Abstract
Background
Statistical cure is achieved when a patient population has the same mortality as cancer-free individuals; however, data regarding the probability of cure after hepatectomy of colorectal liver metastases (CLM) have never been provided. We aimed to assess the probability of being statistically cured from CLM by hepatic resection.
Methods
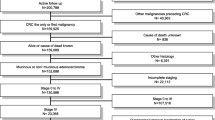
Data from 1,012 consecutive patients undergoing curative resection for CLM (2001–2012) were used to fit a nonmixture cure model to compare mortality after surgery to that expected for the general population matched by sex and age.
Results
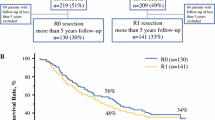
The 5- and 10-year disease-free survival was 18.9 and 15.8 %; the corresponding overall survival was 44.3 and 32.7 %. In the entire study population, the probability of being cured from CLM was 20 % (95 % confidence interval 16.5–23.5). After the first year, the mortality excess of resected patients, in comparison to the general population, starts to decline until it approaches zero 6 years after surgery. After 6.48 years, patients alive without tumor recurrence can be considered cured with 99 % certainty. Multivariate analysis showed that cure probabilities range from 40.9 % in patients with node-negative primary tumors and metachronous presentation of a single lesion <3 cm, to 1.5 % in patients with node positivity, and synchronous presentation of multiple, large CLMs. A model for the calculation of a cure fraction for each possible clinical scenario is provided.
Conclusions
Using a cure model, the present results indicate that statistical cure of CLM is possible after hepatectomy; providing this information can help clinicians give more precise answer to patients’ questions.


Similar content being viewed by others
References
Jemal A, Bray F, Center MM, et al. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90.
US Cancer Statistics Working Group. United States cancer statistics: 1999–2010 incidence and mortality Web-based report. Atlanta, GA: US Department of Health and Human Services, Centers for Disease Control and Prevention and National Cancer Institute; 2013. Available at: http://www.cdc.gov/uscs. Accessed 1 Feb 2014.
Garden OJ, Rees M, Poston GJ, et al. Guidelines for resection of colorectal cancer liver metastases. Gut. 2006;55(Suppl 3):iii1–8.
Tomlinson JS, Jarnagin WR, DeMatteo RP, et al. Actual 10-year survival after resection of colorectal liver metastases defines cure. J Clin Oncol. 2007;25:4575–80.
Pulitanò C, Castillo F, Aldrighetti L, et al. What defines “cure” after liver resection for colorectal metastases? Results after 10 years of follow-up. HPB (Oxford). 2010;12:244–9.
Statistical Methodology and Applications Branch, Data Modeling Branch, National Cancer Institute. Cansurv, version 1.1. Available at: http://surveillance.cancer.gov/cansurv/index.html. Accessed 1 Feb 2014.
Othus M, Barlogie B, Leblanc ML, et al. Cure models as a useful statistical tool for analyzing survival. Clin Cancer Res. 2012;18:3731–6.
Lambert PC, Thompson JR, Weston CL, et al. Estimating and modeling the cure fraction in population-based cancer survival analysis. Biostatistics. 2007;8:576–94.
Terminology Committee of the IHPBA. The Brisbane 2000 terminology of liver anatomy and resections. Abingdon: Taylor & Francis; 2000. p. 333–9.
Smoll NR, Schaller K, Gautschi OP. The cure fraction of glioblastoma multiforme. Neuroepidemiology. 2012;39:63–9.
Fuller AF, Griffiths CT. Gynecologic oncology. Amsterdam: Wolters Kluwer; 1983.
Lambert PC. Modeling of the cure fraction in survival studies. Stata J. 2007;3:1–25.
Tsodikov AD, Ibrahim JG, Yakovlev AY. Estimating cure rates from survival data: an alternative to two-component mixture models. J Am Stat Assoc. 2003;98:1063–78.
Italian population life tables. Available at: http://demo.istat.it/. Accessed 1 Dec 2013.
Adam R, Bismuth H, Castaing D, et al. Repeat hepatectomy for colorectal liver metastases. Ann Surg. 1997;225:51–60.
Adam R, De Gramont A, Figueras J, et al. The oncosurgery approach to managing liver metastases from colorectal cancer: a multidisciplinary international consensus. Oncologist. 2012;17:1225–39.
Cvancarova M, Aagnes B, Fosså SD, et al. Proportion cured models applied to 23 cancer sites in Norway. Int J Cancer. 2013;132:1700–10.
Dal Maso L, Guzzinati S, Buzzoni C, et al. Long-term survival, prevalence, and cure of cancer: a population-based estimation for 818,902 Italian patients and 26 cancer types. Ann Oncol. 2014;25:2251-60.
Viganò L, Capussotti L, Lapointe R, et al. Early recurrence after liver resection for colorectal metastases: risk factors, prognosis, and treatment. A LiverMetSurvey-based study of 6,025 patients. Ann Surg Oncol. 2014;21(4):1276–1286.
Tai P, Yu E, Cserni G, et al. Minimum follow-up time required for the estimation of statistical cure of cancer patients: verification using data from 42 cancer sites in the SEER database. BMC Cancer. 2005;5:48.
Acknowledgment
This work is dedicated to the memory of Prof. Lorenzo Capussotti.
Disclosure
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cucchetti, A., Ferrero, A., Cescon, M. et al. Cure Model Survival Analysis After Hepatic Resection for Colorectal Liver Metastases. Ann Surg Oncol 22, 1908–1914 (2015). https://doi.org/10.1245/s10434-014-4234-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-014-4234-0