Abstract
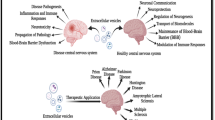
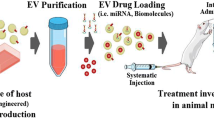
The role of extracellular vesicles (EVs) in the central nervous system, and in particular the brain, is a rapidly growing research area. Importantly, the role for EVs in the nervous system spans from early development through to old age, with EVs being associated with several different neurological disorders. To date, researchers have been studying the function of EVs in the nervous system in three major areas: (i) the role of EVs in promoting disease pathways, (ii) the ability of EVs to be used as a diagnostic tool to identify cellular changes in the nervous system, and (iii) the potential use of EVs as therapeutic tools for the delivery of biomolecules or drugs to the nervous system. In each of these settings the analysis and use of EVs performs a different function, highlighting the breadth of areas in which the EV field is applicable. A key aspect of EV biology is the ability of vesicles to cross biological barriers, in particular the blood brain barrier. This allows for the measurement of serum EVs that contain information about cells in the brain, or alternatively, allows for the delivery of biomolecules that are packaged within EVs for therapeutic use.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Acquatella-Tran Van Ba I, Imberdis T, Perrier V (2013) From prion diseases to prion-like propagation mechanisms of neurodegenerative diseases. Int J Cell Biol 2013:975832. https://doi.org/10.1155/2013/975832
Adams JB, Johansen LJ, Powell LD, Quig D, Rubin RA (2011) Gastrointestinal flora and gastrointestinal status in children with autism—comparisons to typical children and correlation with autism severity. BMC Gastroenterol 11:22. https://doi.org/10.1186/1471-230x-11-22
Akers JC, Ramakrishnan V, Kim R, Skog J, Nakano I, Pingle S, Kalinina J, Hua W, Kesari S, Mao Y, Breakefield XO, Hochberg FH, Van Meir EG, Carter BS, Chen CC (2013) miR-21 in the extracellular vesicles (EVs) of cerebrospinal fluid (CSF): a platform for glioblastoma biomarker development. PLoS One 8(10):e78115. https://doi.org/10.1371/journal.pone.0078115
Asai H, Ikezu S, Tsunoda S, Medalla M, Luebke J, Haydar T, Wolozin B, Butovsky O, Kügler S, Ikezu T (2015) Depletion of microglia and inhibition of exosome synthesis halt tau propagation. Nat Neurosci 18(11):1584–1593. https://doi.org/10.1038/nn.4132
Banigan MG, Kao PF, Kozubek JA, Winslow AR, Medina J, Costa J, Schmitt A, Schneider A, Cabral H, Cagsal-Getkin O, Vanderburg CR, Delalle I (2013) Differential expression of Exosomal microRNAs in prefrontal cortices of schizophrenia and bipolar disorder patients. PLoS One 8(1):e48814. https://doi.org/10.1371/journal.pone.0048814
Batool A, Hill TDM, Nguyen NT, Langa E, Diviney M, Mooney C, Brennan GP, Connolly NMC, Sanz-Rodriguez A, Cavanagh BL, Henshall DC (2020) Altered biogenesis and microRNA content of hippocampal exosomes following experimental status epilepticus. Front Neurosci 13:1404–1404. https://doi.org/10.3389/fnins.2019.01404
Bhalala OG, Pan L, Sahni V, McGuire TL, Gruner K, Tourtellotte WG, Kessler JA (2012) microRNA-21 regulates astrocytic response following spinal cord injury. J Neurosci 32(50):17935–17947. https://doi.org/10.1523/jneurosci.3860-12.2012
Braak H, Del Tredici K, Rüb U, de Vos RA, Jansen Steur EN, Braak E (2003) Staging of brain pathology related to sporadic Parkinson’s disease. Neurobiol Aging 24(2):197–211. https://doi.org/10.1016/s0197-4580(02)00065-9
