94(11): 1029–1037
Chodosh S, DeAbate CA, Haverstock D, Aneiro L, Church D (2000) Short-course moxifloxacin therapy for treatment of acute bacterial exacerbations of chronic bronchitis. The Bronchitis Study Group. Respir Med 94(1): 18–27
Wilson R, Kubin R, Ballin I, Deppermann KM, Bassaris HP, Leophonte P, Schreurs AJ, Torres A, Sommerauer B (1999) Five day moxifloxacin therapy compared with 7 day clarithromycin therapy for the treatment of acute exacerbations of chronic bronchitis. JAntimicrob Chemother 44(4): 501–513
Gotfried MH, DeAbate CA, Fogarty C, Mathew CP, Sokol WN (2001) Comparison of 5-day, short-course gatifloxacin therapy with 7-day gatifloxacin therapy and 10-day clarithromycin therapy for acute exacerbation of chronic bronchitis. Clin Ther 23(1): 97–107
Masterton RG, Burley CJ (2001) Randomized, double-blind study comparing 5- and 7-day regimens of oral levofloxacin in patients with acute exacerbation of chronic bronchitis. Int J Antimicrob Agents 18(6): 503–512
Norrby SR (2001) Optimal treatment strategies for acute exacerbations of chronic bronchitis: high-risk patients. Chemotherapy 47 Suppl 4: 47–52
Read RC, Kuss A, Berrisoul F, Kearsley N, Tones A, Kubin R (1999) The efficacy and safety of a new ciprofloxacin suspension compared with co-amoxiclav tablets in the treatment of acute exacerbations of chronic bronchitis. Respir Med 93(4): 252–261
Anzueto A, Niederman MS, Tillotson GS (1998) Etiology, susceptibility, and treatment of acute bacterial exacerbations of complicated chronic bronchitis in the primary care setting: ciprofloxacin 750 mg b.i.d. versus clarithromycin 500 mg b.i.d. Bronchitis Study Group. Clin Ther 20(5): 885–900
Chodosh S, Schreurs A, Siami G, Barkman HW, Anzueto A, Shan Moesker H, Stack T, Kowalsky S, the Bronchitis Study Group (1998) Efficacy of oral ciprofloxacin versus clarithromycin for treatment of acute bacterial exacerbations of chronic bronchitis. Clin Infect Dis 27: 730–738
Chodosh S, McCarty J, Farkas S, Drehobl M, Tosiello R, Shan M, Aneiro L, Kowalsky S (1998) Randomized, double-blind study of ciprofloxacin and cefuroxime axetil for treatment of acute bacterial exacerbations of chronic bronchitis. The Bronchitis Study Group. Clin Infect Dis 27(4): 722–729
DeAbate CA, Henry D, Bensch G, Jubran A, Chodosh S, Harper L, Tipping D, Talbot GH (1998) Sparfloxacin vs ofloxacin in the treatment of acute bacterial exacerbations of chronic bronchitis: a multicenter, double-blind, randomized, comparative study. Sparfloxacin Multicenter ABECB Study Group. Chest 114(1): 120–130
Anzueto A, Rizzo JA, Grossman RF (1999) The infection-free interval: its use in evaluating antimicrobial treatment of acute exacerbation of chronic bronchitis. Clin Infect Dis 28(6): 1344–1345
Grossman RF (1998) The value of antibiotics and the outcomes of antibiotic therapy in exacerbations of COPD. Chest 113(4 Suppl): 249S–255S
Nouira S, Marghli S, Belghith M, Besbes L, Elatrous S, Abroug F (2001) Once daily oral ofloxacin in chronic obstructive pulmonary disease exacerbation requiring mechanical ventilation: a randomised placebo-controlled trial. Lancet 358(9298): 2020–2025
Ho PL, Tse WS, Tsang KW, Kwok TK, Ng TK, Cheng VC, Chan RM (2001) Risk factors for acquisition of levofloxacin-resistant Streptococcus pneumoniae: a case-control study. Clin Infect Dis 32(5): 701–707
Nicolau DP, Ambrose PG (2001) Pharmacodynamic profiling of levofloxacin and gatifloxacin using Monte Carlo simulation for community-acquired isolates of Streptococcus pneumoniae. Am JMed 111 Suppl 9A: 13S–18S
Low DE, de Azavedo J, Weiss CA, Mazzulli T, Kuhn M, Church D et al (2002) Antimicrobial resistance among clinical isolates of Streptococcus pneumoniae in Canada during 2000. Antimicrob Agents Chemother 46 (5): 1295–1301
Thomsbeny C, Sahm DF, Kelly LJ, Critchley IA, Jones ME, Evangelista AT, Karlowsky JA (2002) Regional trends in antimicrobial resistance among clinical isolates of Streptococcus pneumoniae, Haemophilus influenzae, and Moraxella catarrhalis in the United States: Results from the TRUST Surveillance Program, 1999–2000. Clin Infect Dis 34 Suppl 1: S4–S16
Author information
Authors and Affiliations
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2003 Springer Basel AG
About this chapter
Cite this chapter
Low, D.E. (2003). Fluoroquinolones for the treatment of respiratory tract infections other than pneumonia. In: Ronald, A.R., Low, D.E. (eds) Fluoroquinolone Antibiotics. Milestones in Drug Therapy. Birkhäuser, Basel. https://doi.org/10.1007/978-3-0348-8103-6_11
Download citation
DOI: https://doi.org/10.1007/978-3-0348-8103-6_11
Published:
Publisher Name: Birkhäuser, Basel
Print ISBN: 978-3-0348-9437-1
Online ISBN: 978-3-0348-8103-6
eBook Packages: Springer Book Archive