Brothers HM, Gosztyla ML, Robinson SR (2018) The physiological roles of amyloid-β peptide hint at new ways to treat Alzheimer’s disease. Front Aging Neurosci 10:118. https://doi.org/10.3389/fnagi.2018.00118
Bryant-Waugh R, Markham L, Kreipe RE, Walsh BT (2010) Feeding and eating disorders in childhood. Int J Eat Disord 43(2):98–111. https://doi.org/10.1002/eat.20795
Cao Z, Wu Y, Liu G, Jiang Y, Wang X, Wang Z, Feng T (2019) α-Synuclein in salivary extracellular vesicles as a potential biomarker of Parkinson’s disease. Neurosci Lett 696:114–120. https://doi.org/10.1016/j.neulet.2018.12.030
Cherian A, Thomas SV (2009) Status epilepticus. Ann Indian Acad Neurol 12(3):140–153. https://doi.org/10.4103/0972-2327.56312
Ciechanover A, Kwon YT (2015) Degradation of misfolded proteins in neurodegenerative diseases: therapeutic targets and strategies. Exp Mol Med 47(3):e147–e147. https://doi.org/10.1038/emm.2014.117
Collier TJ, Redmond DE Jr, Steece-Collier K, Lipton JW, Manfredsson FP (2016) Is alpha-synuclein loss-of-function a contributor to Parkinsonian pathology? Evidence from non-human primates. Front Neurosci 10:12–12. https://doi.org/10.3389/fnins.2016.00012
Cumba Garcia LM, Peterson TE, Cepeda MA, Johnson AJ, Parney IF (2019) Isolation and analysis of plasma-derived exosomes in patients with glioma. Front Oncol 9(651). https://doi.org/10.3389/fonc.2019.00651
De Rubeis S, He X, Goldberg AP, Poultney CS, Samocha K, Ercument Cicek A, Kou Y, Liu L, Fromer M, Walker S, Singh T, Klei L, Kosmicki J, Fu S-C, Aleksic B, Biscaldi M, Bolton PF, Brownfeld JM, Cai J, Campbell NG, Carracedo A, Chahrour MH, Chiocchetti AG, Coon H, Crawford EL, Crooks L, Curran SR, Dawson G, Duketis E, Fernandez BA, Gallagher L, Geller E, Guter SJ, Sean Hill R, Ionita-Laza I, Jimenez Gonzalez P, Kilpinen H, Klauck SM, Kolevzon A, Lee I, Lei J, Lehtimäki T, Lin C-F, Ma’ayan A, Marshall CR, McInnes AL, Neale B, Owen MJ, Ozaki N, Parellada M, Parr JR, Purcell S, Puura K, Rajagopalan D, Rehnström K, Reichenberg A, Sabo A, Sachse M, Sanders SJ, Schafer C, Schulte-Rüther M, Skuse D, Stevens C, Szatmari P, Tammimies K, Valladares O, Voran A, Wang L-S, Weiss LA, Jeremy Willsey A, Yu TW, Yuen RKC, Cook EH, Freitag CM, Gill M, Hultman CM, Lehner T, Palotie A, Schellenberg GD, Sklar P, State MW, Sutcliffe JS, Walsh CA, Scherer SW, Zwick ME, Barrett JC, Cutler DJ, Roeder K, Devlin B, Daly MJ, Buxbaum JD, The DDDS, homozygosity Mapping Collaborative for A, Consortium UK, The Autism Sequencing C (2014) Synaptic, transcriptional and chromatin genes disrupted in autism. Nature 515(7526):209–215. https://doi.org/10.1038/nature13772
Du Y, Yu Y, Hu Y, Li XW, Wei ZX, Pan RY, Li XS, Zheng GE, Qin XY, Liu QS, Cheng Y (2019) Genome-wide, integrative analysis implicates exosome-derived microRNA dysregulation in schizophrenia. Schizophr Bull 45(6):1257–1266. https://doi.org/10.1093/schbul/sby191
Dujardin S, Lécolle K, Caillierez R, Bégard S, Zommer N, Lachaud C, Carrier S, Dufour N, Aurégan G, Winderickx J, Hantraye P, Déglon N, Colin M, Buée L (2014) Neuron-to-neuron wild-type tau protein transfer through a trans-synaptic mechanism: relevance to sporadic tauopathies. Acta Neuropathol Commun 2:14–14. https://doi.org/10.1186/2051-5960-2-14
Ferrara D, Pasetto L, Bonetto V, Basso M (2018) Role of extracellular vesicles in amyotrophic lateral sclerosis. Front Neurosci 12(574). https://doi.org/10.3389/fnins.2018.00574
Fevrier B, Vilette D, Archer F, Loew D, Faigle W, Vidal M, Laude H, Raposo G (2004) Cells release prions in association with exosomes. Proc Natl Acad Sci USA 101(26):9683. https://doi.org/10.1073/pnas.0308413101
Fiandaca MS, Kapogiannis D, Mapstone M, Boxer A, Eitan E, Schwartz JB, Abner EL, Petersen RC, Federoff HJ, Miller BL, Goetzl EJ (2015) Identification of preclinical Alzheimer’s disease by a profile of pathogenic proteins in neurally derived blood exosomes: a case-control study. Alzheimer’s Dementia 11(6):600–607.e601. https://doi.org/10.1016/j.jalz.2014.06.008
Fussi N, Höllerhage M, Chakroun T, Nykänen N-P, Rösler TW, Koeglsperger T, Wurst W, Behrends C, Höglinger GU (2018) Exosomal secretion of α-synuclein as protective mechanism after upstream blockage of macroautophagy. Cell Death Dis 9(7):757–757. https://doi.org/10.1038/s41419-018-0816-2
Gerdes H-H, Bukoreshtliev NV, Barroso JFV (2007) Tunneling nanotubes: a new route for the exchange of components between animal cells. FEBS Lett 581(11):2194–2201. https://doi.org/10.1016/j.febslet.2007.03.071
Geschwind MD (2015) Prion diseases. Continuum (Minneap Minn) 21(6 Neuroinfectious Disease):1612–1638. https://doi.org/10.1212/CON.0000000000000251
Gilman SR, Iossifov I, Levy D, Ronemus M, Wigler M, Vitkup D (2011) Rare de novo variants associated with autism implicate a large functional network of genes involved in formation and function of synapses. Neuron 70(5):898–907. https://doi.org/10.1016/j.neuron.2011.05.021
Goedert M, Clavaguera F, Tolnay M (2010) The propagation of prion-like protein inclusions in neurodegenerative diseases. Trends Neurosci 33(7):317–325. https://doi.org/10.1016/j.tins.2010.04.003
Goldvaser H, Gutkin A, Beery E, Edel Y, Nordenberg J, Wolach O, Rabizadeh E, Uziel O, Lahav M (2017) Characterisation of blood-derived exosomal hTERT mRNA secretion in cancer patients: a potential pan-cancer marker. Br J Cancer 117(3):353–357. https://doi.org/10.1038/bjc.2017.166
Götz J, Chen F, van Dorpe J, Nitsch RM (2001) Formation of neurofibrillary tangles in P301l tau transgenic mice induced by Abeta 42 fibrils. Science 293(5534):1491–1495. https://doi.org/10.1126/science.1062097
Grad LI, Yerbury JJ, Turner BJ, Guest WC, Pokrishevsky E, O’Neill MA, Yanai A, Silverman JM, Zeineddine R, Corcoran L, Kumita JR, Luheshi LM, Yousefi M, Coleman BM, Hill AF, Plotkin SS, Mackenzie IR, Cashman NR (2014) Intercellular propagated misfolding of wild-type Cu/Zn superoxide dismutase occurs via exosome-dependent and -independent mechanisms. Proc Natl Acad Sci 111(9):3620. https://doi.org/10.1073/pnas.1312245111
Grey M, Linse S, Nilsson H, Brundin P, Sparr E (2011) Membrane interaction of α-synuclein in different aggregation states. J Parkinsons Dis 1(4):359–371. https://doi.org/10.3233/jpd-2011-11067
Guescini M, Genedani S, Stocchi V, Agnati LF (2010) Astrocytes and Glioblastoma cells release exosomes carrying mtDNA. J Neural Transm 117(1):1–4. https://doi.org/10.1007/s00702-009-0288-8
Guo BB, Bellingham SA, Hill AF (2016) Stimulating the release of exosomes increases the intercellular transfer of prions. J Biol Chem 291(10):5128–5137. https://doi.org/10.1074/jbc.M115.684258
Guo T, Noble W, Hanger DP (2017) Roles of tau protein in health and disease. Acta Neuropathol 133(5):665–704. https://doi.org/10.1007/s00401-017-1707-9
Hafner Bratkovič I (2017) Prions, prionoid complexes and amyloids: the bad, the good and something in between. Swiss Med Wkly 147:w14424. https://doi.org/10.4414/smw.2017.14424
Haque S, Harries LW (2017) Circular RNAs (circRNAs) in health and disease. Genes (Basel) 8(12):353. https://doi.org/10.3390/genes8120353
Harrison EB, Hochfelder CG, Lamberty BG, Meays BM, Morsey BM, Kelso ML, Fox HS, Yelamanchili SV (2016) Traumatic brain injury increases levels of miR-21 in extracellular vesicles: implications for neuroinflammation. FEBS Open Bio 6(8):835–846. https://doi.org/10.1002/2211-5463.12092
Hazelton I, Yates A, Dale A, Roodselaar J, Akbar N, Ruitenberg MJ, Anthony DC, Couch Y (2017) Exacerbation of acute traumatic brain injury by circulating extracellular vesicles. J Neurotrauma 35(4):639–651. https://doi.org/10.1089/neu.2017.5049
Henshall DC (2014) MicroRNA and epilepsy: profiling, functions and potential clinical applications. Curr Opin Neurol 27(2):199–205. https://doi.org/10.1097/WCO.0000000000000079
Henshall DC, Hamer HM, Pasterkamp RJ, Goldstein DB, Kjems J, Prehn JHM, Schorge S, Lamottke K, Rosenow F (2016) MicroRNAs in epilepsy: pathophysiology and clinical utility. Lancet Neurol 15(13):1368–1376. https://doi.org/10.1016/s1474-4422(16)30246-0
Hyman SL, Stewart PA, Schmidt B, Cain U, Lemcke N, Foley JT, Peck R, Clemons T, Reynolds A, Johnson C, Handen B, James SJ, Courtney PM, Molloy C, Ng PK (2012) Nutrient intake from food in children with autism. Pediatrics 130(Suppl 2):S145–S153. https://doi.org/10.1542/peds.2012-0900L
Iguchi Y, Eid L, Parent M, Soucy G, Bareil C, Riku Y, Kawai K, Takagi S, Yoshida M, Katsuno M, Sobue G, Julien J-P (2016) Exosome secretion is a key pathway for clearance of pathological TDP-43. Brain 139(12):3187–3201. https://doi.org/10.1093/brain/aww237
Johnstone RM, Adam M, Hammond JR, Orr L, Turbide C (1987) Vesicle formation during reticulocyte maturation. Association of plasma membrane activities with released vesicles (exosomes). J Biol Chem 262(19):9412–9420
Kamelgarn M, Chen J, Kuang L, Arenas A, Zhai J, Zhu H, Gal J (2016) Proteomic analysis of FUS interacting proteins provides insights into FUS function and its role in ALS. Biochim Biophys Acta (BBA) Mol Basis Dis 1862(10):2004–2014. https://doi.org/10.1016/j.bbadis.2016.07.015
Kapogiannis D, Dobrowolny H, Tran J, Mustapic M, Frodl T, Meyer-Lotz G, Schiltz K, Schanze D, Rietschel M, Bernstein H-G, Steiner J (2019) Insulin-signaling abnormalities in drug-naïve first-episode schizophrenia: transduction protein analyses in extracellular vesicles of putative neuronal origin. Eur Psychiatry 62:124–129. https://doi.org/10.1016/j.eurpsy.2019.08.012
Kim AH, Reimers M, Maher B, Williamson V, McMichael O, McClay JL, van den Oord EJ, Riley BP, Kendler KS, Vladimirov VI (2010) MicroRNA expression profiling in the prefrontal cortex of individuals affected with schizophrenia and bipolar disorders. Schizophr Res 124(1–3):183–191. https://doi.org/10.1016/j.schres.2010.07.002
Kim DK, Nishida H, An SY, Shetty AK, Bartosh TJ, Prockop DJ (2016) Chromatographically isolated CD63+CD81+ extracellular vesicles from mesenchymal stromal cells rescue cognitive impairments after TBI. Proc Natl Acad Sci USA 113(1):170–175. https://doi.org/10.1073/pnas.1522297113
Kolarova M, García-Sierra F, Bartos A, Ricny J, Ripova D (2012) Structure and pathology of tau protein in Alzheimer disease. Int J Alzheimers Dis 2012:731526–731526. https://doi.org/10.1155/2012/731526
Kordower JH, Chu Y, Hauser RA, Freeman TB, Olanow CW (2008) Lewy body-like pathology in long-term embryonic nigral transplants in Parkinson's disease. Nat Med 14(5):504–506. https://doi.org/10.1038/nm1747
Korkut C, Ataman B, Ramachandran P, Ashley J, Barria R, Gherbesi N, Budnik V (2009) Trans-synaptic transmission of vesicular Wnt signals through Evi/Wntless. Cell 139(2):393–404. https://doi.org/10.1016/j.cell.2009.07.051
Korkut C, Li Y, Koles K, Brewer C, Ashley J, Yoshihara M, Budnik V (2013) Regulation of postsynaptic retrograde signaling by presynaptic exosome release. Neuron 77(6):1039–1046. https://doi.org/10.1016/j.neuron.2013.01.013
Kovac S, Dinkova Kostova AT, Herrmann AM, Melzer N, Meuth SG, Gorji A (2017) Metabolic and homeostatic changes in seizures and acquired epilepsy-mitochondria, calcium dynamics and reactive oxygen species. Int J Mol Sci 18(9):1935. https://doi.org/10.3390/ijms18091935
Kral TV, Eriksen WT, Souders MC, Pinto-Martin JA (2013) Eating behaviors, diet quality, and gastrointestinal symptoms in children with autism spectrum disorders: a brief review. J Pediatr Nurs 28(6):548–556. https://doi.org/10.1016/j.pedn.2013.01.008
Lashuel HA, Overk CR, Oueslati A, Masliah E (2013) The many faces of α-synuclein: from structure and toxicity to therapeutic target. Nat Rev Neurosci 14(1):38–48. https://doi.org/10.1038/nrn3406
Laurent M (1996) Prion diseases and the ‘protein only’ hypothesis: a theoretical dynamic study. Biochem J 318(Pt 1):35–39. https://doi.org/10.1042/bj3180035
Lecker SH, Goldberg AL, Mitch WE (2006) Protein degradation by the ubiquitin–proteasome pathway in Normal and disease states. J Am Soc Nephrol 17(7):1807. https://doi.org/10.1681/ASN.2006010083
Lee HJ, Patel S, Lee SJ (2005) Intravesicular localization and exocytosis of alpha-synuclein and its aggregates. J Neurosci 25(25):6016–6024. https://doi.org/10.1523/jneurosci.0692-05.2005
Lee Y, Park J-Y, Lee E-H, Yang J, Jeong B-R, Kim Y-K, Seoh J-Y, Lee S, Han P-L, Kim E-J (2017) Rapid assessment of microbiota changes in individuals with autism spectrum disorder using bacteria-derived membrane vesicles in urine. Exp Neurobiol 26(5):307–317. https://doi.org/10.5607/en.2017.26.5.307
Long Q, Upadhya D, Hattiangady B, Kim D-K, An SY, Shuai B, Prockop DJ, Shetty AK (2017) Intranasal MSC-derived A1-exosomes ease inflammation, and prevent abnormal neurogenesis and memory dysfunction after status epilepticus. Proc Natl Acad Sci USA 114(17):E3536–E3545. https://doi.org/10.1073/pnas.1703920114
Mandelkow EM, Mandelkow E (1998) Tau in Alzheimer’s disease. Trends Cell Biol 8(11):425–427. https://doi.org/10.1016/s0962-8924(98)01368-3
Marchetto MC, Carromeu C, Acab A, Yu D, Yeo GW, Mu Y, Chen G, Gage FH, Muotri AR (2010) A model for neural development and treatment of Rett syndrome using human induced pluripotent stem cells. Cell 143(4):527–539. https://doi.org/10.1016/j.cell.2010.10.016
Marí-Bauset S, Zazpe I, Mari-Sanchis A, Llopis-González A, Morales-Suárez-Varela M (2014) Food selectivity in autism spectrum disorders: a systematic review. J Child Neurol 29(11):1554–1561. https://doi.org/10.1177/0883073813498821
Mathieu M, Martin-Jaular L, Lavieu G, Théry C (2019) Specificities of secretion and uptake of exosomes and other extracellular vesicles for cell-to-cell communication. Nat Cell Biol 21(1):9–17. https://doi.org/10.1038/s41556-018-0250-9
Mattsson N, Zetterberg H, Hansson O, Andreasen N, Parnetti L, Jonsson M, Herukka SK, van der Flier WM, Blankenstein MA, Ewers M, Rich K, Kaiser E, Verbeek M, Tsolaki M, Mulugeta E, Rosén E, Aarsland D, Visser PJ, Schröder J, Marcusson J, de Leon M, Hampel H, Scheltens P, Pirttilä T, Wallin A, Jönhagen ME, Minthon L, Winblad B, Blennow K (2009) CSF biomarkers and incipient Alzheimer disease in patients with mild cognitive impairment. JAMA 302(4):385–393. https://doi.org/10.1001/jama.2009.1064
Mulle JG, Sharp WG, Cubells JF (2013) The gut microbiome: a new frontier in autism research. Curr Psychiatry Rep 15(2):337. https://doi.org/10.1007/s11920-012-0337-0
Nishikawa R, Sugiyama T, Narita Y, Furnari F, Cavenee WK, Matsutani M (2004) Immunohistochemical analysis of the mutant epidermal growth factor, deltaEGFR, in glioblastoma. Brain Tumor Pathol 21(2):53–56. https://doi.org/10.1007/bf02484510
O’Roak BJ, Vives L, Girirajan S, Karakoc E, Krumm N, Coe BP, Levy R, Ko A, Lee C, Smith JD, Turner EH, Stanaway IB, Vernot B, Malig M, Baker C, Reilly B, Akey JM, Borenstein E, Rieder MJ, Nickerson DA, Bernier R, Shendure J, Eichler EE (2012) Sporadic autism exomes reveal a highly interconnected protein network of de novo mutations. Nature 485(7397):246–250. https://doi.org/10.1038/nature10989
Pagano G, Ferrara N, Brooks DJ, Pavese N (2016) Age at onset and Parkinson disease phenotype. Neurology 86(15):1400–1407. https://doi.org/10.1212/WNL.0000000000002461
Patz S, Trattnig C, Grünbacher G, Ebner B, Gülly C, Novak A, Rinner B, Leitinger G, Absenger M, Tomescu OA, Thallinger GG, Fasching U, Wissa S, Archelos-Garcia J, Schäfer U (2013) More than cell dust: microparticles isolated from cerebrospinal fluid of brain injured patients are messengers carrying mRNAs, miRNAs, and proteins. J Neurotrauma 30(14):1232–1242. https://doi.org/10.1089/neu.2012.2596
Pavlyukov MS, Yu H, Bastola S, Minata M, Shender VO, Lee Y, Zhang S, Wang J, Komarova S, Wang J, Yamaguchi S, Alsheikh HA, Shi J, Chen D, Mohyeldin A, Kim S-H, Shin YJ, Anufrieva K, Evtushenko EG, Antipova NV, Arapidi GP, Govorun V, Pestov NB, Shakhparonov MI, Lee LJ, Nam D-H, Nakano I (2018) Apoptotic cell-derived extracellular vesicles promote malignancy of glioblastoma via intercellular transfer of splicing factors. Cancer Cell 34(1):119–135.e110. https://doi.org/10.1016/j.ccell.2018.05.012
Pellicano C, Benincasa D, Pisani V, Buttarelli FR, Giovannelli M, Pontieri FE (2007) Prodromal non-motor symptoms of Parkinson’s disease. Neuropsychiatr Dis Treat 3(1):145–152. https://doi.org/10.2147/nedt.2007.3.1.145
Perets N, Hertz S, London M, Offen D (2018) Intranasal administration of exosomes derived from mesenchymal stem cells ameliorates autistic-like behaviors of BTBR mice. Mol Autism 9(1):57. https://doi.org/10.1186/s13229-018-0240-6
Perets N, Oron O, Herman S, Elliott E, Offen D (2020) Exosomes derived from mesenchymal stem cells improved core symptoms of genetically modified mouse model of autism Shank3B. Mol Autism 11(1):65. https://doi.org/10.1186/s13229-020-00366-x
Pierce K, Gazestani VH, Bacon E, Barnes CC, Cha D, Nalabolu S, Lopez L, Moore A, Pence-Stophaeros S, Courchesne E (2019) Evaluation of the diagnostic stability of the early autism spectrum disorder phenotype in the general population starting at 12 months. JAMA Pediatr 173(6):578–587. https://doi.org/10.1001/jamapediatrics.2019.0624
Pitkänen A, Kharatishvili I, Karhunen H, Lukasiuk K, Immonen R, Nairismägi J, Gröhn O, Nissinen J (2007) Epileptogenesis in experimental models. Epilepsia 48(s2):13–20. https://doi.org/10.1111/j.1528-1167.2007.01063.x
Politis M, Wu K, Molloy S, P GB, Chaudhuri KR, Piccini P (2010) Parkinson’s disease symptoms: the patient’s perspective. Mov Disord 25(11):1646–1651. https://doi.org/10.1002/mds.23135
Prusiner SB, Scott MR, DeArmond SJ, Cohen FE (1998) Prion protein biology. Cell 93(3):337–348. https://doi.org/10.1016/s0092-8674(00)81163-0
Rajendran L, Honsho M, Zahn TR, Keller P, Geiger KD, Verkade P, Simons K (2006) Alzheimer’s disease β-amyloid peptides are released in association with exosomes. Proc Natl Acad Sci 103(30):11172–11177. https://doi.org/10.1073/pnas.0603838103
Rodriguez JI, Kern JK (2011) Evidence of microglial activation in autism and its possible role in brain underconnectivity. Neuron Glia Biol 7(2-4):205–213. https://doi.org/10.1017/s1740925x12000142
Ronemus M, Iossifov I, Levy D, Wigler M (2014) The role of de novo mutations in the genetics of autism spectrum disorders. Nat Rev Genet 15(2):133–141. https://doi.org/10.1038/nrg3585
Sardar Sinha M, Ansell-Schultz A, Civitelli L, Hildesjö C, Larsson M, Lannfelt L, Ingelsson M, Hallbeck M (2018) Alzheimer’s disease pathology propagation by exosomes containing toxic amyloid-beta oligomers. Acta Neuropathol 136(1):41–56. https://doi.org/10.1007/s00401-018-1868-1
Schapira AHV (2006) Mitochondrial disease. Lancet 368(9529):70–82. https://doi.org/10.1016/S0140-6736(06)68970-8
Sharma P, Mesci P, Carromeu C, McClatchy DR, Schiapparelli L, Yates JR 3rd, Muotri AR, Cline HT (2019) Exosomes regulate neurogenesis and circuit assembly. Proc Natl Acad Sci USA 116(32):16086–16094. https://doi.org/10.1073/pnas.1902513116
Sharples RA, Vella LJ, Nisbet RM, Naylor R, Perez K, Barnham KJ, Masters CL, Hill AF (2008) Inhibition of γ-secretase causes increased secretion of amyloid precursor protein C-terminal fragments in association with exosomes. FASEB J 22(5):1469–1478. https://doi.org/10.1096/fj.07-9357com
Shi M, Liu C, Cook TJ, Bullock KM, Zhao Y, Ginghina C, Li Y, Aro P, Dator R, He C, Hipp MJ, Zabetian CP, Peskind ER, Hu SC, Quinn JF, Galasko DR, Banks WA, Zhang J (2014) Plasma exosomal α-synuclein is likely CNS-derived and increased in Parkinson’s disease. Acta Neuropathol 128(5):639–650. https://doi.org/10.1007/s00401-014-1314-y
Skog J, Würdinger T, van Rijn S, Meijer DH, Gainche L, Sena-Esteves M, Curry WT Jr, Carter BS, Krichevsky AM, Breakefield XO (2008) Glioblastoma microvesicles transport RNA and proteins that promote tumour growth and provide diagnostic biomarkers. Nat Cell Biol 10(12):1470–1476. https://doi.org/10.1038/ncb1800
Spillantini MG, Schmidt ML, Lee VMY, Trojanowski JQ, Jakes R, Goedert M (1997) α-Synuclein in lewy bodies. Nature 388(6645):839–840. https://doi.org/10.1038/42166
Sproviero D, La Salvia S, Giannini M, Crippa V, Gagliardi S, Bernuzzi S, Diamanti L, Ceroni M, Pansarasa O, Poletti A, Cereda C (2018) Pathological proteins are transported by extracellular vesicles of sporadic amyotrophic lateral sclerosis patients. Front Neurosci 12:487–487. https://doi.org/10.3389/fnins.2018.00487
Stafstrom CE, Carmant L (2015) Seizures and epilepsy: an overview for neuroscientists. Cold Spring Harb Perspect Med 5(6). https://doi.org/10.1101/cshperspect.a022426
Tan G, Wang L, Liu Y, Zhang H, Feng W, Liu Z (2020) The alterations of circular RNA expression in plasma exosomes from patients with schizophrenia. J Cell Physiol. https://doi.org/10.1002/jcp.29873
Thal DR, Rüb U, Orantes M, Braak H (2002) Phases of A beta-deposition in the human brain and its relevance for the development of AD. Neurology 58(12):1791–1800. https://doi.org/10.1212/wnl.58.12.1791
Tsilioni I, Theoharides TC (2018) Extracellular vesicles are increased in the serum of children with autism spectrum disorder, contain mitochondrial DNA, and stimulate human microglia to secrete IL-1β. J Neuroinflammation 15(1):239. https://doi.org/10.1186/s12974-018-1275-5
Vargas DL, Nascimbene C, Krishnan C, Zimmerman AW, Pardo CA (2005) Neuroglial activation and neuroinflammation in the brain of patients with autism. Ann Neurol 57(1):67–81. https://doi.org/10.1002/ana.20315
Vella LJ, Sharples RA, Lawson VA, Masters CL, Cappai R, Hill AF (2007) Packaging of prions into exosomes is associated with a novel pathway of PrP processing. J Pathol 211(5):582–590. https://doi.org/10.1002/path.2145
Wang L, Christophersen CT, Sorich MJ, Gerber JP, Angley MT, Conlon MA (2011a) Low relative abundances of the mucolytic bacterium Akkermansia muciniphila and Bifidobacterium spp. in feces of children with autism. Appl Environ Microbiol 77(18):6718–6721. https://doi.org/10.1128/aem.05212-11
Wang WX, Huang Q, Hu Y, Stromberg AJ, Nelson PT (2011b) Patterns of microRNA expression in normal and early Alzheimer’s disease human temporal cortex: white matter versus gray matter. Acta Neuropathol 121(2):193–205. https://doi.org/10.1007/s00401-010-0756-0
Williams AM, Dennahy IS, Bhatti UF, Halaweish I, Xiong Y, Chang P, Nikolian VC, Chtraklin K, Brown J, Zhang Y, Zhang ZG, Chopp M, Buller B, Alam HB (2019) Mesenchymal stem cell-derived exosomes provide neuroprotection and improve long-term neurologic outcomes in a swine model of traumatic brain injury and hemorrhagic shock. J Neurotrauma 36(1):54–60. https://doi.org/10.1089/neu.2018.5711
Yan S, Zhang H, Xie W, Meng F, Zhang K, Jiang Y, Zhang X, Zhang J (2017) Altered microRNA profiles in plasma exosomes from mesial temporal lobe epilepsy with hippocampal sclerosis. Oncotarget 8(3):4136–4146. https://doi.org/10.18632/oncotarget.13744
Yelamanchili SV, Chaudhuri AD, Chen LN, Xiong H, Fox HS (2010) MicroRNA-21 dysregulates the expression of MEF2C in neurons in monkey and human SIV/HIV neurological disease. Cell Death Dis 1(9):e77. https://doi.org/10.1038/cddis.2010.56
Yelamanchili SV, Lamberty BG, Rennard DA, Morsey BM, Hochfelder CG, Meays BM, Levy E, Fox HS (2015) MiR-21 in extracellular vesicles leads to neurotoxicity via TLR7 signaling in SIV neurological disease. PLoS Pathog 11(7):e1005032. https://doi.org/10.1371/journal.ppat.1005032
Yuyama K, Sun H, Mitsutake S, Igarashi Y (2012) Sphingolipid-modulated exosome secretion promotes clearance of amyloid-β by microglia. J Biol Chem 287(14):10977–10989. https://doi.org/10.1074/jbc.M111.324616
Zhang Z, Chang H, Li Y, Zhang T, Zou J, Zheng X, Wu J (2010) MicroRNAs: potential regulators involved in human anencephaly. Int J Biochem Cell Biol 42(2):367–374. https://doi.org/10.1016/j.biocel.2009.11.023
Zhang L, Dong LY, Li YJ, Hong Z, Wei WS (2012) miR-21 represses FasL in microglia and protects against microglia-mediated neuronal cell death following hypoxia/ischemia. Glia 60(12):1888–1895. https://doi.org/10.1002/glia.22404
Zhang Y, Chopp M, Zhang ZG, Katakowski M, Xin H, Qu C, Ali M, Mahmood A, Xiong Y (2017) Systemic administration of cell-free exosomes generated by human bone marrow derived mesenchymal stem cells cultured under 2D and 3D conditions improves functional recovery in rats after traumatic brain injury. Neurochem Int 111:69–81. https://doi.org/10.1016/j.neuint.2016.08.003
Zhao R-T, Zhou J, Dong X-L, Bi C-W, Jiang R-C, Dong J-F, Tian Y, Yuan H-J, Zhang J-N (2018) Circular ribonucleic acid expression alteration in exosomes from the brain extracellular space after traumatic brain injury in mice. J Neurotrauma 35(17):2056–2066. https://doi.org/10.1089/neu.2017.5502
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2021 The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Mazurskyy, A., Howitt, J. (2021). Extracellular Vesicles in Neurological Disorders. In: Mathivanan, S., Fonseka, P., Nedeva, C., Atukorala, I. (eds) New Frontiers: Extracellular Vesicles. Subcellular Biochemistry, vol 97. Springer, Cham. https://doi.org/10.1007/978-3-030-67171-6_16
Download citation
DOI: https://doi.org/10.1007/978-3-030-67171-6_16
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-67170-9
Online ISBN: 978-3-030-67171-6
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)